How Differences Between Commercial Medicare Professional Service Prices Could Result In Different Policy Impacts
Introduction
As rising health care costs force difficult choices for families, employers, and federal, state, and local governments, a range of policy proposals are emerging to address health care spending in the U.S. In this presidential election year, there has been heightened attention on lowering health care costs and making care more affordable, which will likely accelerate with the election of President Biden. Several Members of Congress and nearly every Democratic presidential primary candidate supported substantial health care reforms ranging from “Medicare for All” to a public option.
Several states also have considered legislation to lower health care costs. Washington State, for example, enacted Cascade Care, which will offer a state-sponsored plan on their individual market exchange that will cap payments for all providers and facilities at a percentage of Medicare rates. New Mexico considered a Medicaid buy-in, which would have leveraged Medicaid reimbursement rates, and Colorado’s proposed state public option included a base reimbursement rate for hospitals tied to Medicare. A common way in which these policy proposals aim to lower health care costs is by linking the payments made by private health insurers to what Medicare and Medicaid would pay for similar services.
Rate Cap
Rate Cap Combined with a Rate Floor
Benchmarking Commercial Rates
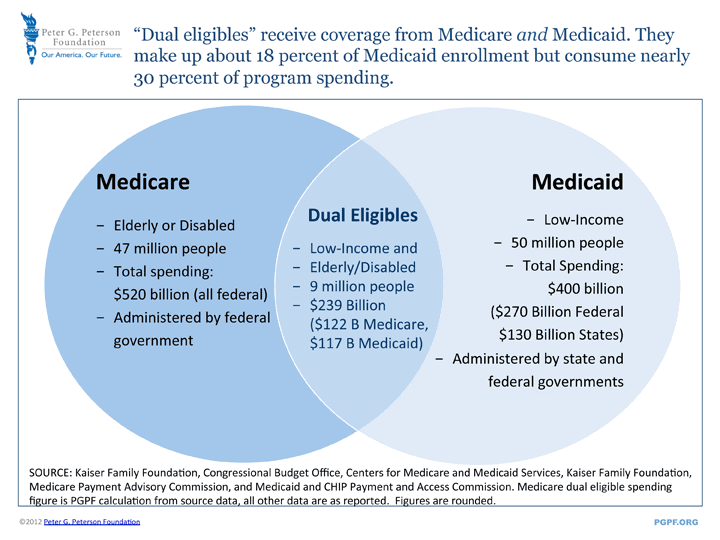
Medicare Vs Medicaid Coverage
Medicare and Medicaid are both programs provided by the U.S government that have been around since 1965.
Medicare is a federal insurance program available to you if youre over 65, regardless of your income.
Medicaid is an assistance program that is for low-income people of any age. Medicaid is both a federal and state program. So this means it varies from state to state as it is run individually under federal guidelines.
If you are eligible for both programs, you can use both once you turn 65 as long as you continue to meet eligibility requirements!
What Is Medicare What Is Medicaid
Medicare is a federal program generally for people who are 65 or older or have a qualifying disability or medical condition. Medicare Part A and Part B are provided by the federal government, and Medicare Part C and Part D, while federally governed, are provided by private insurance companies.
Medicaid is a state government program that helps pay health care costs for people with limited income and resources, and different programs exist for specific populations. Medicaid plans vary from state-to-state but follow federal guidelines for benefits.
Also Check: Medicaid Cost Sharing With Medicare
Medicare And Medicaid Coverage Explained
By Bethany K. Laurence, Attorney
Medicare and Medicaid are very different. Medicaid is a federal program for low-income, financially needy people, set up by the federal government and administered differently in each state.
Medicare was created to deal with the high medical costs that older citizens face relative to the rest of the population — especially troublesome given their reduced earning power. However, eligibility for Medicare is not tied to individual need. Rather, it is an entitlement program you are entitled to it because you or your spouse paid for it through Social Security taxes.
Although you may qualify for and receive coverage from both Medicare and Medicaid, you must meet separate eligibility requirements for each program being eligible for one program does not necessarily mean you are eligible for the other. If you qualify for both, Medicaid will pay for most Medicare Part A and B premiums, deductibles, and copayments.
The information below provides the basics of each program.
What Is The Difference Between A Federally Qualified Health Center And A Rural Health Clinic
Although FQHCs and RHCs both provide primary care to underserved and low-income populations, there are some fundamental differences.
| Rural Health Clinics |
|---|
For a more complete comparison, see HRSA’s Comparison of the Rural Health Clinic and Federally Qualified Health Center Programs.
Recommended Reading: Air Purifier Covered By Medicaid
What Are The Differences Between Medicare And Medicaid Reimbursement
- how the government pays health care providers for Medicare and Medicaid patients, why health care providers hate Medicare and Medicaid
Please Share!
It can be hard to find a good doctor who accepts Medicare and Medicaid patients, but there are valid reasons for the medical professions hesitance in treating patients with these forms of coverage. If you had to change doctors or noticed a change in how you get treated after you enrolled in Medicare or Medicaid, it might help if you saw the issue from the healthcare systems perspective.
Medicare and Medicaid are government programs, so they force doctors and hospitals to fill out complex paperwork to get paid for the medical services they provide to beneficiaries of these programs. The government then takes its sweet time in paying the medical professionals and facilities for the services rendered. The government calls these payments reimbursements, and Medicare and Medicaid do not handle this process the same. What are the differences between Medicare and Medicaid reimbursement?
Medicaid
Medicaid provides medical insurance for people with little or no income. The program receives both state and federal funding. Every state forms its own Medicaid program. Medicaid benefits can vary widely from one state to another. Each Medicaid program sets the amount it will pay for office visits, hospital stays and every kind of medical service you can imagine.
Medicare
References:
What Are The Major Strategies To Ensure Quality Of Care
The ACA required the U.S. Department of Health and Human Services to establish a National Quality Strategy,32 a set of national aims and priorities to guide local, state, and national quality improvement efforts, supported by partnerships with public and private stakeholders. The strategy includes annual reporting on a selected set of quality measures.33
Since 2003, the Agency for Healthcare Research and Quality has published the annual National Healthcare Quality and Disparities Report, which reports on national progress in health care quality improvement. The 2018 report found that the quality of U.S. health care had improved overall from 2000 to 2016, but that improvement was inconsistent. For example, while most person-centered care and patient-safety measures improved, affordability did not.34
Federal law requires certain providers to report data on the quality of their care, and the Centers for Medicare and Medicaid Services to publicly report performance on quality measures. For example, Hospital Compare is an online public resource summarizing the performance of more than 4,000 hospitals on measures of care processes, care outcomes, and patient experiences. Related quality-reporting programs include Nursing Home Compare and Physician Compare.
Recommended Reading: Dcbs Ky Medicaid Phone Number
How Do You File A Medicare Reimbursement Claim
As we mentioned earlier, it is rare for you to have to file a claim if you have original Medicare and the service provider is a participating provider.
You can view any outstanding claims by checking your Medicare Summary Notice or by going to MyMedicare.gov.
Medicaid Reimbursement Varies By State
The greatest difference between Medicare and Medicaid reimbursement structures is that each state controls its own Medicaid program. Consequently, every Medicaid program differs based on state regulations.
However, most Medicaid reimbursement models use fee-for-service, managed care, or a combination of both to pay providers.
Fee-for-service payment dominates Medicare reimbursement structures across states. Over one-half of Medicaid spending in 2015 stemmed from a fee-for-service payment model, the Medicaid and CHIP Payment and Access Commission reported.
Fee-for-service Medicaid reimbursement models pay providers by the volume of services they provide to beneficiaries. States establish their Medicaid reimbursement rates under fee-for-service models, but policymakers must base the rates according to the following federal methodologies:
- Healthcare costs associated with providing services
- Review of commercial payer rates
- Percentage of what Medicare reimburses for equivalent services
Most Medicaid fee-for-service methodologies set rates by the charge for services or maximum allowable price, whichever is lesser. Thirty-eight out of the 51 US Medicaid programs using this method, a recent MACPAC report showed.
In contrast to a fee schedule, states pay providers based on either a percentage of Medicare payment, a state-determined market assessment, or a relative value scale.
However, they can also include varying levels of financial risk or value-based reimbursement.
Recommended Reading: How Do I Know If My Medicaid Is Still Active
What Is Being Done To Promote Delivery System Integration And Care Coordination
The ACA introduced several levers to improve the coordination of care among medical/clinical providers in the largely specialist-driven health care system. For example, the law supported adoption of the patient-centered medical home model, which emphasizes care continuity and coordination via primary care, as well as evidence-based care, expanded access, and prevention and chronic care management.
The ACA also expanded the Centers for Medicare and Medicaid Services ability to test alternative payment models that reward quality, reduce costs, and aim to improve care coordination. This trend has since been continued by public and private payers.
One of these alternative payment models is bundled payments, whereby a single payment is made for all the services delivered by multiple providers for a single episode of care. Another trend is the proliferation of accountable care organizations . These networks of providers assume contractual responsibility for providing a defined population with care that meets quality targets. Providers in ACOs share in the savings that constitute the difference between forecasted and actual health care spending.
Dental And Vision Care
As with many forms of Medicaid care, dental and visual care is available to all children but may or may not be available to adults, as states can decide whether either type of care will be covered. State programs are more likely to cover emergency dental care than ongoing preventive care, such as cleanings or fillings. Some states will cover one eye exam and one pair glasses every three years for adults 21 and older.
Similar to how Medicaid covers dental care, Medicare tends only to cover emergency dental care and dental surgery. It does not cover routine preventive care or dentures. Hospitalizations related to dental ailments will be covered under Medicare Part A, but the cost of a dentist or periodontist will not be covered. Vision care is similarly limited under Medicare, with the program generally not covering any non-emergency and/or non-disease-related eye problems.
Also Check: Blue Shield Of California Medicaid
Income Adjustments And Outlier Screens
There are several reasons why discrepancies may exist between calculated net income and reported net incomes. First, errors may be present in the practice cost calculations that enter into the decomposition equation. Total physician practice costs were estimated by summing the following costs: office, equipment, supplies, and automobile costs malpractice insurance and physician and employee salaries.
Second, a problem arises when income data are reported within ranges and interval midpoints are used to approximate reported incomes. Discrepancies appear when a physician’s actual income does not coincide with these midpoints. For example, a $50,000 discrepancy is possible if an incorporated physician reports his gross income within the $400,000-$500,000 range when, in fact, his actual gross income is $400,000. By calculating net income as a residual and then comparing it with the reported value, either or both the gross and net incomes were moved to the endpoints of the allowable range.
Approximately 20 percent of the sample were missing gross revenue and/or net income values. Replacement values for the missing data had to be calculated. Gross revenue was estimated by the following reduced-form equation:
GRf
where GR = gross revenue ,
GS
NOTE: t statistics in parentheses.
Find Cheap Medicare Plans In Your Area

In the United States, there are currently two government-provided health insurance policies that citizens can enroll in: Medicare and Medicaid. While they both provide general health insurance benefits, there are differences in eligibility and coverage that are crucial to identify and be aware of the largest being that Medicare is available to adults who are over 65 years old whereas Medicaid is only available to low-income families.
You May Like: Blue Cross Complete Medicaid Providers
The A B C And Ds Of Medicare Reimbursement
CMS divides Medicare coverage into four parts, each with their own claims reimbursement structures. Medicare Parts A and B are considered traditional Medicare and cover inpatient and outpatient services, whereas Part C includes Medicare Advantage plans and Part D covers prescription drugs.
Traditional Medicare reimbursement
Approximately two-thirds of Medicares benefit spending stems from services performed by providers in traditional Medicare.
The providers who receive traditional Medicare reimbursement range from hospitals, physicians, post-acute care facilities, and hospice agencies to durable medical equipment suppliers, ambulance providers, and laboratories. Medicare reimburses each provider type using separate payment rates and systems.
However, traditional Medicare reimbursement generally falls into two categories: Part A services and Part B services.
Medicare Part A services include inpatient hospital, skilled nursing facility, nursing home, hospice, and home health care. Providers primarily receive Medicare reimbursement for the hospital-based services under the inpatient prospective payment system .
Under the IPPS, hospitals receive a prospective payment per beneficiary discharge. CMS determines the rate based on one of over 700 Diagnosis Related Groups , which adjust payments according to patient age, sex, secondary diagnosis, and services received.
CMS also adjusts OPPS rates by the hospital wage index to offset geographical variations in healthcare costs.
Difference Between Medicare And Medicaid
Medicare and Medicaid are two different programs run by the Government.
These are run and supported by different parts of government and mainly benefit various groups. Generally, the similarities between Medicare and Medicaid can be distilled down to who manages them, who benefits, how much users pay and what programs they provide.
The key differences are provided below:
- People receiving Medicare coverage pay a part of the cost for issues like hospital stays by deductibles. Medicare needs small monthly payments for services outside the hospital, such as visiting a doctor or taking preventive care. Many out-of-pocket costs may also apply to things like prescription drugs while people who receive Medicaid coverage often do not have to pay for covered costs at all, but in some situations, a minor copayment is required.
- Reimbursements for the medicare come from a federal trust fund. Most of that funds money comes from payroll taxes. Furthermore, premiums, deductibles and copays help pay for Medicare benefits. In the case of Medicaid, it is similar but many of the details, including reimbursement rates, vary by state. Doctors may choose not to consider Medicaid in situations where the reimbursement rate is much lower than the cost of the treatment. This is sometimes true in Medicare, too.
Also Check: Birthing Centers That Accept Medicaid
Medicare Payments And Provider Costs
To assess the adequacy of Medicares hospital payment rates, MedPAC regularly compares the programs payments to hospitals care delivery costs. Their findings show that, across all hospitals over the period from 2010 to 2018, costs for the treatment of Medicare beneficiaries have exceeded Medicare payments, resulting in negative and declining aggregate Medicare margins .87 Both MedPAC and American Hospital Association analyses show aggregate all-payer hospital margins have remained positive between 6% and 8% during the same period due to the contribution of private payers.88,89 Somehospital industry groups and researchers see these data as evidence that higher payment rates from private insurers are necessary to offset the financial strain of Medicares relatively low rates.90
Figure 6: Medicare Margins are Negative Overall, but Have Been Positive for Relatively Efficient Hospitals Until Recently
How Do Rhcs Meet The Healthcare Needs Of Rural Medicare Beneficiaries
RHCs were first created to meet the primary care needs of rural Medicare beneficiaries. Access and Capacity to Care for Medicare Beneficiaries in Rural Health Clinics, a 2019 policy brief from the University of Minnesota Rural Health Research Center, summarizes the findings of a voluntary survey of 111 RHCs. The survey found that 87% of RHCs accept walk-in appointments and 65% of RHCs had appointments available for existing Medicare beneficiaries. However, 37% of RHCs had appointments available for new beneficiaries within one day, and the average wait time for an appointment for new beneficiaries was 5 days.
While RHCs provide primary services to rural residents, RHCs often must refer patients to other providers when specialty care is required. Access to Specialty Care for Medicare Beneficiaries in Rural Communities notes that 22% of Medicare beneficiaries that had appointments at RHCs needed specialty care, but 64% of RHCs had difficulty finding specialists to which they could refer these patients.
You May Like: Kids Dentist That Take Medicaid
Geographic And Specialty Distribution
Much national concern exists over the geographic and specialty maldistribution of physicians. This maldistribution has limited access to primary care services and increased health care costs through the provision of more intensive and, consequently, higher priced services. The literature on physician location and specialty choice indicates that financial incentives play a minor role in the physician decision process. Nevertheless, from a Federal policy perspective, Medicare and Medicaid reimbursement practices should support, or at least not contradict, government policies to attract physicians into shortage specialties and under-served areas.
shows the relationship between physician density and average Medicare and Medicaid prevailing charges for specialists. A continuum exists from the least to the most physician-dense areas for Medicare specialist fees. Prevailing charges average 33 percent higher in counties with more than 175 physicians per 100,000 population than in counties with fewer than 75 physicians per 100,000 population. In contrast, there appears to be very little relationship between Medicaid fees and physician density.
