Medicaid Income Eligibility Chart State By State
The following is each of the states, listed alphabetically. Under your state of residence, you will find all of the relevant information regarding the Medicaid Income Eligibility Chart for each of three programs available: regular, in-home nursing care, and institutional nursing care.
Additionally, each of these programs will have additional information about the income limits for those who are single, married with both spouses applying, and married with only one spouse applying.
Who Can Get Medicaid In North Carolina
You should apply for Medicaid if your income is low and you match one of the descriptions below:
- You think you are pregnant
- The parent or caretaker of a child and/or teenager under the age of 19.
- You are a child or teenager age 18 or under.
- An adult age 65 or older.
- You are legally blind.
- Living with a disability or disabled.
- You are in need of nursing home care.
Top Rated Assisted Living Communities By City
For persons with limited financial resources, Medicaid pays for nursing home care. For those who wish to live at home or in assisted living, sometimes Medicaid will pay for care in those locations if it can be obtained at a lower cost than in a nursing home. It does this through Medicaid Waivers, which are also called Home and Community Based Services Waivers or Waiver Funded Services.
You May Like: What Does It Take To Get Medicaid
What Healthcare Does Medicaid Cover In North Carolina
Through Medicaid, people gain access to health care services that may not be affordable without it. Additionally, some programs and benefits include special protectionssuch as provider network and payment methodsthat help ensure services are accessible. Medicaid also provides preventive care and other services help people stay healthy and avoid costlier care.
Medicaid covers medical and health care services such as:
- Doctors visits
Medicaid does not cover the following types of medical services:
- Cosmetic procedures or surgeries
- Unnecessary hospital expenses, like TV rentals or meals for guests
- Experimental treatments, supplies, equipment or drugs
- Any services not covered under the State Plan for Medical Assistance
Learn more about medical and health care services that are covered by Medicaid in North Carolina on the Division of Health Benefits page here.
How To Make Changes To Your Medicaid Application
North Carolina Medicaid recipients must report changes that can influence their eligibility status within 10 days of the change.
You can report a change in the following ways:
- By phone at 1 662-7030.
- In person at a local Division of Social Services office. Find contact information for local DSS offices in North Carolina here.
Also Check: Medicaid Services Department Frankfort Ky
Medicaid For Applicants Requiring Nursing Home Care
The long-term care Medicaid program covers health care costs for adults who are disabled or age 65 and older who need nursing home care. This program is available for residents of skilled nursing facilities and to applicants who need skilled nursing facility care while living at home in a county with a North Carolina PACE program. Note that skilled nursing care is a higher level of medical need than an adult care home, also known as an assisted living facility, or an independent retirement community. PACE is a Medicaid covered managed care program with the goal of providing the recipient with care at home and at a local PACE facility to prevent the recipient from needing nursing home care.
Family & Childrens Medicaid Recertifications And Changes:
When information is required to complete your FCH Medicaid Recertification, documents must be returned by the due date on the request sent to you. Documents can be mailed in, dropped off using the DSS drop boxes located outside of the DSS building, or dropped off at the scanning area on the 1st floor of the DSS building.
to turn in information on the floor at the receptionist desk.)
For more information contact: 910-323-1540
Don’t Miss: Do I Qualify For Medicaid In Nebraska
Where Can Medicare Beneficiaries Get Help In North Carolina
Seniors Health Insurance Information Program
Free volunteer Medicare counseling is available by contacting the Seniors Health Insurance Information Program at 1-855-408-1212.
The SHIIP can help beneficiaries enroll in Medicare, compare and change Medicare Advantage and Part D plans, and answer questions about state Medigap protections. SHIIP counselors may also be able to provide referrals for home care agencies or long-term care services. This website has more information about the services HIICAP offers.
Elder Law Attorneys
Elder law attorneys can help individuals plan for Medicaid long-term care benefits. The National Academy of Elder Law Attorneys has a search feature beneficiaries can use to find an elder attorney locally.
Medicaid Income Eligibility Chart For 2022
If you are looking into applying to receive Medicaid, whether it is for the first or hundredth time, your eligibility is decided based on your income. However the income eligibility can change from year to year, depending on the economy and what sort of care you require.
The Medicaid Income Eligibility chart is a tool for determining if your income falls under the limit, depending on if you need regular medicaid or Medicaid for long-term nursing care. All you need to do is find the listings for your state, line that up with the care you need, and then you will see the income limit for both single and married applicants.
If you are looking for an overview of the Medicaid Income Eligibility Chart regarding your situation, this is the article you need to read. Here, I will be providing all of the information for each state, type of care, and marital status for those who are trying to learn the facts. Read on to get more information about the benefits that are available to you!
Also Check: New York Medicaid State Plan
Are There Options If I Make More Than The Limit
There might be some options to still receive Medicaid benefits if you make more than the income limit in your state.
The options do differ from state to state, but the majority do offer a pathway for those who would be considered medically needy and have high medical expenses.
If someone who requires a lot of medical care has too high of an income, they might be able to spend that income on their medical costs and then have that count against their income.
For example, if someone was $500 over the income limit in their state and that state has a program for the medically needy, they might be permitted to spend that excess income on their medical expenses and then receive Medicaid benefits after. This helps those with high than average medical costs be put on more equal footing for income eligibility requirements.
Not every state offers this particular program, however. For a great resource on the sorts of waivers, exceptions, and other eligibility information, visit this website. Once you click on your state of residence, you should be able to see which waivers are available in your state for those who exceed the income limit.
Overview Of Medicaid For Long
Long-term care becomes medically necessary for many individuals as they age, and as the number of people requiring care increases, so do the costs of services. According to Genworth Financial, a North Carolina resident can expect to spend between $53 – $250 per day on long-term care, making it difficult for low-income seniors to pay for their care.
The increasing costs of long-term care have encouraged thousands of seniors to apply for Medicaid in hopes of receiving assistance to pay for their care. Medicaid is funded and operated jointly by the Federal government and the State of North Carolina, with the Federal government paying for 66.9% of Medicaids budget. For every $1 North Carolina spends on Medicaid, the federal government will spend $2.02.
Medicaid for long-term care is available to anyone over the age of 65 who meets the programs medical and financial requirements. If a person requires a nursing home level of care and they fall within Medicaids income and asset limits, they may receive benefits to pay for long-term care. Those who do not meet Medicaids income requirements may also qualify to receive benefits if they participate in a spend down program.
Recommended Reading: Dental Places That Accept Medicaid
Does North Carolina Help With My Medicare Premiums
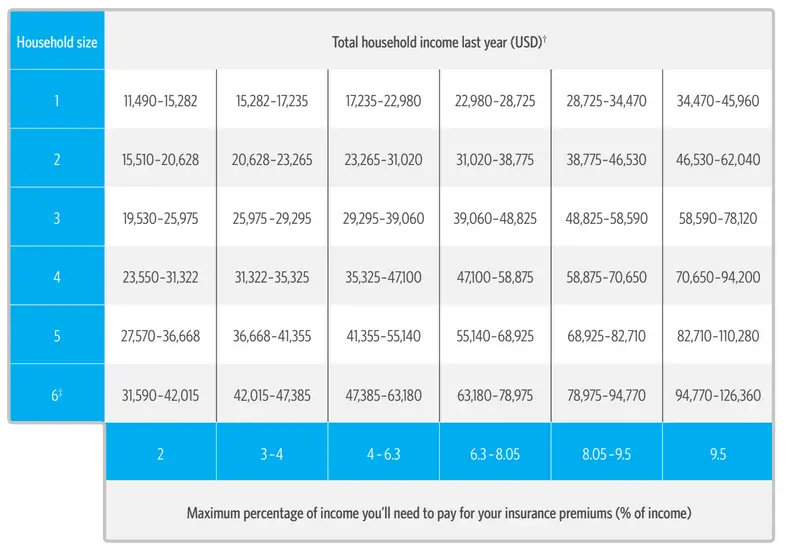
Many Medicare beneficiaries who struggle to afford the cost of Medicare coverage are eligible for help through a Medicare Savings Program . In North Carolina, these programs pay for Medicare Part B premiums, Medicare Part A and B cost-sharing, and in some cases Part A premiums.
- Comprehensive Medicare-Aid : The income limit is $1,063 a month if single and $1,437 a month if married. MQB-Q pays for Part A and B cost sharing, Part B premiums, and if a beneficiary owes them it also pays their Part A premiums.
- Limited Medicare-Aid : The income limit is from QMB levels up to $1,276 a month if single and $1,724 a month if married. MQB-B pays for Part B premiums.
- Limited Medicare-Aid Capped Enrollment : The income limit is from SLMB levels up to $1,436 a month if single and $1,940 a month if married. MQB-E pays for Part B premiums.
MSP asset limits: There asset limits for MQB-Q, MQB-B and MQB-E are $7,860 if single and $11,800.
North Carolina Medicaid Income Limit Charts
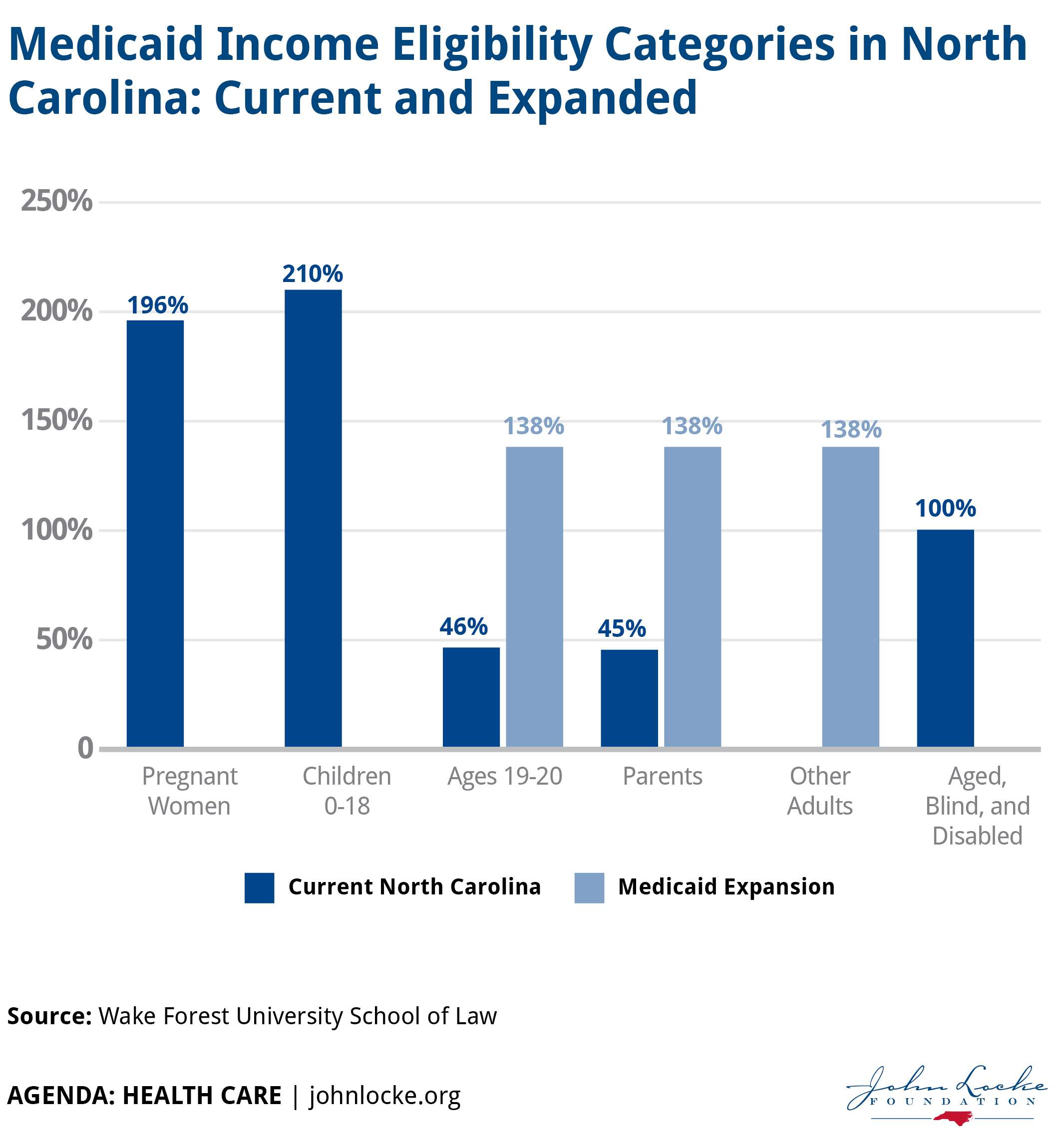
The North Carolina Medicaid eligibility income limit charts are divided by groups.
For example, the first chart is focused on income limits for children who qualify for Medicaid.
Similarly, the second chart below focuses on the Medicaid income limits for adults in North Carolina who qualify for Medicaid.
North Carolina Medicaid Income Limit for Children
Below is the income limit for children by age category. Find the age category your child falls into and you will see the income limit by household size.
| North Carolina Medicaid Income Limit Children |
| Children Medicaid Ages 0-1 |
| N/A |
How to Read the North Carolina Medicaid Income Limits Charts Above
You cannot have an income higher than the Federal Poverty Level percentage described for your group to be eligible for Medicaid.
Similarly, when you identify the income group that applies to you, the income limit you see refers to the maximum level of income you can earn to qualify for benefits.
For example, if you are pregnant, to qualify for Medicaid, you cannot have an income higher than 196% of the Federal Poverty Level which for a family of two is $34,143 as shown in the chart above.
Also Check: How Do I Change My Primary Care Physician For Medicaid
What Do I Need For Proof Of Income
In order to prove that you fall within the limit for income eligibility, you will need to provide documentation of all sources of income that you have.
Documents to include are things like pay stubs from wages, copies of social security deposits, copies of alimony checks, and award letters from any other monthly financial benefit that you may receive.
It would also be helpful to have all of your most recent income tax returns and any other tax forms that would be relevant to verifying your income.
Some states are able to electronically gather the resources to verify your income, which does simplify the process as well as eliminate fraud. To find out if your state has this technology for your application, click here to learn more about the application process in your state of residence.
Who’s Eligible For Medicaid For The Aged Blind And Disabled In North Carolina
Medicare covers a great number services including hospitalization, physician services, and prescription drugs but Original Medicare doesnt cover important services like vision and dental benefits. Some beneficiaries those whose incomes make them eligible for Medicaid can receive coverage for those additional services if theyre enrolled in Medicaid for the aged, blind and disabled .
In North Carolina, Medicaid ABD covers preventive and restorative care, as well as dentures and oral surgery services for adults. However, Medicaid ABD does not cover routine eye visits or eyeglasses for adults.
This is the same income limit as MQB-Q meaning MQB-Q enrollees who meet Medicaids more restrictive asset limit receive full Medicaid benefits.
Asset limits: The asset limit is $2,000 if single and $3,000 if married.
North Carolinas Medicaid spend-down for Medicaid ABD benefits and long-term care
In North Carolina, applicants with incomes higher than the eligibility limit for Medicaid for the aged, blind and disable can enroll in the Medicaid spend-down, which allows medical bills to be subtracted from income that is counted toward the Medicaid eligibility limit. This is called the Medicaid Deductible program in North Carolina.
Also Check: Find A Neurologist That Takes Medicaid
North Carolina Medicaid Income Limit
The North Carolina Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the North Carolina Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 210 percent of FPL
- Any child age 1-5 with a family income up to 210 percent of FPL
- Children ages 6- 18 with family income up to 133 percent of FPL
- CHIP for children with family income up to 211 percent of FPL
- Pregnant women with family income up to 196 percent of FPL
- Parents of minor children with family income up to 41 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 100% of the FPL
How To Find Out Who Meets The Requirements For Medicaid
What are the requirements for Medicaid? You can get basic information on NC Medicaid benefits eligibility through the following:
Since Medicaid applications are time-consuming, it is to your benefit to ensure you qualify for Medicaid benefits before engaging in the process. If you do not qualify for Medicaid and decide to file your paperwork regardless, the outcome will most likely remain the same. Save valuable time by confirming your eligibility status beforehand.
Read Also: Yearly Income To Qualify For Medicaid
What Happens To My Medicaid If I Move
North Carolina Medicaid recipients must report changes that can influence their eligibility status, including relocating to a new address.
If you move to a new residence within North Carolina, you can update your address with the North Carolina Division of Social Services in the following ways:
- By phone at 1 662-7030.
- In person at a local Division of Social Services office. Find contact information for local DSS offices in North Carolina here.
Note: Medicaid benefits do not transfer. If you move to a new state, you must reapply for Medicaid in your new location. If you have further questions about moving with Medicaid, visit the national Medicaid Contact Us here.
Planning For Medicaid In North Carolina
Prior to applying for Medicaid, its important for applicants to plan how they will use their resources. If an applicant improperly transfers their assets to a friend or family member, Medicaid may assume they are doing so to make it more likely for them to receive benefits. However, Medicaid expects all beneficiaries to use their resources to pay for their care before receiving assistance, and may therefore penalize an applicant who initiates any uncompensated transfers.
When a person applies for Medicaid coverage of long-term care, they are subject to a lookback period of sixty months . The lookback period occurs directly prior to when a person applies for Medicaid, and Medicaid may evaluate any transfers which may have occurred during the lookback period to assess their validity. Any uncompensated transfers the applicant initiates may qualify as gifts, and may incur penalties as a result.
Applicants can avoid Medicaid penalties by documenting their transfers and avoiding probate. If a person completes a transfer properly, they may not face a penalty period, making it crucial for applicants to plan ahead before applying to Medicaid.
Read Also: What Is The 1 800 Number For Medicaid
Food And Nutrition Services
The Food and Nutrition Program is a federal food assistance program that provides low-income families a monthly supplemental allotment of benefits issues via Electronic Benefit Transfer cards . The Food stamp program is an entitlement program, so all eligible individual and households can receive assistance.
You may be eligible for Food and Nutrition Services if your total income falls below the appropriate gross income limits for your household size. Eligibility workers determine which income limit applies to your household.
Eligible individuals will receive Food and Nutrition benefits no later than thirty days from the date of application. Individuals with special circumstances will be given an opportunity to receive Food and Nutrition benefits within seven days of the application. View more information apply through the North Carolina Health and Human Servicess online program.
Family & Childrens Medicaid

Family and Childrens Medicaid is a health insurance program that serves low-income individuals, children, and parents. For information regarding the different types of Medicaid in North Carolina and to see if you are potentially eligible, visit the Division of Medical Assistance web site at
AM I ELIGIBLE?
- To be eligible for Medicaid, you must be a US Citizen or provide proof of eligible immigration status unless you are only applying for emergency services.
- You must live in North Carolina and provide proof of residency
- You must have a social security number or have applied for one.
- Income and resource limits vary depending on the Medicaid Program and eligibility.
APPLYING FOR FAMILY & CHILDRENS MEDICAID:
- Apply online at
- Apply at Johnston County DSS at 714 North Street Smithfield NC 27577. Applications are taken between 8:00 am to 5:00 pm, Monday Friday
- Mail In Application: https://dma.ncdhhs.gov/medicaid/get-started/apply-for-medicaid-or-health-choice
- Request that an application be mailed to you by calling 919-989-5300
FAMILY & CHILDRENS MEDICAID RECERTIFICATIONS AND CHANGES:
When information is required to complete your FCH Medicaid Recertification, documents must be returned by the due date on the request sent to you. Documents can be mailed in, dropped off using the DSS drop boxes located outside of the DSS building, or dropped off at the inside drop box of building 1.
Contact Us
Domestic Violence
Also Check: Does Medicare Or Medicaid Cover Cremation
