Once I Am Receiving Medicare Can I Keep My Same Provider
Check with your provider to see if they accept your new Medicare coverage. Some providers may not accept your new coverage.
Any Apple Health coverage you are approved for when you are receiving Medicare will work as a secondary insurance to Medicare. This means that Medicare will pay first, and other coverage will pay after that.
If you are not eligible for Medicare, you may be eligible to purchase a Qualified Health or Dental Plan through Washington Healthplanfinder. You can explore your options:
- Online: Visit Washington Healthplanfinder and login to your account
- Mobile app: Download the WAPlanfinder app to create an account and apply for coverage. Available on the App Store and Google Play.
- Phone: Call the Washington Healthplanfinder Customer Support Center at 1-855-923-4633
Does Washington Help With My Medicare Premiums
Many Medicare beneficiaries who struggle to afford the cost of Medicare coverage are eligible for help through a Medicare Savings Program . In Washington, these programs pay for Medicare Part B premiums, Medicare Part A and B cost-sharing, and in some cases Part A premiums.
- Qualified Medicare Beneficiary : The income limit is $1,064 a month if single and $1,437 a month if married. QMB pays for Part A and B cost sharing, Part B premiums, and if a beneficiary owes them it also pays their Part A premiums.
- Specified Low-income Medicare Beneficiary : The income limit is from SLMB levels up to $1,276 a month if single and $1,724 a month. SLMB pays for Part B premiums.
- Qualifying Individuals : The income limit is from SLMB levels up to $1,436 a month if single and $1,940 a month if married. QI pays for Part B premiums.
- Qualified Disabled Working Individuals : The income limit is $2,127 a month for applicants who live alone and $2,874 a month for applicants who live with another person. QDWI pays the Part A premiums owed by certain disabled beneficiaries who have returned to work.
MSP asset limits: The asset limit for QMB, SLMB and QI is $7,860 if single and $11,800 if married. QDWIs asset limit is $4,000 for applicants living alone and $6,000 for applicants living with another person.
Certain assets are not counted including a first home, household belongings, one car, and some prepaid burial plans.
Unitedhealthcare Connected For Mycare Ohio
UnitedHealthcare Connected® for MyCare Ohio is a health plan that contracts with both Medicare and Ohio Medicaid to provide benefits of both programs to enrollees. If you have any problem reading or understanding this or any other UnitedHealthcare Connected® for MyCare Ohio information, please contact our Member Services at from 7 a.m. to 8 p.m. Monday through Friday for help at no cost to you.
Si tiene problemas para leer o comprender esta o cualquier otra documentación de UnitedHealthcare Connected® de MyCare Ohio , comuníquese con nuestro Departamento de Servicio al Cliente para obtener información adicional sin costo para usted al de lunes a viernes de 7 a.m. a 8 p.m. .
Also Check: Medicaid Cost Sharing With Medicare
Washington Copes Medicaid Waivers Program
PayingForSeniorCare is committed to providing information, resources, and services free ofcharge to consumers that help seniors and their families make better decisions about senior living and care.
We may receive business-to-business compensation from senior care partnerships and/or website advertising. This compensation doesnt dictate our research and editorial content, nor how we manage our consumerreviews program. PayingForSeniorCare independently researches the products and services that oureditorial team suggests for readers. Advertising and partnerships can impact how and where products,services, and providers are shown on our website, including the order in which they appear, but theydont determine which services or products get assessed by our team, nor which consumer reviews getpublished or declined.
PayingForSeniorCare.com awards some companies with badges and awards based on our editorial judgment. We dont receive compensationfor these badges/awards: a service provider or product owner may not purchase the award designation orbadge.
Learn moreabout our mission and how we are able to provide content and services to consumers free of charge.
American Disabilities Act Notice
In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
You May Like: How Do I Know If My Medicaid Is Still Active
Washington Medicaid Income Limit Charts
The Washington Medicaid eligibility income limit charts are divided by groups.
For example, the first chart is focused on income limits for children who qualify for Medicaid.
Similarly, the second chart below focuses on the Medicaid income limits for adults in Washington who qualify for Medicaid.
Washington Medicaid Income Limit for Children
Below is the income limit for children by age category. Find the age category your child falls into and you will see the income limit by household size.
| Washington Medicaid Income Limit Children |
| Children Medicaid Ages 0-1 |
| $59,398 |
How to Read the Washington Medicaid Income Limits Charts Above
You cannot have an income higher than the Federal Poverty Level percentage described for your group to be eligible for Medicaid.
Similarly, when you identify the income group that applies to you, the income limit you see refers to the maximum level of income you can earn to qualify for benefits.
For example, if you are pregnant, to qualify for Medicaid, you cannot have an income higher than 193% of the Federal Poverty Level which for a family of two is $33,621 as shown in the chart above.
Washington Has Accepted Federal Medicaid Expansion
- 1,965,401 Number of Washingtonians covered by Medicaid/CHIP as of May 2021
- 847,825 Increase in the number of Washingtonians covered by Medicaid/CHIP fall 2013 to May 2021
- 54% Reduction in the uninsured rate from 2010 to 2019
- 76% Increase in total Medicaid/CHIP enrollment in Washington since 2013
Don’t Miss: How To Get Help With Medicaid
How To Apply For Medicaid Online In Washington
Candidates can apply for Medicaid in Washington online if they are 18 years of age or older. Where do you sign up for Medicaid online? File a WA Medicaid application via web by visiting the Washington HealthPlanFinder website. Once there, applicants will be asked to enter required information to create an account.
To apply for Medicaid online, have the following details handy:
- The year in which an applicant is seeking coverage
- ZIP code
- Estimated household income
- Pay frequency
The above information is used to determine the Medicaid eligibility of an interested beneficiary. When a candidate chooses to apply for Medicaid online, the electronic system utilizes personal information and income details to generate estimated results. The web-based Medicaid application forms then produce eligible government-sponsored health plans to join.
Since the Medicaid online application requires further review, be on the lookout for correspondence regarding true Medicaid eligibility following a Medicaid application submission. Feel free to follow up directly with a Washington Medicaid representative if need be.
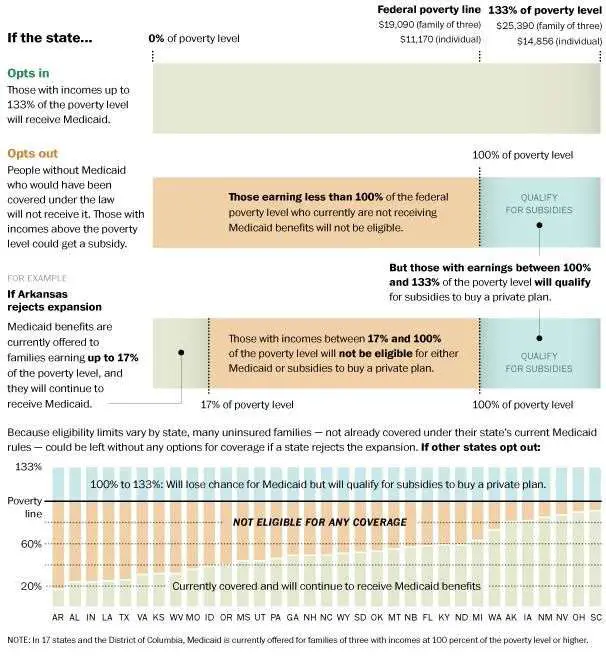
Expansion Under The Affordable Care Act
The Affordable Care Act provided for the expansion of Medicaid to cover childless adults whose income is 138 percent of the federal poverty level or below. The provision for expanding Medicaid went into effect nationwide in 2014. As of November 2018, a total of 36 states and Washington, D.C., had expanded or voted to expand Medicaid.
Washington expanded Medicaid under the Affordable Care Act in 2014. GovernorJay Inslee expressed support for Medicaid expansion in 2013 when he stated that it is “as close as what you might call a ‘no brainer’ as there is in state government.”
Support
Arguing in support of the expansion of Medicaid eligibility, the Center for American Progress states that the expansion helps increase the number of people with health insurance and benefits states economically. The organization argues that by providing health insurance to those who would otherwise be uninsured, Medicaid expansion allows low-income families to spend more money on food and housing:
| â | Medicaid coverage translates into financial flexibility for families and individuals, allowing limited dollars to be spent on basic needs, including breakfast for the majority of the month or a new pair of shoes for a job interview. | â |
| âCenter for American Progress |
Opposition
The National Federation of Independent Business also advocated against Medicaid expansion in February 2017, arguing that the federal government may not always agree to cover 90 percent of the costs:
Recommended Reading: Pregnancy Medicaid Florida Phone Number
What Is Washington Medicaid
Washington Medicaid pays for low-income residents to receive medical and behavioral care services provided by professionals throughout the state. Known as Apple Care, Washington’s Medicaid program covers a wide variety of services, including preventive care, diagnostic screenings and treatment for acute and chronic illnesses.
Medicaid Coverage For Nursing Homes
As referenced above, Medicaid is a government health insurance program available to people with limited income and resources. If you are age 65 or older, blind, or disabled and meet income and resource requirements, Washington’s Medicaid program, called Apple Health, provides coverage for nursing home residents under certain circumstances.
To obtain Apple Health coverage for nursing home care, you must be financially eligible, and you must need the kind of care nursing homes provide. Nursing homes provide 24-hour supervised nursing care, personal care, therapy, nutrition management, organized activities, and other services.
To apply for LTC Medicaid for nursing home coverage, you must submit an application to the Washington Department of Social and Health Services , either in paper or online. In general, you must meet financial requirements and require a level of care that cannot be met anywhere but in a nursing home.
Typically, your care nursing facility can assist you with the Medicaid application process or you can apply directly with the DSHS. Before you apply, make sure that to the best of your knowledge you meet the eligibility criteria.
Recommended Reading: Medicaid For The Elderly And People With Disabilities
Withinreach Is Here To Help
Health insurance enrollment can be confusing but WithinReach is here to help. Our friendly, local, and knowledgeable staff can help you understand and apply for health insurance based on your needs and budget.
We are certified as âin-person assistersâ by the Washington State Health Benefit Exchange. Regardless of your financial situation, we are here to guide you through the system and help you understand and apply for health insurance. Visit our online Benefit Finder or call the WithinReach Help Me Grow Washington Hotline at 1-800-322-2588 today to get started. Or, read on to learn more about health insurance.
Who Can Get Medicaid In Washington
You should apply for Medicaid if your income is low and you match one of the descriptions below:
- You think you are pregnant
- The parent or caretaker of a child and/or teenager under the age of 19.
- You are a child or teenager age 18 or under.
- An adult age 65 or older.
- You are legally blind.
- Living with a disability or disabled.
- You are in need of nursing home care.
You May Like: Eye Exam Places That Take Medicaid
How Many People Are On Medicaid
According to the Centers for Medicare & Medicaid Services, as of November 2020, here are the number of people enrolled in Medicaid and Chip in the entire United States:
- 78,521,263 individuals were enrolled in Medicaid and CHIP
- 72,204,587 individuals were enrolled in Medicaid
- 6,695,834 individuals were enrolled in CHIP
Where Can I Apply For Medicaid In Washington
Medicaid is administered by the State Health Care Authority in Washington. You can apply online for Medicaid for Medicaid ABD or the MSP. Applicants can also call 855-242-8282 with questions about their Medicaid application.
An in-person interview is always required when applying for long-term care benefits, and many states also require one for Medicaid ABD. However, states cant require an interview if youre only applying for an MSP.
Josh Schultz has a strong background in Medicare and the Affordable Care Act. He coordinated a Medicare technical assistance contract at the Medicare Rights Center in New York City, and represented clients in extensive Medicare claims and appeals. In addition to advocacy work, Josh helped implement federal and state health insurance exchanges at the technology firm hCentive. He has also held consulting roles, including at Sachs Policy Group, where he worked on Medicare and Medicaid related client projects.
You May Like: Can You Get Plan B For Free With Medicaid
How Does Medicaid Provide Financial Assistance To Medicare Beneficiaries In Washington
Many Medicare beneficiaries receive Medicaid financial assistance that can help them with Medicare premiums, lower prescription drug costs, and pay for expenses not covered by Medicare including long-term care.
Our guide to financial assistance for Medicare enrollees in Washington includes overviews of these programs, including Medicaid long-term care benefits, Extra Help, and eligibility guidelines for assistance.
Do I Qualify For Medicaid
Medicaid provides free or low-cost health coverage to some low-income people, families and children, pregnant women, the elderly, and people with disabilities. Many states have expanded their Medicaid programs to cover all people below certain income levels. Medicaid qualifications depend partly on whether your state has expanded its program.
You May Like: Does Maryland Medicaid Cover Abortions
Unitedhealthcare Connected Benefit Disclaimer
This is not a complete list. The benefit information is a brief summary, not a complete description of benefits. For more information contact the plan or read the Member Handbook. Limitations, copays and restrictions may apply. For more information, call UnitedHealthcare Connected® Member Services or read the UnitedHealthcare Connected® Member Handbook. Benefits, List of Covered Drugs, pharmacy and provider networks and/or copayments may change from time to time throughout the year and on January 1 of each year.
You can get this document for free in other formats, such as large print, braille, or audio. Call , TTY 711, 8 a.m. – 8 p.m., local time, Monday – Friday . The call is free.
You can call Member Services and ask us to make a note in our system that you would like materials in Spanish, large print, braille, or audio now and in the future.
Language Line is available for all in-network providers.
Puede obtener este documento de forma gratuita en otros formatos, como letra de imprenta grande, braille o audio. Llame al , TTY 711, de 08:00 a. m. a 08:00 p. m., hora local, de lunes a viernes correo de voz disponible las 24 horas del día,/los 7 días de la semana). La llamada es gratuita.
Puede llamar a Servicios para Miembros y pedirnos que registremos en nuestro sistema que le gustaría recibir documentos en español, en letra de imprenta grande, braille o audio, ahora y en el futuro.
Los servicios Language Line están disponibles para todos los proveedores dentro de la red.
Who Is Eligible For Medicaid In Washington
Apple Health provides health insurance coverage for qualifying children, pregnant women, parents, seniors, and individuals with disabilities. See the Eligibility page on the Washington State Health Care Authority website for details. Below is a summary of income limits for non-elderly adults and children.
- Adults with incomes up to 138% of the federal poverty level
- Children with household incomes up to 210% of poverty
- Pregnant women with incomes up to 193% of poverty.
- Children are eligible for CHIP with household incomes up to 312% of poverty.
Apple Health for Kids is available to children even if they are undocumented immigrants. In that case, only state Medicaid funds are used to provide coverage, and families with income above 200% of the poverty level will have to pay higher premiums to cover a child who is undocumented. Pregnant undocumented immigrants are also eligible for state-funded Apple Health coverage.
Read Also: Where To Get Braces With Medicaid
Medicaid Asset Rules In Washington
Medicaid for LTC has different resource rules than those for other Apple Health programs. Resources are assets like real property, personal property, life insurance with a cash value, vehicles, motorhomes, boats, IRAs, bank accounts and cash. You will have to total up all of these to determine how much you have in resources.
If you are a single person, you can have only up to $2,000 in resources with a few allowable exclusions such as a car and your home . If you are married, your non-applicant spouse at home can keep up to $126,420 worth of joint assets.
What Are The Medicaid Eligibility Requirements
Medicaid beneficiaries generally must be residents of the state in which they are receiving Medicaid. They must be either citizens of the United States or certain qualified non-citizens, such as lawful permanent residents. In addition, some eligibility groups are limited by age, or by pregnancy or parenting status.
Recommended Reading: Does Medicaid Cover A Breast Reduction
What If Im Turned Down By Medicaid
- You may be able to buy a private health plan through the Marketplace instead for the 2018 plan year in the fall. You may qualify for savings based on your income through a premium tax credit and savings on out-of-pocket costs.
- If you don’t qualify for either Marketplace or Medicaid savings, you still have options. Learn more here.
Who Can Get Medicaid
- No matter your state, you may qualify for Medicaid based on your income, household size, disability, family status, and other factors. But if your state has expanded Medicaid coverage, you can qualify based on your income alone.
- Enter your household size and state. We’ll tell you who is eligible for Medicaid, if your state expanded and if you qualify for Medicaid based only on your income.
- If you think you have Medicaid eligibility, you can create an account and fill out a Marketplace application. If it looks like anyone in your household qualifies for Medicaid or CHIP, we’ll send your information to your state agency. They’ll contact you about enrollment. You can apply any time of year.
- If you don’t qualify for Medicaid, we’ll tell you if you qualify for financial help to buy a Marketplace health plan instead.
Read Also: Florida Medicaid Gold Card Providers
