Disability Advocates Praise New York State Medicaid Policy Changes
The new guidelines, which will took effect on February 1, come after a string of complaints from people with disabilities whose Medicaid insurance plans refused to cover wheelchairs appropriate to their needs. For years, vague and conflicting language in New York States Medicaid guidelines has encouraged insurance plans to refuse to pay for wheelchairs needed for use outside of a persons home, leaving many individuals with disabilities stranded.
Problems Prompt Calls for Change
In one case, a man with cerebral palsy who is able to get around his home with a walker but who needs a wheelchair to venture outside his home was told by his insurer that Medicaid does not pay for wheelchairs for use outside the home, a position not supported by longstanding regulations. Though that decision denying the mans wheelchair was reversed at a fair hearing and he eventually received the equipment he needed, that process took seven months after his doctor requested that he be provided with a wheelchair. For those seven months he was stranded without the chair he needed.
ICS, a nonprofit that runs the first and only Health Home dedicated to the needs of people with physical disabilities, also wrote a white paper for the States review to support the advocacy effort.
Disability Advocates applaud Medicaid guidelines change
Wheelchair users say change was long overdue
Christopher Engelhardt
Medicaid Cancer Treatment Program
The Medicaid Cancer Treatment Program for breast and/or cervical cancer or colorectal and/or prostate cancer provides full Medicaid coverage for individuals whose income is higher than the Medicaid medically needy income levels. See below, Additional Medicaid Benefits, Medicaid Cancer Treatment Program.
A New Standardized Task
The 2020 Budget required DOH to develop a uniform “tasking tool” that would wpresumably translate findings made in the Uniform Assessment System nurse assessment into a plan of care with the number of hours to be approved. The law says the tool must be evidence-based and used to assist managed care plans and local departments of social services to make appropriate and individualized determinations for … the number of personal care services and CDPAP hours of care each day. The tool is supposed to identify how Medicaid recipients’ needs for assistance with activities of daily living can be met through telehealth and family and social supports. .
In early May 2021, DOH posted a Request for Information for the new Uniform Tasking Tool.
This was never implemented and Gov. Hochul’s proposed Budget for 2022-23 would abandon this effort and instead just issue guidelines and standards for plans and local districts to make appropriate and indivdiualized determinations for utilization.
Side note: How would telehealth assist with preparing meals and assisting a consumer with transferring and toileting?!
Also Check: Neurologist In Alexandria La That Accept Medicaid
States Are Looking To Medicaid Mcos To Develop Strategies To Identify And Address Social Determinants Of Health
Many states are leveraging MCO contracts to promote strategies to address social determinants of health. For FY 2020, over three-quarters of the 41 MCO states reported leveraging Medicaid MCO contracts to promote at least one strategy to address social determinants of health . For FY 2020, about three-quarters of MCO states reported requiring MCOs to screen enrollees for social needs providing enrollees with referrals to social services or partnering with community-based organizations . Almost half of MCO states reported requiring MCOs to employ community health workers or other non-traditional health workers . KFFs 2017 survey of Medicaid managed care plans found that a majority of plans were actively working to help beneficiaries connect with social services related to housing, nutrition, education, or employment.
Figure 13: State MCO Contract Requirements Related to Social Determinants of Health, FYs 2019-2020
Topics
How Will The Consumer Choose A Plan
- If the consumer has a primary care provider who belongs to any Nassau County contracted health plan, they can choose that plan.
- They can call any doctor. If that doctor belongs to any Nassau County contracted health plan, they can choose that one.
- They can look at the list of providers for each health plan and choose from the list.
- If the consumer does not choose a health plan voluntarily within 60 days of notice to do so, they will automatically be assigned to a health plan.
Read Also: Blue Cross Blue Shield Medicaid
What Is A Medicaid State Plan And A State Plan Amendment
A Medicaid State Plan is a written agreement between a state and the federal government outlining the details of the states Medicaid program, including benefits, provider rate methodologies, and who is eligible for coverage. It gives an assurance that a state will abide by federal rules, which allows the state to claim federal Medicaid matching funds. See Californias Medicaid State Plan for an example of how a Medicaid State Plan is organized.
To make changes to the Medicaid State Plan, a state submits a state plan amendment to the Centers for Medicare and Medicaid Services for review and approval. An approved SPA results in permanent changes to the states Medicaid program, and may include content such as the addition of new populations or providers, changes in benefit coverage, changes in what administrative expenditures the state expects the federal government to pay for , and changes in reimbursement methodologies.
It is important to note that CMS approval of SPAs is guided by the statutory and regulatory terms and conditions of the Medicaid program including, but not limited to:
- Comparable benefits must be available to all eligibility groups to which the benefit package applies
- Benefits must be offered statewide and
- Beneficiaries must have the freedom to choose their provider .
A searchable list of SPAs that have been approved by CMS can be found here.
How To Apply For Medicaid In In New York
Due to the fact that you must stick to specific instructions with regards to submitting your paperwork, the application guidelines are different in New York than those in other states. The qualifying criteria are actually spread into two separate groups. These are MAGI and non-MAGI groups. You have to file differently depending on which group you fall into.
When it comes to MAGI application guidelines, this group includes foster children, children under 19, beneficiaries of the FPBP , relatives of caregivers or parents, women undergoing fertility treatments and pregnant women. If you fall into this group, you will have to apply for the Medicaid program via the New York State Department of Health Marketplace.
To be eligible under the non-MAGI eligibility group, you must be a recipient of one of the following:
- Medicaid Cancer Treatment Program
- ADC-related medical needy, or the
- Medicare Savings Program
If you belong to this group, you should apply for Medicaid at your local Department of Social Services.
You May Like: How To Become A Medicaid Consultant
Lookback Likely Delayed Until At Least April 1 2022 And Possibly Not Until July 1 2022
See more about how the lookback will be implemented here and in the webinar – link below.
NYLAG Evelyn Frank program director Valerie bogart has conducted several webinars on the changes:
-
View January 26, 2022 recorded webinar hereand download PowerPoint here
-
Note that since this webinar conducted, implementation date has been delayed to May 1, 2022 for Independent Assessor.
View May 21, 2021 recording of Elder Law Forum sponsored by Pierro, Connor & Strauss LLP – with speakers Valerie Bogart of NYLAG, Al Cardillo of the Home Care Association, a Medicaid Home Care Application Case Study, and a panel on Medicaid home care fair hearings.
Click here for agenda and . . Click here for link to all videos.
Children And Adults Are More Likely To Be Enrolled In Mcos Than Seniors Or Persons With Disabilities However States Are Increasingly Including Beneficiaries With Complex Needs In Mcos
As of July 2019, 36 MCO states reported covering 75% or more of all children through MCOs . Of the 34 states that had implemented the ACA Medicaid expansion as of July 2019,6 29 were using MCOs to cover newly eligible adults and the large majority of these states covered more than 75% of beneficiaries in this group through MCOs. Thirty-two MCO states reported covering 75% or more of low-income adults in pre-ACA expansion groups through MCOs. In contrast, only 21 MCO states reported coverage of 75% or more of seniors and people with disabilities. Although this group is still less likely to be enrolled in MCOs than children and adults, over time, states have been moving to include seniors and people with disabilities in MCOs.
Figure 4: MCO managed care penetration rates have grown across Medicaid eligibility groups
Also Check: When Does Medicaid End For A Child In Nc
Dental Care That Keeps You Smiling
Healthfirst believes that providing you with good dental care is important to your overall healthcare. Covered services include regular and routine dental services such as preventive dental checkups, cleanings, X-rays, fillings, and other services to check for any changes or abnormalities that may require treatment and/or follow-up care for you. You do not need a referral from your PCP to see a dentist.
Unitedhealthcare Senior Care Options Plan
UnitedHealthcare SCO is a Coordinated Care plan with a Medicare contract and a contract with the Commonwealth of Massachusetts Medicaid program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is a voluntary program that is available to anyone 65 and older who qualifies for MassHealth Standard and Original Medicare. If you have MassHealth Standard, but you do not qualify for Original Medicare, you may still be eligible to enroll in our MassHealth Senior Care Option plan and receive all of your MassHealth benefits through our SCO program.
Also Check: Income To Qualify For Medicaid
Obtaining An Additional 1% Federal Medicaid Match: Us Preventive Services Task Force
States can obtain a one percentage point federal match rate increase for covered preventive services when covering and reimbursing all USPSTF grade A and B preventive services and approved vaccines recommended by the Advisory Committee on Immunization Practices , and their administration, without cost-sharing. If the state utilizes a managed care delivery system, it must also make these services available to those enrolled in managed care and the one percentage point increase will be applied to the managed care expenditures.
Covering the National DPP lifestyle change program at no cost to members may also aid states in securing this additional 1% federal Medicaid match. For states pursuing the one percentage point increase in their FMAP per Section 4106 of the ACA, the counseling requirements referenced in the following recommendations can be met through coverage of the National DPP lifestyle change program.
Abnormal Blood Glucose and Type 2 Diabetes Mellitus: Screening. The USPSTF recommends screening for abnormal blood glucose in adults aged 35 to 70 years who are nonpregnant, overweight, or obese. Clinicians should offer or refer patients with abnormal blood glucose to effective preventive interventions.
Coverage of the National DPP lifestyle change program is also indirectly related to two additional USPSTF grade A and B preventive services. These services reference National DPP lifestyle change program inclusion criteria.
Disabled Adult Child Provision
Under certain circumstances when SSI recipients become entitled to Social Security Disability Insurance benefits based on their parents record, they may lose their SSI cash benefits. However, they should continue to maintain their Medicaid benefits, even if over the income guidelines. This is known as the Disabled Adult Child Provision. See below, Additional Medicaid Benefits, Disabled Adult Child Provision.
Read Also: Nursing Homes In Huntsville Al That Take Medicaid
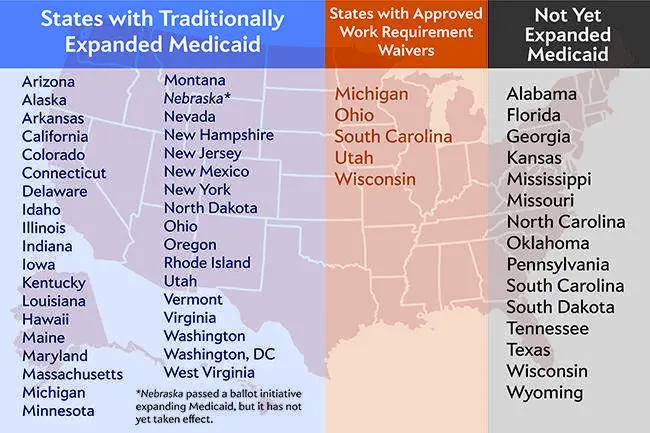
New York Has Accepted Federal Medicaid Expansion
- 7,201,854 Number of New Yorkers covered by Medicaid/CHIP as of September 2021
- 1,523,437 Increase in the number of New Yorkers covered by Medicaid/CHIP fall 2013 to September 2021
- 47% Reduction in the uninsured rate from 2013 to 2017
- 20% Increase in total Medicaid/CHIP enrollment in New York since Medicaid expansion took effect
Hochul Shells Out Billions To Help Herself Not Ny Taxpayers
If Hochuls plan becomes law, the state will need to handle the transition carefully: Do whatevers necessary to limit the chaos and expense of the bidding process. Guard against corruption by making the process fully transparent, with pre-established criteria for choosing winners.
And why on Earth does Hochul suggest considering whether plan providers are for-profit companies? If they offer the best product at the lowest cost, who cares if they make a profit?
All this, of course, amounts to a modest reform of a Medicaid program that costs more than $80 billion a year and, though meant for the poor, covers nearly 40% of the states population. But small steps for small feet.
Lets just hope any improvements the state makes to this part of the program more than offset any damage it causes.
Read Also: What Does My Medicaid Cover
/7 Access To Telemedicine With Teladoc*
Talk to a doctor any timefor a $0 copay. Connect with board-certified doctors through video chat or phone for prescriptions, help diagnosing and treating non-emergency conditions, and more. Access to dermatologists is also available.
*Telemedicine isnt a replacement for your Primary Care Provider . Your PCP should always be your first choice for care .
See better with Healthfirst Vision Benefits
American Disabilities Act Notice
In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
Read Also: Apply For Sc Medicaid Online
See Better With Healthfirst Vision Benefits
Taking care of your eyes doesnt just mean having clear vision. An annual eye exam can help detect a number of health risks, such as diabetes, thyroid disease, high blood pressure, and other conditions. Healthfirst has made it easy for our members to take advantage of this often overlooked preventive service by providing access to comprehensive vision care.
Dental Care That Keeps You Smiling
Unitedhealthcare Connected Benefit Disclaimer
This is not a complete list. The benefit information is a brief summary, not a complete description of benefits. For more information contact the plan or read the Member Handbook. Limitations, copays and restrictions may apply. For more information, call UnitedHealthcare Connected® Member Services or read the UnitedHealthcare Connected® Member Handbook. Benefits, List of Covered Drugs, pharmacy and provider networks and/or copayments may change from time to time throughout the year and on January 1 of each year.
You can get this document for free in other formats, such as large print, braille, or audio. Call , TTY 711, 8 a.m. – 8 p.m., local time, Monday – Friday . The call is free.
You can call Member Services and ask us to make a note in our system that you would like materials in Spanish, large print, braille, or audio now and in the future.
Language Line is available for all in-network providers.
Puede obtener este documento de forma gratuita en otros formatos, como letra de imprenta grande, braille o audio. Llame al , TTY 711, de 08:00 a. m. a 08:00 p. m., hora local, de lunes a viernes correo de voz disponible las 24 horas del día,/los 7 días de la semana). La llamada es gratuita.
Puede llamar a Servicios para Miembros y pedirnos que registremos en nuestro sistema que le gustaría recibir documentos en español, en letra de imprenta grande, braille o audio, ahora y en el futuro.
Los servicios Language Line están disponibles para todos los proveedores dentro de la red.
Read Also: Braces Place That Take Medicaid
On Nov 8 2021 State Doh Posted A Webinar Issued Clarifying Which Of The Recent Personal Care And Cdpap Regulation Changes Will Go Into Effect On Nov 8 2021
This explains further their letter of Nov. 1, with this info
Final regulations were posted on the NYS DOH website on August 31, 2021 published in the NYS Register on Sept. 8, 2021. Direct link to regulation is here. The regulations have an effective date of Nov. 8, 2021, but much of it will be delayed. We are disappointed that the final regulations are virtually same as the proposed state regulations to which NYLAG and other organizations submitted in March 2021. Most of our recommendations were rejected.
WHAT STARTS NOVEMBER 8, 2021 – The regulation cuts back on consumer rights after a “Transition Period.” These changes will make it easier for a plan to reduce hours after a consumer is required to transition to a new MLTC plan. This could be after their old plan closes, or after they received Immediate Need services for 120 days, or after they first became enrolled in Medicare and had previously received home care from a “mainstream” Medicaid managed care plan. Read more about these transition rights and how they are changing along with advocacy tips, here.
-
WHAT IS DELAYED: The new minimum of 3 ADLs for home care and MLTC, and the new Independent Assessor procedures, both of which were enacted in the 2020 State budget will NOT be implemented yet, new date not yet announced. Read about the home care changes here . Some of these changes await CMS approval because of “maintenance of effort” requirements of the ARPA COVID relief legislation.
Read about the .
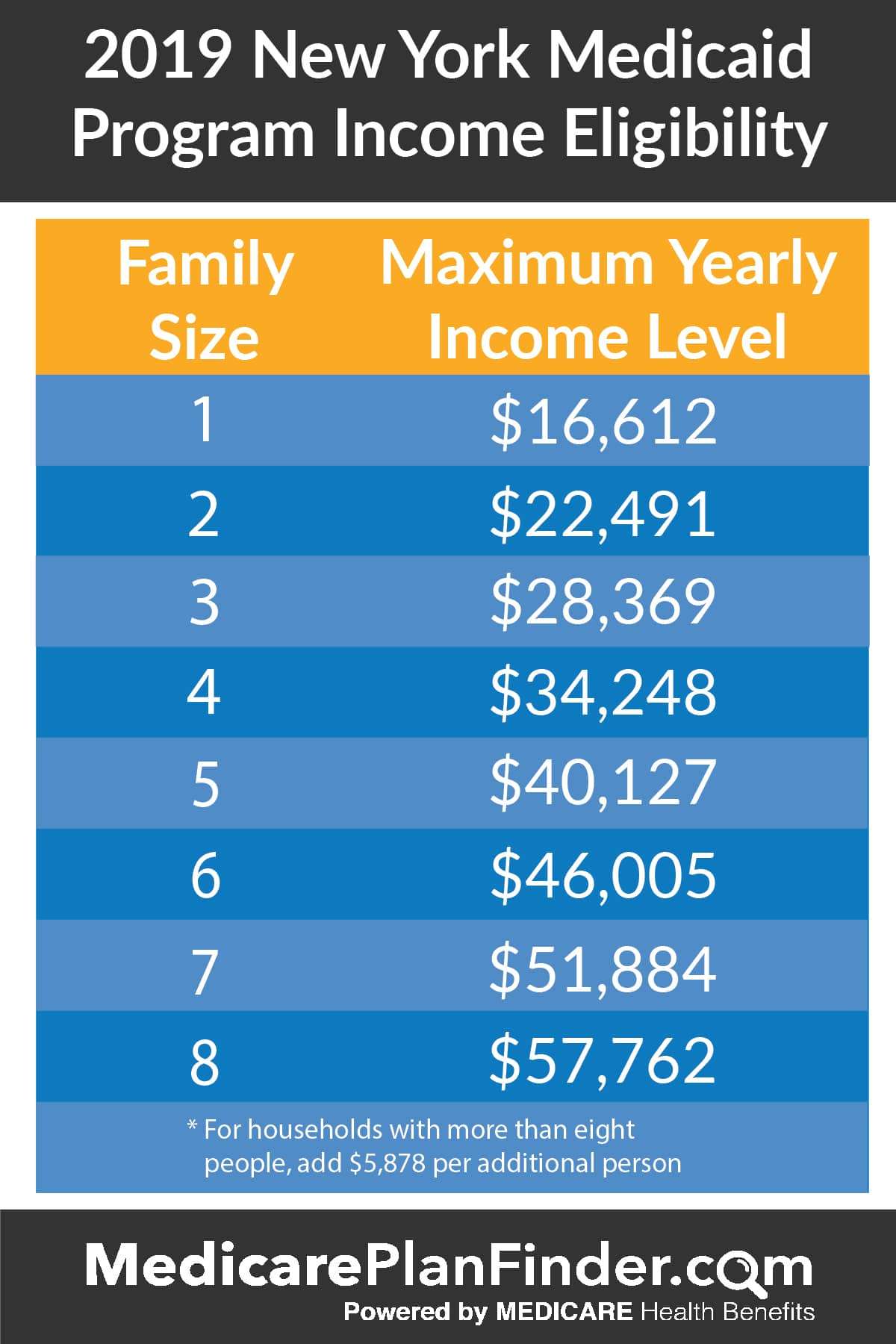
Income Requirements For New York Medicaid

The income requirements for Medicaid are based on various resource levels for the state. For example, the income requirements for people who are over the age of 65, blind, or otherwise disabled are different than they are for people who are single or who are married but without any children. Additionally, assets are to be accounted for. When it comes to getting around the Medicaid financial requirements, you can only have more money if you are over 65, a child, pregnant, blind, or otherwise disabled.
In general, you can only have income that is not over 138% of the FPL for your size family or household. If you would like to see specifics as far as what you can earn for your household size, click here.
Don’t Miss: Is Nebraska Total Care Medicaid
