Medicare Coverage For Skilled Nursing Care
What are the specific instances where Medicare will cover long-term care? If you or your loved one sustains an injury or suffers some other unfavorable health incident and you are admitted to the hospital for at least three days, Medicare may cover your stay at a skilled nursing facility for up to 100 days. Your stay will only be covered as long as it is deemed medically necessary for your rehabilitation, your condition is steadily improving, and you are expected to return home eventually.
In these qualified situations, Medicare will cover the total cost of a skilled nursing facility for the first 20 days. On days 21 through 100, youll be responsible for covering a daily co-pay , and Medicare will cover the rest. After 100 days, Medicare coverage ends, and youll have to pay the full bill. Again, this coverage hinges on the fact that youre receiving skilled nursing care for rehabilitative purposes and youre showing signs of improvement.
What about Medicaid? Learn how much Medicaid pays for long-term care.
Medicaid Benefits And Services
The services covered by Medicaid vary from program to program and from state to state. What follows are general Medicaid benefits which are typically available in most states.
The Affordable Care Act does not significantly impact Medicaid long term care benefits for the elderly. Therefore, repeal by the Trump administration will have limited impact.
How Can I Start Planning For Long
Now that weve debunked the myth that Medicare covers long-term care , how can you start working on your long-term care plan?
First, get educated about long-term care options. Youre already doing this by learning the truth about Medicare and Medicaid. Great job!
Next, figure out which family members and friends might be able to help you when the time comes. While these conversations can be hard, its better to have them well before you actually need the help. And, again, make sure youre not relying on your loved ones for 100% of your care. This is usually not realistic.
Finally, we recommend getting long-term care insurance when you turn 60 years old. The older you are, the more likely youll be denied coverage. Assess how much care you might need and think about what your expectations are during retirement and beyond.
Don’t Miss: How To Get Copy Of Medicaid Card Online
How Can A Professional Medicaid Planner Help
Professional Medicaid planners provide a wide variety of assistance, from helping with the Medicaid application paperwork to restructuring finances to ensure eligibility. The rules of Medicaid eligibility are complex, state-specific and ever-changing. And the eligibility requirements differ for a single individual versus a married couple. The application process can be exceptionally complex when only one spouse of a married couple is applying for long-term Medicaid. Applications can be further complicated when one spouse is receiving veterans benefits. Professional Medicaid planners are extremely knowledgeable in the complexities of Medicaid, as well as have experience in situations, such as yours, where one spouse will be entering a Medicaid-funded nursing home. Working with a professional is particularly beneficial if you and your spouse are over the income and / or asset limit. Because being over the limits doesnt necessarily equate to denial of Medicaid services. To learn more about professional Medicaid planners, .
Determining Your Medicaid Co
As mentioned before, instead of having a standard co-pay, the amount covered by Medicaid is based on your income. In order to determine your individual Medicaid co-pay, start by taking your total monthly income from all sources. Next, subtract your Personal Needs Allowance. This allowance varies by state but is typically around $50. Then, deduct any qualified medical expenses, such as health insurance premiums. And finally, if you have a community spouse at home who is eligible for an income shift based on the Monthly Maintenance Needs Allowance rules, deduct that amount as well. The resulting amount is then paid to the facility as your Medicaid co-pay, and Medicaid covers the rest.
Interested in finding out what your Medicaid co-pay would be? Get connected with a qualified long-term care planning professional near you!
Read Also: Medicaid Where’s My Ride
What Types Of Care Does Medicaid Normally Cover
For older and disabled adults, Medicaid covers services that other insurance programs may not. Even though there is a federally mandated minimum coverage requirement, each state may add services and programs covered by Medicaid. States are required to cover the following under Medicaid:
- Inpatient hospital services
- Transportation to medical care
- Other services involve pediatric and pregnant mothers
Some states have added benefits under Medicaid that can include others like optometry, podiatry, prescription drugs, respiratory, physical and occupational therapy, speech, language, and hearing disorders. Please check with your state to determine exactly what programs you might be eligible for and what medical services are covered.
Depending on the state, Medicaid also has the advantage of providing expanded home care services. Medicaid can also pay family members who provide caregiving to a loved one. Personal care assistance, although not mandated by the federal government, might be offered. This includes help with bathing, dressing, toileting, housekeeping, and cooking.
Under Medicare, these aide services are not permitted under the medical home health benefit. Medicaid may pay for these services on an ongoing basis as long as the need remains the same.
What Do Va Long
For extended care services, veterans may be subject to a co-payment of up to $97 per day. The amount of the co-payment depends on the veterans VA health system priority group and individual financial circumstances, and also on the type of care or service provided. The amount of co-payment for extended care services is based on income, and for some services, co-pay amounts are based on the assets held by both the veteran and the veterans spouse.
For extended care services expected to last 180 days or less, the VA looks only at the income of the veteran and spouse, taking into account the veterans expenses. For extended care services expected to last 181 days or longer , the VA looks at the income and the assets of the veteran and spouse. Details of these financial calculations are available from the VAs publication VA Copays and Charges.
Read Also: Missouri Medicaid For College Students
Medicaid Nursing Home Benefits
Medicaid pays 100% of nursing home costs in most cases if you meet eligibility requirements. In most states, the monthly income limit is $2,382 for individuals or $4,764 for spouses. Your countable resources must be less than $2,500. Income and resources that count toward the limit include:
- Wages
- Propertyâ
- Life insuranceâ
âIn most states, Medicaid looks at your income over the last 5 years. Any assets you transferred out of your possession within that time may still count toward your income. Do not try to transfer financial assets in order to qualify for Medicaid.ââ
You may be penalized for violating Medicaid rules. This can result in having to pay for your nursing home care out-of-pocket until you meet eligibility requirements.ââ
Keep in mind that eligibility is on a rolling basis. It is possible to make as little as $1 over the monthly income limit and not qualify for the entire month. If this happens, you may have to pay for your nursing home care and related expenses yourself.ââ
Types of nursing home coverage. You have three nursing home options with Medicaid:
- Skilled nursing â care related to medical issues and related services
- Rehabilitation â staying in a facility short-term following an illness, injury, or surgery â
- Long-term care â around-the-clock care at a facility because of a mental or physical condition â
Skilled Nursing Facility Care Under Medicare: Whats Covered And When
- Strict limitations apply to Medicare coverage for skilled nursing facilities. A hospital stay is required prior to receiving skilled nursing facility coverage. Following a hospitalization, medical services are covered for the first 100 days after discharge. Copayments are required after the original coverage term has expired.
If you believe that Medicare will cover skilled nursing care, you are not entirely incorrect. However, coverage restrictions might be difficult to understand, and there are some standards you must complete before you can book your trip. Briefly stated, Medicare will cover some short-term skilled nursing facility stays in particular circumstances. If you require continuous or long-term care in a skilled nursing facility, you will be required to pay for these services out of pocket or to rely on other government programs to cover the costs.
Medicare is a government health-care program that provides coverage for adults over the age of 65, as well as those with certain medical conditions. Medicare coverage is divided into a number of distinct schemes, each of which provides a different level of coverage at a different price.
Don’t Miss: How To Get Medicaid Certified
Assisted Living / Senior Living Communities
The number of state Medicaid programs helping with assisted living is increasing, and this trend looks like it will continue until assisted living assistance is available nationwide. As of mid 2019, in 44 states and the District of Columbia, Medicaid pays for some assisted living fees, mostly by way of Medicaid Home and Community-Based Services Waivers. To be clear, Medicaid will not pay for room and board or rent in assisted living communities. However, there are other programs open to Medicaid beneficiaries that can help. In addition, there are assisted living-like programs that may not be called assisted living, but provide a very similar experience. Read each states assisted living policy and learn about specific Medicaid waivers here. Often positioned as an alternative to assisted living or nursing home care, adult foster care is covered by Medicaid in many states. Read states adult foster care policies here.
Ohio’s Medicaid Resource Limit
In addition, to qualify for Medicaid in Ohio, you must have no more than $2,000 in resources . Resources are assets like money and property. Some property does not count toward the resource limit. In Ohio, for example, your car can be exempt, and your home is exempt up to an equity value of $585,000 in 2019. If you have more equity in your house, it will be counted toward the resource limit. Personal belongings are also exempt. Retirement accounts are counted as assets only to the extent you can withdraw money from them.
If you have a spouse who will continue to live “in the community” , then one car is exempt with no restrictions on its value. In addition, your home is exempt so long as your spouse still lives there.
You May Like: Annual Income To Qualify For Medicaid
How To Find Out If Your Home Health Care Is Covered By Medicare
Before you start getting your home health care, the home health agency should tell you how much Medicare will pay. The agency should also tell you if any items or services they give you arent covered by Medicare, and how much youll have to pay for them. This should be explained by both talking with you and in writing.
Medicare For Drug And Alcohol Rehab

Medicare is accessible to everybody over the age of 65, as well as to those who are physically disabled. Medicare is provided in exchange for a monthly premium that is determined by the recipients annual income. People with lesser incomes pay cheaper insurance rates. Treatment for drug addiction might be covered by Medicare for inpatient and outpatient treatment. It is divided into four sections, each of which covers a distinct aspect of addiction rehabilitation programs.
Also Check: Apply For Pregnancy Medicaid Alabama
Cognitive Or Behavioral Issues
Memory and other cognitive issues due to dementia or Alzheimers may prevent the person from living independently or even in assisted living. Behavioral problems could also be preventing someone from residing safely in a less restrictive environment.
Some states will not accept dementia as the only reason to qualify for nursing home care. There must be other skilled needs as well. This is to prevent families from using a Medicaid nursing home bed without a skilled nursing need. Each state will determine the nursing home level of care and use several assessment tools to determine eligibility. A re-evaluation of nursing home needs is done every 12 months.
How And When Medicaid Can Pay For A Nursing Home
Medicaid was created in 1965 as a social healthcare program to help people with low incomes receive medical attention. Many seniors rely on Medicaid to pay for long-term nursing home care.
Most people pay out of their own pockets for long-term care until they become eligible for Medicaid. Though Medicare is an entitlement program, Medicaid is a form of welfareor at least thats how it began. So to be eligible, you must become impoverished under the programs guidelines, says Laura M. Krohn, a Rhode Island-based elder law attorney.
Let’s look at how the economics work, and how Medicaid can be used to pay for a nursing home.
You May Like: Qualifying For Medicaid In Arizona
How Much Does Medicare Pay For Long
Many seniors are under the assumption that Medicare will cover some or all of their long-term care. Unfortunately, that is not the case. Medicare only covers a nursing home stay in specific circumstances for elderly or disabled individuals who are recovering from an injury, illness, or some other adverse health event. On the other hand, seniors who require custodial carethat is, assistance with their activities of daily living, such as eating, bathing, dressing, toileting, and transferringmust use other sources to pay for their long-term care.
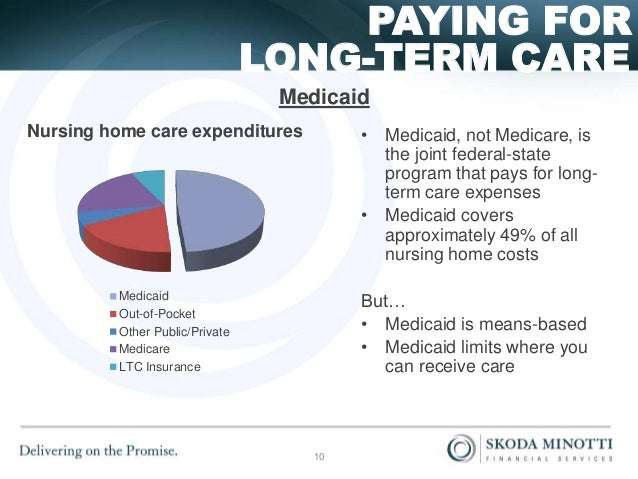
READ: Medicare vs. Medicaid: Paying for Long-Term Care
Statistics On Medicaid In The Us
- States are permitted to expand Medicaid coverage to almost all low-income individuals under the age of 65 under the Affordable Care Act signed into law in 2010. A drug use problem affects about one-quarter of Medicaid beneficiaries over the age of 18 who are over the age of 18. 2, Over 6,500 people seek emergency medical attention every day for substance abuse-related disorders. 2
- Medicaid paid for more than 42 percent of all births in the United States in 2018, according to the National Center for Health Statistics. 7
- In 2017, Medicaid covered more than 30% of the cost of long-term care for those who live in nursing homes or continuing care retirement communities. 7
Recommended Reading: Does Medicaid Cover Auto Accidents In Michigan
Residential Care Or Inpatient Treatment Centers
Residents of inpatient/residential live-in treatment programs get drug and alcohol therapy while they are residing on-site at the institution.
For the most part, inpatient treatments take anywhere from 15 to 90 days, depending on whatever program youre in and your specific requirements. According to the length of the treatment program, Medicaid may pay for in-patient residential therapy.
Medicaid And Rehabilitation Coverage
Health insurance provided by the Medicaid program, a joint federal-state initiative, helps millions of individuals with low financial resources pay for healthcare, which might include the expenses of rehabilitation that Medicare does not cover. The majority of the time, if you are dual-eligible for Medicare and Medicaid, your rehab services will be billed to Medicare first, with any residual expenditures being transferred to Medicaid.
You may still be required to satisfy a deductible or contribute a portion of the cost of your rehab before your Medicaid benefits kick in, but these benefits will most likely continue for as long as your rehab is judged medically necessary by the Medicaid program.
You May Like: How To Apply For Medicaid In Houston
What If You Need More Time
Health insurance provided by the Medicaid program, a joint federal-state initiative, helps millions of individuals with little financial resources pay for healthcare, which might include the expenses of rehabilitation that are not covered by Medicare. Your rehab services will most likely be billed to both Medicare and Medicaid, with any residual expenditures being transferred to Medicaid if you are dual-eligible for both programs. Before your Medicaid benefits may kick in, you may still be required to satisfy a deductible or contribute a portion of the cost of your therapy.
Contribution To Cost Of Care

Medicaid requires you to contribute most of your income to your long-term care when you are living in a nursing home or receiving home health care services. You are allowed to keep a small fixed amount of money as a “personal needs allowance” to pay for uncovered medical expenses and, if you live at home, for food, clothing, and housing, or if you live in a nursing home, for small extras like snacks, subscriptions, and personal products. You must pay the remainder toward your long-term care.
The amount of money that you are allowed to keep each month depends on your state’s rules and may also vary depending on your living arrangements: if you live in a nursing home, your personal needs allowance may be lower than if you live in an assisted living facility or adult foster home, and if you live with your spouse and receive home health care services, your personal needs allowance may be lower than if you live alone and receive home health care services.
Some states will allow you to put excess income above the Medicaid limit into a trust in order to qualify for Medicaid. At your death, the trust proceeds go first to pay off any long-term care that the state provided. Because long-term care is so expensive, there is usually very little left over for heirs.
Don’t Miss: Nursing Homes In Huntsville Al That Take Medicaid
North Carolina’s Medicaid Program Will Pay For A Nursing Home Only If You Have Limited Income And Assets And You Need Skilled Nursing
Updated By Douglas Witten
In North Carolina, Medicaid is a common source of funding for long-term care, particularly when people have already used up all of their own assets to pay for private care. And this doesn’t take longin 2018, the average daily cost of a private room in a nursing home in North Carolina was $254. Plus, private health insurance policies generally do not cover long term care, very few people purchase private long-term care insurance policies, and Medicare coverage for long-term care services is very limited.
In North Carolina, Medicaid is administered by the Division of Medical Assistance . To apply for Medicaid, contact the Department of Social Services office in your county. You can also apply online.
Not everyone can get Medicaid to pay for nursing home care in North Carolina, however. You must medically require skilled nursing care, and your income and assets must fall under the state Medicaid limits. The eligibility rules for long-term care services like nursing homes are different than for other Medicaid services.
