Does Georgia Help With My Medicare Premiums
Many Medicare beneficiaries who struggle to afford the cost of Medicare coverage are eligible for help through a Medicare Savings Program . In Washington, D.C., this program pays for Medicare Part B premiums, Medicare Part A and B cost-sharing, and in some cases Part A premiums.
- Qualified Medicare Beneficiary : The income limit is $1,064 a month if single or $1,437 a month if married. QMB pays for Part A and B cost sharing, Part B premiums, and if an enrollee owes them it also pays for their Part A premiums.
- Specified Low-income Medicare Beneficiary : The income limit is from QMB levels up to $1,276 a month if single or $1,724 a month if married. SLMB pays for Part B premiums.
- Qualifying Individuals : The income limit is from SLMB levels up to $1,436 a month if single or $1,940 a month if married. QI pays for Part B premiums.
MSP asset limits: Georgia uses the federal asset limit for QMB, SLMB and QI which are $7,860 if single and $11,800 if married.
State And Federal Spending
During fiscal year 2016, Medicaid spending nationwide amounted to nearly $553.5 billion. Spending per enrollee amounted to $7,067 in fiscal year 2013, the most recent year for which per-enrollee figures were available as of June 2017. Total Medicaid spending grew by 33 percent between fiscal years 2012 and 2016. The Medicaid program is jointly funded by the federal and state governments, and at least 50 percent of each state’s Medicaid funding is matched by the federal government, although the exact percentage varies by state. Medicaid is the largest source of federal funding that states receive. Changes in Medicaid enrollment and the cost of healthcare can impact state budgets. For instance, in Georgia, the percentage of the state’s budget dedicated to Medicaid rose from 19.5 percent in 2010 to 21.9 percent in 2015. However, state cuts to Medicaid funding can also mean fewer federal dollars received by the state.
During fiscal year 2016, combined federal and state spending for Medicaid in Georgia totaled about $9.8 billion. Spending on Georgia’s Medicaid program increased by about 15.4 percent between fiscal years 2012 and 2016. Hover over the points on the line graph below to view Medicaid spending figures for Georgia. Click on the red bar below the graph to view these figures as compared with three of Georgia’s neighboring states.
Georgia Pathways Would Be Costly For The State And Complicated For Enrollees
Although Georgia Pathways is currently on hold due to the legal dispute over the work requirement and premiums, it could still be implemented at a later date. Lets take a look at what the state wants to do in terms of partial Medicaid expansion.
As part of the waiver proposal, Georgia asked CMS to provide the state with full Medicaid expansion funding , despite the fact that the state would only be implementing a partial expansion of Medicaid. A similar request from Utah was rejected by the Trump administration in 2019, and CMS followed the same process for Georgia: The federal government will not provide the 90% funding match for Georgias partial Medicaid expansion, but will instead pay the states normal federal matching rate of 67%. This means it will cost Georgia more to cover the expanded Medicaid population than it would if the state were to simply expand Medicaid fully, as called for in the ACA.
Under the Georgia Pathways program, enrollees must report their community engagement on a monthly basis. But if they comply with the community engagement requirement for at least six consecutive months, theyll be exempt from the reporting requirement and will only have to report changes, if applicable. Eligibility will continue to be redetermined annually.
Recommended Reading: Does Disability Count As Income For Medicaid
What Are The Medicaid Income Limits For 2022
Finding out if you are eligible for Medicaid can be quite a headache. Since Medicaid is jointly funded by federal and state governments, there are different eligibility criteria for each state! One of the biggest factors for Medicaid eligibility are the income limits.
If you are trying to learn more about whether your income is within the Medicaid income limit for your state of residence, then you are reading the right article!
I will be explaining which sources of monthly incoming money are considered income, how each state decides their income limit, and providing an easy-to-use list of each states income limits for the year 2022.
Read on to learn more about Medicaid income limits and determine if your income would be considered within the limit set by your state of residence!
How Does Medicaid Provide Financial Help To Medicare Beneficiaries In Georgia
Many Medicare beneficiaries receive assistance from Medicaid with Medicare premiums, prescription drug costs, and expenses not covered by Medicare including long-term care.
Our guide to financial assistance for Medicare enrollees in Georgia includes overviews of these programs, including Medicaid nursing home benefits, Extra Help, and eligibility guidelines for assistance.
Recommended Reading: Can You Have Insurance And Medicaid
How Do I Apply For Medicaid In Georgia
The Georgia Department of Human Services administers the Medicaid program in Georgia. You can apply for Medicaid ABD or an MSP using this website . Medicaids phone number is 423-4746 in case you have questions about your application.
Josh Schultz has a strong background in Medicare and the Affordable Care Act. He coordinated a Medicare ombudsman contract at the Medicare Rights Center in New York City, and represented clients in extensive Medicare claims and appeals. In addition to advocacy work, Josh helped implement federal and state health insurance exchanges at the technology firm hCentive. He has also held consulting roles, including at Sachs Policy Group, where he worked on Medicare and Medicaid related client projects.
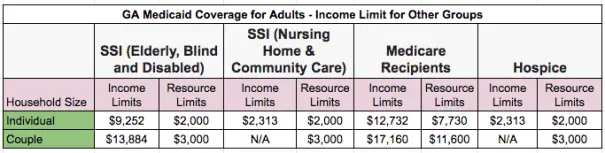
Georgia Medicaid Income Limit Charts
The Georgia Medicaid eligibility income limit charts are divided by groups.
For example, the first chart is focused on income limits for children who qualify for Medicaid.
Similarly, the second chart below focuses on the Medicaid income limits for adults in Georgia who qualify for Medicaid.
Georgia Medicaid Income Limit for Children
Below is the income limit for children by age category. Find the age category your child falls into and you will see the income limit by household size.
| Georgia Medicaid Income Limit Children |
| Children Medicaid Ages 0-1 |
| N/A |
How to Read the Georgia Medicaid Income Limits Charts Above
You cannot have an income higher than the Federal Poverty Level percentage described for your group to be eligible for Medicaid.
Similarly, when you identify the income group that applies to you, the income limit you see refers to the maximum level of income you can earn to qualify for benefits.
For example, if you are pregnant, to qualify for Medicaid, you cannot have an income higher than 141% of the Federal Poverty Level which for a family of two is $24,562 as shown in the chart above.
Read Also: Sign Up For Alabama Medicaid
Medicaid Dental In Georgia
Considering how expensive dental care can be, it would be wise to determine whether Medicaid can help you offset the costs of obtaining it.
Unfortunately, Medicaid dental Georgia services are pretty limited, especially for adults. You can only get dental services if the situation is an emergency or life-threatening. And even so, each medical issue will be handled on a case-by-case basis.
However, Medicaid is kinder to children. They can get regular checkups, pain relief, infection treatment, emergency care, teeth restoration and dental health services. Unfortunately, fewer than 33 percentof dentists accept Medicaid in Georgia, so getting help can be challenging.
References
What Do I Need For Proof Of Income
In order to prove that you fall within the limit for income eligibility, you will need to provide documentation of all sources of income that you have.
Documents to include are things like pay stubs from wages, copies of social security deposits, copies of alimony checks, and award letters from any other monthly financial benefit that you may receive.
It would also be helpful to have all of your most recent income tax returns and any other tax forms that would be relevant to verifying your income.
Some states are able to electronically gather the resources to verify your income, which does simplify the process as well as eliminate fraud. To find out if your state has this technology for your application, click here to learn more about the application process in your state of residence.
Don’t Miss: Does Medicaid Pay For Weight Loss Programs
How To Request A Ride With Ga Medicaid Transportation
There are currently two brokers that provide NEMT services to Georgias 159 Counties. They are LogistiCare and Southeastrans.
For the purposes of GA Medicaid Transportation, the state is divided into five regions by county Central Region, East Region, Southwest Region, Atlanta Region, and North Region.
For details about the four regions, and which region your county falls under, see our Georgia Medicaid Transportation post.
What Are The Different Types Of Care Available
Regular Medicaid is the health care benefits program available to all of a states residents, providing they meet the eligibility requirements. Some of the eligibility requirements include:
- Low-income
- Legal status on the United States
- Resident of the state of application
Those who meet these criteria are able to use their regular Medicaid benefits for their doctors visits, hospital care, laboratory testing, and transportation for medical purposes.
The income limit for regular medicaid will be a set amount, depending on state and marital status. Some states allow one lump sum for a married couple and others have an income limit per spouse.
Medicaid for long-term nursing home care is for those who are elderly and can no longer live independently, those with chronic illness, and people with disabilities. At the facility, the residents receive 24/7 supervision and medical care, as well as lodgings and meals.
All state residents who meet the eligibility criteria and require long-term nursing home care are entitled to and will receive the care. There are no waitlists or lotteries for this benefit and you cant be denied if you meet the eligibility requirements.
However, that is not the case with Medicaids home-based nursing care. This care is for seniors who require daily medical assistance but have enough independance to and prefer to age in their own homes.
Don’t Miss: How Does A Person Get On Medicaid
What Is Covered By Georgia Medicaid
Medicaid in Georgia covers a wide range of services that support the health of its beneficiaries. This includes doctors office expenses, diagnostics, hospital visits and dental treatments. Prescription drugs that are used to cure or treat a medical problem are also covered. For example, insulin or antibiotics are covered but not drugs for hair growth.
Waiver programs are used to cover additional services. All waiver programs in Georgia include care coordination, personal support for daily living activities, home health services, emergency response systems and respite care. Additional services are available under each program but may differ based on the enrollee. Nursing home care is also covered by Medicaid in Georgia.
What If I Dont Meet The Eligibility Criteria
Georgia Medicaid has two pathways available to people who dont meet the income eligibility criteria. These are the Medically Needy Pathway and Qualified Income Trusts, also called Miller Trusts. In both cases, a person can spend down their excess income until it meets the Medicaid eligibility.
The Medically Needy Pathway allows income to be spent on medical bills. With Miller Trusts, excess income can be put in a trust so that the person meets the income limit. Money in the trust can be spent on a specific set of purposes, such as paying for long-term care or medical expenses. Upon the recipients death, money left in the trust will go to the state, up to the amount that the state had paid for care.
Neither of these pathways assists people who dont meet the asset limit, however. There are ways to spend down assets as well though. Modifying a home to improve accessibility, such as by adding ramps or a stairlift, are approved expenditures. People can also spend assets on home repairs, paying off debt or by purchasing a funeral trust. It is important not to transfer or sell assets for less than fair market value, as this can make an applicant ineligible for Medicaid for a period of time. Georgia Medicaid looks back five years at any transfers or sales of assets to determine if this has happened.
Also Check: Doctors That Accept Amerigroup Medicaid
When A Nursing Home Is Medically Necessary
Medicaid will pay for a nursing home only when it is medically necessary. You must show that you have a physical or mental impairment, or a combination of the two, that requires continued nursing care under the supervision of a doctor. This is called needing a “nursing home level of care.” You must show that you cannot care for yourself.
The severity of your impairment will determine what type of facility you need. For example, if you require round-the-clock nursing care, then you will need a skilled nursing facility. On the other hand, if you need only intermittent nursing services, but you have an impairment that prevents you from taking care of yourself, then you may need an intermediate care facility. You must meet at least the intermediate level of care for Georgia Medicaid to pay for a nursing home.
In Georgia, before you are admitted to a nursing home, you will get a Pre-Admission Screening and Resident Review . PASRR screening is intended to assess whether you meet the nursing home level of care and also whether a particular facility can meet your needs.
Financial Requirements In 2022
Applicants have a monthly income limit of $2,523 with a resource limit of $2,000. A couple, if both members need long term care, can have a resource limit of $3,000. If one spouse remains without long term care then the resource and income amounts go up considerably.
Amount of assets community spouse may retain: The maximum value of assets a community spouse can retain for self-support without disqualifying the nursing home spouse from eligibility is $137,400. If the community spouses assets do not equal a minimum of $137,400, he/she may be able to keep some of the nursing home spouses resources until the maximum is met.
Community spouse impoverishment protection: If the community spouses income does not equal at least $3,435.00 per month, he/she may keep some of the institutionalized spouses income in order to meet the limit.
Read Also: Does Medicaid Pay For Assisted Living In Washington State
How To Apply For Medicaid
If youre eligible for Medicaid, you can apply all year round through your state’s Medicaid website or HealthCare.gov, the federal health insurance marketplace. If you apply for Medicaid through Healthcare.gov and it looks like you qualify, the federal government will notify your state agency, which will contact you about enrollment. States also generally let you print out paper applications you can mail, fax or return directly to your local government office.
To complete your Medicaid application, you will likely need to provide documentation that you meet your state’s requirements. This documentation may include:
-
Your birth certificate or driver’s license to serve as proof of age and citizenship
-
Recent pay stubs or tax returns to serve as proof of income
-
Copies of bank statements
-
Proof of address, which could include a lease, utility bill statements or a copy of your mortgage
-
Medical records to serve as proof of disability
States have 45 days to process your Medicaid application. They have 90 days if eligibility is tied to a disability . Processing can take longer if applicants do not supply all of the required documentation. If you don’t qualify for Medicaid, you might be able to get subsidized health insurance through Healthcare.gov. However, only certain life events allow you to apply for a marketplace health care plan outside of open enrollment, which takes place from Nov. 1 to Jan. 15.
Ready to shop for life insurance?
Medicaid Income Eligibility Chart State By State
The following is each of the states, listed alphabetically. Under your state of residence, you will find all of the relevant information regarding the Medicaid Income Eligibility Chart for each of three programs available: regular, in-home nursing care, and institutional nursing care.
Additionally, each of these programs will have additional information about the income limits for those who are single, married with both spouses applying, and married with only one spouse applying.
Recommended Reading: Nys Medicaid Rate Private Duty Nursing
How Much Is The Federal Poverty Level
The federal poverty level in 2021 is equal to an income of $12,880 per year for an individual adult, plus $4,540 for each additional household member. Alaska and Hawaii have different benchmarks because of their differing costs of living.
2021 Federal Poverty Level by State|
Number of people in home |
48 states and Washington D.C. |
Alaska |
|---|
Medicaid And Medicare Dual Eligibility
If you qualify for both Medicare and Medicaid, you are considered dual eligible. In this case, you may qualify for a certain type of Medicare Advantage plan called a Dual Eligible Special Needs Plan . D-SNPs are designed to meet the specific needs of people who have Medicaid and Medicare.
You can compare plans online to find out if D-SNPs are available where you live, or you can call to speak with a licensed insurance agent for information about eligibility and enrollment.
Recommended Reading: Is Dementia Considered A Disability For Medicaid
Service Options Using Resources In A Community Environment
Georgia also operates a waiver program called Service Options Using Resources in a Community Environment . SOURCE offers case management services with primary care physicians, payments for services offered in an assisted living home, home health, personal care, delivered meals, and emergency response services. To qualify for SOURCE, you must be an elderly and disabled Georgian and be eligible for SSI. To apply, contact your local office of the Georgia Aging and Disability Resource Connection .
