Prior Authorization And Notification Resources
Demographic Information Updates with TMHP
To Providers: Please update your enrollment and demographic information with TMHP . TMHP is HHSCs provider enrollment administrator and serves as the authoritative source for HHSC Providers enrollment and demographic information. Once you update your enrollment and demographic information with TMHP, your data will be reconciled with the demographic information on file with the MCOs.
To make updates to your current enrollment , please access the web page titled Provider Enrollment and click on Enroll Today at the following URL: Provider Enrollment | TMHP.
For instructions on how to make demographic changes to your current enrollment, please access the web page titled Provider Enrollment and Management System : A Step-by-Step Guide at the following URL: Provider Enrollment and Management System | TMHP.
Otherwise, you can contact TMHP directly at 800-925-9126 for assistance.
Behavioral Health Providers
Learn how to join the Behavioral Health Network, review Community Plan Behavioral Health information, or submit demographic changes at Community Plan Behavioral Health.
Facility/Hospital-Based Providers, Group/Practice Providers and Individually-Contracted Clinicians
The state-specific requirements and process on how to join the UnitedHealthcare Community Plan network is found in the UnitedHealthcare Community Plan Care Provider Manuals.
The Centers for Medicare & Medicaid Services established the Medicaid Managed Care Rule to:
How To Choose A Health Plan
When picking a plan, think about the following:
- Are doctors you already use and like covered by the plan?
- How is the plan rated on issues that are important to you and your family?
- What value-added services are available through the plan?
We also provide tools to help you choose the best plan for you and your family.
How Will Hhsc Verify Individuals With Complex Conditions Are Getting The Care They Need In A Managed Care Setting
HHSC has a contract with all Texas Medicaid managed care health plans. The contract lists requirements the health plans must meet to get paid. For example, health plans must provide members with medically necessary services in a timely manner and appropriate setting. When a health plan does not meet its requirements, HHSC will address the issue and ensure the member’s needs are met.
Don’t Miss: Eye Doctors In Traverse City That Accept Medicaid
How Will Hhsc Provide Consumer Direction In A Managed Care Model
Medicaid managed care includes consumer-directed services that allow individuals who receive certain services to hire and manage the people who provide their services. The following services are available for self-direction:
- Personal assistance services
- Professional therapies
- Respite
- Supported employment
- Employment assistance
- Cognitive rehabilitation therapy
Consumer-directed services will continue to be an option in the STAR+PLUS model as it is in traditional Medicaid. In addition, the STAR+PLUS health plans are required to submit quarterly consumer directed services utilization reports to HHSC for review.
How Does Medicare Work With Medicaid Managed Care
 Medicaid Case Management Services in …” alt=”Texas Medicaid 101 > Medicaid Case Management Services in …”>
Medicaid Case Management Services in …” alt=”Texas Medicaid 101 > Medicaid Case Management Services in …”> If someone is in both programs, the client will use Medicare for their health care needs, prescription drugs and medications. The client’s Medicaid health plan will provide Medicaid long-term services and supports needs and will cover certain medications not covered at all, or only partially, by Medicare.
Recommended Reading: Assisted Living That Accepts Medicaid In Nj
Expansion Of Medicaid Managed Care
Most people in Texas who have Medicaid get their services through managed care. In this system the member picks a health plan and gets Medicaid services through that health plan’s network of providers. Most health plans offer Medicaid members extra services not available through traditional Medicaid.
Right now, there are three Medicaid managed care programs in Texas: STAR, STAR+PLUS, and STAR Health. The 2013 Texas Legislature approved several expansions of Medicaid managed care and directed HHSC to develop a performance-based payment system that rewards outcomes and enhances efficiencies. Managed care expansion plans include:
Will Managed Care Change The Types Or Amounts Of Services A Member Receives
Members will continue to receive the types and amounts of services that most appropriately meet their medical needs. Needs are determined by the results of an assessment and development of an individual service plan, where appropriate. Medicaid health plans are required to provide all covered medically necessary services to members. Medically necessary means that services are:
- Reasonably necessary to prevent illness or medical conditions, or provide early screening, interventions, and treatments for conditions that cause suffering or pain, cause physical deformity or limitations in function, threaten to cause or worsen a handicap, cause illness or infirmity of a recipient, or endanger life.
- Provided at appropriate locations and at the appropriate levels of care for the treatment of clients’ conditions.
- Consistent with health care practice guidelines and standards that are issued by professionally-recognized health care organizations or governmental agencies.
- Consistent with the diagnoses of the conditions.
- No more intrusive or restrictive than necessary to provide a proper balance of safety, effectiveness, and efficiency.
Also Check: Is Invisalign Covered By Medicaid
Current News Alerts And Messages From Texas Hhsc
Find COVID-19 vaccine availability for your state or territory
Use this list of local health departments to learn about availability in your area. Availability may vary by location and time. We encourage you to check back often as information becomes more available.
Dental Prevention – More than Mouth Care
Correlations between dental and chronic systemic diseases have frequently been reported, particularly with respect to periodontitis with diabetes mellitus type 2 andcardiovascular disease.1 Our child and youth members have dental coverage as a benefit.
Texas Community Plan Quality Newsletter
UnitedHealthcare Community Plan of Texas continually strives to make improvements that can make a difference in our members lives. One way we do this is by looking at the following Healthcare Effectiveness Data and Information Set measures, which are gathered through a National Committee for Quality Assurance tool that can help find ways to enhance health care.
Making the Most of Life While Living With Complex Care Needs
We use complex care management for our members who are living with chronic and/or complex conditions and have a high risk of worsening health and repeat hospitalizations.
Help When and Where Its Needed
Find COVID-19 vaccine availability for your state or territory
Dental Prevention – More than Mouth Care
Texas Community Plan Quality Newsletter
Making the Most of Life While Living With Complex Care Needs
Help When and Where Its Needed
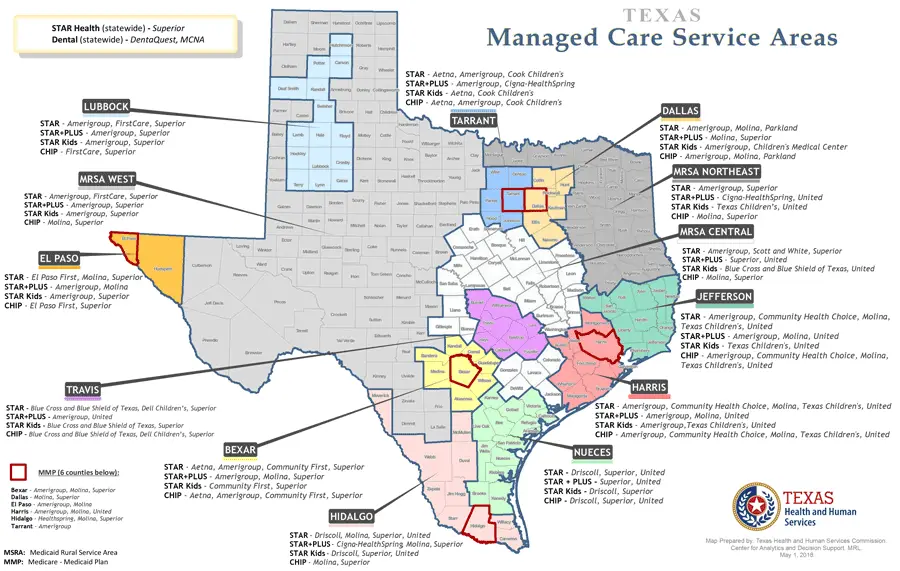
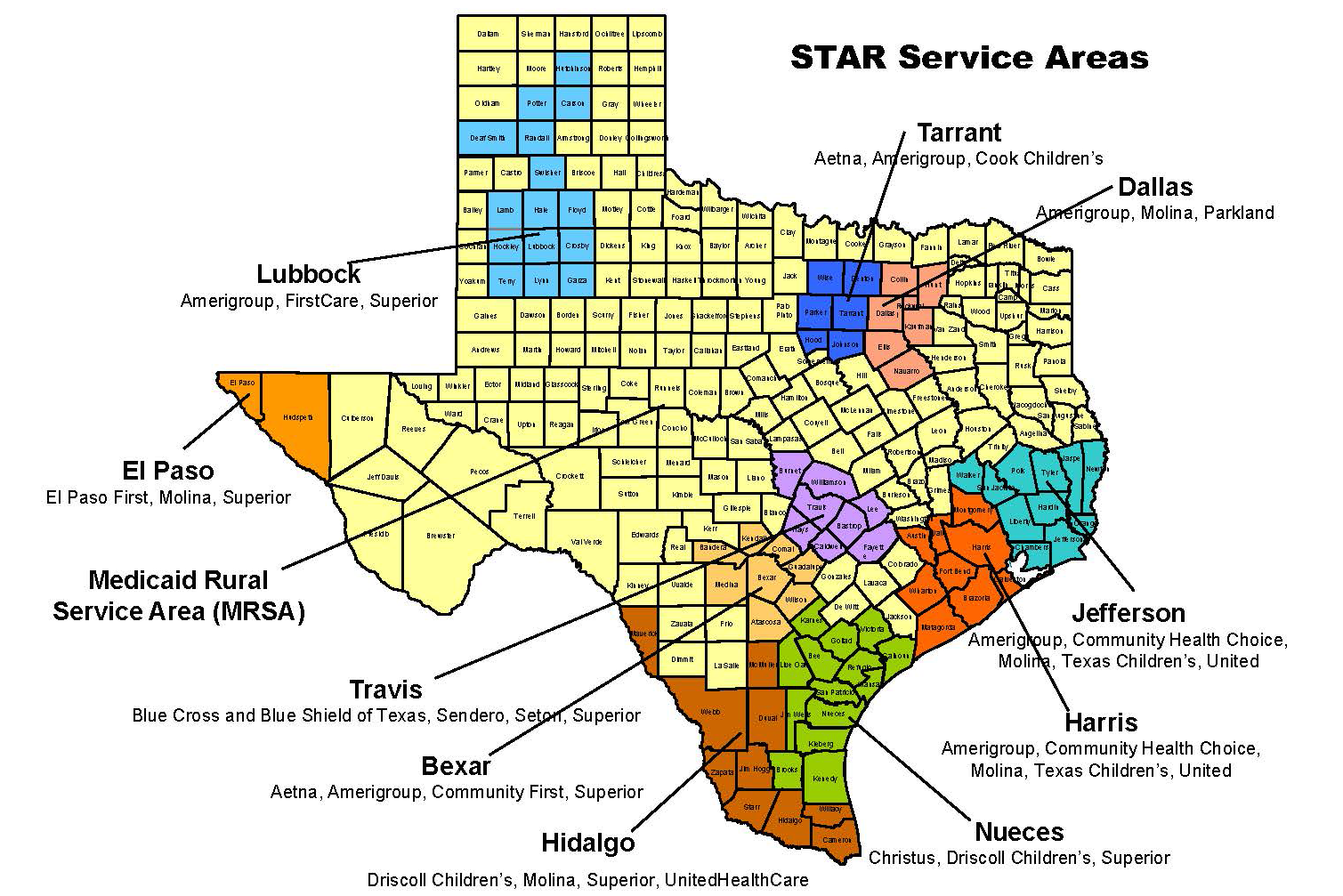
Star Medicaid Managed Care Program
Most people who have Medicaid in Texas get their coverage through the STAR managed care program. STAR covers low-income children, pregnant women and families. STAR members get their services through health plans they choose.
If you’re new to STAR, you’ll choose a health plan from the ones available in your service area . Learn more about how to choose or change your health plan.
You May Like: Does Medicaid Pay For Dentures In Nc
Medicaid Managed Care Market Tracker
Medicaid MCO State-Level Enrollment Data
-
about this data collection
-
This Data Collection, the Medicaid Managed Care Market Tracker, provides information related to risk-based Medicaid managed care organizations that provide comprehensive services, including acute care services and, in some cases, long-term services and supports as well, to Medicaid enrollees. In addition, the Tracker provides information on parent firms that own Medicaid MCOs in two or more states.
The data in the Medicaid Managed Care Tracker are current to the date or period specified in the sources for each table.
The information in this Tracker is public information and may be reproduced with appropriate citation.
Executive Commissioner’s Commitment To Improving Member And Provider Experience In Medicaid Managed Care
Executive Commissioner Chris Traylor held stakeholder meetings in 2015 to gather input on ways to improve the managed care landscape, from both the member and provider perspective. According to Executive Commissioner Traylor, the purpose was to improve provider experience in managed care and ultimately to ensure the 4.5 million people relying on the Medicaid and Children’s Health Insurance Program programs have appropriate access to services to enable them to live strong, productive lives. He also shared thoughts that it is important as Texas evolves from fee-for-service to managed care, to project future needs to create the best system possible.
HHSC responses were shared directly with stakeholder groups in February 2016, updates were posted to the website on April 11, 2016, and July 22, 2016, and biannual updates on items in progress or under discussion will continue to be shared on the website. Items that are closed as of the last update will be provided in a separate file as there will be no further update. Items were closed either as complete, no action to be taken, or other . In each update, changes to previous responses are noted with red strikethrough for language that is being removed in order to provide an update, and new language is provided in red.
Questions about this project can sent to .
Recommended Reading: I Am On Disability Can I Get Medicaid
What Is A Provider Network
Provider networks are organizations of health care providers that deliver services within managed care health plans. Managed care enrollees are expected to use network providers.
In Texas, there are four types of Medicaid: STAR, STAR+PLUS, STAR Health, and traditional Medicaid. The type of Medicaid coverage a person gets depends on where the person lives and what kind of health issues the person has.
- Clients receive traditional Medicaid if they are not in a managed care network.
Healthy Texas Women Program
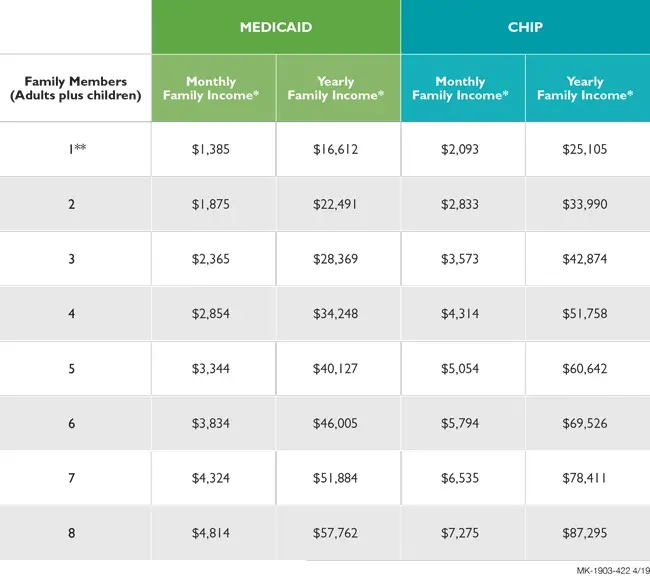
Have you lost your Medicaid benefits? The Healthy Texas Women Program provides family planning exams, related health screenings, and birth control to women ages 18 to 44 whose household income is at or below the programs income limits .
You must submit an application to find out if you can get services through this program. Visit this site for more information.
Don’t Miss: Blue Cross Blue Shield Medicaid
Health Plan Report Cards
People across Texas shared their thoughts about their health plan, and rated them, one to five stars, on the services their plan provided.You can compare plans using the overall ratings or by looking at the services that matter the most for you and your family.
You can view the report cards on the Managed Care Report Cards page. Click the program you are enrolled in and find your service area to see plans available to you.
Will There Be A Limit On Prescription Drugs
- If a member is enrolled in a Medicaid health plan and not Medicare, there is no limit on the medicines they can fill each month.
- If an individual is enrolled in Medicaid and Medicare Part D, the individual’s Part D health plan will cover most medicines. Medicare Part B also covers certain medicines. Medicaid covers a limited number of medicines that are not covered by Medicare.
- If an adult is transitioning from fee-for-service Medicaid, which currently has a limit on medicines, into managed care, they will receive unlimited prescriptions once they are enrolled in managed care.
Also Check: Does Medicaid Pay For Ed Drugs
Video Result For Illinois Medicaid Managed Care Plans
Illinois pharmacy owners pinched by Medicaid…
Expanding Illinois’ Managed Care of Medicaid
Medicaid managed care program press conference
careillinoiscare
carecaremanagedcarecare
managedcare
managedcarecare
managedcarecarecare
care
caremanagedcarecarecare
bestiamhp.net
managedcarecarecare
care
carecarecarecare
caremanagedcarecare
care
bestwww.enrollhfs.illinois.gov
caremanagedcare
tipwww.medicaidplanningassistance.org
managedcare
managedcarecare
Illinois pharmacy owners pinched by Medicaid…
Expanding Illinois’ Managed Care of Medicaid
Medicaid managed care program press conference
Managed Medicaid at UI Health
How Do States Deliver Care In Medicaid
States administer their Medicaid programs and determine how to deliver care. Federal law requires states to provide certain mandatory benefits and allows states the choice of covering other optional benefits. Comparisons across states should consider differences in their benefits and care delivery approaches. For example, some states choose to deliver Medicaid health benefits and additional services through managed care organizations. States may also use waiver authorities, such as 1915, 1915 waivers, or section 1115 demonistrations to offer coverage or extend benefits to a target population. The following data show examples of the ways states can vary in benefit coverage and how they deliver care.
You May Like: Medicaid Funded Home Care Services
What Is A Managed Care Organization
HHSC contracts with managed care organizations, licensed by the Texas Department of Insurance, and pays them a monthly amount to coordinate health services for Medicaid clients enrolled in their health plan. The health plans contract directly with doctors and other health care providers to create provider networks their members can use. The health plans are required to provide all covered medically necessary services to their members.
Is Targeted Case Management And Mental Health Rehabilitative Services Covered Under Managed Care In The Future
Yes, targeted case management for individuals with mental illness and mental health rehabilitative services is available through managed care. Mental health targeted case management and mental health rehabilitative services are available to Medicaid recipients who are assessed and determined to have a severe and persistent mental illness such as schizophrenia, major depression, bipolar disorder and children and adolescents ages 3 through 17 years with a diagnosis of a mental illness who exhibit a serious emotional disturbance. Legislative direction was given to HHSC to make these services available in Medicaid managed care to provide better coordination of care by integrating physical and behavioral health care for these Medicaid recipients.
Recommended Reading: Does Ira Count As Income For Medicaid
What Is Service Coordination
Service coordination is a STAR+PLUS benefit that helps members identify and coordinate service and benefit needs and develop a plan to allow them to live in the most independent setting possible. A health plan service coordinator will work directly with plan members, family members, doctors, and community supports to make sure all health care and long-term services and supports needs are met. Service coordination will also be a benefit in the STAR Kids program. A health plan service coordinator:
- Makes home visits and assesses member needs.
- Coordinates with Medicaid and Medicare providers.
- Arranges for other services such as medical transportation.
- Coordinates other community supports, such as housing.
Why Choose Community
As a local nonprofit health plan, Community Health Choice gives you plenty of reasons to join our Community. From the benefits and special programs we offer to the way our Member Services team helps you make the most of them, Community is always working life forward for you and your family.
I always tell people to choose Community Health Choice. I tell them its the best health insurance they will ever be with. Chandolyn
Recommended Reading: Family Of Three Income For Medicaid
