Other Financial Assistance Options For In
While the above programs help many people finance in-home care, they will not cover all costs for everyone. There are other ways to pay for in-home care, including out-of-pocket arrangements with siblings, annuities, reverse mortgages, private insurance and more. Read Caring.coms Guide to In-Home Care Costs to learn more about these alternative payment options.
Does Missouri Medicaid Cover Home Health Care
Missouri Medicaid, also known as MO HealthNet, does cover home health care of all kinds. Seniors and disabled individuals who are Missouri residents and who qualify for Medicaid in Missouri will be able to receive home health care that is covered by Missouri Medicaid. There are many ways to receive home health care, and the Consumer Directed Services program is becoming one of the most popular choices for Missouri residents.
The CDS program is a way for seniors and disabled individuals in Missouri to receive home health care from an individual of their choosing in the way that they indicate. Whereas other home health care providers do not allow the patient to choose the way in which they receive care , CDS lets the patient choose. In addition, family members of a patient are permitted to sign up as caregivers with the CDS program, meaning that the patient may receive care from a family member, and also that the family member may be reimbursed for their time that they spend caregiving.
In addition to home health care , Missouri Medicaid may also cover the following related expenses:
â Primary care physician services
â Disease testing and treatment
â Cost of certain medications
â Transportation to and from medical establishments
â Emergency room visits
â Cost of certain medical equipment and medical equipment repair services
Eligibility For Missouris Cds Program
Just because you are eligible for Medicaid in Missouri does not mean you are also eligible for CDS caregiving services. In order to take advantage of Missouriâs CDS program, you must also meet the following qualification:
– Be 18 years of age or older
– Be able to direct his or her own care
– Be physically disabled
– Be capable of living independently with the services of a personal care attendant
– Require at least a nursing facility level of care
Over 20% of people in the U.S. currently act as caregivers to an adult or child with special needs. Not only are many of them unpaid for this work, but 61% also have jobs outside of their caregiving duties. Consumer Directed Services allow this work to be compensated.
Don’t Miss: Department Of Social Services Medicaid
Medicaid Certified Home Care Agency In Missouri
There are certain regulations that need to be followed by homecare agencies that expect to file Medicaid claims in Missouri. Different states offer different criteria for Medicaid claims that should be followed by the agencies for ensuring eligibility for the claims. The information regarding the certifications and licensing is provided by the Bureau of Licensing and Certification or states Department of Human Services.
Governing Body: Missouri Medicaid
Home And Community Services

Most ill or disabled Missourians can remain in their own homes and avoid or delay institutionalization with the help of support services. Home and community-based services, administered by the Division of Senior and Disability Services , are available to eligible persons 60 or older and to adults with disabilities between the ages of 18 and 59.
DSDS administers two different programs, available in every county: in-home services and consumer-directed services.
In-home services are designed to assist in meeting the unmet needs of a person and provide necessary assistance for the person to remain in the least restrictive environment.
In general, IHS consists of personal care, nursing services, housekeeping, respite, and adult day care services.
Consumer-directed services , although similar in nature to in-home services, are provided to persons with a physical disability and do not include any task performed by a licensed professional. A participant of CDS must be able to direct the care planning process and hire an attendant. In general, CDS consists of personal care .
For information regarding eligibility criteria and funding sources for in-home services or consumer-directed services, contact DSDS at 866-835-3505.
For persons currently receiving services who want a change in care plan, contact the DSDS Regional Evaluation Team.
Don’t Miss: Does Doctors Care Accept Medicaid
What Are The Qualifications To Receive Cds
In Missouri, you must first be eligible for Medicaid to qualify for Consumer Directed Services. This program is administered by the Missouri Department of Social Servicesâ MO HealthNet Division.
If youâre not sure if you qualify for Medicaid or need help applying, you can contact the Family Support Division and they assist you with your application.
What Is A Cds Caregiver
In the state of Missouri, those who are eligible for Medicaid and who are disabled or too ill to care for themselves can also take advantage of a program called Consumer Directed Services.
This Medicaid-based program allows consumers to remain in their homes and communities instead of being moved to an institution. It does this by allowing a person of the clientâs choosing to receive compensation for providing essential support services. These caregivers can be an acquaintance or even certainly family members.
While many caregivers in the U.S. help their loved ones with daily tasks without pay, the CDS program lets some of them earn income for their services. In Missouri, the average pay rate is between $10 and $11 per hour for CDS caregiver pay.
However, itâs important to make sure to follow all Medicaid rules when a caregiver is hired as all states investigate potential incidents of Medicaid fraud.
Recommended Reading: Dentist That Accept Medicaid In Henderson Nv
To Qualify For Consumer
- Medicaid eligible
- 18 years of age or older
- Able to direct their own care
- Capable of living independently with the services of CDS
- Require at least a nursing facility level of care.
Individuals on Medicaid will need to meet Missouri Division of Senior and Disability Services requirements. DSDS will complete an assessment to determine the individuals personal care and home care needs (bathing, housekeeping, transportation, laundry and other needs. A personalized care plan will be forwarded to At Home Care CDS. Once a care plan is received, At Home Care CDS will help you hire the appropriate aide.
Medicaid Income Rules In Missouri
In Missouri, to qualify for Medicaid-paid nursing home care, known as “vendor coverage,” all of a single applicant’s income must go towards the cost of care. For an eligible individual, MO HealthNet would pay the cost of skilled nursing or intermediate care in excess of the person’s income. Note that these LTC income rules may be different from the income limits for those applying for other health care benefits from Medicaid. For example, applicants for HCBS Medicaid waiver programs, discussed below, must meet a 2020 monthly income limit of $1,370.
For purposes of determining Medicaid LTC eligibility, any income an applicant receives, from any source, is considered. However, when only one spouse of a married couple applies for Medicaid, the income of the non-applicant spouse is not counted, so that he or she has enough funds on which to live. Additionally, the non-applicant spouse is entitled to keep a minimum monthly needs allowance, which may range from $2,113.75 to $3,216.
If you qualify for Medicaid and live in a nursing home, you will be expected to spend almost all income on your care. MO HealthNet allows nursing home residents receiving Medicaid to keep only $50 per month as a personal needs allowance.
Don’t Miss: Dentist That Accept Medicare Medicaid
Medicaid Coverage For Nursing Homes
If you are age 65 or older, blind, or disabled and meet income and resource requirements, MO HealthNet provides coverage for nursing home residents under certain circumstances.
To obtain coverage for nursing home care, you must be financially eligible, and you must need the kind of care nursing homes provide. Nursing homes provide 24-hour supervised nursing care, personal care, therapy, nutrition management, organized activities, and other services.
For more information, visit Missouri’s MO HealthNet for Seniors page or call 373-4636. You can also access an MO HealthNet application form here.
Before you apply for Medicaid coverage, make sure that to the best of your knowledge you meet the eligibility criteria. Typically, your nursing care facility can assist you with the Medicaid application process. For other questions about MO HealthNet and nursing home coverage, call the Missouri DSS at 735-2966. You can also click here to identify and contact your local Family Support Division resource center.
Does Medicaid Pay For Home Caregivers Or Assisted Living Care
One of the questions that Im sometimes asked is whether Medicaid pays for home caregivers or assisted living care. As to homecare, let me first distinguish Medicaid from Medicare. Medicare pays for skilled care, which can include home visits by physical, occupational, speech therapists or other skilled nursing care. Medicare does not pay for custodial care. As to Medicaid, in Illinois no, it does not pay for home care. In Missouri it can, but only if the person is certified to have such a high level of need that they would qualify to be in a nursing home. As to Assisted Living Care, in Missouri no Medicaid doesnt pay for it. In Illinois, there are a limited number of assisted livings, known as supportive living facilities that are certified Medicaid providers. We can help you to find one in your area.
Read Also: Wellcare Of Ky Medicaid Phone Number
How Integrity Home Care + Hospice Can Help
Integrity is a CDS agency, and an FMS Vendor. What that means for you is that Integrity will act as a fiscal manager, processing payroll and taxes for your attendants, as well as performing background checks and providing advocacy and case management support.
Q: Who qualifies for CDS?A: Anyone with active Missouri Medicaid, who is 18+ years old, has a physical disability that restricts their ability to care for themselves, has the ability and desire to self-direct their own care and supervise an attendant, and meets level of need as determined by DHSS assessment.
Q: Who can be an attendant for a CDS recipient?A: Anyone the participant chooses who is 18+ with a clear background screening, including friends and family .
How To Know If Youre Eligible For Medicaid In Missouri
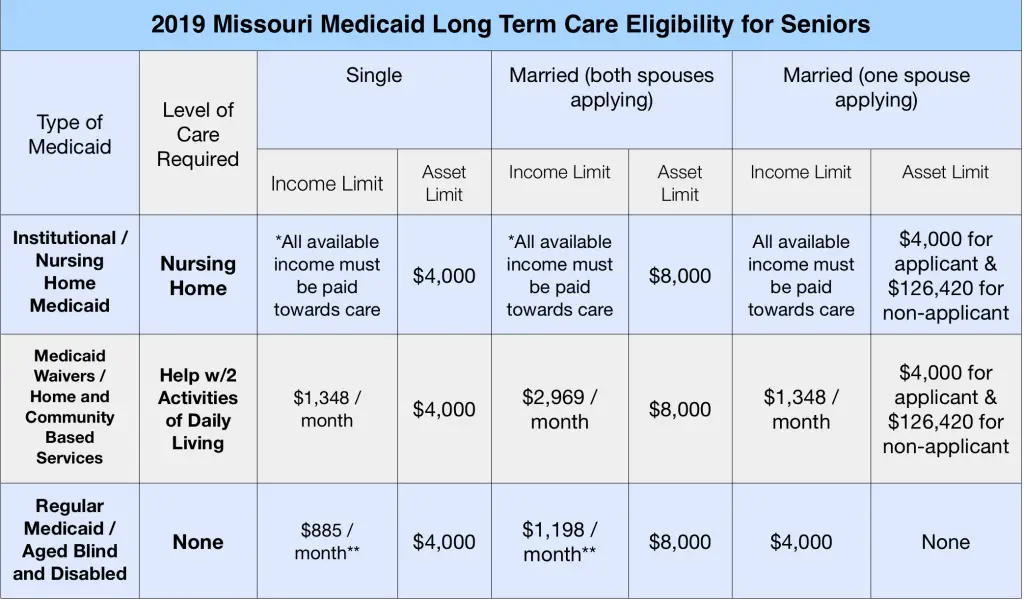
Medicaid is a group of programs available to various individuals based on their medical and financial needs, so it may be difficult to determine which programs you qualify for without applying. To receive regular Medicaid for the aged, blind or disabled in Missouri, your monthly income cant exceed $963 if youre applying individually or $1,297 if youre applying as a couple. Assets are limited to $5,035 per person. Income limits are slightly higher for applicants who are blind and for certain programs that require a nursing home level of care.
2022 Medicaid Income Limits for Seniors in Missouri
As part of the Medicaid application process, you may be asked to prove your:
- Age and disability
- The clinical need for long-term care for some programs
- Financial need for assistance
Don’t Miss: How Do You Know What Medicaid Plan You Have
How To Find An In
Whether you are looking for yourself or a loved one, finding a quality home care provider can be a stressful process. When you hire an in-home care aide youre placing a lot of trust in the hands of the person by inviting them into your home, so youll want to be diligent in your search. At Caring.com, were here to help weve created a helpful checklist below that can help guide you through the process of both determining your needs and finding a home care agency that will provide the best care possible.
How Does Cds Work
Consumer Directed Services allows you to direct your own care. You assume the role of employer and are responsible for recruiting, selecting, training, managing and terminating your attendants. These caregivers may be anyone other than a spouse, including friends and family who have stepped into the role of caregiver.
Read Also: Birthing Centers That Accept Medicaid
Quality Health Coverage For Missouri Families
Exciting News for Home State Health Plan Members! Home State Health Plan is making it easy for you to manage your health care. You can now log on to a safe and secure Member Health Site that will allow you to better access to health management information. You can use the new website to:
- Change Primary Care Providers
- Order new Member ID cards
- Keep track of your health plan benefits
- Update mailing addresses and phone numbers
- View Provider Claim Information
- Reach out to your health plan representative
To visit our new Member Health Site, just click the Log In tab at the top of the home page. All you need to do is register and log in. Its easy and its secure. If you need more information about the new Home State Member Health Site, please call us at .
Home State Health gives you access to the care you need to keep your family healthy. MO HealthNet Managed Care benefits cover pregnant women and newborns, children and adults. Home State Health provides a wide range of healthcare services. We want you to receive the personal attention you deserve. Learn about your healthcare benefits, log in to manage your care, and learn more about staying healthy.
Missouris Division Of Senior And Disability Services
In Missouri, home-based care services are run through the stateâs Division of Senior and Disability Services . They make sure Medicaid-eligible people get the care they need. These people include:
– People who are over 60
– Adults with disabilities between the ages of 18 and 59
Missouriâs Medicaid program was expanded on October 1, 2021 to include adults ages 19-64 who are not disabled but who meet certain income qualifications. However, access to the CDS program is still limited for this group, so you will need to double check your eligibility.
The state of Missouriâs Medicaid system can be confusing because the DSDS runs two similar programs: In-home services and consumer-directed services . These two programs provide slightly different services, so itâs important to talk to someone about the program you are eligible for.
– In-home services are available to people with a physical disability and do not include coverage for tasks performed by licensed medical professionals.
– Consumer Directed Services allows people who are able to understand and direct their own care to hire an attendant to help them do daily tasks.
For information regarding eligibility criteria for both in-home services or consumer-directed services, contact DSDS at 866-835-3505.
Recommended Reading: Can You Have Both Medicare And Medicaid
Find Home Care Agencies Near You
To find quality home care providers near you, simply input the zip code or city where you would like to start your search. We have an extensive directory of home care agencies all across the nation that includes in-depth information about each provider and hundreds of thousands of reviews from seniors and their loved ones.
Driving Better Home Care For Missouri Medicaid Patients During Covid
When the citizens of Missouri voted to expand Medicaid coverage in August of 2020, they envisioned expanded access to insurance for 230,000 citizens who would not qualify under the existing income requirements. The Missouri Medicaid program, MO HealthNet, offers coverage for medical, dental and vision care, as well as other services for children, low income individuals and families, the blind and the disabled.
For these individuals, the new coverage will provide an important safety net, which is crucial with the pandemic affecting access to safe medical care amidst rising unemployment. For elderly and disabled individuals at risk of needing nursing home care, this expansion includes valuable options for in-home care that can help them stay healthier while avoiding COVID-19 exposure.
With as many as 40% of U.S. COVID-19 deaths potentially linked to nursing home-acquired infections, avoiding nursing home admissions wherever possible is critical for health care providers working with disabled and elderly patients. Avoiding long-term care has been a goal for health care professionals as evidence shows that the right in-home services can keep patients healthier and happier longer, and at a lower cost to insurers, both public and private. But for many Missouri families, this care was not financially possible to provide, or desirable, without the Medicaid expansion and before the COVID-19 pandemic.
Also Check: What Does Medicaid Cover In California
We Deliver Medicaid Services Throughout The St Louis Metro
The Medicaid program for the state of Missouri is called MO-Health Net. The purpose of the MO-Health Net Division is to purchase and monitor health care services for low income and vulnerable Citizens of the State of Missouri.
Algonquin Nurses Home Health Care I , LLC delivers care throughout the metro area under this program. Our clients receive care as authorized by the Department of Health and Senior Services and Division of Senior and Disability Services.
Algonquin Nurses provides services for Medicaid Title 19 clients, Medicaid Waiver and Specialty Programs designed according to the needs of the client. This would include Home and Community Based Services , Consumer Directed Services , Aids/HIV Waiver Services, and Healthy Child and Youth .
Algonquin Nurses also provides services through the VA Attendant and Home- Chore Program with the Veterans Administration however this is not Medicaid authorized.
Our staff in the Medicaid Division of Algonquin Nurses is State Medicaid Certified and trained. They believe and respect the rights of individuals to have a choice in their own decision to live independently and freely. Our Administrative and support staff who work directly with our clients are dedicated to serve the elderly, disabled, children youth, low income and VA consistently in their homes and communities.
Our Medicaid Division Staff, provide services all of:
- St. Louis County and City
- St. Charles County
