Income Limits In Arkansas For Medicaid
In Arkansas the individual receiving Medicaid cannot have income over $2,250. If their income is over that amount, they will need to do some Medicaid Planning to create eligibility. One strategy that works well is a Miller Trust . If an individual is married, the spouse’s income does not typically count towards the income cap, but it is important to maximize income protection via the Monthly Needs Allowance rules. The maximum amount of income the Medicaid office allows a community spouse to keep in Arkansas is $3,090 and the minimum amount is $ 2,003. All of an individual’s monthly income must go towards their cost of care, which can include medical bills, prescriptions and other health care costs, aside from $40 which is for a personal needs allowance. The income limits are based as a percentage of the Supplemental Security Income defined by the Social Security Administration’s Federal Poverty Levels and change every year.
Is It Hard To Qualify For Medicaid
As long as you meet the eligibility rules in your state, it is not hard to qualify for Medicaid. After all, almost 74 million Americans are covered by the program.
Contact your state Medicaid program in order to apply for Medicaid. Applications are generally reviewed and approved within 90 days and typically are reviewed sooner.
What Are The Medicaid Income Limits For 2022
Finding out if you are eligible for Medicaid can be quite a headache. Since Medicaid is jointly funded by federal and state governments, there are different eligibility criteria for each state! One of the biggest factors for Medicaid eligibility are the income limits.
If you are trying to learn more about whether your income is within the Medicaid income limit for your state of residence, then you are reading the right article!
I will be explaining which sources of monthly incoming money are considered income, how each state decides their income limit, and providing an easy-to-use list of each states income limits for the year 2022.
Read on to learn more about Medicaid income limits and determine if your income would be considered within the limit set by your state of residence!
Recommended Reading: Nursing Homes That Accept Medicaid
Arkansas Medicaid Asset Limits 2019
Individuals in Arkansas are allowed to keep $2,000 when they apply to Medicaid for long term care. If they are over this amount, they must spend down on care. It is important to note, that individuals are not allowed to give gifts of any amount for a period of 5 years prior to applying to Medicaid. If an individual’s assets are more than $2,000, they should learn about Medicaid Planning strategies. This asset limit only applies to assets that are considered countable assets. Some examples of countable assets include savings accounts, bank accounts, retirement accounts and a second home. If you have multiple assets and are looking to access Medicaid, it may make sense to speak with a Medicaid Planner or Elder Law attorney in Arkansas.
Couples that both require Medicaid for long term care in Arkansas are allowed to keep $3,000 in assets. If there is one spouse that requires care, and one that does not, the spouse that does not receive care is referred to as the Community Spouse. The Community spouse is allowed to keep 50% of their assets up to $123,600 in countable assets which is known as the Community Spouse Resource Allowance. The Community Spouse is allowed to keep 100% of their marital assets up to $24,720 .
How Long Does It Take To Get Approved For Medicaid In Arkansas
3 to 6 monthsTypically, a Medicaid application takes 3 to 6 months to process, unless a disability determination needs to be made. The process time can also increase if the required documentation is not provided promptly. The Department of Human Services is responsible for administering the Medicaid program in Arkansas.
Also Check: Does Maryland Medicaid Cover Abortions
State And Federal Spending
During fiscal year 2016, Medicaid spending nationwide amounted to nearly $553.5 billion. Spending per enrollee amounted to $7,067 in fiscal year 2013, the most recent year for which per-enrollee figures were available as of June 2017. Total Medicaid spending grew by 33 percent between fiscal years 2012 and 2016. The Medicaid program is jointly funded by the federal and state governments, and at least 50 percent of each state’s Medicaid funding is matched by the federal government, although the exact percentage varies by state. Medicaid is the largest source of federal funding that states receive. Changes in Medicaid enrollment and the cost of healthcare can impact state budgets. For instance, in Arkansas, the percentage of the state’s budget dedicated to Medicaid rose from 20.0 percent in 2010 to 25.5 percent in 2015. However, state cuts to Medicaid funding can also mean fewer federal dollars received by the state.
During fiscal year 2016, combined federal and state spending for Medicaid in Arkansas totaled about $6 billion. Spending on Arkansas’ Medicaid program increased by about 44.5 percent between fiscal years 2012 and 2016. Hover over the points on the line graph below to view Medicaid spending figures for Arkansas. Click on the red bar below the graph to view these figures as compared with three of Arkansas’ neighboring states.
Transition To Arkansas Works In 2017
In April 2016, lawmakers in Arkansas voted to approve and fund an overhaul of Medicaid expansion in Arkansas, dubbed Arkansas Works. The state submitted the new waiver proposal to CMS in June 2016, and CMS reviewed it over the following months. In December 2016, CMS granted approval for most of the modifications the state had requested, with a five-year extension of the Arkansas Works Medicaid demonstration waiver, which took effect in 2017 .
Under Arkansas Works, enrollees with income above the poverty level now pay modest premiums for their coverage , unemployed enrollees are referred to job training/referral, and enrollees can obtain coverage from their employers with supplemental funding from Medicaid.
But only about 20% of the 63,000 enrollees subject to premiums actually paid those premiums in 2017. . The state reported that of the people referred to job training, less than 5% followed through and obtained work referrals. And only one person ever used the Medicaid premium assistance program for employer-sponsored insurance.
Additional changes to Arkansas Medicaid expansion were approved by state lawmakers in May 2017, and Governor Hutchinson submitted an amendment to the states waiver in June 2017, which was under HHS review for several months. The proposed changes, detailed below, were mostly approved by the Trump Administration, although the states proposal to cap Medicaid eligibility at the poverty level was rejected.
You May Like: Vein Clinics That Take Medicaid
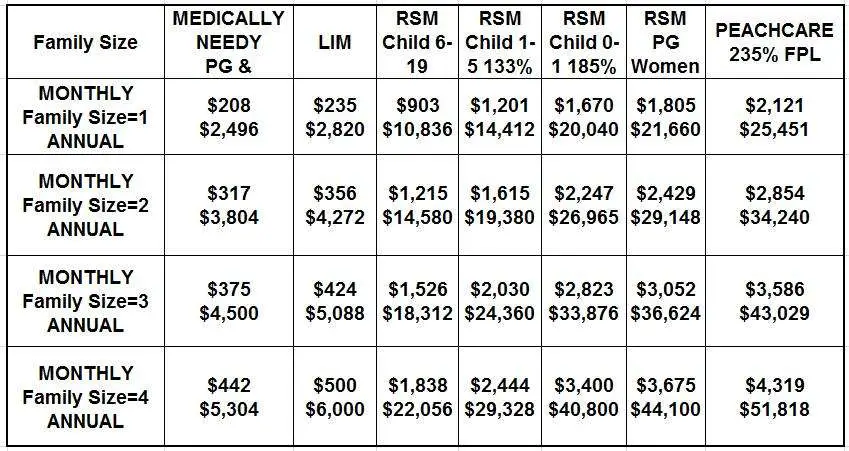
Arkansas Medicaid Income Limit
The Arkansas Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the Arkansas Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 142 percent of FPL
- Any child age 1-5 with a family income up to 142 percent of FPL
- Children ages 6- 18 with family income up to 142 percent of FPL
- CHIP for children with family income up to 211 percent of FPL
- Pregnant women with family income up to 209 percent of FPL
- Parents of minor children with family income up to 17 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 80% of the FPL
- Adults without dependents under Medicaid expansion with income up to 133% of the FPL
How To Apply For Medicaid
If youâre eligible for Medicaid, you can apply all year round through your state’s Medicaid website or HealthCare.gov, the federal health insurance marketplace. If you apply for Medicaid through Healthcare.gov and it looks like you qualify, the federal government will notify your state agency, which will contact you about enrollment. States also generally let you print out paper applications you can mail, fax or return directly to your local government office.
To complete your Medicaid application, you will likely need to provide documentation that you meet your state’s requirements. This documentation may include:
-
Your birth certificate or driver’s license to serve as proof of age and citizenship
-
Recent pay stubs or tax returns to serve as proof of income
-
Copies of bank statements
-
Proof of address, which could include a lease, utility bill statements or a copy of your mortgage
-
Medical records to serve as proof of disability
States have 45 days to process your Medicaid application. They have 90 days if eligibility is tied to a disability . Processing can take longer if applicants do not supply all of the required documentation. If you don’t qualify for Medicaid, you might be able to get subsidized health insurance through Healthcare.gov. However, only certain life events allow you to apply for a marketplace health care plan outside of open enrollment, which takes place from Nov. 1 to Jan. 15.
Free in your inbox each Friday.
Sign up now
Recommended Reading: How To Renew Medicaid Ny Online
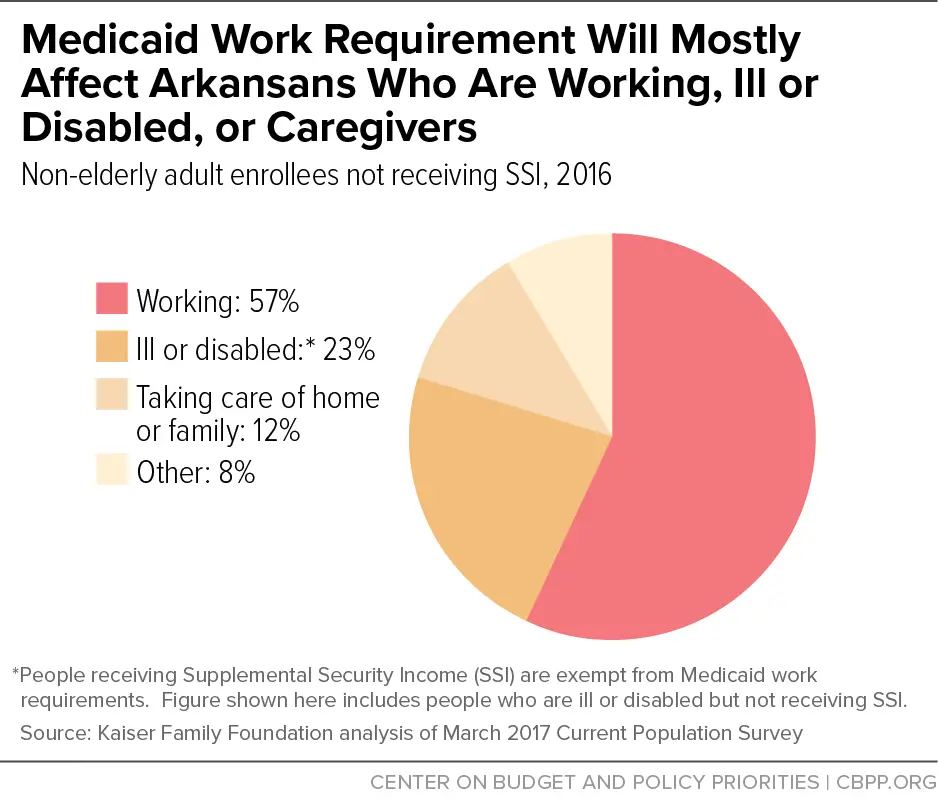
Does Arkansas Have A Medicaid Work Requirement
Arkansas implemented a Medicaid work requirement in 2018, described below in detail. But Federal Judge James Boasberg overturned the Medicaid work requirements in Kentucky and Arkansas as of March 2019, noting that officials had not taken steps to prevent coverage losses stemming from the work requirement.
The Biden administration officially withdrew the states Medicaid work requirement waiver approval in March 2021, although it had not been in effect for two years prior to that.
So Arkansas is no longer removing people from the Medicaid program for failure to comply with the work requirement or reporting requirement, and the people who had already lost their coverage under the work requirement rules were able to re-apply for Medicaid although many may not be aware that their access to Medicaid has been reinstated .
As of March 2021, there were more than 905,000 people enrolled in Arkansas Medicaid and CHIP, which was higher than it had been in the months following implementation of the work requirement, but still lower than it had been in 2018, despite the fact that the COVID pandemic had been ongoing for a year.
Medicaid Spending In Arkansas
This article does not contain the most recently published data on this subject. If you would like to help our coverage grow, consider donating to Ballotpedia.
| Medicaid spending in Arkansas |
Arkansas’Medicaid program provides medical insurance to groups of low-income people and individuals with disabilities. Medicaid is a nationwide program jointly funded by the federal government and the states. Medicaid eligibility, benefits, and administration are managed by the states within federal guidelines. A program related to Medicaid is the Children’s Health Insurance Program , which covers low-income children above the poverty line and is sometimes operated in conjunction with a state’s Medicaid program. Medicaid is a separate program from Medicare, which provides health coverage for the elderly.
This page provides information about Medicaid in Arkansas, including eligibility limits, total spending and spending details, and CHIP. Each section provides a general overview before detailing the state-specific data.
HIGHLIGHTS
Don’t Miss: What’s Better Medicare Or Medicaid
Medicaid And Medicare Dual Eligibility
If you qualify for both Medicare and Medicaid, you are considered dual eligible. In this case, you may qualify for a certain type of Medicare Advantage plan called a Dual Eligible Special Needs Plan . D-SNPs are designed to meet the specific needs of people who have Medicaid and Medicare.
You can compare plans online to find out if D-SNPs are available where you live, or you can call to speak with a licensed insurance agent for information about eligibility and enrollment.
Qualifying For Medicare And Arkansas Medicaid
If you are 65 or older, have ALS, ESRD, or youve received SSDI for at least 25 months, you may qualify for Medicare. People who have both Medicare and Medicaid may qualify for a type of Medicare Advantage plan called a Dual Special Needs Plan .
Medicare Advantage plans are private insurance plans that can offer benefits that neither Original Medicare nor Medicaid covers, such as fitness classes and meal delivery.
Many DSNPS have low or $0 monthly premiums, which means that you may be able to receive all of the supplemental benefits Medicare Advantage plans can offer at little or no additional cost to you.
Many people have to wait until the Annual Enrollment Period , which is from October 15 to December 7, to make changes to their coverage. However, you qualify for a Special Enrollment Period if you have a DSNP.
Your DSNP SEP allows you to make one change per quarter from January to September. You can still make a change during the fourth quarter, but you can only make a change during AEP. The change you make during AEP will take effect on January 1 the following year.
A licensed agent with Medicare Plan Finder can help you find out if you qualify for a DSNP and help you enroll. To learn more about Dual Special Needs Plans call 1-844-431-1832 or contact us here today.
Also Check: Washington State Medicaid Residency Requirements
If Your Medicaid Is With Your Ldss To Order A New Medicaid Benefit Identification Card Please Call Or Visit Your Local Department Of Social Services
In this post, we are going to explain in detail the virginia medicaid income limits for 2021. Determine your eligibility for this benefit All income standards are expressed as a percentage of the federal poverty. Jun 23, 2021 · read arkansas medicaid eligibility requirements for long term care for seniors including the income, assets and level of care requirements. If your medicaid is with your ldss, to order a new medicaid benefit identification card, please call or visit your local department of social services.
If your medicaid is with your ldss, to order a new medicaid benefit identification card, please call or visit your local department of social services. Medically needy income limit arkansas: Sep 01, 2021 · arkansas expanded medicaid by usingmedicaid funds to purchase exchange plans for eligible enrollees. All income standards are expressed as a percentage of the federal poverty. Income limit the income limit for all of the ltss programs is three times the current ssi standard payment amount for an individual. May 06, 2021 · 2021 medically needy income limits for medicaid eligibility (these figures do not necessarily change annually. May 01, 2021 · the medicaid income limit is the most important criteria for deciding whether you qualify for medicaid in your state. Medicaid provides health coverage to millions of americans, including children, pregnant women, parents, seniors and individuals with disabilities.
Who Qualifies For Medicaid
In all but 13 states, adults who make below a certain income may qualify for Medicaid. In all states, Medicaid is available to people who make a low income and also meet other criteria such as being at least 65 years old, disabled, pregnant or other qualifications.
Each state runs its own Medicaid programs with its own set of qualifying criteria.
Read Also: How Can I Check The Status Of My Medicaid
Lawsuit Over Arkansas Medicaid Work Requirement Was Slated For Scotus But Hearing Was Canceled And Work Requirement Waiver Was Then Rescinded By Hhs
The Trump administration appealed the case, as expected, and a panel of three judges on the U.S. Court of Appeals for DC heard oral arguments in the appeal in October 2019. During the arguments, all three judges expressed concerns about the coverage losses that stem from Medicaid work requirements, which was the crux of Boasbergs ruling earlier in the year that suspended the work requirement. And in February 2020, the three-judge panel unanimously ruled that it was arbitrary and capricious for HHS to approve the Arkansas Works waiver, and upheld Boasbergs ruling to overturn the states Medicaid work requirement. So the work requirement has remained suspended.
In July 2020, however, the Trump administration asked the Supreme Court to intervene and allow Arkansas to reinstate its work requirement once the COVID-19 situation is under control enough to allow the unemployment rate to return to normal levels. The Supreme Court justices agreed to hear the case, and oral arguments in the lawsuit, Arkansas v. Gresham, were scheduled for March 29, 2021 at the Supreme Court.
But the Biden administration does not support Medicaid work requirements, and asked the Supreme Court to cancel the hearing. That request was granted, and Arkansas v. Gresham was not heard by the Supreme Court.
Soon thereafter, in March 2021, HHS officially withdrew approval for the Medicaid work requirement in Arkansas.
How Do You Calculate Your Medicaid Income Eligibility
Follow these steps to calculate whether or not your income may qualify you for Medicaid:
- Find the FPL for your household using the chart above
- Multiply that number by your states Medicaid income limit found below, and then divide by 100
For example, if there are two people living in your household and you live in Arizona, you would multiply $17,420 by 138 and then divide by 100. That equals $24,039.60.
You may also multiply $17,420 by 1.38.
Also Check: Primary Care Doctors Who Take Medicaid
Similar Program New Name
After 2016, Medicaid expansion in Arkansas was called Arkansas Works instead of the Private Option. But it was widely noted that the fundamental mechanics of the new program were very similar to the Arkansas Health Care Independence Program, which was the name of the Arkansas waiver program from 2014 through 2016. Arkansas still uses Medicaid funds to purchase private coverage for eligible enrollees in the exchange, which was the basic premise of the Private Option in the first place.
But lawmakers who were opposed to the Private Option were able to end it and replace it with Arkansas Works in many cases, fulfilling campaign promises but without the ramifications that would ensue if the state were to kick 300,000+ people off their health insurance .
