Who Qualifies For Medicaid
In all but 13 states, adults who make below a certain income may qualify for Medicaid. In all states, Medicaid is available to people who make a low income and also meet other criteria such as being at least 65 years old, disabled, pregnant or other qualifications.
Each state runs its own Medicaid programs with its own set of qualifying criteria.
Whos Eligible For Medicaid For The Aged Blind And Disabled In Ohio
Medicare covers a great number services including hospitalization, physician services, and prescription drugs but Original Medicare doesnt cover important services like vision and dental benefits.
Medicare can also leave its enrollees with large co-pays, coinsurances and deductibles. Some beneficiaries those whose incomes make them eligible for Medicaid can receive coverage for Medicare cost sharing and services only Medicaid covers if theyre enrolled in Medicaid for the aged, blind and disabled .
In Ohio, Medicaid ABD covers extensive dental benefits, including cleanings, x-rays, extractions, fillings, and dentures. Medicaid ABD also covers one eye exam and a pair of eyeglasses every 12 months for adults 60 and older.
Asset limits: The asset limit is $2,000 if single and $3,000 if married.
Help with prescription drug costs in Ohio
Medicare beneficiaries who have limited incomes and assets can apply for Extra Help a federal program that lowers prescription drug expenses under Medicare Part D. The income limit is $1,615 a month for singles and $2,175 a month for couples, and the asset limit is $14,610 for individuals and $29,160 for spouses.
South Dakota Medicaid For Certain Newborns
South Dakota children born to women eligible for South Dakota Medicaid are also eligible for South Dakota Medicaid.
Eligibility Requirements
- The child must be born to a woman eligible for and receiving South Dakota Medicaid on the date of the childs birth.
- There is no resource or income limit.
- Coverage continues from the month of birth until the end of the month in which the child turns one year of age as long as the child continues to live in South Dakota.
Read Also: Washington State Medicaid Eligibility Seniors
What Is Spousal Impoverishment
Medicaid is a joint federal and state program that helps people with limited income and few assets cover health care costs. Strict financial criteria dictate who is eligible for Medicaid coverage, especially when it comes to long-term services and supports . This makes sense for a single applicant, but how does a married couple meet these financial eligibility requirements?
Recent research shows that the national median cost of a semi-private nursing home room is $7,756 per month. Even couples who have made legal and financial preparations for retirement can quickly exhaust their savings when just one spouse develops a need for this level of care. Sadly, many people have not been willing or able to put funds aside for their future needs. Most older adults rely heavily on benefits from the Social Security Administration as their main source of income in retirement. According to the SSA, half of married elderly beneficiaries receive 50 percent or more of their income from Social Security even though the average monthly benefit for retired workers in December 2020 was only $1,544.
According to Medicaid.gov, These provisions help ensure that this situation will not occur and that community spouses are able to live out their lives with independence and dignity. Now, community spouses are permitted to keep a certain amount of income and assets to pay for their living expenses even after their ill spouses qualify medically and financially for long-term care Medicaid.
Income Requirements For Ohio Medicaid
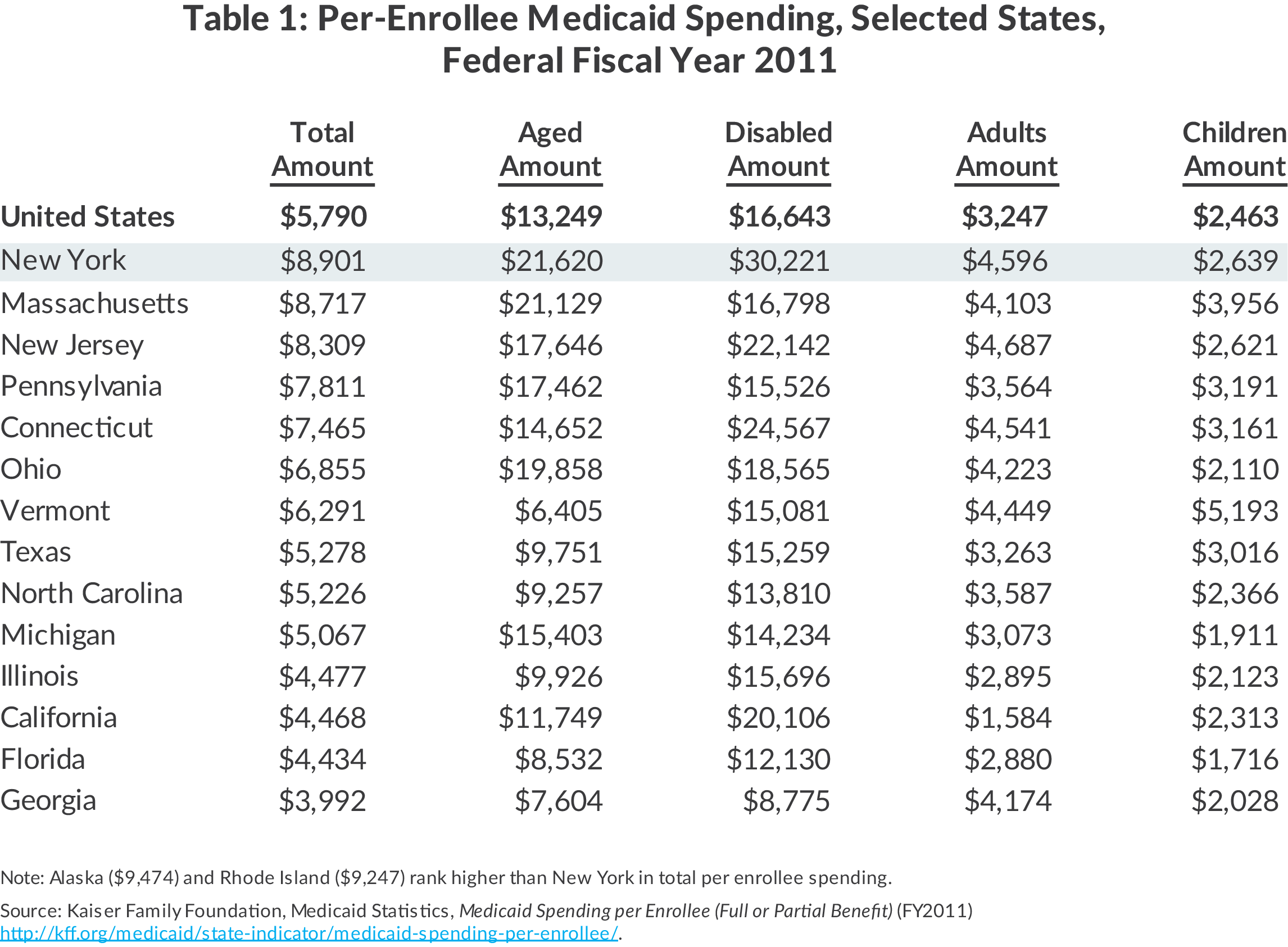
Household size and total amount of income versus outgoing bills plays a part in determining the income limit for each family. Single-family households can make up to $15,800 per year, while a four-person family can bring in $32,319 per year to qualify. Those who fall well below the poverty line, as well as children and pregnant women, qualify most often.
Recommended Reading: Washington State Medicaid Residency Requirements
Is It Hard To Qualify For Medicaid
As long as you meet the eligibility rules in your state, it is not hard to qualify for Medicaid. After all, almost 74 million Americans are covered by the program.
Contact your state Medicaid program in order to apply for Medicaid. Applications are generally reviewed and approved within 90 days and typically are reviewed sooner.
How To Apply For Medicaid In In Ohio
Multiple methods exist for applying for Ohio Medicaid. Many people have taken to the online version which is fast to use and initiates a quick response. A pop-up window comes on the screen when attempting to start a new application. It allows users to either sign in with an existing account or create an account if it is their first time. Provide a first and last name, date of birth, and social security number to sign up and start the process.
Those who do not wish to use the online version may instead visit their local office to fill out a paper form. It can get submitted directly to a worker who can assess the information and approve or deny the claim. It is also possible to apply by telephone by calling the Ohio Medicaid Consumer Hotline at 324-8680.
Recommended Reading: Will Medicaid Pay For Nose Surgery
Are You In Need Of Assistance With Long
Long-Term Services and Supports include services that:
- support individuals who need ongoing care due to age, physical or intellectual disability or chronic illness and
- assist an individual or their caregiver, to live as independently as possible in their homes and communities.
Examples include: meals, transportation, chore services, personal care, counseling, respite for caretakers, adult day health care, benefits counseling, home modifications, assistive technology, etc.
If you would like more information, please take the Assess My Needs survey from the Department of Health and Human Services.
Medicaid For The Working Disabled
Eligibility for Medicaid for the Working Disabled is based on the current year Federal Poverty Level guidelines. Medicaid for the Working Disabled has higher income and resource eligibility guidelines than MABD.
- The monthly income limit for individuals who are blind or disabled, and who work at least a few hours each month, is 250% FPL.
- There is a resource test for Medicaid for the Working Disabled. The limit is $10,000 for one person and $15,000 for a couple. See our Resource Limits Medicaid page.
Dont Miss: What Is Medicaid Buy In Program
You May Like: United Healthcare Customer Service Medicaid
Medicaid And The Asset Test
When it comes to non-MAGI Medicaid eligibility, both your income and your assets come into play. Most of the government programs that qualify you for Medicaid use an asset test. SSI sets the standard.
If your income and assets are above a certain level, you will not qualify for the program. In 2021, the income limit is set at $2,382 per month and the asset limits at $2,000 for an individual.
MAGI Medicaid does not cover everything. Your assets come into play when it comes to Long-Term Services and Supports , the part of Medicaid that pays for long-term care in a nursing home.
Not everything you own will count toward your assets. If you have too many assets, you will need to spend down before you will be eligible for Medicaid. How you spend down, however, is important, because you can be penalized for high-value gifts or transfers made within the past 60 months , aka the Medicaid look-back period.
Medicaid Eligibility In Ohio
Funded by both the federal and state government, the health insurance program known as Medicaid was designed with low-income families in mind. Children, elderly, and disabled members of society are often first among the list of eligible applicants in the state of Ohio. Before applying, it is important to note the states specific criteria for getting approved and accepted into the program to receive coverage.
Read Also: How Do I Qualify For Medicare And Medicaid
Don’t Miss: Is It Bad To Be On Medicaid
Ohio Medicaid Income Limits Summary
We hope this post on Ohio Medicaid Income Limits was helpful to you.
If you have any questions about Medicaid in the state of Ohio, you can ask us in the comments section below.
Help us spread the word! If you found this post on Ohio Medicaid Income Limits helpful, help us spread the word by sharing it using the Share this button below.
Be sure to check out our other articles about Medicaid.
How Do I Become Eligible For Medicaid In My State
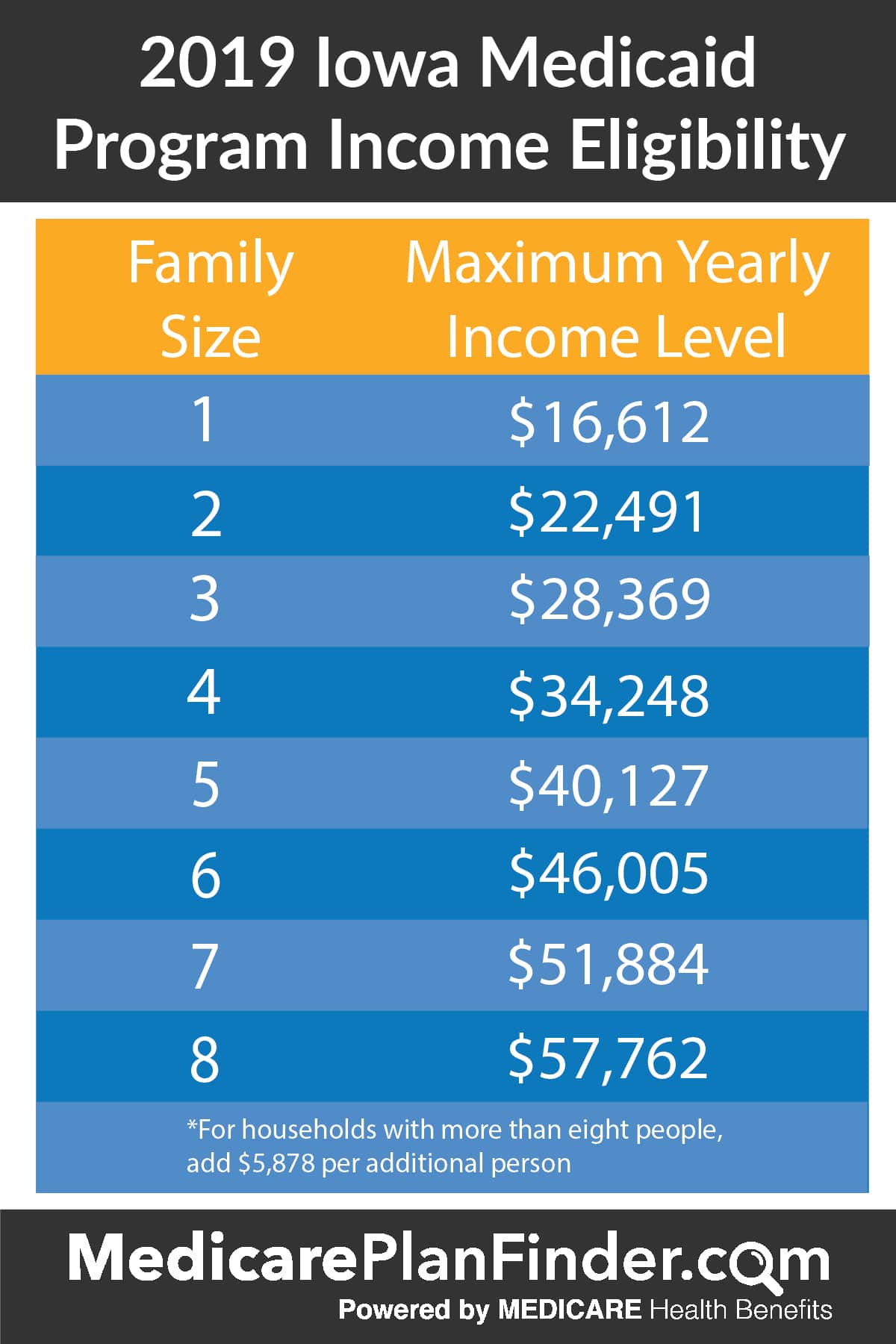
Most states have multiple pathways to Medicaid eligibility. Furthermore, many states allow the use of Miller Trusts or Qualified Income Trusts to help person who cannot afford their care costs to become Medicaid eligible. There are also Medicaid planning professionals that employ other complicated techniques to help person become eligible.
Dont Miss: What Is The Income Limit For Arkansas Medicaid
You May Like: How To Get Medicaid For Seniors
See If You Can Sign Up For Health First Colorado
You may qualify for Health First Colorado if you meet the monthly income guidelines:
| Family Size |
Can I still sign up for a plan through Connect for Health Colorado if I qualify for Health First Colorado?
- Yes. You can still purchase a private health insurance plan at full price if you qualify for Health First Colorado.
- NOTE: If you qualify for Health First Colorado or CHP+, you will not qualify for financial help to lower the cost of your health insurance plan through Connect for Health Colorado. You will pay full price for your health insurance plan.
I applied through Connect for Health Colorado and was told that my application was sent to Health First Colorado. Whats next?
- Watch your mail or email. You will get a notification from the State of Colorado with your application results. You will also receive a letter or email if more information is needed to complete the process.
- You may also check the results of your application through your PEAK account.
- If you do not have a PEAK account, you can create one at Colorado.gov/PEAK.
- You can use your Connect for Health Colorado log-in and password information to sign into PEAK.
- You can also use PEAK to manage your Health First Colorado or CHP+ benefits, print benefit cards, report changes and more.
How Different States Value A Home For Medicaid Eligibility
Each state decides what programs Medicaid offers and the eligibility criteria and the value of ones home equity is one of the eligibility criteria. This means that it is essential to understand the requirements as it pertains to where you live. Many people can get off track due to the wrong information that they find online. Unfortunately, these mistakes can have some drastic impacts such as being denied Medicaid or losing ones home.
In addition to each state having different requirements, the rules regarding home equity can change every year. While this can mean that it is more difficult to find out if you qualify, there are some added benefits to routine changes. For example, as many homes increase in value, some Medicaid recipients would be disqualified from the program if lawmakers didnt increase the amount of equity allowed for their constituents.
It is also important to be aware that they are three types of Medicaid long term care programs: Nursing Home Medicaid, HCBS Waivers and ABD Medicaid. As HCBS Waiver and ABD Medicaid are provided to the beneficiary while they are living in their home, their home is exempt. This is also true if they are applying for Nursing Home Medicaid and their spouse remains in the home.
| 50 State Home Equity Exemption Limits for Medicaid Eligibility |
| State |
Don’t Miss: What’s The Income Level For Medicaid
Spousal Impoverishment Prevention Coverage
This coverage applies to couples where one needs Nursing Care Services in a facility or at home.
The spouse receiving the nursing care services is allowed $3,000. The spouse who remains in the community is entitled to keep half of the couple’s countable assets, but not less than $26,076 and not more than $130,380 for calendar year 2021.
The spouse receiving the nursing care services may keep up to $65 of their monthly income and may deem income to bring the income of the spouse in community up to $2,550 per month and any dependent household members up to $718.
Medicaid For Children And Adults
Eligibility for Medicaid and Dr. Dynasaur are based on the current year Federal Poverty Level guidelines.
- The monthly income limit for adults ages 19 through 64, who are not blind or disabled, is 138% FPL.
- The monthly income limit for children under age 19 is 317% FPL. . There is a monthly premium for some households based on your income. For families up to 195% FPL, there is no premium. There are no prescription co-payments.
- The monthly income limit for Vermonters who are pregnant is 213% FPL. Dr. Dynasaur for pregnant women provides the same coverage as Medicaid, plus full dental coverage. There are no premium or prescription co-pays with this type of Dr. Dynasaur.
Recommended Reading: Does Fidelis Medicaid Cover Bariatric Surgery
District Of Columbia Medicaid
Eligibility overview: Washington, D.C., has one of the most generous Medicaid programs in the U.S., covering adults with household incomes up to 215% of the FPL as part of its expansion program. It also has programs for pregnant, parent/caretaker, elderly, disabled and child residents.
Income requirements: The expansion covers adults without dependents who make up to $2,082 a month when applying on their own. Elderly, blind or disabled D.C. residents are eligible if they make up to 100% of the FPL, or $1,073.33 per month for one individual, and have resources below $4,000 for one person. D.C. also covers pregnant women with incomes up to 319% of the FPL, or $4,703.40 monthly for a two-person household, and parents/caretakers with incomes up to 216% of the FPL.
How to apply for Washington, D.C. Medicaid: You can apply online at DC Health Link or by visiting your closest Income Maintenance Administration Service Center.
Other notable programs: Long-term care and nursing home care services Spend Down, a Medicaid program for people who exceed income limits, but have high medical bills Emergency Medicaid for people who cant qualify for standard Medicaid due to citizenship/immigration status.
Breast And Cervical Cancer Program
The Breast and Cervical Cancer Program is for South Dakota women who need treatment for breast or cervical cancer, including pre-cancerous conditions and early stage cancer.
Eligibility Requirements
- A woman must have been screened for breast and cervical cancer under the Breast and Cervical Cancer Control Program, administered by the Department of Health.
- A woman must be uninsured.
- A woman must meet age requirements.
- An individuals yearly income can be up to $25,520.
- Eligibility coverage ends when a woman’s course of treatment is completed or the state has determined that she no longer meets the criteria for this eligibility category.
Recommended Reading: Does Md Anderson Take Medicaid
What Is The Lowest Income To Qualify For Medicaid
There are 13 states that do not grant Medicaid access to individuals based on income alone.
Of those that do, only Wisconsin uses a limit lower than 138%. An individual in Wisconsin can make no more than the federal poverty level in order to qualify for Medicaid.
Texas has the lowest income limit to qualify on a family basis, at 17% of the FPL. A two-parent household with one child in Texas can make no more than $37,332 and qualify for Medicaid.
How To Calculate Magi For Medicaid Eligibility
Follow the steps below, to calculate your MAGI for Medicaid Eligibility. Please note that this includes estimating any future income that may impact your MAGI.
Step 1
Calculate your households adjusted gross income by using your most recent federal income tax return. Additionally, you can find your AGI on line 7 of IRS Form 1040.
Step 2
Second, add the following types of income to your AGI:
- Tax-exempt foreign income
Do not include Supplemental Security Income .
Step 3
Lastly, adjust your estimate for any changes you expect.
Be sure to consider things future changes or adjustments for all members of your household, such as:
- Expected raises
- New jobs or other employment changes, including changes to your work schedule or self-employment income
- Include changes to income from other sources, like Social Security or investments
- Changes in your household, like gaining or losing dependents. Gaining or losing a dependent can have a big impact on your savings.
In conclusion, you now have successfully calculated your MAGI. Additionally, you should have an estimate of your expected income.
The Nevada Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the Nevada Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
Don’t Miss: Doctors Who Accept Priority Health Medicaid
How Do I Enroll In The Aca
There are several ways to sign up:
-
Enroll online through Healthcare.gov.
-
Use the Find Local Help tool to locate in-person assistance in your area with a navigator as well as with an agent or broker. All of them are trained to walk you through the marketplace process, and services are free.
-
Apply through the website of a certified enrollment partner, such as a private health insurance company.
-
Enroll by phone by contacting the at 800-318-2596. This line is available 24 hours a day, 7 days a week excluding holidays with service in English and other languages.
-
Complete and mail an application.
