Determine How You Will Submit Claims To Emedny
Providers are given several options for submitting claims to eMedNY
Option 1: HIPAA Compliant Claim Formats Submitted Directly to eMedNY
Option 2: Medicaid’s Electronic Provider Assisted Claim Entry System web-based application
- Claims: Professional Institutional and Dental
- Claim Status Requests**
- Prior Approval Requests
- Eligibility Verification
*Real-time means that the claims are processed instantaneously and the provider can view the status of a real-time claim within seconds. There is no need to wait for a remittance statement to be mailed to find out about the status of submitted claims. **The status of claims submitted via the ePACES batch feature is generally available within 24 hours. To enroll in ePACES:
Option 3 Paper Claim Forms
Provider Electronic Transmitter Identification Number Application
Page 3:
Mail the Original completed application to:Computer Sciences CorporationPO Box 4614Rensselaer, NY 12144-8614
***Upon receipt of Submitter ID, Please call NY Medicaid at 1-800-343-9000 option 2 to request a FTP Logon User ID and Password***
- Enter your Billing Agency’s Name, Addres, Phone and Fax numbers
- Enter the Adminstrator and Contact information
- Sign and Date
Page 3:
- If you are using this form to obtain an ETIN, leave blank. If you wish to add a provider ID number to an existing ETIN, indicate the ETIN in the top left corner of the form
- Enter the name of the Billing Service
- Enter the Date
- Enter Provider Name, NPI, and Medicaid Provider ID number
- Provider must sign and date this form and enter their contact information
- This must be signed by a Notary Public
- Please enter the Provider/Business or Billing Service Name as the “Trading Partner”
- Please enter your name, title, and sign
Notification Of Determination By Nys Doh
A written determination of approval or denial of the submitted application will be sent to the provider.
If the application is approved, a letter containing the provider’s MMIS ID Number, the effective date when services may be provided to an enrolled client, and other information related to their enrollment will be sent to the enrollee.
Recommended Reading: Does Medicaid Cover Gastric Bypass In Michigan
Medicaid Enrollment Requirements And Compliance Deadlines For Managed Care Providers
Federal and state laws require all Medicaid Managed Care network furnishing , ordering, prescribing, referring and/or attending providers to be enrolled with the New York State Medicaid program. For more information, see the January 2018 issue of the Medicaid Update article titled Medicaid Managed Care and Children’s Health Insurance Program Network Providers Must Enroll in the New York State Medicaid Program.
Beginning, , EmblemHealth will deny claims from non-enrolled providers. You must be enrolled either as a fee-for-service billing provider or as an OPRA provider to continue receiving payment for services provided to EmblemHealth Medicaid members.
Enrollment of Physicians, Nurse Practitioners, Physician Assistants, Podiatrists, Dentists, Optometrists, Audiologists, and Certified Nurse Midwives
- Providers and practitioners who wish to receive payment for covered NYS Medicaid services should apply as an Individual Billing Medicaid. Information regarding how to enroll is available on the eMedNY Provider Enrollment & Maintenance web page.
- Providers who only wish to enroll as a non-billing provider may alternatively enroll as an OPRA provider on the eMedNY Provider Enrollment & Maintenance web page.
- Exceptions to the prescriber enrollment requirements for certain authorized prescribers are outlined in the March 2021 issue of the Medicaid Update article titled Pharmacy Billing Guidance Exceptions for Non-Enrolled Prescribers.
Pharmacy Enrollment
| Provider Type |
|---|
Setting Up Remittance Advice Receipt And Payment Options
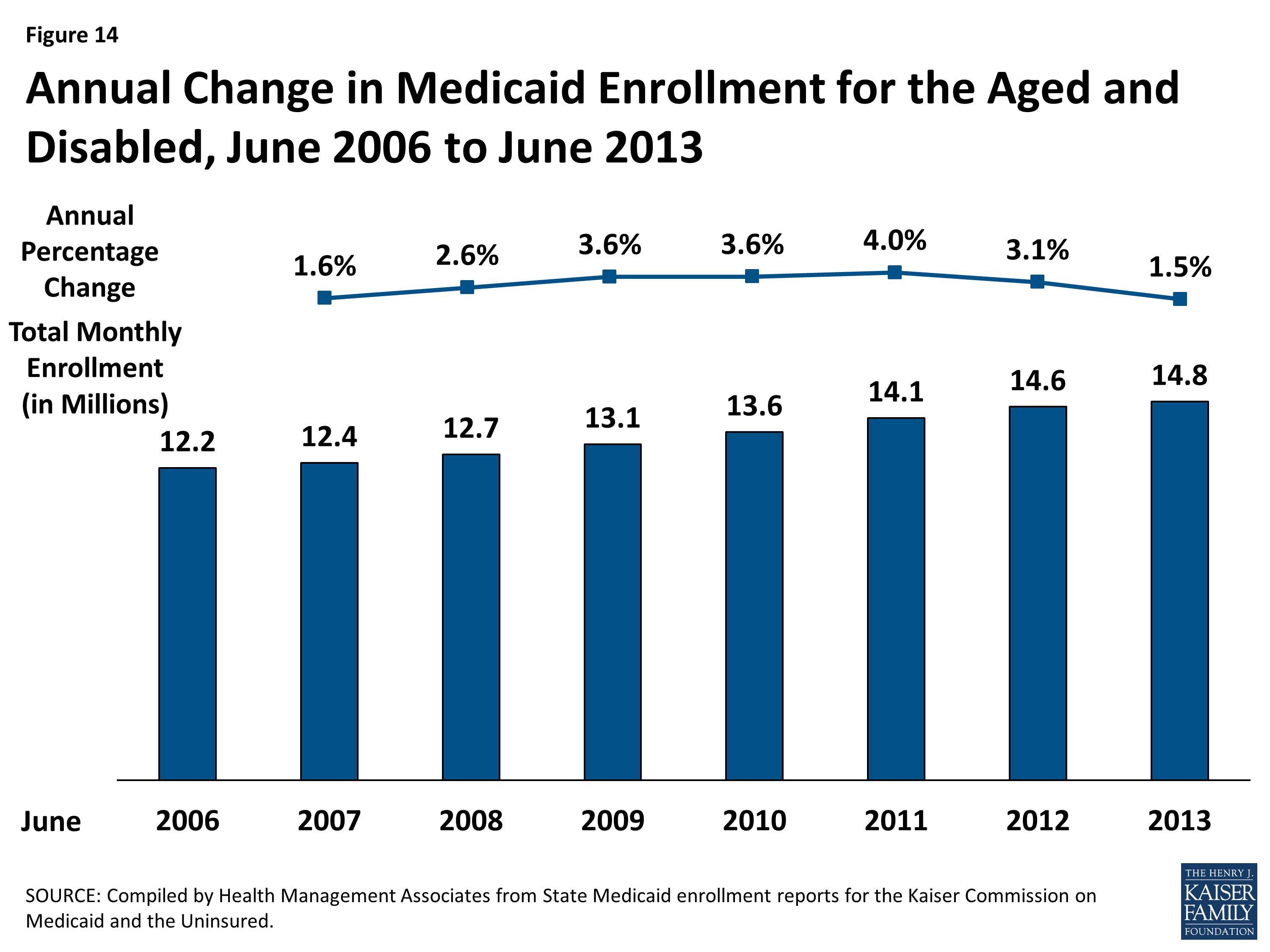
The processing of most Medicaid transactions is performed by the eMedNY fiscal agent for the NYS Medicaid Program. eMedNY processes transactions 24 hours a day, 7 days a week and issues checks and remittance statements weekly, for processed claims.
Remittance Advices are generated every week for claims submitted from Thursday to Wednesday prior, and are available in multiple formats.
- Electronic Electronic remittances are issued in a HIPAA-compliant format known as the 835 or 820 therefore software is required to interpret the remittance information.
- PDF Remittance AdvicePDF version of the paper remittance is viewed with Adobe Reader® which is available free of charge. This Remittance Advice format may be downloaded and stored electronically. Additionally, it is not held with any corresponding paper Medicaid check for two weeks but released to you two weeks earlier. In order to receive the New York Medicaid paper remittance advice in a PDF format through eMedNY eXchange,
- Paper Medicaid checks and paper remittances are held for two weeks and two days before being issued to the provider.
ENQUIRIES: Questions should be directed to the eMedNY Call Center at 1-800-343-9000. Before submitting claims, providers may also phone the Call Center to request training from a eMedNY Regional Representative.
Read Also: I Am Pregnant And Need To Apply For Medicaid
Waiting For A Response
Once the complete provider enrollment packet has been received, the documents will be processed. Processing will take approximately two weeks from the date of receipt. After processing, a confirmation will be faxed to you as notification to begin filing claims electronically. If neither confirmation nor a returned packet is received after two weeks, contact the EMedNY EDI Technology Support Center at 1-800-343-9000 option 2.Please be advised, ERA Request forms are processed Every Thursday at EMedNY.
Medicaid Provider Enrollment Requirements By State
The following information includes state-specific provider enrollment requirements for states where BCBS Plans offer Medicaid products. Please refer to the table below for state-specific Medicaid provider enrollment requirements if your claim has been denied and you have received notice from a BCBS Plan that the state where the member is enrolled in Medicaid requires that providers enroll in that states Medicaid program before the BCBS Plan can issue payment.
Products and services are provided by Horizon Blue Cross Blue Shield of New Jersey, Horizon Insurance Company, Horizon Healthcare of New Jersey, and/or Horizon Healthcare Dental, Inc., each an independent licensee of the Blue Cross Blue Shield Association. Communications may be issued by Horizon Blue Cross Blue Shield of New Jersey in its capacity as administrator of programs and provider relations for all its companies. The Blue Cross® and Blue Shield® names and symbols are registered marks of the Blue Cross Blue Shield Association. The Horizon® name and symbols are registered marks of Horizon Blue Cross Blue Shield of New Jersey.
Read Also: South Carolina Medicaid Long Term Care
Provider Business Module Management
Responsible for the business of provider enrollment. Staff will design, develop, and implement solutions for provider regulation compliance through close coordination with the Centers for Medicare and Medicaid Services, the Office of the Inspector General, and Medicaid Program Integrity, and other states’ Medicaid programs coordinate with internal and external partners in support of the Medicaid Enterprise System and operational processes participate in development and implementation of system enhancements through close working relationship with the fiscal agent represent the Agency on national meetings and work groups related to provider screening develop operational process standards through process mapping develop reporting mechanisms to manage Provider Enrollment Unit workloads and data anomalies document regulatory requirements and proof of compliance provide transparency to Provider Enrollment Unit activities assist Medicaid Policy and Publication Units with maintenance of provider guides, training materials, and rule documents and design, develop, and implement fiscal agent monitoring processes and reporting mechanisms in support of contract enforcement, including the use of CAPs and sanctions to enforce compliance.
Unitedhealthcare Senior Care Options Plan
UnitedHealthcare SCO is a Coordinated Care plan with a Medicare contract and a contract with the Commonwealth of Massachusetts Medicaid program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is a voluntary program that is available to anyone 65 and older who qualifies for MassHealth Standard and Original Medicare. If you have MassHealth Standard, but you do not qualify for Original Medicare, you may still be eligible to enroll in our MassHealth Senior Care Option plan and receive all of your MassHealth benefits through our SCO program.
Recommended Reading: Does Medicaid Cover Dental For Kids
Section 1135 Waiver Flexibilities
Department of Health & Human ServicesCenters for Medicare & Medicaid Services7500 Security Boulevard, Mail Stop S2-26-12Baltimore, Maryland 21244-1850
New York State Department of HealthEmpire Plaza
Re: Section 1135 Flexibilities Requested in March 23, 2020 Communication
Dear Commissioner Zucker:
Your communication to CMS on March 23, 2020, detai1ed a number of federal Medicaid, and Medicare requirements that pose issues or challenges for the health care delivery system in all counties in New York and requested a waiver or modification of those requirements. Attached, please find a response to your requests for waivers or modifications, pursuant to section 1135 of the Social Security Act, to address the challenges posed by COVID-19. This approval addresses those requests related to Medicaid and Medicare.
To streamline the section 1135 waiver request and approval process, CMS has issued a number of blanket waivers for many Medicare provisions, which primarily affect requirements for individual facilities, such as hospitals, long term care facilities, home health agencies, and so on. Waiver or modification of these provisions does not require individualized approval, and, therefore, these authorities are not addressed in this letter. Please refer to the current blanket waiver issued by CMS.
Sincerely,
APPROVAL OF FEDERAL SECTION 1135 WAIVER REQUESTS
CMS Response: March 26, 2020
State Fair Hearing Requests and Appeal Timelines
Provider Enrollment
Medicaid Enrolled Provider Listing
This is a list of active Medicaid fee-for-service , Managed Care Only and Ordering, Prescribing, Referring, Attending providers. Data elements include the providers Medicaid Provider ID, NPI, provider or facility name, Medicaid type, profession or service, provider specialty, service address, city, state, zip code, county, telephone number, latitude, longitude, enrollment begin date, next anticipated revalidation date, date the file was extracted from the data warehouse and a Medically Fragile Children and Adults Directory Indicator.
Tags: consumer resources, community health and chronic disease, strategic initiatives, mmis, npi, medicaid, managed care, mmc, provider enrollment, 21st century cures act, emedny, part 438, childrens health insurance, fee-for-service, ffs, opra
This dataset has the following 19 columns:
| Column Name |
|---|
Also Check: Does Medicaid Give You A Free Breast Pump
What Do I Need To Apply
The necessary documentation needed to apply for Medicaid also depends on your category, specifically whether you fall under the Modified Adjusted Gross Income or non-MAGI guidelines. These guidelines are defined in the section below.
MAGI eligibility groups include:
- Pregnant women
- Infants and children under 19 years of age
- Childless adults who are not pregnant, 19-64 years of age, not on Medicare, and could be certified disabled but not on Medicare
- Parents/caretaker relatives
- Family Planning Benefit Program and/or
- Children in foster care
Non – MAGI Eligibility Groups include:
- Individuals 65 years of age or older, who are not a parent or caretaker relative,
- individuals who are blind or disabled who do not meet the criteria of any of the MAGI eligibility groups
- Residents of Adult Home run by LDSS, OMH Residential Care Centers/Community Residences
- Individuals eligible for the following programs:
- COBRA
- AIDS Health Insurance Program
- Medicaid Buy-in Program for Working People with Disabilities
- Medicaid Cancer Treatment Program
Application for Non-MAGI
The following paper application may only be printed and completed if you are applying at an LDSS for Medicaid because you are over 65 years of age or an individual in your household is deemed certified blind or disabled, or you are applying for Medicaid with a spenddown.
English, Spanish, Chinese, Haitian Creole, Italian, Korean, Russian
Providing A Medical Home For Clients
Providers are the crucial players in any quality health-care program. Providers enrolled with Texas Medicaid and other health-care programs render essential medical and preventive health-care services to clients while focusing on providing the best medical care possible. Texas Medicaid providers help ensure that each patient can receive high quality, comprehensive health-care services within their community.
Learn More About Texas State Health-Care Programs
Recommended Reading: Ny Medicaid Provider Enrollment Form For Groups
Unitedhealthcare Community Plan How To Enroll
After December 31, 2013, you can no longer apply for Family Health Plus. If you think you may qualify, you can apply on the New York State of Health website, or by calling .
You may be eligible to join if you live in any of the following counties: Albany, Bronx, Broome, Cayuga, Chautauqua, Chemung, Chenango, Clinton, Columbia, Dutchess, Erie, Essex, Franklin, Fulton, Genesee, Greene, Herkimer, Jefferson, Kings, Lewis, Livingston, Madison, Monroe, Nassau, New York, Niagara, Oneida, Onondaga, Ontario, Orange, Orleans, Oswego, Queens, Rensselaer, Richmond, Rockland, Schenectady, Seneca, St. Lawrence, Suffolk, Tioga, Ulster, Warren, Wayne, Westchester, Wyoming, and Yates..UnitedHealthcare Community Plan has Certified Application Counselors in your neighborhood to help you complete your application on the New York State of Health website. Just call and a representative will call you to schedule an appointment.
UnitedHealthcare Community Plan has Certified Application Counselors in your neighborhood to help you complete your application on the New York State of Health website. Just call and a representative will call you to schedule an appointment.
For more information on Medicaid and Child Health Plus, call New York Health Options at . For more information on Medicaid Managed Care, call New York Medicaid Choice at .
Updating Medicaid Provider File
Pursuant to Part 810 of OASAS regulations providers are required to obtain prior OASAS approval for certain changes in their operating status in order to maintain their operating certificates and Medicaid provider status in good-standing. Such changes, which must also be reported to DOH may include but are not limited to, changes in certified site locations, establishment of additional service locations and changes in ownership. Billing Medicaid for services provided at sites not currently certified by OASAS can result in Medicaid audit disallowances.
If a provider has given OASAS prior notification and received approval for changes to their operating certificate, as required by OASAS regulations, OASAS will provide DOH and the provider with the necessary written correspondence to update the Medicaid file. The DOH will send the provider confirmation of changes made to the Medicaid provider file.
Read Also: Does Medicaid Cover A Breast Reduction
Promoting Continuity Of Care
When families are faced with unemployment or loss of employer-based health coverage, they turn to Texas Medicaid or another health-care program to provide the health care they and their loved ones need. Providers who enroll as Texas Medicaid and other state health-care programs providers can continue to see existing patients during those times of change.
Providers may also render service to families with mixed coverage .
Unitedhealthcare Dual Complete Plans
Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
You May Like: How To Apply For Medicaid In Md
Learn Medicaid Billing Policies And Procedures
Before rendering service to a client, providers need to become familiar with the policies and procedures of the Medicaid Program.
- Begin with Information for All Providers:
- Select the Provider Manual for your type from the Provider Manuals Page. Each manual contains :
- Policy Documents
- Institutional or Practititioner Billing Guidelines
- Provider-specific Billing Guidelines
Required Documents For Those Applying For New Submitter Ids
The following documents are required enrollment documents that must be completed, signed and returned to the EMedNY office prior to initiation of electronic claims submission or inquiry.Note: You may be required to use Internet Explorer to open the links listed below.
If the links listed above do not work properly, please download these forms from:www.emedny.org
If you have any questions regarding any of the documents in this package, please phone the EMedNY EDI Technology Support Center at 1-800-343-9000 option 2.
We can now process 276/277 requests . If this is a transaction you would like to utilize please make sure to enroll with the payer.
| Vendor Name – AXIOM Systems, Inc. |
| Contact – EDI Team |
| Address – 241 East 4th Street, Suite 200Frederick, MD 21701 |
You May Like: How To Renew Medicaid Benefits
Healthcare Legal Alert: Expedited Medicaid Provider Enrollment Options In Response To Coronavirus Public Health Emergency
On April 20, 2020, the New York State Department of Healths Bureau of Medicaid Provider Enrollment announced that expedited enrollment options including online enrollment are now available for temporarily enrolling providers who are responding to the coronavirus public health emergency. In addition to the expedited enrollment process, New York Medicaid is waiving application fees and the site visit and fingerprint-based criminal background check screening requirements for these applicants.
There are, however, limitations as to which providers may use the new expedited Provisional Temporary Provider Enrollment application process and the duration of such enrollment status.
Expedited enrollment is available only for nurses , nurse practitioners, physicians and registered physician assistants who are not currently enrolled in New York Medicaid and who do not have a New York Medicaid enrollment application pending. Also, to be eligible, a provider must be enrolled in Medicare or another states Medicaid program or, alternatively, must not be currently excluded from New York State Medicaid, cannot appear on the Office of Inspector General Exclusions Database, and must be licensed and legally authorized in at least one state or United States territory to practice or deliver the service for which they file professional services claims.
The PTPE application requires the following data elements:
Expedited Submission of PTPE Applications
Option 1 Online Form:
Option 2 Email:
