Option 3 Download Application
You can , complete it, and mail it to your County Assistance Office office or submit it in person.
Additionally, you can Call the Consumer Service Center for Health Care Coverage at 1-866-550-4355.
Resources LimitsMedicaid eligibility for some is also determined using resource and household size in comparison to resource limits.
However, the resource limits do not apply to the following groups:
- Adults Age 19-64
South Dakota Medicaid For Individuals In Assisted Living Facilities Nursing Facilities Or Homes
Individuals in assisted living centers, Nursing Facilities or Homes who meet all eligibility criteria may qualify for South Dakota Medicaid.
Eligibility Requirements
- A person must be 65 years or older. If under age 65, a person must be blind or disabled.
- A person must be a resident of South Dakota and meet certain citizenship requirements of the United States.
- Medical needs of the individual are such that they require a level of care provided in a nursing home.
- The monthly income limit is 300 percent of the SSI Standard Benefit Amount.
- The resource limit is $2,000. Resources include items such as checking and savings accounts and certificates of deposit.
How Medicaid Eligibility Is Determined
Income eligibility is determined by your modified adjusted gross income , which is your taxable income, plus certain deductions. Those deductions include non-taxable Social Security benefits, individual retirement contributions and tax-exempt interest. For most people, MAGI is identical or very close to your adjusted taxable income, which you can find on your tax return. Specific income requirements in dollars rise alongside the size of your household.
Our guide focuses on each stateâs major programs for adults. Most are only available to state residents, U.S. citizens, permanent residents or legal immigrants .
Looking for insurance for a child? Check out our guide to the Children’s Health Insurance Program .
Don’t Miss: Does Medicaid Cover Glasses In Texas
Nevada Medicaid Expansion Update
Nevadas then-Governor Brian Sandoval announced in December 2012 that the state would expand Medicaid starting in 2014.
Governor Sandoval was the first Republican governor to commit to expanding Medicaid.
The state projected about 78,000 people would be newly eligible for Medicaid as a result of the expansion.
However, more than 200,000 were enrolled in expanded Medicaid within the first three years.
Governor Sandoval vetoed a Medicaid buy-in program in 2017.
How Do I Know If I Qualify For Medicaid Services
If youre unsure whether you meet the Medicaid qualifications and income requirements, you can use a Medicaid calculator. Simply enter your information, including your state/zip code, income, household size and the number of adults and children you want to enroll.
Health For California is here to help you determine your Medi-Cal eligibility. Our free agents are always available to answer your question. If you want to enroll yourself or your family in Medi-Cal, get your free quote today.
Not sure how Obamacare affects your health care plans in California? Learn how the ACA works in California, including benefits, costs and enrollment.
Don’t Miss: Dermatologist In Lake Charles That Accept Medicaid
How To Determine Size Of Household To Identify Which Income Limit Applies
The income limits increase with the “household size.” In other words, the income limit for a family of 5 may be higher than the income limit for a single person. HOWEVER, Medicaid rules about how to calculate the household size are not intuitive or even logical. There are different rules depending on the “category” of the person seeking Medicaid. Here are the 2 basic categories and the rules for calculating their household size.
People who are Disabled, Aged 65+ or Blind – “DAB” or “SSI-Related” Category — NON-MAGI – See this chart for their household size. These same rules apply to the Medicare Savings Program, with some exceptions explained in this article.
Everyone else — MAGI – All children and adults under age 65, including people with disabilities who are not yet on Medicare — this is the new “MAGI” population. Their household size will be determined using federal income tax rules, which are very complicated.
New rule is explained in State’s directive 13 ADM-03 – Medicaid Eligibility Changes under the Affordable Care Act of 2010 pp. 8-10 of the PDF, This PowerPoint by NYLAG on MAGI Budgeting attempts to explain the new MAGI budgeting, including how to determine the Household Size. See slides 28-49. Also seeLegal Aid Society and Empire Justice Center materials
Effective Date Of Coverage
Once an individual is determined eligible for Medicaid, coverage is effective either on the date of application or the first day of the month of application. Benefits also may be covered retroactively for up to three months prior to the month of application, if the individual would have been eligible during that period had he or she applied. Coverage generally stops at the end of the month in which a person no longer meets the requirements for eligibility.
Don’t Miss: How Does One Get Medicaid
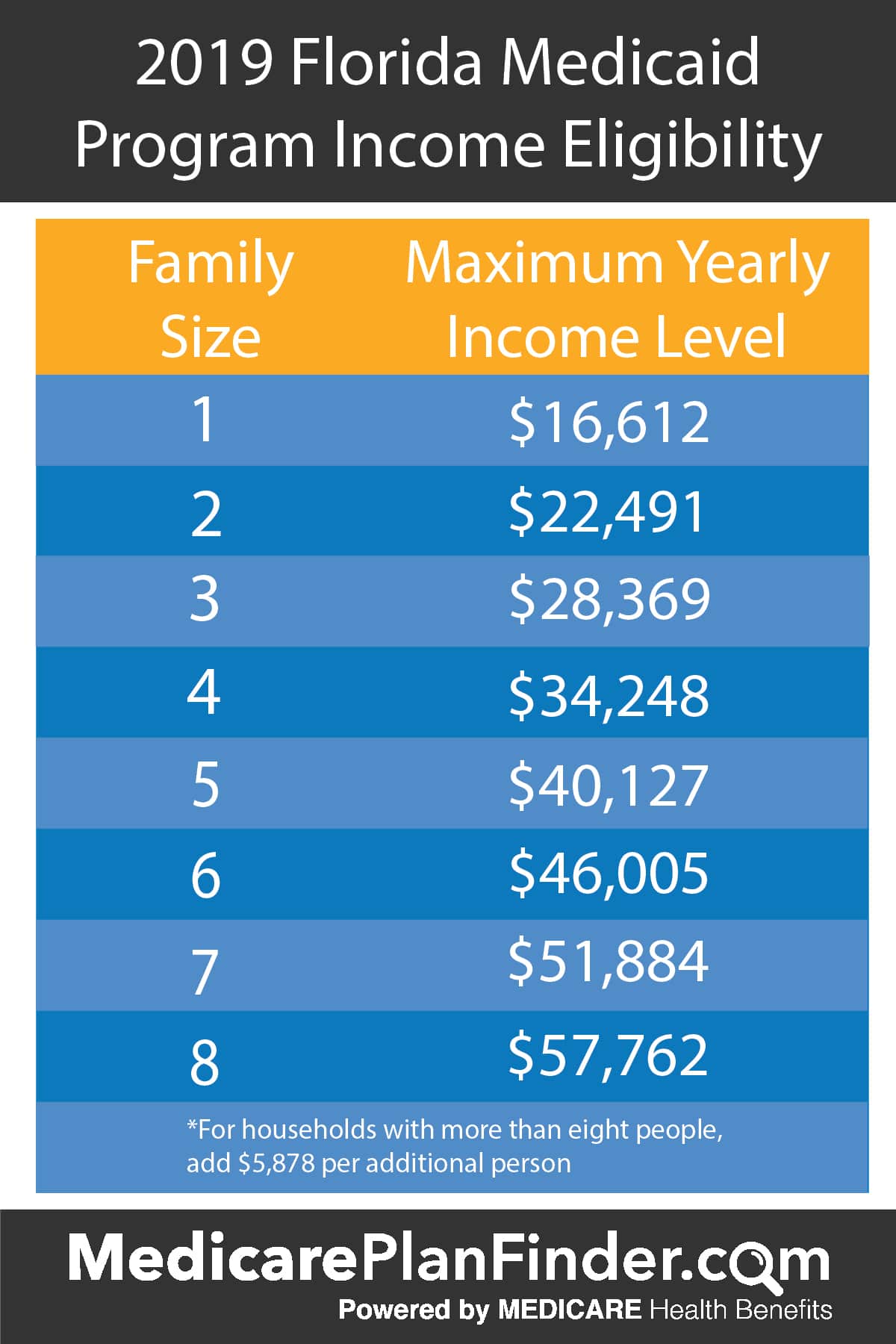
Medicaid For Children And Adults
Eligibility for Medicaid and Dr. Dynasaur are based on the current year Federal Poverty Level guidelines.
- The monthly income limit for adults ages 19 through 64, who are not blind or disabled, is 138% FPL.
- The monthly income limit for children under age 19 is 317% FPL. . There is a monthly premium for some households based on your income. For families up to 195% FPL, there is no premium. There are no prescription co-payments.
- The monthly income limit for Vermonters who are pregnant is 213% FPL. Dr. Dynasaur for pregnant women provides the same coverage as Medicaid, plus full dental coverage. There are no premium or prescription co-pays with this type of Dr. Dynasaur.
How Is The Federal Poverty Level Used In Health Care
The federal poverty level is used to determine eligibility for Medicaid and CHIP to determine eligibility for ACA premium tax credits and cost-sharing reductions and eligibility for Medicare Savings Programs .
Medicaid and CHIP:
- In states that have expanded Medicaid, Americans under the age of 65 will qualify for Medicaid if they earn up to 138% of the federal poverty level.
- In states that havent expanded Medicaid, the eligibility guidelines are stricter, with much lower income limits for parents and coverage generally not available at all to non-disabled childless adults, regardless of how low their income is. This creates a coverage gap that exists in a dozen states as of 2021.
- For people who are disabled or 65+, Medicaid eligibility also depends on assets .
- CHIP eligibility is also based on the federal poverty level, but the specific thresholds vary from one state to another.
- For Medicaid and CHIP eligibility determinations, the current years federal poverty level numbers are used .
Premium tax credits:
Cost-sharing reductions:
| If more than 8 in household / family, add $4,480 per additional person. | If more than 8 in household / family, add $5,600 per additional person. | If more than 8 in household / family, add $5,150 per additional person. |
You May Like: Amerigroup Medicaid Texas Breast Pump
Caution: What Is Counted As Income May Not Be What You Think
For the NON-MAGI Disabled/Aged 65+/Blind, income will still be determined by the same rules as before, explained in this outline and these charts on income disregards. However, for the MAGI population – which is virtually everyone under age 65 who is not on Medicare – their income will now be determined under new rules, based on federal income tax concepts – called “Modifed Adjusted Gross Income” . There are good changes and bad changes.
GOOD: Veteran’s benefits, Workers compensation, and gifts from family or others no longer count as income.
BAD: There is no more “spousal” or parental refusal for this population and some other rules. For all of the rules see:
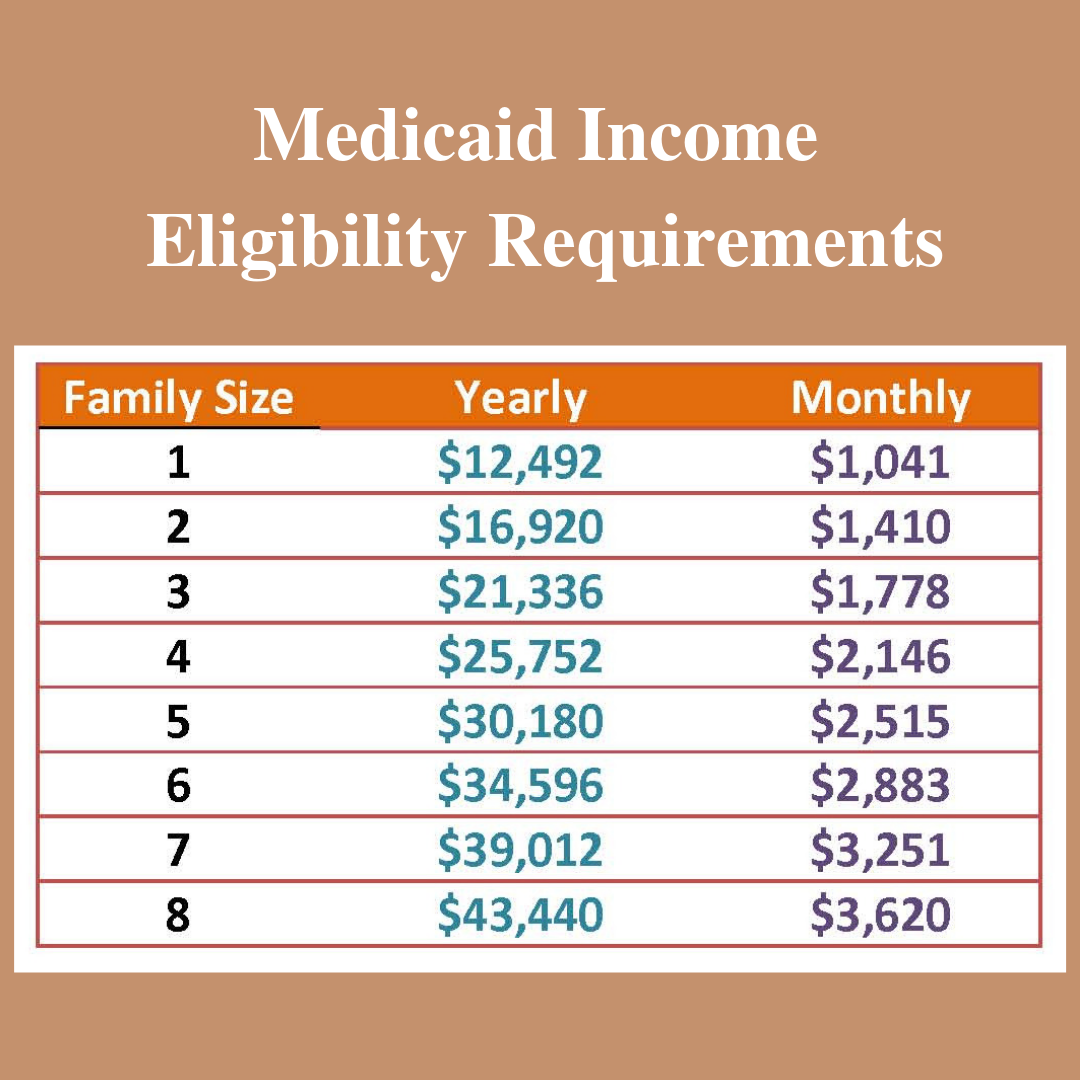
Household Gross Income Is Then Compared To The Limits Shown Below Based On Household Size For The Applicable Program
Eligibility is determined for medicaid first, then chip using. Some states are expanding their medicaid programs. Every year the medicaid rules change regarding the value of assets one can own, and the amount of income one can have, and still qualify for long term care. (this figure is equivalent to.
Recommended Reading: Does Medicaid Cover Long Term Care Facilities
How To Apply For Medicaid
If youâre eligible for Medicaid, you can apply all year round through your state’s Medicaid website or HealthCare.gov, the federal health insurance marketplace. If you apply for Medicaid through Healthcare.gov and it looks like you qualify, the federal government will notify your state agency, which will contact you about enrollment. States also generally let you print out paper applications you can mail, fax or return directly to your local government office.
To complete your Medicaid application, you will likely need to provide documentation that you meet your state’s requirements. This documentation may include:
-
Your birth certificate or driver’s license to serve as proof of age and citizenship
-
Recent pay stubs or tax returns to serve as proof of income
-
Copies of bank statements
-
Proof of address, which could include a lease, utility bill statements or a copy of your mortgage
-
Medical records to serve as proof of disability
States have 45 days to process your Medicaid application. They have 90 days if eligibility is tied to a disability . Processing can take longer if applicants do not supply all of the required documentation. If you don’t qualify for Medicaid, you might be able to get subsidized health insurance through Healthcare.gov. However, only certain life events allow you to apply for a marketplace health care plan outside of open enrollment, which takes place from Nov. 1 to Jan. 15.
Free in your inbox each Friday.
Sign up now
Medicaid For The Working Disabled
Eligibility for Medicaid for the Working Disabled is based on the current year Federal Poverty Level guidelines. Medicaid for the Working Disabled has higher income and resource eligibility guidelines than MABD.
- The monthly income limit for individuals who are blind or disabled, and who work at least a few hours each month, is 250% FPL.
- There is a resource test for Medicaid for the Working Disabled. The limit is $10,000 for one person and $15,000 for a couple. See our Resource Limits Medicaid page.
Don’t Miss: What Is Medicaid Buy In Program
How Much Is Va P
Storen said Virginia will continue to issue monthly benefits at least through the end of the 2020-2021 academic year to families of students learning virtually or in a hybrid format. Fully remote students will receive $121.40 per month and hybrid students will receive $60.70 per month on P-EBT cards, according to DSS.
How To Calculate Magi For Medicaid Eligibility
Follow the steps below, to calculate your MAGI for Medicaid Eligibility. Please note that this includes estimating any future income that may impact your MAGI.
Step 1
Calculate your households adjusted gross income by using your most recent federal income tax return. Additionally, you can find your AGI on line 7 of IRS Form 1040.
Step 2
Second, add the following types of income to your AGI:
- Tax-exempt foreign income
Do not include Supplemental Security Income .
Step 3
Lastly, adjust your estimate for any changes you expect.
Be sure to consider things future changes or adjustments for all members of your household, such as:
- Expected raises
- New jobs or other employment changes, including changes to your work schedule or self-employment income
- Include changes to income from other sources, like Social Security or investments
- Changes in your household, like gaining or losing dependents. Gaining or losing a dependent can have a big impact on your savings.
In conclusion, you now have successfully calculated your MAGI. Additionally, you should have an estimate of your expected income.
You May Like: Having A Baby On Medicaid
Nevada Medicaid Income Limit
The Nevada Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the Nevada Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 160 percent of FPL
- Any child age 1-5 with a family income up to 160 percent of FPL
- Children ages 6- 18 with family income up to 133 percent of FPL
- CHIP for children with family income up to 200 percent of FPL
- Pregnant women with family income up to 160 percent of FPL
- Parents of minor children with family income up to 31 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 74% of the FPL
- Adults without dependents under Medicaid expansion with income up to 133% of the FPL
Income And Resource Limits For New York State Public Health Insurance Programs
NYS updated the 2021 levels with GIS 21 MA/06 -with the 2021 Federal Poverty Levels
- Attachment I
- Attachment III MAGI levels for 2021
- Attachment IV MAGI levels for 2021
- Attachment V PICKLE reduction factors – see more about Pickle here
|
Disabled, 65+ or Blind and have Medicare |
MAGI *138% FPL***Children < 5 and pregnant women have HIGHER LIMITS than shown |
For MAGI-eligible people over MAGI income limit up to 200% FPL No long term care. |
|
| $884 | $1300 | $1,482 | |
|
$15,900 |
$23,400 |
NO LIMIT** | NO LIMIT |
* MAGI and ESSENTIAL plan levels are based on Federal Poverty Levels, which are not released until later in 2021. 2020 levels are used until then.
NEED TO KNOW PAST MEDICAID INCOME AND RESOURCE LEVELS?
HOW TO READ THE HRA Medicaid Levels chart –
MAGI INCOME LEVEL of 138% FPL applies to most adults who are not disabled and who do not have Medicare, AND can also apply to adults with Medicare if they have a dependent child/relative under age 18 or under 19 if in school. 42 C.F.R. § 435.4.
Certain populations have an even higher income limit –
- 224% FPL for pregnant women and babies < age 1,
- 154% FPL for children age 1 – 19.
- See all income limits on MAPDR-01 HRA income limits chart.
Don’t Miss: Anthem Healthkeepers Plus Medicaid Transportation
Elderly Individuals Who Would Require Nursing Home Care If Not For Special Services Performed In Their Home
Elderly individuals living independently in their own homes may be eligible for South Dakota Medicaid.
Eligibility Requirements
- A person must be in need of nursing facility care.
- A person must not be a resident of a hospital, nursing facility or an intermediate care facility for the mentally retarded.
- A person must be a resident of South Dakota and meet certain citizenship requirements of the United States.
- The monthly income limit is 300 percent of the SSI Standard Benefit Amount.
- The resource limit is $2,000. Resources include items such as checking or savings accounts and certificates of deposit.
to the standard Medicaid covered services
Homemaker Services: Teaching and providing home management skills, promoting self-care, making beds, changing linens, washing dishes, laundry work, floor care and housecleaning. Providing meal preparation, shopping and menu planning. Providing non-South Dakota Medicaid in mobility, personal comfort and grooming of the individual. Arranging for transportation.
Private Duty Nursing: Nursing services provided by a licensed nursing professional for recipients with chronic and stable conditions who require more individual and continuous care than is available from a part-time or intermittent nursing service.
Adult Day Care: Services providing out-of-home structured health and social services on a regularly scheduled basis and in daytime settings.
Home And Community Based Services For Developmentally Disabled
Home and Community Based Services provides South Dakota Medicaid for individuals with developmental disabilities who would otherwise be institutionalized in a Medicaid-funded hospital, nursing facility or an intermediate care facility.
Eligibility Requirements
- A person must be developmentally disabled.
- A person must be aged, blind or disabled.
- A person must reside in the home of a parent, other relative, legal guardian, adult foster care home licensed by the state, special therapeutic foster home licensed by the state, community residential facilities approved by the Department of Human Services, supervised apartment approved by the Department of Human Services, or community habilitation facilities approved by the Department of Human Services of an individuals own home.
- A person’s monthly income must be less than 300 percent of the SSI Standard Benefit Amount . The resource limit is $2,000 for an individual. Resources include items such as checking and savings accounts and certificates of deposit.
to the standard Medicaid covered services
Case Management and Consumer Support: This includes adaptive equipment needed not to exceed $500 per person per year. Examples of adaptive equipment would be communication devices, eyeglasses, hearing aids, etc.
Other Information for Home and Community Based Services can be found here: Department of Human Services’ Division of Developmental Disabilities
Recommended Reading: Braces Place That Take Medicaid
Can Anyone Access My Bank Account
While many banks no longer allow for this, some banks will still provide general amount account balance amount information to people that simply call and request it. For example, if someone knows your checking account information, they can call the bank to verify funds on a check even if no check actually exists.
North Carolina Medicaid Income Limit
The North Carolina Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the North Carolina Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 210 percent of FPL
- Any child age 1-5 with a family income up to 210 percent of FPL
- Children ages 6- 18 with family income up to 133 percent of FPL
- CHIP for children with family income up to 211 percent of FPL
- Pregnant women with family income up to 196 percent of FPL
- Parents of minor children with family income up to 41 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 100% of the FPL
Also Check: Does Medicaid Cover Root Canals For Adults
