Therapies Covered By Class
For me as a parent, CLASS has covered all the therapy servicesand Im not talking about things like speech therapy, occupational therapy or physical therapy. I mean things like horseback riding, music therapy, aquatic therapy, recreational therapy, and other types of programs. It also pays for respite and attendant care. This is a waiver Im very familiar with, so if you have any questions please let me know.
Get A Medicaid Waiver For Kids With Special Needs
A guest post by Natasha Cornin
It has been a little more than a year since the start of my journey to obtain a Medicaid waiver for my six-year-old son with autism, but I am relieved to say I finally walked through the Front Door and obtained a Medicaid Service Coordinator for my son another step toward accessing additional therapy, family reimbursement and more.
Access to the services offered through a Medicaid Waiver is managed by the state department of the Office for People with Developmental Disabilities . Once your child is deemed eligible for the Waiver, youll enter the second phase to obtain services through OPWDD. As an ASD mom who felt overwhelmed and frustrated through the lengthy process to access Waiver services, it is my sincere hope that this post provides some valuable guidance on the process and what to expect in order to make the next parents journey easier and less stressful. Just be aware, there may be some variations in your city/state. This is my experience with my states procedures.
Step 1
Contact an information and referral service to schedule a neuropsychological, psychosocial and family history evaluation. I went with YAI/LINK since weve always received services through YAI and they have been professional and compassionate.
Step 2
Go through the evaluation process to determine whether your child meets the eligibility requirement to access additional services and support through the Waiver/OPWDD.
Step 3
Step 4
Step 5
Children’s Benefits From The Affordable Care Act
A few provisions in the Affordable Care Act benefit Children with Special Health Care Needs. Most importantly, the ACA raised the Medicaid eligibility level for most individuals to 133% FPL. In many states, that means that children who were in CHIP programs were able to enroll in Medicaid programs instead, and gained access to more benefits like EPSDT services. In addition, because of the ACA, children who age out of the foster care system are now able to keep their Medicaid coverage until they turn 26.
The ACA also offers increased federal funding to states to encourage the development of programs that might help CSHCN. For example, states can opt to create a system of “health homes” to coordinate care so that people with chronic conditions can receive comprehensive, wraparound case management services. CSHCN are likely to benefit in states that choose to offer the health home option because they will be able to get better access and organize all of their care needs.
Recommended Reading: Pueblo Dentists That Take Medicaid
Medicaid And Special Needs
Medicaid, jointly funded by the federal government and individual states, is arguably the most important public benefit available to individuals with disabilities. While eligibility guidelines, services and payment rates vary widely, the federal government requires that all state Medicaid programs pay for physician visits, prescriptions, hospitalization, lab work, x-rays and nursing home care. In addition, all states must provide periodic health screenings and treatment to Medicaid-covered children under the age of six.
Although Medicaid is available only to those having limited income and assets, once an individual with disabilities reaches the age of 18, family assets are no longer considered, making it an important consideration in all special needs estate planning.
In addition, most states have established Medicaid waiver programs with less stringent income/asset requirements. The most common of these are intended to support the needs of individuals with severe disabilities who are eligible for long-term, institutionalized care, but whose families prefer that they remain in a community setting. Typical services include home aides, day habilitation, family respite and therapeutic services. Some states will cover expenses for individuals to live in small, community-based group homes.
Other Public And Private Transportation
If you want to introduce your child to a little more independence, you might have to pay for it, but there are accessible choices. Most city buses, for example, come fully equipped with a wheelchair lift and special seating for people with disabilities or special health care needs. In some cities, your family can use a regular city bus, taxi, or a light rail. Fares for these types of transportation are sometimes reduced for children and adults with disabilities or special health care needs. Its a good idea to call the public transportation agency in your area or visit their website to check and see what they have. Find it using this Texas Department of Transportations public transportation locator. They might ask for proof of your childs disability or special health care needs to approve a reduced fare card.
Many school districts and the Texas Department of Aging and Rehabilitative Services also have hands-on training for older children to learn how to use the bus system or learn about public transportation in their community. Some community programs might help your child learn to drive and get their drivers license if they are able. These are all ways your child can feel more independent. Our Grants and Other Funding Sources page also lists some private programs you can apply for to help you make special out-of-town trips for medical care.
You May Like: Fidelis Care Medicaid Phone Number
How Does Having A Child With Special Health Care Needs Affect Families
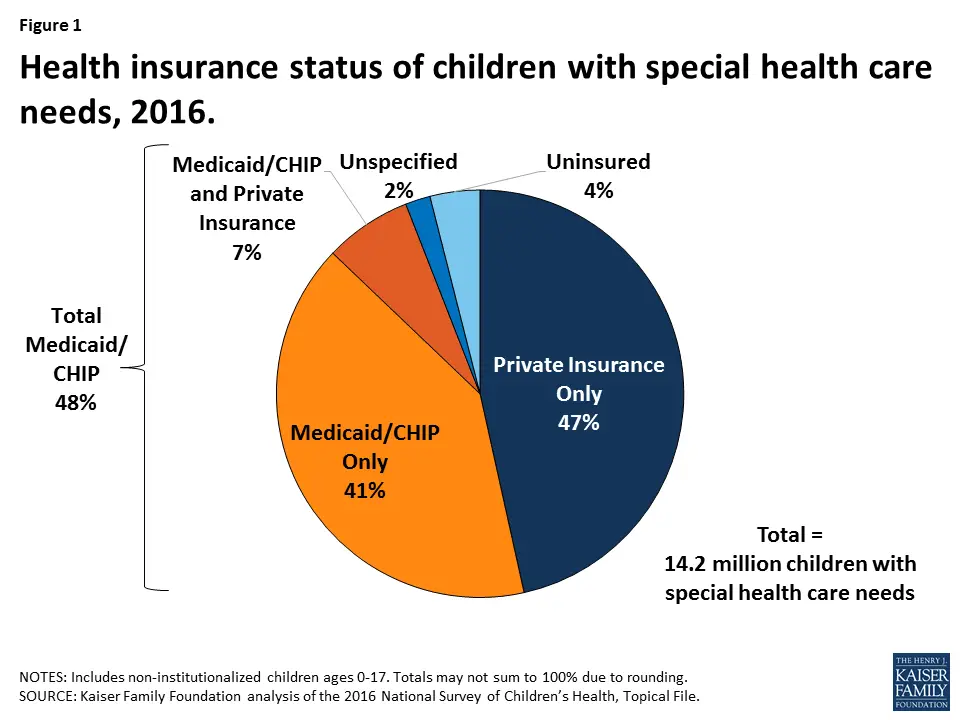
Medicaid/CHIP children with special health care needs find their health care more affordable than those with private insurance only. Medicaid/CHIP-only children with special health care needs are more than four times as likely to report that their out-of-pocket health care costs are always reasonable compared to those with private insurance alone . Only 3% of Medicaid/CHIP-only children with special health care needs reported paying $1000 or more in out-of-pocket medical expenses compared to 38% of those with private insurance alone . Medicaid program rules entirely exempt certain populations and services from premiums and copays and otherwise require cost-sharing to be nominal. This reflects the fact that the Medicaid population tends to have low incomes and, as in the case of children with special health care needs, may have multiple and ongoing service needs which could lead to high costs without cost-sharing protections.
What Does Medicaid Cover
Medicaid coverage can vary from state to state. However, its worth checking out your plan to see if youre paying for commonly-covered medical supplies and services out of pocket when you dont have to be. Typically, you should be able to get the basics like therapies and additional doctor visits covered, but Medicaid can cover so much beyond the routine expenses special needs parents are so familiar with.
Don’t Miss: Nursing Homes That Accept Medicaid
What Child Care Services Are Available For My Child
If your family is eligible for Child Care Subsidy and your child has a special need, your childâs sliding fee will be waived and your childâs provider will be paid an additional amount for their services.
NOTE: If you have other children who do not have a special need, you may still be responsible for paying their sliding fee.
Once Youre Selected From The Waiting List
Once you come up on the list you are notified through the mail. Make sure you keep your mailing address and phone numbers up to date with these programs! They will send you a letter and set up a meeting with you. You will have to pick two different agencies to work with, a direct service agency, and a case management company. They will set up a meeting with those agencies and you, theyll explain how the waiver works, and then they will set up a budget for you. Usually, it takes a little time to get that budget through the state and sometimes its remanded back. Its usually about a three month wait for services to start. Youll be notified of a start date for your services once your waiver has gone through.
Every year you will meet with those same service providers to review your budget. These service providers will also be in touch with you throughout the year. They do quarterly meetings where they check in and see how things are going. They have a structure set up. Is it smooth all the time? No. Its like any business or agency. Sometimes you have great service providers, and sometimes you have people who move through that system who just arent as skilled as others. Its very important that you educate yourself and remain aware of what your rights are, and what you are eligible for with those waivers.
I hope this answers a few more questions! Feel free to send me messages, because I will reach out and do another video and blog if you have further questions!
Recommended Reading: Qualify For Medicaid Washington State
How Do I Apply
Apply through a local health service office in your region. Social workers are available to help with the process. Find your region. To find the office nearest you, see the Public Health Coverage List or Public Health Coverage Map.
The following must be submitted:
- Proof of income
- Proof of insurance
Application documents may be submitted to your regional office, or to CSHCN via the fax number and email address in the Contact Us section below. You may also mail your application documents to:
CSHCN Services ProgramP.O. Box 149030Austin, TX 78714-9947
If you are a parent of a child with special health care needs, you must also apply for benefits for your child under the Childrens Health Insurance Program and Medicaid.
Access To Care And Service Utilization Among Children With Special Health Care Needs
While Medicaid/CHIP-only children with special health care needs are more likely to find their insurance benefits adequate compared to those covered by private insurance alone, a group of these Medicaid children recently filed a lawsuit arguing that a new Section 1115 waiver in Tennessee could worsen access to care. For details, see Box 1 below. Another challenge is the change in benefit package experienced by individuals who age out of comprehensive coverage provided through the Medicaid EPSDT benefit at age 21. If needed services are not covered by Medicaid, this can have implications for those with chronic conditions as they try to maintain continuity of care and remain in the community as they age into young adulthood, as private insurance is unlikely to cover LTSS and paying for services out-of-pocket may be unaffordable. For example, a recent New York Times article details how in New York, the change from medically fragile child to medically fragile adult includes lower Medicaid payment rates for nurses that could result in young adults with disabilities losing access to in-home services and being forced to move into nursing homes.
Box 1: Medicaid Children with Special Health Care Needs Challenge Tennessee Medicaid Waiver Approval
Also Check: Residential Treatment Centers That Accept Medicaid
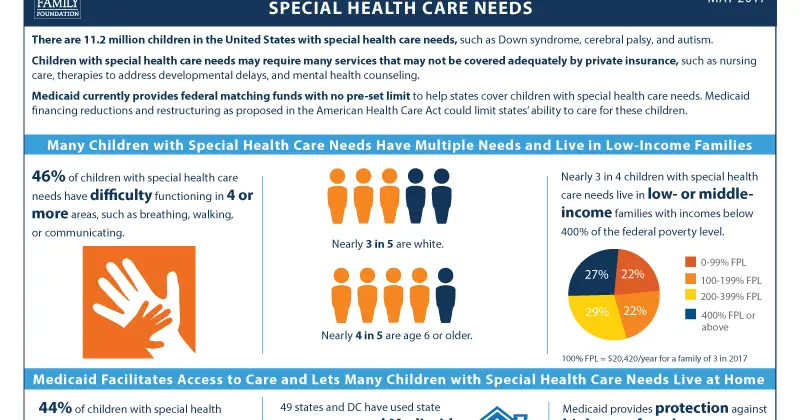
What Health Conditions And Needs Do Children With Special Health Care Needs Have
Medicaid/CHIP-only children with special health care needs are more likely to have greater health needs compared to those with private insurance only. Medicaid/CHIP-only children with special health care needs are three times as likely to experience fair or poor health and 1.5 times as likely to report their health usually or always affects their daily activities somewhat or a great deal health compared to children with private insurance only . Medicaid/CHIP-only children with special health care needs are more likely to have multiple functional difficulties than those with private insurance only, with just under half of the Medicaid/CHIP-only group reporting four or more functional difficulties, compared to less than one-third with private insurance only . Medicaid/CHIP-only children with special health care needs also are more likely to report serious difficulty in each of the six functional areas compared those with private insurance only . For example, Medicaid/CHIP-only children with special health care needs are almost three times more likely to have serious difficulty dressing/bathing and two times more likely to have serious difficult walking or doing errands compared to children with private insurance alone.
Diapers For Children Over Age Three
Most kids are in diapers until theyre about two, but potty training may be more difficult or even unrealistic depending on your childs needs. Thats why many states cover diapers if your differently-abled child is age three or older. You wont be able to pick these up at your local grocery store youll have to order them from a medical supplier who accepts your childs insurance. You can ask your pediatrician or your insurer for a list of approved suppliers.
Read Also: Can A Person Have Medicaid And Private Insurance
Medicaid Waiver Programs For Special Needs Kids Part 2
Weve had some discussions lately about the Medicaid waivers in the state of Texas. Ive gotten a lot of positive feedback from these, for explaining what they are and how they work and especially for giving the parent perspective on these waivers. If youre just tuning in, I did a previous video and blog about what these waivers are, and what waivers are available.
Today Im going to talk a little bit more about the process. Last time I told you about a very important website: medicaidwaiver.org. If you go there you find information specifically about the waivers available in Texas. It will also tell you about the waiting list that is in place for these waiverswhich, as I said is lengthy, although the length depends on the particular waiver.
You May Have To Update
- How much money you make
- Where you live
- And other papers that show your childs diagnosis
If your child loses Medicaid because of your income changing, make sure that you re-apply using this PH-95 checklist. Your child can still get Medicaid using the PH-95 category even if you make too much money for Medicaid.
Read Also: Dentist In Montgomery Al That Accept Medicaid
How Does Medicaid Work
Once you have applied for Medicaid for your child and received their benefits cards, you will need to:
- Pick a managed care plan. You will receive a letter in the mail that will give you the options available in your area.
- Pick a main doctor that is in network with the managed care plan you pick. You can find a doctor in the following ways:
- Call the Medicaid enrollment broker for help at .
- Use the provider directories that came in the mail with your enrollment packet.
Your childs main doctor will then refer you to specialists and therapists who also take Medicaid and can help your child. All Medicaid programs encourage families to use the medical home model of care.
Who Are Children With Special Health Care Needs
Children with special health care needs with Medicaid/CHIP as their sole source of coverage are more likely to live in a low-income household, compared to those with private insurance only. Nearly two-thirds of Medicaid/CHIP-only children with special health care needs live in a household with income at or below 138% of the federal poverty level compared to 7% of children with private coverage only . Federal Medicaid program rules cover children with household incomes up to 138% FPL, but all states opt to expand financial eligibility to higher income levels: as of January 2021, the median financial eligibility level for Medicaid/CHIP children nationally is 255% FPL . Some children with special health care needs qualify for Medicaid based solely on their familys low income. Other children with special health care needs may qualify for Medicaid through various disability-related pathways, which may expand income limits to 300% SSI or only consider the childs own, and not their parents, income.
Don’t Miss: Qualified Health Plan Vs Medicaid
What You Need To Qualify For Medicaid Coverage Of Supplies
If your child has one or more of the above conditions while also experiencing incontinence, you will need a prescription from their healthcare provider for pediatric incontinence products. You will also need a signed letter of medical necessity that explains why the products are needed. The letter will include a list of the medical supplies to be used, and how many disposable supplies will be needed on a monthly basis. This letter must be signed within the last year.
You will also need accurate diagnostic information pertaining to the underlying condition, as well as any other medical diagnosis.
The good news is that Aeroflow Urology can take care of all of this for you! Simply complete our quick insurance qualification form and let us handle all of the paperwork and communication with your childs pediatrician and insurance provider.
Who Is Eligible For Services
Anyone who:
- Is 20 or younger or any age with a diagnosis of cystic fibrosis.
- Has an income level at or below 200 percent of the federal poverty level.
- Has a medical condition that
- Is expected to last at least one year
- Will limit one or more major life activities
- Requires a higher level health care
- Has physical symptoms. Having only a mental, behavioral or emotional condition, or a delay in development wont qualify).
Recommended Reading: Does Medicaid Cover Paragard Iud
Medicaid Transportation Services For Children With Disabilities
When you have a child with a disability or special health care needs, finding low-cost and accessible transportation is challenging if you do not own a car or your car cannot transport your child comfortably. If your child has Medicaid, there is a transportation program that will give you some of those rides at no cost to you.
On this page, we talk about the Medicaid transportation benefit and some other transportation choices you might have in your community and how to use them. Our Grants and Other Funding Sources page also lists some transportation programs for times when you have specific challenges. Your child has choices and rights with any form of transportation, from city buses to taxis to paratransit.
Below are some forms of transportation that might meet your familys needs, depending on if you live in a city, town, suburb, or rural area of Texas.
- City buses or light rails.
- Taxis or getting help from a friend to share a ride.
- Paratransit: a type of transportation designed for people with disabilities or special health care needs .
