North Carolina’s Specialized Foster Care Plan
On July 1, 2022, the Department of Health and Human Services will launch the statewide Specialized Foster Care Plan. This specialized plan is intended to meet the unique needs of North Carolina children and youth currently and formerly involved in the child welfare system and to address receiving seamless, integrated, and coordinated health care.
The Foster Care Plan will integrate comprehensive physical and behavioral health services while maintaining treatment plans when placements change. This plan will also include care management services to improve coordination among service providers, families, involved entities and other stakeholders involved in serving Foster Care Plan members.
To access the white paper on North Carolina’s Specialized Foster Care Plan or to view a recent webinar providing an overview of this plan, visit the DHHS website for the Specialized Foster Care Plan
What Other Rights Do You Have Under Nc Medicaid Managed Care
- Get free advice in your preferred language from the Enrollment Broker about whether you have to be enrolled in a managed care health plan and what health plan is the best choice for you and your family.
- Get out-of-network care if medically necessary services are not available in your health plans network.
- Have no interruption of care when moving in or out of Medicaid Managed Care or between health plans.
- Appeal if your health plan denies, reduces or stops coverage for health care you need.
- Contact the NC Medicaid Ombudsman at 877-201-3750 if you experience any problems.
Icymi: Open Enrollment Period For Nc Medicaid Managed Care Now Open Through May 14
The North Carolina Department of Health and Human Services recently announced the launch of the statewide open enrollment for NC Medicaid Managed Care. Beneficiaries can now enroll through one of four channels:
The NC Medicaid Managed Care website offers a wide variety of tools and resources to assist beneficiaries in choosing a primary care provider and a health plan for their families care. Resources include frequently asked questions, a chat function, and the Medicaid and NC Health Choice Provider and Health Plan Lookup Tool. The Lookup Tool offers four categories of search capabilities, advanced search based on specialty and the ability to view all providers within an organization/location and by practice name.
Open enrollment ends May 14, 2021. Beneficiaries who enroll with a health plan during open enrollment will have the opportunity to select a PCP from a list of contracted providers. If they do not choose a health plan before May 14, one will be assigned to them by NC Medicaid. In the first 90 days after their coverage effective date, beneficiaries can change health plans for any reason. After that, unless there is a special reason, beneficiaries cannot change health plans until the next Medicaid recertification date.
Recommended Reading: Does Medicaid Cover Gym Memberships
Virtual Statewide Quality Forum
The North Carolina Department of Health and Human Services Division of Health Benefits and North Carolina AHEC, in conjunction with the five Medicaid managed care health plans, hosted a Virtual Statewide Quality Forum in October 2021 to help providers, practice managers, and quality managers succeed with Medicaid Managed Care quality initiatives.
Topics included DHHS NC Medicaid Managed Care Quality Strategy, statewide performance improvement initiatives for SF2022 , Health Plan and AHEC Provider Supports, and Quality Measure Data and Reporting. The session also included a question and answer forum for participants.
Access the October 12, 2021 Recording, Slides and Transcript.
Webinar Series: Quality & Population Health
This series, formerly the Advanced Medical Home Webinar Series, is designed to support providers, practice managers, quality improvement professionals, care managers, and clinically integrated networks .
February 24, 2022 | Healthy Opportunities & EvaluationsMarch 24, 2022 | COVIDApril 28, 2022 | NC InCK APMMay 26, 2022 | Prenatal/postpartum PIP
View recordings and slides for past webinar below:December 9, 2021 | Advanced Medical Homes: Incentives Plan: Recording, Slides and TranscriptOctober 14, 2021 | Integrated Care for Kids / Healthy Opportunity Pilots: Impacts to AMHs: Recording, Slides and TranscriptSeptember 9, 2021 | AMH Quality Measures /Medicaid Statewide QI Projects FY22, Provider Supports: Recording, Slides and Transcript
Read Also: How Much Do You Have To Earn To Get Medicaid
Is This Medicaid Expansion
No. The move to managed care will not change the number of enrollees in North Carolinas Medicaid program. Instead, itll section existing enrollees into narrower insurance networks.
Medicaid expansion is a separate policy debate about adding enrollees to the program under an Obama-era provision of the Affordable Care Act. North Carolina has yet to expand its Medicaid program, and debates over the issue brought the state budget process grinding to a halt in 2019.
Amh Provider Manual 20 Released
A Message from NCTracks on Behalf of NC Medicaid:The Department recently released the Advanced Medical Home Provider Manual 2.0 . This version reflects program expectations as well as recent program modifications and changes that impact provider contracts. It replaces the prior version issued on December 12, 2019. Additional guidance and program information are available on the Advanced Medical Home webpage.
You May Like: How To Get In Touch With Medicaid
Open Enrollment Begins Monday March 15th
Beginning Monday, March 15, Medicaid beneficiaries are able to enroll into Medicaid managed care health plans. Last week, NC DHHS began mailing enrollment packets statewide and launched the NC Medicaid Enrollment Call Center and a mobile app called NC Medicaid Managed Care.
Beneficiaries can reach the NC Medicaid Enrollment Call Center at 833-870-5500 or download the app on Google Play or the App Store.
The NC Medicaid enrollment website is also a resource for members to select a health plan.
The next important milestone for providers it to ensure they execute a contract before April 12th, so you are included in the period of auto-enrollment, beginning May 15.
Access the NC DHHS Provider Playbooks to read more about each milestone in the transition to Medicaid manged care.
Apply For Medicaid In North Carolina
Online at HealthCare.gov or at ePass. You can enroll by phone at 1-800-318-2596. You can also apply in person at your local County Department of Social Services office or complete a paper application.
Eligibility: The aged, blind, and disabled. Also, parents with dependent children are eligible for Medicaid with a household income up to 45% of poverty level, and children are eligible for Medicaid or CHIP with incomes up to 211% of poverty maternity-related coverage is available for pregnant women with incomes up to 196% of poverty.
Also Check: How To Obtain Medicaid In Florida
Too Early To Declare The Program A Success
With North Carolinas managed care program launch on July 1, time will tell if the program is a success. The state certainly seems to check all the boxes when it comes to designing a person-centered care program, but like all state-managed care programs, there will be some hurdles for North Carolina to overcome.
One question is whether or not health plans will offer enough providers in rural areas. This is a challenge that affects patients in all states, so it will be interesting to see how North Carolina approaches the issue.
Another issue is that of the 1.6 million Medicaid beneficiaries in North Carolina, only 200,000 chose their health plan. That left 1.4 million to be auto-enrolled in one of the five health plans. This can create confusion, especially if individuals are assigned to health plans that dont cover their current providers. Enrollees can change their plan assignment in the first 90 days for whatever reason, but this can still cause upheaval and gaps in services and care.
Despite these small hurdles, initially, there are strong hopes for the states Medicaid Managed Care program.
What If I Missed The Deadline Or Chose The Wrong Plan
State health officials anticipate that roughly 15-20 percent of affected enrollees will choose a plan, thats been the experience in other states that have transitioned to managed care.
The rest of the states Medicaid beneficiaries will be enrolled automatically. Everyone including those who chose a plan can switch to a different plan in the first year if the one youre in doesnt suit your needs.
Read Also: How Do I Find My Medicaid Number Online
Unitedhealthcare Dual Complete Plans
Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
How Do I Find Out Which Plan Has My Doctors
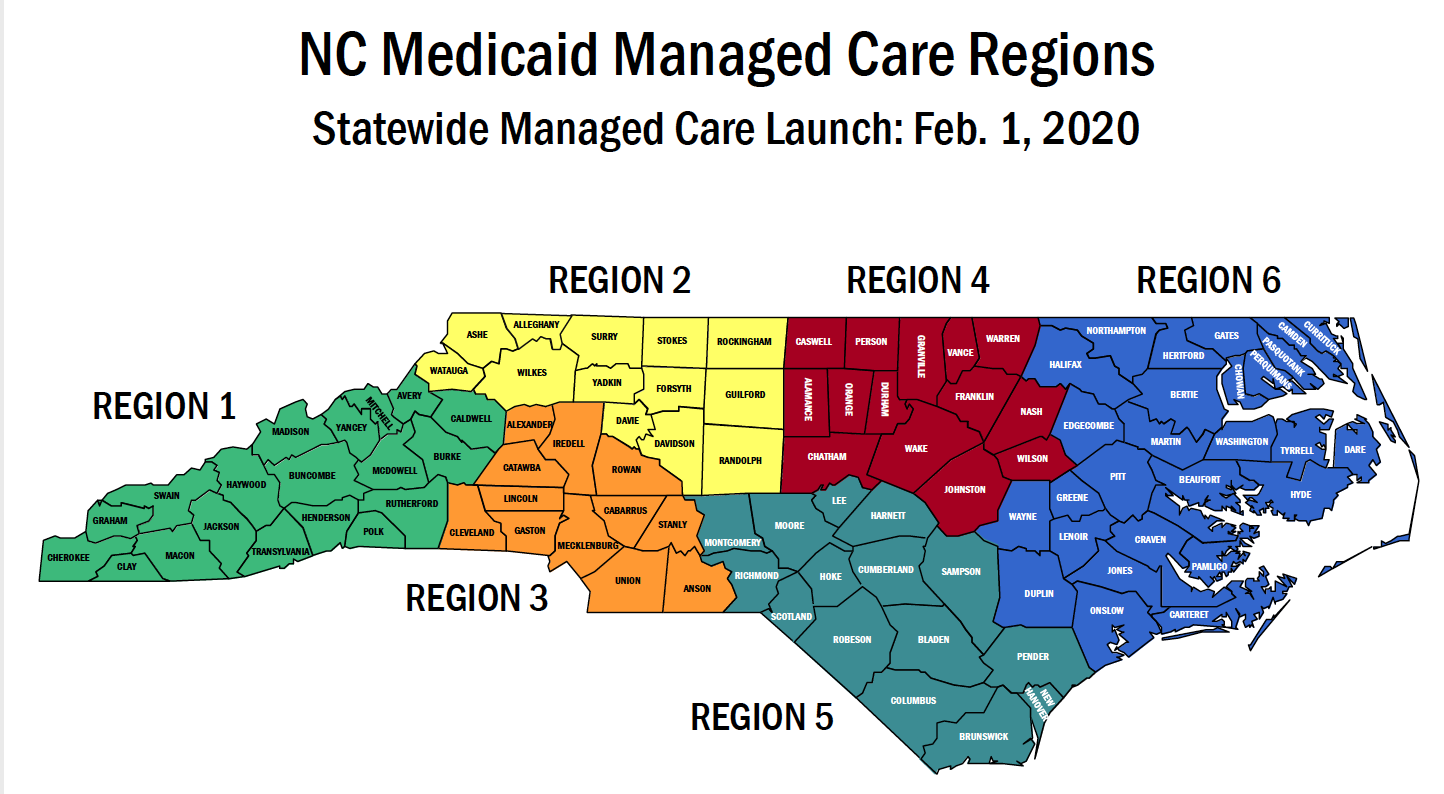
To find out which of the five networks include your current providers, visit the states database. You can also call your doctors office and ask them directly.Sponsor
Be aware that, in some instances, this is changing. Doctors practices are still signing up with the different MCOs, and your favorite physicians might be willing to sign up with one of the MCOs that meet your needs if you ask them.
Recommended Reading: Pediatric Dentist St Louis Medicaid
Find And View Providers And Health Plans
This website has new tools to help you find and view primary care providers and health plans.
Medicaid and NC Health Choice Provider and Health Plan Lookup ToolYou can use the Medicaid and NC Health Choice Provider and Health Plan Lookup Tool to find a PCP. Our new provider search will help you find the best PCP for you and your family.
To search for a provider, go to Find a provider.
Health Care Option GuideYou can use the Health Care Option Guide to view health plans. It will help you choose the best health plan to meet your health care needs.
To view health plans, go to View health plans.
Nc Medicaid Managed Care Launches
Starting July 1, nearly 1.6 million Medicaid beneficiaries in North Carolina began receiving the same Medicaid services in a new way through NC Medicaid Managed Care health plans.
Starting July 1, 2021, most Medicaid beneficiaries began receiving the same Medicaid services in a new way. Called “NC Medicaid Managed Care,” beneficiaries choose a health plan and get care through a health plan’s network of doctors. Some beneficiaries are remaining in traditional Medicaid, which is called NC Medicaid Direct.
Recommended Reading: How Do I Know If My Medicaid Is Still Active
What Is The Ombudsman Program
Our program helps North Carolina Medicaid and NC Health Choice beneficiaries understand the Medicaid program and changes happening as the State moves to NC Medicaid Managed Care. We offer help if people with Medicaid have trouble getting access to health care, and we connect people to resources like legal aid, social services, housing resources, food assistance and other programs. We provide free, confidential support and education about the rights and responsibilities people have under NC Medicaid.
Adding Billing Rendering And Attending Provider Taxonomy To Professional And Institutional Edi Claims
Health plans have identified a common billing error of providers submitting professional and institutional EDI claims with missing or invalid billing provider, rendering provider and attending provider taxonomy codes.
When billing NC Medicaid Direct claims, providers may have directed clearinghouses to append billing provider, rendering provider, or attending provider taxonomy codes to the claims. This process may not have been established for NC Medicaid Managed Care claims being submitted to the prepaid health plans , causing these claims to deny for missing or invalid taxonomies.
Providers should work with their clearinghouses to ensure that the same processes are followed when submitting claims to NC Medicaid Direct and the PHPs.
To facilitate timely adjudication, providers should include the billing provider taxonomy and, when applicable, the rendering provider taxonomy and attending provider taxonomy on claims before sending them to a clearinghouse.
- On professional claims the billing provider taxonomy should be included in EDI loop 2000A and the rendering provider taxonomy, when applicable, should be included in EDI loop 2310B.
- On institutional claims the billing provider taxonomy should be included in EDI loop 2000A and the attending provider taxonomy, when applicable, should be included in EDI loop 2310A.
Read Also: How Do You Apply For Medicaid In Ny
See What Unitedhealthcare Has To Offer
Its your health. Its your choice.
Everyone deserves affordable health care, including you.
That includes working adults, people with disabilities, pregnant women and children.
If thats you, check out UnitedHealthcare Community Plan Medicaid.
We have the Medicaid services and extras that can make a real difference in your life. All at no cost to you.
- Find a doctor you trust in our network.
- Unlimited doctor visits for adults.
- Vision coverage.
- Transportation to and from doctor appointments.
- 24/7 NurseLine to answer your health questions.
Sometimes, you might need a little extra help. Get extras not covered by Medicaid.
- Earn rewards for keeping you and your baby healthy.
- Earn gift cards for getting preventative services.
- Support and treatment to reach a healthy weight.
- Members 18 and older can get free GED Exam Voucher and materials.
We also offer resources to help you make the most of your plan. Including:
- Member Advocates
Visit NC medicaidplans dot gov for more information.
Helping you live a healthier life.
We are here for you, North Carolina
Remember to choose UnitedHealthcare Community Plan.
And get the Plan that gets you more.
To learn more about UnitedHealthcare Community Plan, visit UHCCommunityPlan.com forward slash NC.
Discount valid until 12/31/22. Discount valid only for in-store purchases of eligible Walgreens brand health and wellness products by current members.
Looking for the federal governments Medicaid website? Look here at Medicaid.gov.
Nc Medicaid Specialized Foster Care Plan Update Webinar
Sharing on behalf of DHHS:
The NC Department of Health and Human Services will hold a webinar on June 4, 2021, from noon to 1 p.m. to update the public and interested stakeholders on the development of the Specialized Foster Care Plan.
The Department will review planning efforts underway for the Specialized Foster Care Plan and allow time for questions and answers. The webinar is open to the public and all interested stakeholders.
To register for the webinar simply click the link below. Feel free to share the webinar invitation and registration link with others who may be interested in attending.
Update on North Carolinas Specialized Foster Care Plan
Noon 1 p.m., June 4, 2021: Register in advance
For more information visit the Specialized Foster Care Plan page or contact
Don’t Miss: Who Gets Medicaid In Florida
North Carolina Medical Society Medicaid Transformation Resources
The NCMS has developed a Medicaid Transformation landing page where you can access a wealth of information to help guide you and your practice. Additionally, the NCMS has created a Medicaid Transformation Issues form to log any specific issues you are encountering during this transformation. Information we compile from these online forms will be used to better serve you and your patients as we undergo this transition.
Why Is It Happening What Does It Mean
At a five-year average of $14.83 billion in combined state and federal spending, Medicaid is one of the states biggest budget items. The move will change Medicaid, the largest public insurer in the state, into something that looks and acts more like private health insurance.
Legislators pushed for making the transition back in 2015, arguing that it would give the state more budget predictability while keeping enrollees healthy. The idea is to pay insurers based on health outcomes, such as controlling a patients cholesterol or blood sugar rather than paying for each test, prescription or doctors visit.
North Carolina is the largest state in the country that hasnt yet moved to whats called managed care. Nationwide, more than two-thirds of all Medicaid beneficiaries receive most or all of their care via managed care organizations . Part of the appeal for state lawmakers is that these companies are mandated to deliver quality care but theyre also at risk, meaning that theyre on the hook if costs spiral out of control.
On the other hand, Medicaid is a profitable business for these insurers. Managed care giant Centene, one of the companies that will be providing care in North Carolina, earned $111 billion in revenue and $5 billion in profits in 2020, up from the previous year.Sponsor
Don’t Miss: Colorado Medicaid Customer Service Phone Number
Healthy Opportunities Network Lead Award Update
The North Carolina Department of Health and Human Services has selected organizations to serve three regions of the state, marking a major milestone towards launching the nations first comprehensive program to test evidence-based, non-medical interventions designed to reduce costs and improve the health of Medicaid beneficiaries.
Nc Medicaid Managed Care Health Plan Assignments Completed For Beneficiaries
The North Carolina Department of Health and Human Services announced all Medicaid beneficiaries currently eligible to transition to managed care have selected or been assigned a health plan with 97% enrolled in a plan that includes their current primary care provider in network.
View the entire press release from The Department, published on May 26, 2021
Read Also: Montefiore Medicaid Office Bronx Ny
North Carolinas Shift To Medicaid Managed Care
Since 2005, North Carolina has had a Medicaid Primary Care Case Management system in place to manage the I/DD community. This was a fee-for-service structure designed to provide high-value care with predictable costs, but there was a lack of standardization.
Over time, the North Carolina General Assembly became frustrated with the inability to accurately predict costs. There was a large fluctuation in program costs that made it difficult for the state to budget appropriately. Spurred on by this, in 2015, the General Assembly passed legislation requiring the DHHS to shift from an FFS model to managed care.
Once the legislation was passed in 2015, North Carolina began its transition to managed care. However, the program was tied up in court for over three years.
Companies that lost out on bids for a share of the $30 billion that North Carolina will spend over the next 5 years filed a slew of challenges in court, alleging that the DHHS improperly reviewed and awarded bids. Aetna, one of the companies that filed a challenge in court, lost out on being awarded the bid by a razor-thin margin in the scoring system implemented by DHHS. The motion requested that the contracts be tossed out and the procurement process started over, due to perceived conflicts of interest.
