I What You Should Expect To Pay For Home Care In Arkansas
Per Genworths 2021 Cost of Care Survey, in-home care costs an average of $4,185 per month. This typically covers assistance with daily activities and personal care provided by an aide. You can expect to pay $4,195 per month for home health care, which includes clinical or rehabilitative care provided by a nurse, therapist or other licensed health care professional.
Contribution To Cost Of Care
Medicaid requires you to contribute most of your income to your long-term care when you are living in a nursing home or receiving home health care services. You are allowed to keep a small fixed amount of money as a “personal needs allowance” to pay for uncovered medical expenses and, if you live at home, for food, clothing, and housing, or if you live in a nursing home, for small extras like snacks, subscriptions, and personal products. You must pay the remainder toward your long-term care.
The amount of money that you are allowed to keep each month depends on your state’s rules and may also vary depending on your living arrangements: if you live in a nursing home, your personal needs allowance may be lower than if you live in an assisted living facility or adult foster home, and if you live with your spouse and receive home health care services, your personal needs allowance may be lower than if you live alone and receive home health care services.
Some states will allow you to put excess income above the Medicaid limit into a trust in order to qualify for Medicaid. At your death, the trust proceeds go first to pay off any long-term care that the state provided. Because long-term care is so expensive, there is usually very little left over for heirs.
Paying For Nursing Home Care Before You Are Medicaid Eligible
If you are suffering from a serious illness or disability, you may eventually need to move into a facility that provides constant care, but that can be a problem without advance planning. While Medicaid covers the cost of a nursing home for those who qualify, unexpected problems during the lengthy application period may put your family in a difficult financial situation.
Also Check: Medicaid Provider Enrollment Phone Number
Michigan Medicaid Expansion Update
Michigan expanded Medicaid as of April 2014. The expanded Medicaid program is called Healthy Michigan.
Nearly 750,000 Michiganders are enrolled in expanded Medicaid as of mid-2020, up from about 650,000 before the COVID-19 pandemic began.
In addition, work requirement for Medicaid took effect as of January 2020, but a judge overturned it in March 2020.
University of Michigan researchers reported that the expansion of Medicaid in Michigan resulted in about 30,000 new jobs.
Furthermore, it resulted in a $2.3 billion increase in personal income in the state in 2016.
Are There Options If I Make More Than The Limit
There might be some options to still receive Medicaid benefits if you make more than the income limit in your state.
The options do differ from state to state, but the majority do offer a pathway for those who would be considered medically needy and have high medical expenses.
If someone who requires a lot of medical care has too high of an income, they might be able to spend that income on their medical costs and then have that count against their income.
For example, if someone was $500 over the income limit in their state and that state has a program for the medically needy, they might be permitted to spend that excess income on their medical expenses and then receive Medicaid benefits after. This helps those with high than average medical costs be put on more equal footing for income eligibility requirements.
Not every state offers this particular program, however. For a great resource on the sorts of waivers, exceptions, and other eligibility information, visit this website. Once you click on your state of residence, you should be able to see which waivers are available in your state for those who exceed the income limit.
Also Check: Medicaid For Pregnant Non Citizens
What Counts As Income
The monthly financial amount that you receive from employment wages, benefits from Social Security, payments from a pension plan. Alimony, and payouts from stocks, IRAs, and other investment returns.
Mostly likely, if it is a form of money that you receive monthly, then it would count as income. However, if you are not sure about one of your sources of money, it is always better to err on the side of caution and check with your Medicaid program coordinators.
For applicants who are single or divorced, these monthly amounts are simply added up and the total number is the amount you can compare to the income eligibility limits in your state of residence. If it matches or is less than the limit for your state, you should be able to receive Medicaid health care benefits.
For applicants who are married, the protocol for evaluating income limit can differ depending on which state you reside in.
Most states have either one limit amount that each spouse can contribute to asymmetrically or a limit amount where each spouse can only make up one half of the total. Also, there are a few states where you are considered a single applicant, regardless of marital status.
There are also cases where you are married, but only one spouse is applying for Medicaid benefits. Again, the protocol will differ depending on the state of your residence. Most states will either treat the spouse applying as a single applicant or will consider their income limit as a married applicant.
What About Assisted Living Medicaid Or In
Assisted living or in-home Medicaid in Florida is very difficult to access. If the applicant’s assets are less than the income and asset limit, this does not mean the applicant will get Medicaid to help pay for assisted living. There is a long waitlist to get Medicaid for assisted living care and we have no way of telling when or if the elder will come off the wait list. We have more on assisted living Medicaid and bypassing the assisted living waitlist here.
Recommended Reading: Does Medicaid Pay For Partials
Transferring Assets And Medicaid Eligibility
A number of people who eventually need Medicaid assistance have gifted cash or cash-equivalent assets to their children or other members of the family either inadvertently or deliberately prior to applying for Medicaid. Any transfer for less than value, whether it is a gift or at a reduced purchase price, is subject to a penalty from Medicaid at any time during 60 months from the date of the gift. The penalty is calculated by dividing the less-than-value amount of the transfer by the average monthly Medicaid nursing home cost in the state. Each state publishes its monthly average Medicaid cost at least yearly.
The penalty is calculated by dividing the $500,000 by the state Medicaid penalty rate which is $5,000 a month. The result is a period of 100 months or approximately 8 years where John must pay for his nursing home cost out of his own pocket before Medicaid will start helping him cover the cost. When John transferred the assets he started the clock ticking on what is called “the look back.” This is a period of 60 months or five years in which Medicaid can assess the penalty if a transfer for less than value has occurred. After the look back has been met, Medicaid cannot assess a penalty.
Transfers of the home may also be made under certain conditions without Medicaid penalty. Here are those exceptions.
A: Have A Professional Informal Eligibility Assessment
Once you have made the decision that the applicant will be financially eligible, it is recommended you confirm this assessment with a professional. Submitting your application correctly the first time is a lot of work, but its still much easier than having to appeal a denial. Any mistakes make a delay or denial of benefits more likely, even if the applicant is eligible.
One way to get help is a benefits counselor at your local Area Agency on Aging. AAA offices are meant to help with exactly this sort of issue for older adults, and they will be experts on your specific state requirements. Theyre also free. The downside of getting help from AAA, however, is that theyre busy and may not be able to assist as soon as youd like. To find your local AAA office, .
Another option to get help with your Medicaid application is a Certified Medicaid Planner. Unlike the AAA benefits counselor, CMPs are paid services. CMPs will, however, offer an initial consultation for free. https://cmpboard.org/ For much more on Medicaid planning, see below.
Read Also: Can You Get Medicaid At Age 62
New Mexico Medicaid Income Limit
The New Mexico Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the New Mexico Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 300 percent of FPL
- Any child age 1-5 with a family income up to 300 percent of FPL
- Children ages 6- 18 with family income up to 240 percent of FPL
- CHIP for children with family income up to 300 percent of FPL
- Pregnant women with family income up to 250 percent of FPL
- Parents of minor children with family income up to 42 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 74% of the FPL
- Adults without dependents under Medicaid expansion with income up to 133% of the FPL
Example Of How Penalty Period Is Calculated
Diane transfers $97,030 to her son in December 2019 and $97,030 to her daughter in January 2020. She then applies for Medicaid in January 2020, at which point she meets all eligibility requirements except for the uncompensated transfers. The penalty period begins to run at that point. Medicaid would deem her ineligible for benefits for the next 20 months . She will be eligible for Medicaid benefits, assuming she still meets all other criteria, in September 2021.
In the event that an applicant and his other family face a situation where gifting is going to create a delay in Medicaid eligibility, or if Medicaid has been denied and the delay of eligibility has been determined by the Department of Children and Family Services, legal steps may be taken to eliminate or reduce the period of ineligibility. Contact our Florida elder law attorneys.
Don’t Miss: How Do I Renew My Child’s Medicaid
What Is A Medicaid Lookback Period
The Medicaid lookback period is a period of time in which any transfers of assets to family members may be subject to scrutiny for Medicaid eligibility. If it’s determined that you specifically transferred assets during the lookback period in order to qualify for Medicaid, this can affect the benefits for which you’re eligible.
When A Nursing Home Is Medically Necessary
Medicaid will pay for a nursing home only when it is medically necessary, meaning that a doctor has said you need a nursing home because you have a condition that requires more care than just room and board. This is called meeting the “nursing home level of care.” In Pennsylvania, to meet the nursing home level of care, you must show that either you need skilled nursing or rehabilitation services or that you need some kind of health-related care to be provided to you on a regular basis. You must show that you cannot provide the care yourself and that you need some type of licensed staff to provide services for you.
In Pennsylvania, before you are admitted to a nursing home, you will get a Pre-Admission Screening and Resident Review . PASRR screening is intended to assess whether you meet the nursing home level of care and also whether a particular facility can meet your needs.
You May Like: Mosquito Repellent Covered By Medicaid
V Free Resources For Aging In Place In Arkansas
Remaining at home has many benefits for seniors, such as living in a familiar environment and being close to loved ones, though aging in place can present some challenges. Arkansas has several free and affordable services to help older adults maintain a high quality of life and live independently, safely and comfortably at home.
| Contact |
Future Medicaid Claims Against Your Estate
If you are over 55 and receive long-term care through Medicaid, or if you are permanently institutionalized before you turn 55, your state’s Medicaid program will have a claim against your estate after your death for the amount that the state spent on your care while you were receiving Medicaid. This is called Medicaid estate recovery. However, the state will not try to recover from your estate until after your spouse dies and only if you have not left any minor or disabled children. Some states, including California, can also recover the cost of Medicaid services other than long-term care servicesâas long as they were incurred after you turned 55.
Self-help services may not be permitted in all states. The information provided on this site is not legal advice, does not constitute a lawyer referral service, and no attorney-client or confidential relationship is or will be formed by use of the site. The attorney listings on this site are paid attorney advertising. In some states, the information on this website may be considered a lawyer referral service. Please reference the Terms of Use and the Supplemental Terms for specific information related to your state. Your use of this website constitutes acceptance of the Terms of Use, Supplemental Terms, Privacy Policy and Cookie Policy. Do Not Sell My Personal Information
Read Also: Is It Hard To Get Medicaid In Florida
Massachusetts Medicaid Income Limits Summary
We hope this post on Massachusetts Medicaid Income Limits was helpful to you.
If you have any questions about Medicaid in the state of Massachusetts, you can ask us in the comments section below.
Help us spread the word! If you found this post on Massachusetts Medicaid Income Limits helpful, help us spread the word by sharing it using the Share this button below.
Be sure to check out our other articles about Medicaid.
Do All Facilities Accept Medicare And/or Medicaid Reimbursement For Care
Many skilled nursing and intermediate care facilities accept Medicare and/or Medicaid reimbursement, but residential care facilities do not. However, residential care facility residents may be eligible for state assistance through the Supplemental Nursing Care grant. In addition residential care facilities may participate in the Medicaid Personal Care Program. The Personal Care Program offers Medicaid-eligible residents assistance with activities of daily living. This program provides residential care residents an alternative to nursing facility care.
Recommended Reading: Aetna Medicaid Louisiana Phone Number
Don’t Miss: Molina Medicaid Michigan Prior Authorization Form
Home Care Waiver Programs
Pennsylvania also operates several Medicaid Waiver programs that provide home health care services to low-income Pennsylvanians.
To qualify for any of Pennsylvania’s Waiver programs, you must meet the nursing home level of care. In addition, you must have income less than $2,163/month and fewer than $8,000 in resources. To apply for waiver programs, contact the Office of Long-Term Living Helpline at 866-286-3636.
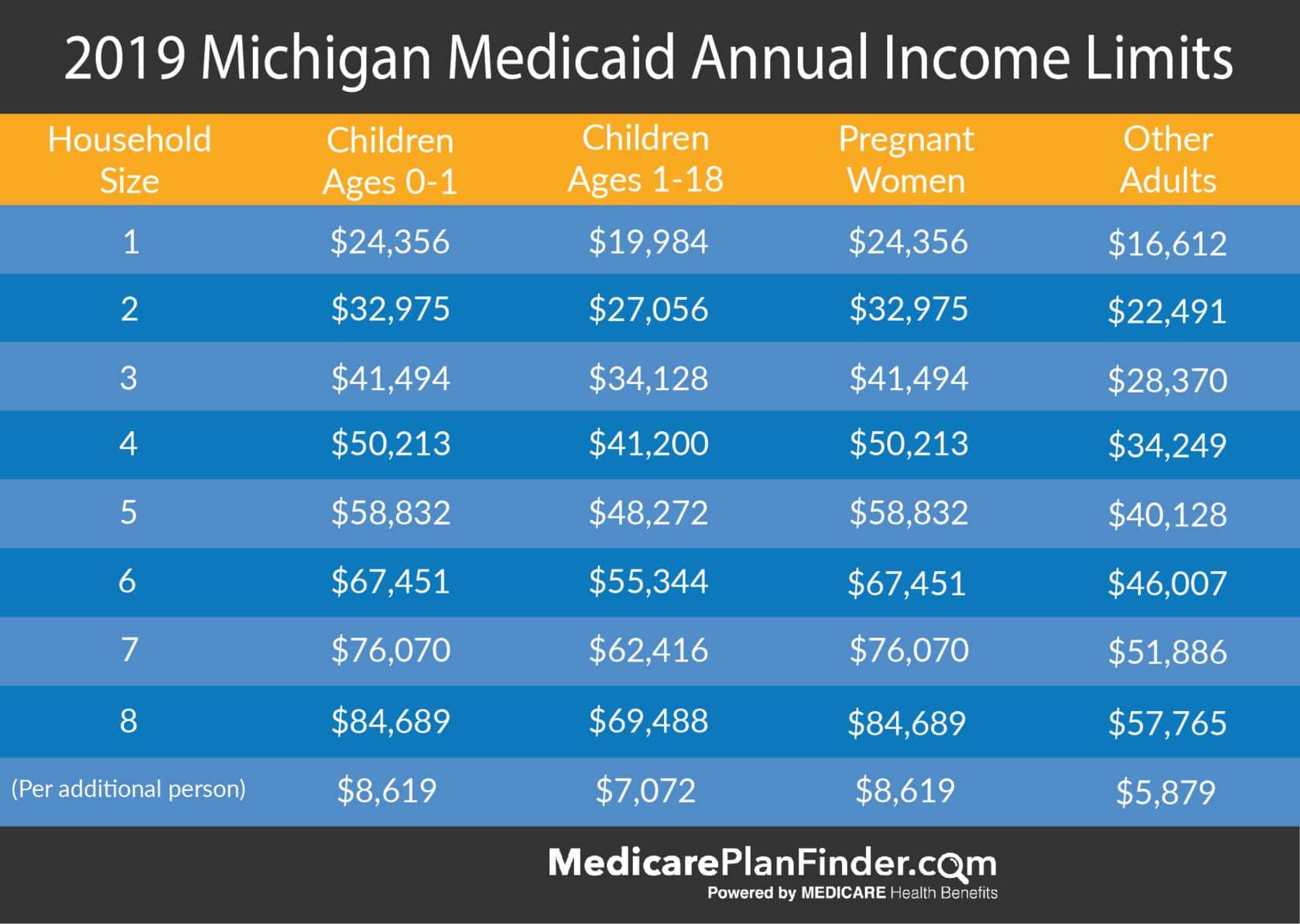
Michigan Medicaid Income Limit Charts
The Michigan Medicaid eligibility income limit charts are divided by groups.
For example, the first chart is focused on income limits for children who qualify for Medicaid.
Similarly, the second chart below focuses on the Medicaid income limits for adults in Michigan who qualify for Medicaid.
Michigan Medicaid Income Limit for Children
Below is the income limit for children by age category. Find the age category your child falls into and you will see the income limit by household size.
| Michigan Medicaid Income Limit Children |
| Children Medicaid Ages 0-1 |
| $59,398 |
How to Read the Michigan Medicaid Income Limits Charts Above
You cannot have an income higher than the Federal Poverty Level percentage described for your group to be eligible for Medicaid.
Similarly, when you identify the income group that applies to you, the income limit you see refers to the maximum level of income you can earn to qualify for benefits.
For example, if you are pregnant, to qualify for Medicaid, you cannot have an income higher than 195% of the Federal Poverty Level which for a family of two is $33,969 as shown in the chart above.
Read Also: Illinois Nursing Homes That Accept Medicaid
Home Care In Arkansas
Arkansas has a population of more than 3 million, with people aged 65 and over making up around 17.4% of that figure. The overall cost of living is lower than the national average, with housing costs significantly more affordable. Property taxes are also among the lowest in the country, making Arkansas a good retirement destination for low-income seniors who wish to age in place. The state has several high-performing hospitals, including Washington Regional Medical Center and UAMS Medical Center. In Arkansas, in-home care costs an average of $4,185 per month, and home health care costs $4,195.
This guide compares the costs of home care throughout Arkansas and details potential funding options. It also contains a list of low-cost resources and regulations for home care providers.
Income Thresholds For The Institutionalized
The 19 remaining States have elected an option that opens the door to Medicaid eligibility for many higher income persons in long-term institutional care without involving the State in the broader medically needy option, under which they would have to cover higher income persons in the community, including medically needy pregnant women and children. It also enables the six medically needy States not covering long-term institutional care for that population to nevertheless cover some higher income persons in institutions.
These States set a special eligibility threshold on income for persons in institutions that can be as high as 300 percent of SSI payment standards. In 1988, the maximum State threshold was $1,072, or three times the SSI level of $354 for an individual. Anyone with gross income over 300 percent of SSI or over the State-set ceiling is ineligible under this option, no matter how extensive their medical bills or how high the charges for nursing home care relative to their ability to pay.
Once they are determined to be eligible under this option, institutionalized recipients must use most of their to income to pay for their care. The amounts that they are expected to contribute are calculated under rules governing the post-eligibility process.
Also Check: Give Me The Number To Medicaid
