Ohio’s Medicaid Income Limit
If you are 65 or older, blind, or disabled, and you need long-term care in a nursing home, then you must have income at or below $2,313 per month to qualify for Medicaid. The 2019 monthly income limit for a married couple with both spouses applying is $4,626.
If your income is above the limit, you still might be able to qualify for Medicaid if the income you have over the limit doesn’t cover your medical expenses. In Ohio, unlike some other states, people who are sixty-five and older, blind, or disabled can use unpaid medical bills, premiums, or nursing facility bills to “spend down” their income and qualify for Medicaid. A worker from ODJFS will determine how much your monthly spend-down amount is. You have to satisfy the spend-down to be eligible for Medicaid each month. You can satisfy your spend-down by showing proof that your medical expenses equal the spend-down amount or by paying the amount directly to ODJFS.
Medicaid For Beginners: 5 Facts About Ohio Medicaid
Everyone has heard of Medicaid. It is one of the largest health insurance providers in Ohio and covers individuals and families who dont have insurance and cant afford to buy it. More than 2.9 million people in Ohio get health insurance through Medicaid every year. But did you know that Medicaid is much more than health insurance for the poor? Here are five facts about Medicaid that might surprise you.
Medicaid is a State-Federal Partnership
People sometimes confuse Medicaid and Medicare. The names sound similar, but they are very different programs. Medicare is a Federal benefit for seniors and some individuals with disabilities and is the same no matter where you live. Medicaid is a Federal-State partnership where each state runs its own Medicaid program. The Federal Government gives the state money if it meets certain Federal guidelines. Every state offers different Medicaid coverage, and some states cover groups that other states dont.
Everyone in Ohio who Financially Needs Medicaid Can Get It
Medicaid is Essential for Ohioans with Disabilities
Individuals with More Serious Conditions have a Medicaid Program Just for Them
Medicaid Helps Pay for Long-Term Care at Home, in Assisted Living, or in a Nursing Home
Medicaid can be confusing and overwhelming. These five facts are geared toward clearing up that confusion as you start to think about Medicaid, decide whats right for you and plan for the care you need.
Lawmakers Voted To Freeze Medicaid Expansion In 2017 Kasich Vetoed
Lawmakers in Ohio came to a compromise on their budget bill on in June 2017 and sent it to Governor Kasich, who had just two days to review it before the June 30 deadline for the state to enact the budget for the 2018 fiscal year, which began July 1, 2017. The Senates version of the bill had included a freeze on new Medicaid expansion enrollments after July 1, 2018, and that provision remained in the bill after it went through the conference committee process to reconcile the differences between the House and Senate versions of the budget.
Kasich had noted that the Medicaid expansion freeze would result in 500,000 people losing coverage in the first 18 months, since people would lose coverage if their income increased and would then be unable to get back on Medicaid if their income subsequently decreased .
Kasich used his line-item veto power to eliminate the Medicaid expansion freeze, and he also vetoed a provision that would have required Medicaid expansion enrollees to pay monthly premiums for their coverage. Monthly premiums for Medicaid expansion populations require approval from CMS the Obama Administration only approved limited premium requirements, and had rejected a more far-reaching premium requirement that Ohio had proposed in 2016 . But the Trump Administration has made it easier for states to impose these types of requirements on Medicaid expansion enrollees.
You May Like: What Is The Household Income Limit For Medicaid
Will Magi Rules Apply To Everyone Seeking Medicaid Coverage
MAGI-Based Eligibility applies to individuals who are considered Covered Families and Children Medicaid categories including families, children up to age 19, pregnant women and adults 19 64 who are below 138% Federal Poverty Level . MAGI rules also apply to time-limited coverage for individuals who were enrolled in Medicaids parent category and lost eligibility due to increased earnings or spousal support.
Providers Subject To On
Federal and state laws require some providers to have pre- and post-enrollment on-site screening visits to ensure program integrity. .
In Ohio, the Public Consulting Group, Inc. will conduct these visits for providers that are not already screened by another state or federal agency. On-site screening visits are conducted without prior notification or appointment. The PCG representatives will have a business card and a letter of introduction, for your verification.
When the PCG representatives arrive at your office, please take a few moments to answer their questions and allow them access to your facility. This will help to complete your on-site visit smoothly. During your site visit, the PCG representatives will review various aspects of your business. Failure to answer their questions and cooperate with the PCG representatives could affect your enrollment or current provider status with Ohio Medicaid.
Also Check: Dual Enrollment Medicare And Medicaid
Ohio Medicaid Income Limit
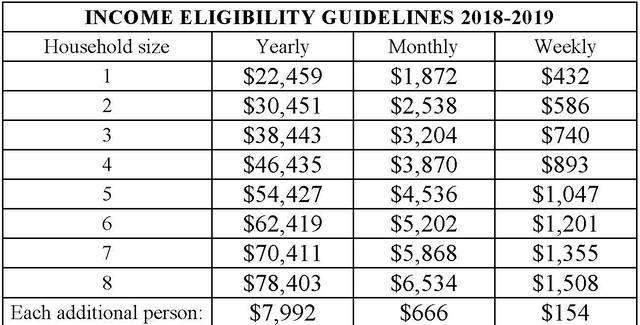
The Ohio Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the Ohio Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 206 percent of FPL
- Any child age 1-5 with a family income up to 206 percent of FPL
- Children ages 6- 18 with family income up to 206 percent of FPL
- CHIP for children with family income up to 206 percent of FPL
- Pregnant women with family income up to 200 percent of FPL
- Parents of minor children with family income up to 90 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 74% of the FPL
- Adults without dependents under Medicaid expansion with income up to 133% of the FPL
Why Is Ohio Using Magi Rules To Determine Who Is Counted In Medicaid Households And What Income Is Being Counted
The introduction of MAGI rules is a federal requirement introduced to all states. MAGI rules make calculating household size and income consistent across the United States. The new MAGI standards are based on federal income tax rules and uses a tax filers family size and income to determine eligibility. If you do not file taxes, your family size will be based on the number and age of the immediate family members who live with you. In general, only income included for federal tax purposes is counted. Income that is not included when filing federal taxes is most likely not counted for MAGI calculations.
For example:
- Child support is not considered income when filing federal taxes. Child support is not counted as income when determining Medicaid eligibility.
- Spousal support is considered income when filing federal taxes. Spousal support is counted as income when determining Medicaid eligibility.
For additional help please visit your local Morrow County Job and Family Services 419-947-9111 or call the Medicaid Hotline at 324-8680.
Read Also: Is Amerihealth Caritas Medicaid Or Medicare
How Much A Spouse Can Keep In Ohio
If you have a spouse who is going to continue to live independently, then Ohio will allow you and your spouse to keep more income and assets to support that spouse.
Your spouse will be allowed to keep some income each month. The amount will depend on how many dependents and expenses he or she has. In 2019, the minimum monthly Community Spouse Income Allowance is $2,057.50, and the maximum is $3,160.50.
Ohio assumes that half of the assets that you had at the time of your first admission to a nursing home ) should belong to your spouse, subject to a limit that changes annually. For married couples, as of 2019 the CSRA is up to a maximum of $126,420. When you apply for Medicaid, ODJFS will tell you how much your community spouse is entitled to keep.
When you apply for Medicaid, your CSRA is subtracted from your countable assets at the time of your application. For example, say Mr. and Mrs. Johnson have $80,000 in countable assets when he moves into a nursing home on February 1st. Mrs. Johnson continues to live in the couple’s home. On that date, Mrs. Johnson’s CSRA is calculated to be $40,000. The Johnsons use their savings to pay for Mr. Johnson’s nursing home care until December 1st, when he applies for Medicaid. On December 1st, Mr. and Mrs. Johnson have $40,000 left in countable assets. Because Mrs. Johnson’s CSRA is $40,000, she is entitled to keep the $40,000. Mr. Johnson then has no countable assets, and he meets the resource eligibility criteria for Medicaid.
Ohio Medicaid Eligibility And Enrollment
- Find out how Ohio Medicaid provides health care services for older adults. Learn about what’s covered, eligibility criteria and how to apply for coverage.
Ohio Medicaid programs help residents of the state access quality health care services, particularly when they’re unable to afford the cost of care on their own. In Ohio, just as in other states across the country, Medicaid programs are administered by the state and must operate within the parameters set forth by the federal government. The state must provide coverage for necessary healthcare services, such as inpatient and ambulatory hospital care.
Eligibility requirements vary from state to state, but in all states, those living below the federal poverty line must be provided with coverage. In some states, including Ohio, coverage is expanded by waivers to help older adults access additional care services, such as assisted living and home care.
Below, we discuss what services Ohio’s standard Medicaid plan covers as well as the various waivers that are available for seniors in the state, who’s eligible and how to apply.
Don’t Miss: Does West Virginia Have Expanded Medicaid
How To Apply For Medicaid In In Ohio
Multiple methods exist for applying for Ohio Medicaid. Many people have taken to the online version which is fast to use and initiates a quick response. A pop-up window comes on the screen when attempting to start a new application. It allows users to either sign in with an existing account or create an account if it is their first time. Provide a first and last name, date of birth, and social security number to sign up and start the process.
Those who do not wish to use the online version may instead visit their local office to fill out a paper form. It can get submitted directly to a worker who can assess the information and approve or deny the claim. It is also possible to apply by telephone by calling the Ohio Medicaid Consumer Hotline at 324-8680.
Attention Waiver Services Provider Applicants
Prior to submitting an application, waiver provider should contact the following for enrollment requirements and assistance:
- For the Ohio Home Care Waiver Visit: for application and enrollment information or contact PCG at 908-1746. Note: Bureau of Criminal identification & Investigation reports for initial provider enrollments ONLY should be sent to: The Ohio Department of Medicaid, Attention: BCII Coordinator, P.O. Box 183017, Columbus, Ohio 43218-3017
- For Passport or Assisted Living waiver programs Visit: for application and enrollment information.
- For Individual Options, Level 1 and SELF waivers – Visit the DODD Gateway: .
You May Like: Can I Change Medicaid Plan
Why Oig Did This Audit
The Patient Protection and Affordable Care Act gave States the option to expand Medicaid coverage to low-income adults without dependent children. It also mandated changes to Medicaid eligibility rules and established a higher Federal reimbursement rate for services provided to these beneficiaries, which led us to review whether States were correctly determining eligibility for these newly eligible beneficiaries. Ohio chose to expand Medicaid coverage.
Our objective was to determine whether Ohio determined Medicaid eligibility for newly eligible beneficiaries in accordance with Federal and State eligibility requirements.
Learn About Medicaid In Ohio
Many people find themselves asking, what is Medicaid in Ohio? even though they have most likely heard of this important program before. Medicaid is a federal- and state-funded health insurance program for low-income families and individuals. In addition to low-income households, Medicaid also provides affordable, government-funded health insurance to individuals with disabilities, children, expectant mothers and senior citizens. This medical assistance program is responsible for providing millions of American citizens who would otherwise go uninsured with health care.
Before Ohio residents can apply for Medicaid benefits, they must make sure they are eligible. In order to be approved for Medicaid assistance, individuals must meet basic requirements regarding their income, citizenship and resident status. It is essential for Medicaid applicants to understand how the program works and what exactly the application process entails in order to ensure successful access to the healthcare benefits Medicaid provides. Oftentimes, finding more information about Medicaid can be tiresome and difficult. Find out everything you need to know about Medicaid by downloading our free guide.
Recommended Reading: Psychiatrist In Nyc That Take Medicaid
Who Can Get Medicaid In Ohio
You should apply for Medicaid if your income is low and you match one of the descriptions below:
- You think you are pregnant
- The parent or caretaker of a child and/or teenager under the age of 19.
- You are a child or teenager age 18 or under.
- An adult age 65 or older.
- You are legally blind.
- Living with a disability or disabled.
- You are in need of nursing home care.
Ohio Medicaid Expansion Update
Governor Kasich announced in early 2013 that Ohio would expand Medicaid under the ACA.
Ohio lawmakers who were opposed to Medicaid expansion brought a lawsuit against the Kasich administration in an effort to block expansion.
Ultimately, in late 2013, the Ohio Supreme Court ruled in favor of Governor Kasich, and Medicaid expansion took effect as scheduled in 2014.
As of June 2019, there were 526,100 Ohio residents enrolled in expanded Medicaid.
Additionally, during the 2015 legislative session, lawmakers agreed to allow Medicaid expansion to continue as a part of a budget agreement.
Therefore, there was no separate legislation on Medicaid expansion.
Ohios Medicaid work requirement waiver was approved in 2019 but has been delayed due to COVID.
Read Also: Dentist In Midland Tx That Take Medicaid
How To Apply For Medicaid In Ohio
Finding out how to apply for Medicaid in Ohio is the next step after a potential applicant has determined his or her eligibility for Medicaid benefits. Applicants need to know where to apply for Medicaid and how to navigate the Medicaid application process in order to increase their chances of filling out a successful application and being admitted into the program. Furthermore, in addition to learning about the Medicaid application, claimants must be prepared with the supporting documents needed to verify and approve the application. Learn more about the OH Medicaid application form by reading the following topics.
Where do you sign up for Medicaid in Ohio?
Fully understanding how to apply for Medicaid benefits in Ohio is essential to a successfully submitted application, since there are a few application methods available. The easiest way to submit an application for Medicaid in OH is by using the online application process. In order to apply for Medicaid online, all a petitioner needs is access to a computer and the internet, which can be found at a local public library if a computer is not readily available. Applying for the Ohio Medicaid program online is fast and convenient, and anyone can use the online system. If a caretaker is filling out a Medicaid application on behalf of a claimant, the caretaker must make sure all supporting documents are prepared.
Information Required on the Medicaid Application Form in Ohio
When A Nursing Home Is Medically Necessary
Medicaid will pay for a nursing home only when it is medically necessary. In other words, you must show that you require a “nursing facility level of care,” meaning that you need the kind of care that can only be provided in a nursing home. In Ohio, there are two nursing facility levels of care: intermediate and skilled. To receive Medicaid-paid nursing facility services in Ohio, you must need at least an intermediate nursing facility level of care. This generally means you must show that you need hands-on assistance with at least two of the following activities: bathing, dressing, eating, grooming, moving around, using the bathroom, and taking your medication.
You can meet the skilled nursing facility level of care by showing that you need daily skilled nursing or therapy services for an unstable medical condition. For a skilled nursing facility, you have to require the kind of services that can only be provided by a licensed therapist or nurse. Your condition is considered unstable if you require extensive monitoring and adjustments to your treatment, and if your condition is unpredictable and might require immediate interventions.
Medicaid will decide which type of facility is appropriate for you and will only pay for a facility that is adequate for your level of care needs.
Read on to find out whether Ohio’s Medicaid program pays for assisted living facilities or home health care.
You May Like: How Do I Renew My Ohio Medicaid Benefits Online
Youth Aged Out Of Foster Care
Who is Eligible? Youth between the ages of 18 and younger than 26 who aged out of foster care on their 18th birthday and received Title IV-E payments.
Description: Provides health care coverage for youth, who aged out of foster care on their 18th birthday, until age 26.
Alien Emergency Medical Assistance
Who is Eligible? Non-U.S. citizens who are not eligible for Medicaid.
Description: Provides coverage for the treatment of emergency medical conditions for certain individuals who do not meet Medicaid citizenship requirements
State Funded Medical Assistance for Non-Citizen Victims of Trafficking
Who is Eligible: Non-Citizen Individuals who are a victim of a severe form of human trafficking and are applying for, or preparing to apply for, a T Non-Immigration Status . Individuals must be an Ohio resident, have countable monthly income at or below 100% of the Federal Poverty Level , and not have eligibility under another category of assistance.
Description: Provides state-funded medical assistance to Non-Citizen Victims of Trafficking who have provided verification of the T-Visa application or evidence of human trafficking. Individuals must file a formal application for a T-Visa within one year of the medical assistance application date.
Refugee Medical Assistance
