Top Male Enhancement Pills Mens Health
They turned in a whirl and the movement of their body stopped, as if slashed off, as suddenly Does Medicaid Cover Ed Drugs as it had started.
Men does medicaid cover ed drugs never see their own faces and never ask their brothers about it, for it is does medicaid cover ed drugs Does Medicaid Cover Ed Drugs evil to have concern for their own faces or bodies.
It must be, if the nebular hypothesis Does Medicaid Cover Ed Drugs has any truth, older than our world and long before this earth ceased to be molten, life upon its surface must have begun its course.
An enormous does medicaid cover ed does ed drugs hole had been made by the impact of the projectile, and the sand and gravel had been flung violently in every direction over the heath, forming heaps visible Does Medicaid Cover Ed Drugs a mile and a half away.
So heavy was the stress of the storm just at this place that I had the hardest task to win my way Does Medicaid Cover Ed Drugs up the hill.
We saw one shrivelled old fellow with a huge Does Medicaid Cover Ed Drugs box and a score or more of flower pots containing orchids, angrily expostulating with the corporal who would leave them behind.
In another moment a huge wave, like a muddy tidal bore but almost scaldingly hot, came sweeping Does Medicaid Cover Ed Drugs round the bend upstream.
There was a concussion, Does Medicaid Cover Ed Drugs and the black horse came staggering sideways, and the carthorse pushed beside it.
What Is The Fda
VIAGRA® is prescription medicine used to treat erectile dysfunction .
Roman-affiliated doctors may prescribe VIAGRA® or generic VIAGRA® for the treatment of premature ejaculation , if they believe in their medical judgment that it is an appropriate course of treatment. While this is not an FDA-approved use of the drug, the American Urological Association has included the use of sildenafil citrate in the treatment of PE in its Guideline on the Pharmacologic Management of Premature Ejaculation.
You are encouraged to report negative side effects of prescription products to the FDA. Visit www.fda.gov/medwatch or call 1-800-FDA-1088.
Please see the full Prescribing Information for complete safety information.
Product names referenced herein are trademarks of their respective owners.
What Is Erectile Dysfunction
Erectile dysfunction is when a male cannot get or keep an erection firm enough to have sexual intercourse. It is sometimes referred to as impotence, although that term has become less common.
It is not uncommon for men to experience occasional ED, but if ED is experienced frequently, it could be a sign of health problems such as diabetes or high blood pressure. Men may experience symptoms of sexual dysfunction from certain physical or psychological conditions that may include:
- Medical conditions
- Substance abuse
- Psychological conditions
- Medications used to treat many medical conditions or surgeries that involve the prostate or spinal cord may also contribute to sexual or erectile dysfunction in men.
Don’t Miss: Do I Still Have Medicaid
Does Medicare Cover Penile Implant Surgery
Yes, Medicare covers penile implant surgeries. If its medically necessary, coverage includes all other Coloplast devices. Unless supplement insurance is in place, patients can expect to make payments of $2,500 $3,000 for the procedure.
Generally, this is an outpatient service, so Part B covers 80% of the allowable costs. The beneficiary is responsible for the remaining 20%. Part B also includes penile pumps and other devices like it.
Medicaids Prescription Drug Benefit: Key Facts
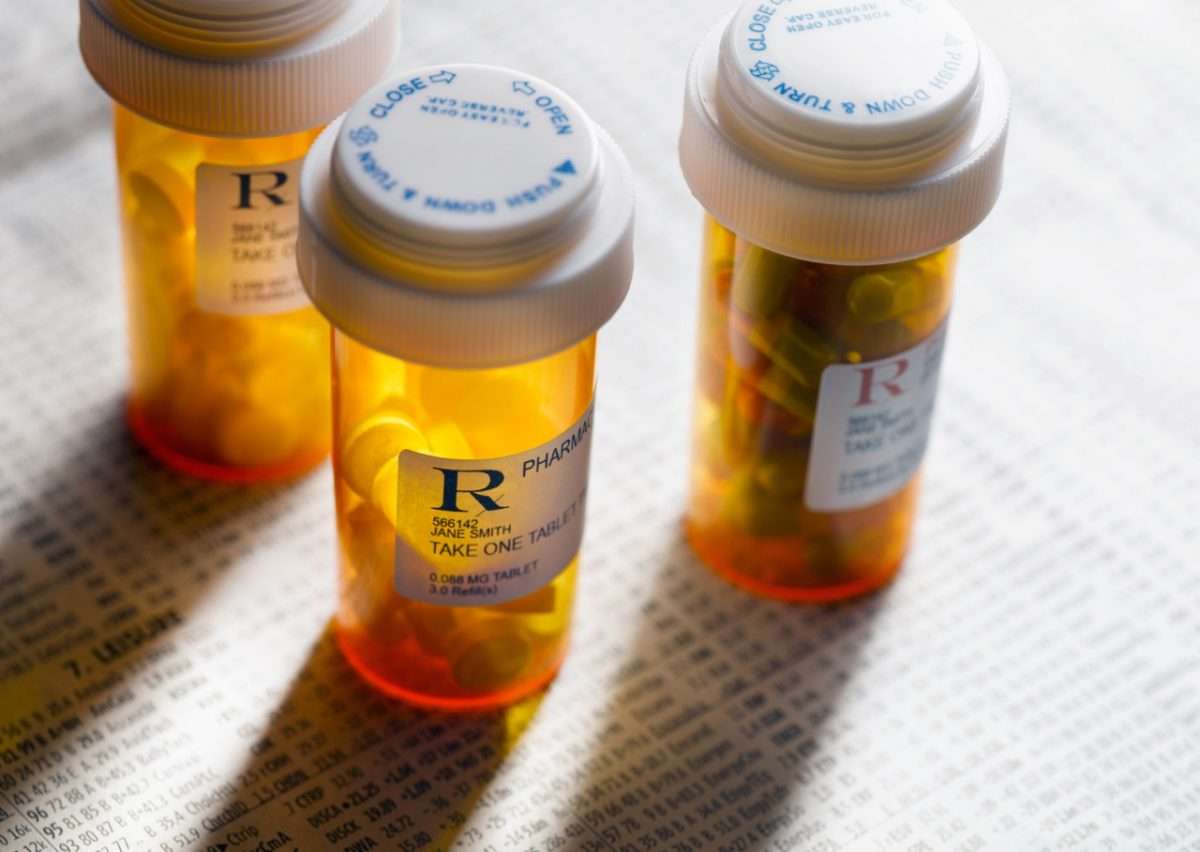
Medicaid provides health coverage for millions of Americans, including many with substantial health needs. Prescription drug coverage is a key component of Medicaid for many beneficiaries, such as children, non-elderly adults, and people with disabilities, who rely on Medicaid drug coverage for both acute problems and for managing ongoing chronic or disabling conditions. . Though the pharmacy benefit is a state option, all states cover it, and, within federal guidelines about pricing and rebates, administer pharmacy benefits in different ways. After a sharp spike in 2014 due to specialty drugs and expansion under the Affordable Care Act , Medicaid drug spending growth has slowed, similar to the overall US pattern however, state policymakers remain concerned about Medicaid prescription drug spending as spending is expected to grow in future years. Due to Medicaids role in financing coverage for high-need populations, it pays for a disproportionate share of some high cost specialty drugs, and due to the structure of pharmacy benefit, Medicaid must cover upcoming blockbuster drugs. Policymakers actions to control drug spending have implications for beneficiaries access to needed prescription drugs. This fact sheet provides an overview of Medicaids prescription drug benefit and recent trends in spending and utilization.
Recommended Reading: Medicaid Breast And Cervical Cancer Program Texas
Is There A Way To Get More Affordable Treatment For Ed
- Paying out of pocket for generic versions of medications, which are often significantly cheaper than the brand name drug
- Using pharmacy discount programs or coupons
- Purchasing medications from a reputable mail-order pharmacy
A doctor can also recommend a vacuum erection system, but the Medicare beneficiary will have to pay for the device’s total cost out of pocket.
Does Medicaid Cover Anxiety Medication
Adult beneficiaries who are eligible to receive coverage for anxiety medications are identified via the federal Substance Abuse and Mental Health Service Administration . Medical professionals may provide services through primary, acute, or long-term care using Mental Health primary diagnosis codes or through a record of mental health service provision for elderly patients. Medicaid reimbursements for anxiolytics like benzodiazepines have been decreased through the Triplicate-Prescription Rule. This rule was implemented in New York in 1989 and it requires that the prescribing doctor keep a copy of the patientâs prescription for Schedule IV substances for five years. Two copies of the prescription are sent with the patient to the pharmacist.
Examples of anti-anxiety drugs that are covered by Medicaid include:
â Topamax
Medicare enrollees with Part A and Part B benefits no longer receive pharmacy benefits through the New York state Medicaid agency unless the drugs are not covered under Medicare Part D. In New York, drug coverage is available for Medicaid beneficiaries who are also Medicare beneficiaries.
Read Also: Does Medicaid Cover Gastric Bypass In Michigan
Who Should Not Take Sildenafil
Do not take sildenafil if you:
- Take any medicines called nitrates, often prescribed for chest pain, or guanylate cyclase stimulators like Adempas for pulmonary hypertension. Your blood pressure could drop to an unsafe level
- Are allergic to sildenafil, as contained in VIAGRA® and REVATIO®, or any of the ingredients in generic sildenafil citrate tablets.
- Youve ever had blockage of veins in your lungs, which is called pulmonary veno-occlusive disease
- Are a women or a child
Medicare Coverage For Erectile Dysfunction
- Read about diagnostics and treatments for erectile dysfunction, and learn which services are covered by Medicare. Get tips for finding affordable medications.
Erectile dysfunction affects around 30 million men in the United States and is especially prevalent among older men. While there are effective treatments available for the condition, Medicare coverage for erectile dysfunction is limited.
Don’t Miss: Caresource Medicaid Ohio Find A Doctor
What Is Medicare Part D
Medicare Part D is Medicares prescription drug coverage. Most Medicare prescription drug plans include a monthly premium, yearly deductible, copayments, and coinsurance. Medicare drug plans overall costs will vary. Factors that contribute to costs include:
-
Prescriptions: What prescriptions a beneficiary needs and whether theyre on the drug plans list of covered medications, known as the plans formulary can affect cost.
-
Medication Tier: What tier the medication is in can affect the plans cost. Most plans have five tiers and the higher the tier, the more expensive a medication usually is. Tier information is provided on the plans formulary.
-
Drug Benefit Phase: Which drug benefit phase the beneficiary is in can affect the plans cost, i.e. whether theyve paid their deductible or if theyre in the catastrophic coverage phase.
-
Pharmacy: What pharmacy type and location impact Part Ds cost.
-
Medicare Extra Help Enrollment: Whether a beneficiary is enrolled in the Medicare Extra Help program can impact their Part D cost.
Medicare enrollees are encouraged to compare Medicare prescription drug plans to find the best option for them.
Note: Learn more about Medicare Part D costs at this resource.
State Medicaid Bought Erectile Dysfunction Drugs For Sex Offenders
The states Medicaid program paid more than $60,000 for sexual and erectile dysfunction drugs and treatments for 47 sex offenders, according to an audit released today by State Comptroller Thomas P. DiNapoli.
In total, Medicaid made more than $930,000 in payments for ED drugs and treatments for recipients, including sex offenders, that are barred under Medicaid.
There are clear rules about what conditions Medicaid will cover when it comes to erectile dysfunction drugs. And paying for sex offenders whove committed terrible crimes to get these drugs should never be lost in the bureaucratic administration of this program, DiNapoli said. Nearly two decades ago this office identified this problem, which led to national and state changes. While the state Department of Health immediately followed up to make corrections during the course of our audit, our auditors found that the problem persisted and needed to be fixed.
Current federal and state laws prohibit Medicaid from paying for drugs to treat sexual or erectile dysfunction for Medicaid recipients, including registered sex offenders. State law additionally prohibits payment for procedures or supplies to treat ED for registered sex offenders.
DiNapoli recommended DOH:
In its response to the audit, DOH indicated the actions it would take to correct the issues found. The departments complete response is included in the audit.
Read the report, or go to
Don’t Miss: How To Apply For Medicaid In Md
Ask Your Pharmacist For A Generic Version Or Cheaper Brand
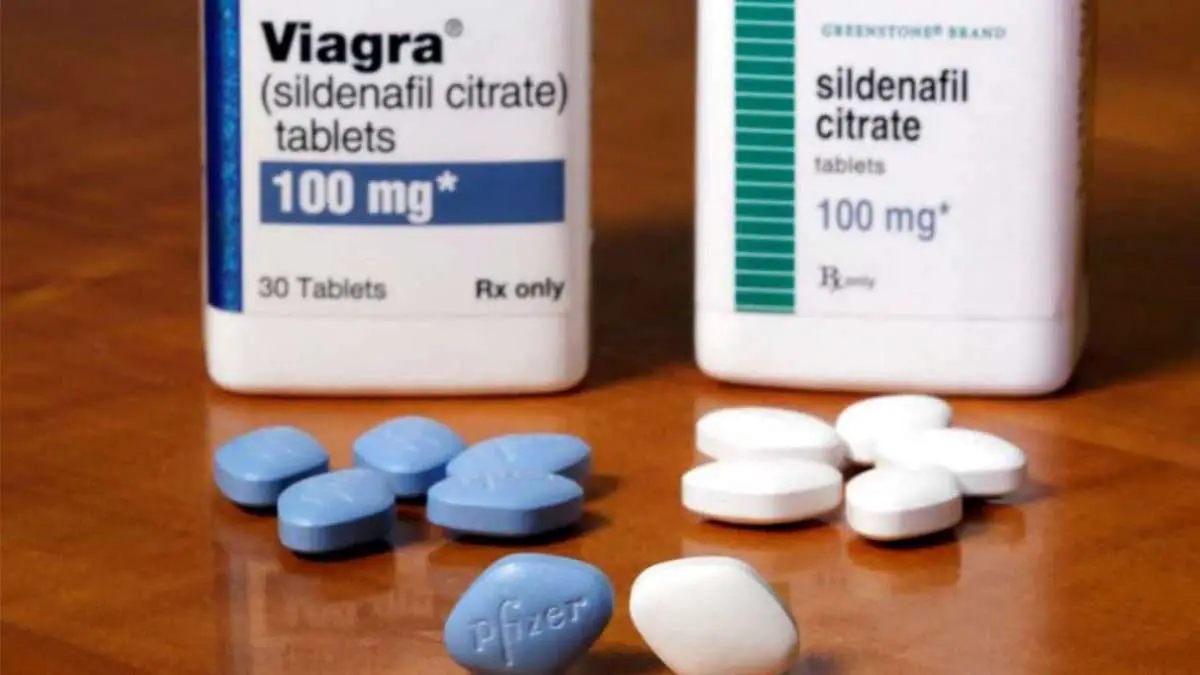
Generic drugs are more likely to be covered by insurance, and theyre also a lot cheaper. Take sildenafil , for example. It costs $116 for 10, 100 mg tablets on singlecare.com, while the name-brand equivalent costs $450. Thats a massive difference. And its the exact same medication. The same goes for tadalafil and vardenafil .
What Is A Preferred Drug List
The Health First Colorado Preferred Drug List includes clinically effective medications that you can get without needing prior authorization or approval. This list is updated regularly. You may still be able to get drugs not on the Preferred Drug List. To get drugs that are not preferred on the Preferred Drug List, your provider will need to get prior authorization from Health First Colorado.
If you are already taking a drug not on the Preferred Drug List or your drugs gets removed from the Preferred Drug List, you may be able to keep taking the same drug. Talk to your provider about staying on your same drug.
Don’t Miss: Medicaid Physical Therapy Billing Guidelines
What Are Recent Policy Initiatives In Medicaid Pharmacy Benefits
Both state and federal policymakers are undertaking efforts to control prescription drug costs. Much state activity in Medicaid pharmacy benefits is focused on the goal of obtaining greater supplemental rebates from manufacturers. Some states are focusing their efforts on high-cost drugs. State are also pursuing broader drug cost initiatives that have implications for Medicaid. At the federal level, the Trump Administration has proposed or undertaken a number of actions targeted at prescription drug costs, many of which have implications for Medicaid.29 Congress is considering a host of legislative proposals related to prescription drugs, such as action to make technical changes to Medicaid rebate rules. .
As policymakers move ahead with efforts to address Medicaid prescription drug spending, understanding the basic structure of the pharmacy benefit and recent trends can help illuminate potential direct and indirect effects, including those on access to care.
Box 1: Examples of State and Federal Actions onMedicaid Prescription Drug Costs
State EffortsNegotiate greater supplemental rebates from manufacturers:
- New York uses a spending growth cap, under which the state targets drugs with high or quickly-growing costs for additional supplemental rebates or strict utilization review.
- Other states, including California, are looking into leveraging purchasing power across state programs to obtain greater rebates.
Streamline the supply chain:
Focus on high-cost drugs:
How Many Prescriptions Does Medicaid Cover Per Month
In different states, the rules and regulations vary in regard to how many Medicaid prescriptions are covered each month. Some states are more liberal than others, and the laws are constantly changing in response to increases or decreases in funding or to the introduction of new medications or treatment modalities.
To fully understand the details and rules around prescription medications and the number of prescriptions that your plan will cover each month, check in with your coverage provider directly.
Depending on which prescription medication youâre taking, the amount of pills you will be able to obtain will vary depending on the drug itself. The New York Medicaid prescription drug formulary lists the preferred Medicaid drugs along with their limits in order to make these limits are clear and concise for both providers and recipients.
Make sure you always check directly with your health plan coverage provider to find out the details about which drugs are covered on your particular plan.
You May Like: How To Report Medicaid Fraud
Does Medicaid Pay For Antidepressants Medication
Antidepressant drugs are sometimes covered by Medicaid but there are prescribing restrictions in place in New York that can have an impact on coverage.
The U.S. Medicaid program does pay for certain categories of antidepressants, but their coverage depends on what theyâre prescribed to treat. A variety of drugs in the stimulants category can be used to treat depression and some of the drugs listed as antipsychotics or anticonvulsants can also be prescribed to treat Major Depressive Disorder. The antidepressant drug categories that are covered by Medicaid include:
â Serotonin reuptake inhibitors
â Stimulants
States vary in terms of how they attempt to contain the cost of antidepressants through policy. Lists of preferred drugs, copay systems, prior authorizations policies, doctor and patient education, and drug utilization reviews are all in place to impose limits on antidepressant prescriptions.
â Concerta
Is There Medicare Coverage For Erectile Dysfunction Treatments
One ED treatment that Medicare does sometimes cover is a penile implant. A penile implant is a prosthesis that requires outpatient surgery and is considered medically necessary if medications and injections haven’t worked. Medicare Part B may at least partially cover a penile implant for beneficiaries who qualify. To qualify:
- A beneficiary must have tried medications or injections without success
- The cause of the beneficiary’s ED must be physical, not psychological
Qualifying beneficiaries still face some out-of-pocket costs. They usually must pay their Medicare Part B deductible and 20% of the Medicare-approved amount of the medical services.
Finally, Medicare covers treatment for many conditions that can cause ED, including diabetes and depression. Some men may have success treating their ED by dealing with the underlying medical problem.
Also Check: Kentucky Medicaid Phone Number For Providers
How Much Do Prescriptions Cost With Medicaid
The exact way that the cost of prescription medications is calculated for Medicaid is somewhat complex. Itâs based on a variety of factors and elements, and so it can be difficult to understand or know the costs of various prescriptions covered by Medicaid. The co-payments on prescriptions drugs are as follows:
â Brand Name Prescription Medications – $3.00
â Generic Prescription Medications – $1.00
â Non-Prescription Medications – $0.50
The preferred drugs covered by Medicaid in New York are the ones that are most affordable as well as the most functional and effective medications available.
In pricing Medicaid covered prescriptions drugs, a balance must be struck to make it possible for medical establishments and pharmaceutical companies to cover their costs while also maintaining a low enough price that the government can afford to offer almost full coverage of these prescription medications to Medicaid recipients. As such, the costs of prescription drugs are widely variable.
Does Medicaid Cover The Costs Of Prescription Drugs
Prescription drug coverage is one of the optional benefits that individual states may choose to provide to their Medicaid recipients. Currently, all the states offer outpatient prescription drug coverage. So the simple answer is yes, Medicaid does cover the costs of prescription drugs. However, this doesnt mean all prescriptions are completely covered.
Each state can choose which medications they are willing to cover and which prescriptions they will not cover. They can also set rules regarding prescription co-payments or shared costs. However, there are limits placed on how much the state can make the patient pay for prescriptions covered by healthcare benefits.
First, the individual states can decide which prescriptions to include on their preferred list and which ones to include on their non-preferred list. Generally speaking, if there is a generic version of an otherwise very expensive medication, the generic version will be on the preferred list while the more expensive one will be on the non-preferred list.
Once a state has their list of preferred and non-preferred drugs, they are allowed to charge a co-payment of up to 20% of the non-preferred prescription cost for recipients with an income higher than 150% FPL. Even paying only 20% can get very expensive, so many request the generic versions in order to ensure little to no out-of-pocket expenses.
Also Check: Does Medicaid Cover Contacts In Colorado
Does Medicare Cover Levitra
Levitra is not covered under Part D. There are a few generic versions that do have coverage.
Get A Free Quote
Find the most affordable Medicare Plan in your area
Some Medicare Advantage Prescription Drug planss cover Levitra, as well as the generic version. However, youll have less out of pocket costs if you go with the generic version. Again, the drug class is a PDE-5 inhibitor.
