We Still Have Savings But Our Work Has Gone Away Is Medicaid An Option
Maybe. The answer varies by state. In general, a single person must have no more than $2,000 in cash assets to qualify. If youre over 65, the requirements are more complex. Whatever your age, there are strict rules about asset transfers. Medicaid may take into consideration any gifts or transfers of cash youve made recently.
What Medicaid Helps Pay For
If you have Medicare and qualify for full Medicaid coverage:
- Your state will pay your Medicare Part B monthly premiums.
- Depending on the level of Medicaid you qualify for, your state might pay for:
- Your share of Medicare costs, like deductibles, coinsurance, and copayments.
- Part A premiums, if you have to pay a premium for that coverage.
People Who Have Both Medicare & Medicaid
People who have both Medicare and full Medicaid coverage are dually eligible. Medicare pays first when youre a dual eligible and you get Medicare-covered services. Medicaid pays last, after Medicare and any other health insurance you have.
You can still pick how you want to get your Medicare coverage: Original Medicare or Medicare Advantage . Check your Medicare coverage options.
If you choose to join a Medicare Advantage Plan, there are special plans for dual eligibles that make it easier for you to get the services you need, include Medicare coverage , and may also cost less, like:
- Special Needs Plans
- Medicare-Medicaid Plans
- Program of All-Inclusive Care for the Elderly plans can help certain people get care outside of a nursing home
You May Like: Glasses Stores That Accept Medicaid
What Documents Are Required For A Medicaid Application
Medicaid applicants must prove that they have limited income and assets in order to be eligible for long-term care services. Before beginning the application process, it is helpful to understand what information you will be required to provide to prove your eligibility.
Medicaid is a state-run program, so the rules can vary from state to state, but in general applicants are not eligible for Medicaid benefits if the applicant’s income exceeds $2,523 a month . Applicants can also have no more than $2,000 in assets in most states.
Local Elder Law Attorneys in Your City
City, State
States require Medicaid applicants to provide the necessary information to prove that they are eligible for benefits. The burden of proof is on the Medicaid applicantnot on the state. In addition to needing to provide identifying information such as a birth certificate and proof of citizenship, following are some of the documents that you may have to provide to the Medicaid agency when you apply for benefits:
The state may use an electronic database to verify some of the information. Intentionally giving false information is a serious offense.
The state looks back five years to determine whether you transferred assets for less than market value within five years of applying for Medicaid. Applicants who gave away assets may be subject to a period of ineligibility.
Learn The Steps To Take If Your Medicaid Application Is Denied
Not everyone who applies for Medicaid can get coverage. After about 30 days of getting a Medicaid application, state officials will send a status. If the application for Medicaid benefits was denied, applicants can appeal the denial.
In some states, applicants who appeal a denial need to have a hearing to state their case. Each state has different rules for filing an appeal, but residents can read the letter of denial for instructions on how to appeal.
Don’t Miss: Pediatricians That Accept United Healthcare Medicaid
How To Apply For Or Renew Apple Health Coverage
Apply for or renew your Apple Health coverage online through Washington Healthplanfinder if you are:
- An adult age 18 to 64 years old.
- Applying for children.
- A parent or caretaker applying with children.
- Pregnant or applying for someone who is pregnant.
You have several options to apply for or renew coverage:
- Online: Go to Washington Healthplanfinder – select the “Apply Now” button.
- Mobile app: Download the WAPlanfinder app select sign in or create an account.
- Phone: Call the Washington Healthplanfinder Customer Support Center at 1-855-923-4633.
When youre ready to apply, youll need:
- Your household monthly income.
- Your immigration information, if that applies to you.
- Dates of birth for each member of your household.
- Social Security numbers for each household member who is applying for coverage and has a SSN. Some programs do not require a SSN. For more information visit our SSN eligibility webpage.
If youre accepted, you’ll receive a ProviderOne services card in about two weeks. Coverage will begin on the first day of the month in which the application was submitted. You’ll have the option to select a managed care plan online or you’ll be auto-enrolled into a plan.
If youre not eligible for Apple Health, you may qualify for help with your health insurance or for other health services. The Washington Healthplanfinder website or WAPlanfinder mobile app will help you with that.
What Income Level Must I Have To Qualify For Medicaid
The answer to this question isit depends on where you live.If your residential state expanded Medicaid during the Obama administration, you may qualify for Medicaid based on your income. If your Medicaid Office didnt expand its program, existing rules are used to determine your eligibility. Your family statuse.g. caring for a young child/children or pregnancy, annual income, family/household size, age, disability, and other criteria are considered.Each familys needs and situation differ. Complete a Medicaid application to learn if you qualify.
Don’t Miss: Washington State Medicaid Eligibility Seniors
Q How Long Will My Medicaid Benefits Remain Active
A. Medicaid is based on month to month eligibility. However, your benefits are redetermined on a yearly basis by DMMA to confirm whether you still remain eligible for the program you are receiving. Certain Medicaid programs require you to report changes in your situation within 10 days of the change. One example of a change that must be reported is new employment.
How Many People Are Enrolled In Medicaid And Chip
According to Medicaid.gov, more than 71 million people are enrolled in Medicaid and CHIP as of September 2017. About 68 million are Medicaid beneficiaries and about 6 million are CHIP beneficiaries:
- Sixteen million additional beneficiaries are enrolled in Medicaid and CHIP benefits .
- Child beneficiaries of the Medicaid program and beneficiaries enrolled in CHIP account for about half of Medicaid/CHIP programs total enrollment.
- The number of beneficiaries receiving Medicaid and CHIP changes from month to month. About 144,000 more beneficiaries were enrolled in August 2017 vs. September 2017.
Recommended Reading: Holistic Dentist That Accept Medicaid
Check The Status Of An Application
The Division of Family Resources provides tools to strengthen families through services that focus on prevention, early intervention, self-sufficiency, family support, and preservation.
You can check the status of your application online by clicking on your county of residence or by calling 1-800-403-0864. You will need to have your case number to check the status of your application.
Please remember that your application must be completed and all required documentation submitted before DFR can begin processing your application.
Pursuant to HIPAA and other applicable federal regulations, DFR is committed to respecting the privacy of each client. For that reason, DFR will not share or disclose information about your case without a signed release. You may download the DFR online.
Who Can Get Medicaid
- No matter your state, you may qualify for Medicaid based on your income, household size, disability, family status, and other factors. But if your state has expanded Medicaid coverage, you can qualify based on your income alone.
- Enter your household size and state. Well tell you who is eligible for Medicaid, if your state expanded and if you qualify for Medicaid based only on your income.
- If you think you have Medicaid eligibility, you can create an account and fill out a Marketplace application. If it looks like anyone in your household qualifies for Medicaid or CHIP, well send your information to your state agency. Theyll contact you about enrollment. You can apply any time of year.
- If you dont qualify for Medicaid, well tell you if you qualify for financial help to buy a Marketplace health plan instead.
Read Also: Medicaid Change Of Information Form
Renewing Your Medicaid Application
You must fill out a new Medicaid application every year to stay in the Medicaid program. The Medicaid application process may be easier each year. For example, if they already have your birth certificate on file, they may not ask for it again with your next application. However, information such as your income or alien status may change from year to year, so youâll be asked to provide an update every time you renew your Medicaid application.
Medicare information is everywhere. What is hard is knowing which information to trust. Because eHealthâs Medicare related content is compliant with CMS regulations, you can rest assured youâre getting accurate information so you can make the right decisions for your coverage.Read more to learn about our Compliance Program.
Nc Medicaid Managed Care

On July 1, 2021, most Medicaid beneficiaries began receiving the same Medicaid services in a new way called “NC Medicaid Managed Care.” Beneficiaries choose a health plan and get care through a health plan’s network of doctors. Some beneficiaries are remaining in traditional Medicaid, which is called NC Medicaid Direct. Learn more.
Note: Public charge rules that relate to determinations about certain legal resident statuses changed in March 2021. Immigrants should know that they and their families can access many public benefits without concern, if they are eligible, and are encouraged to get information about public charge rules in English or Spanish on the NC Justice Center website.
Read Also: Medicaid Indiana Provider Phone Number
Q Who Qualifies For Medicaid
A. Citizenship and Residency To obtain full Medicaid benefits in Delaware, you must be a Delaware resident and either a U.S. citizen or a legally residing noncitizen. Full coverage for noncitizens which include DACA recipients is dependent on the availability of state funding. However, noncitizens can qualify for coverage for emergencies and labor & delivery services if income requirements are met.
Income Level Qualifying for Medicaid is also based on need. Household income must be under certain limits as defined by the Federal Poverty Level and is based on family size. For Long Term Care programs, financial resources must also be under a certain amount. There are also specific programs for individuals who meet certain medical or disability tests, or who qualify due to age or pregnancy. To find out more about different Medicaid and other medical assistance programs, visit DMMA Programs & Services.
Read Also: Dentist In Columbus Ms That Accepts Medicaid
Missed The Apple Health Renewal Deadline
If you’ve missed the deadline to renew, but you would like to continue coverage, please contact us as soon as possible. If we find you eligible within 90 days after the date you lost coverage, we will cover you for the period you were without coverage.
The fastest way to renew your lost coverage is to go online. You may also call 1-855-923-4633.
Recommended Reading: Child Behavioral Therapist That Accept Medicaid
Person Who Is Aged Blind And/or Disabled
Apply if you are aged , blind, or disabled and have limited income and resources. Apply if you are terminally ill and want to get hospice services. Apply if you are aged, blind, or disabled live in a nursing home and have limited income and resources. Apply if you are aged, blind, or disabled and need nursing home care, but can stay at home with special community care services. Apply if you are eligible for Medicare and have limited income and resources.
What Are The State
Benefits for dual eligible beneficiaries candiffer based on your state of residence. Differences by state may include:
- Medicaid offered through Medicaid managed care plans
- fee-for-service Medicaid coverage
- plans that include all Medicare and Medicaid benefits
Income and resource standards are defined by federal law for full Medicaid and the Medicare Savings Programs. At their discretion, states can effectively raise the federally mandated limits.
Youre also considered a dual eligible beneficiary if youre enrolled in Medicare Part A or Part B and receiving cost-sharing through a Medicare savings program .
Below is table summarizing the benefits and eligibility criteria for each of the different MSPs in 2021:
| MSP | ||
|---|---|---|
| Specified Low-Income Medicare Beneficiary program | assists in the payment of Part B premiums | individual monthly income of $1,308 or less, individual resources limit of $7,970 married couple monthly income of $1,762 or less, married couple resources limit of $11,960 |
In addition to the Medicare savings programs, you also may be eligible for some of the following needs-based programs through Medicare:
- PACE : a Medicare-Medicaid joint program that provides medical and social services for people with significant needs who want to continue living at home
- Medicares Extra Help program: can help those with low incomes get the prescription drugs they need at reduced or no cost
Dual eligibility for Medicare and Medicaid means that youre enrolled in Medicare and either:
Recommended Reading: What Is Family Planning Medicaid Nc
Lawfully Residing Targeted Low
States have the option to provide CHIP and Medicaid coverage to children and pregnant women who are lawfully residing in the United States and are otherwise eligible for coverage, including those within their first five years of having certain legal status. If states do not adopt this option, federal law requires a 5-year waiting period before many legal immigrants are permitted to enroll in Medicaid and CHIP. Learn more about providing health coverage to lawfully residing children and pregnant women at 2107 of the Social Security Act, and in SHO# 10-006. A list of states providing Medicaid and CHIP coverage to lawfully residing children and/or pregnant women.
Also Check: Is There A Difference Between Medicaid And Medicare
How Do I Apply For Medicaid
Unlike traditional health insurance, which requires you to apply during a specified enrollment period, you can apply for Medicaid at any time. Apply on healthcare.gov or your state Medicaid website you dont need to wait for Open Enrollment or a Special Enrollment Period. You can get coverage this way during any time as long as you meet the eligibility requirements.
If you applied for Medicaid and got rejected, you can send in an appeal to the state Medicaid office. If you lose Medicaid coverage for any reason, then you will be given the opportunity to shop for a health plan on the Obamacare marketplace.
Learn about how to apply for Obamacare.
Ready to shop health insurance?
Read Also: Does Medicare Or Medicaid Cover Cremation
You May Like: Is Medicaid The Best Insurance
Does Every State Offer Expanded Medicaid
As of June 29, 2022, 36 states and Washington, D.C., have accepted federal funding to expand Medicaid under the ACA. Those that have not adopted the expansion measures are: North Carolina, South Carolina, Florida, Georgia, Alabama, Tennessee, Mississippi, Texas, Kansas, Wisconsin, South Dakota, and Wyoming.
Financial Documents And Resources
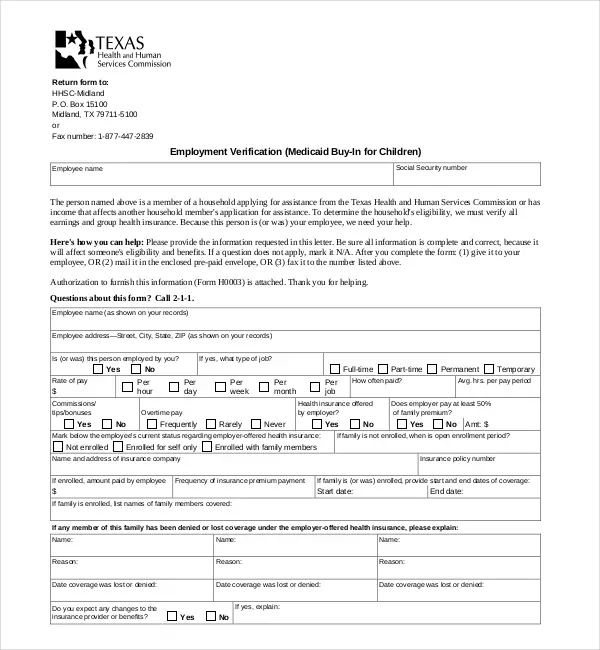

Provide checking and savings account statements, annuities, money market accounts, property deeds , Certificates of Deposit , retirement accounts , motor vehicle title/value , mortgage loan, stock or bond accounts, property proceeds, HUD-1, prepaid funeral contract, burial plot details, life insurance policies , or special needs trusts.
Recommended Reading: Department Of Human Services Nj Medicaid
What Information Is Not Required On The Medicaid Application
Adults older than 21 years of age will not need to put their parents information on their application as long as they are filing taxes separately. Partners who are not married and children of an unmarried partner can also be kept out of the application. However, keep in mind that household size is important when it comes to Medicaid income requirements.
In most cases, you dont need to sit down for an interview when you apply for Medicaid, but you may have to do an interview if youre applying for other programs at the same time.
Where Do You Sign Up For Medicaid
Some states let you apply to the U.S. Medicaid program online, by mail, over the phone and in person. Many states even let you apply for other types of benefits, like food stamps and TANF, using the same application.
Many states have a paper Medicaid application form that you can print online or have sent to you. You can also pick up an application in person at a human services office. You can also sign up for Medicaid by fax in most states.
In many states, the same office that runs Medicaid also runs other health benefits programs such as the Childrens Health Insurance Program . Also, some states may have different Medicaid applications for children, the elderly or people with a disability. Make sure youre uusing the right application for your situation.
Recommended Reading: Psychiatrist That Take Medicaid In Arkansas
Mental Health Support Opportunities
Beginning March 15, 2021, the Agency for Health Care Administration is pleased to provide a toll-free telephone helpline for immediate short-term mental health support and counseling services that will be in addition to the behavioral health services Medicaid recipients already receive. The helpline is available at no cost to eligible Medicaid recipients who are not currently in a managed care plan, ages 18 and over. Recipients may call 1.844.503.1140 for immediate help or to schedule a counseling session.
The Agency is making the new telephone helpline available 24 hours a day, 365 days a year.
- Short-Term Support: Includes an initial assessment and one to three telephone or virtual counseling services with follow-up as needed.
- Long-Term Care/Treatment: If the initial assessment indicates that a recipient is in need of long-term care/treatment, the recipient will be connected to appropriate resources such as a behavioral health Medicaid provider in the recipients community or another appropriate referral based on their need.
- Emergent/Urgent: If the initial assessment indicates an emergent potentially life-threatening situation is emerging, the recipient will be immediately connected to local emergency services. Until emergency services have arrived, the recipient will remain actively engaged with a KEPRO counselor on the line until services have arrived
