Staying On Health First Colorado
Usually, once approved for Health First Colorado , you continue to qualify as long as your situation doesnt change. If your income, immigration status, residency, or household size changes, let your county human services department know within 10 days of the change. You can do this in person, by phone, or by email. When you report your changes, the county tells you whether you continue to get Health First Colorado or if you have new health coverage options, like individual coverage with subsidies or the Medicaid Adult Buy-In.
Is It Right For You
Health First Colorado is government-funded health coverage for people in certain situations. You may qualify if you:
- Have low to moderate income, no matter how much you have in resources or whether you have a disability. Learn more about income-based Health First Colorado .
- Get Supplemental Security Income benefits or qualify for SSIs 1619 rule, which helps people who used to get SSI. In either case, you automatically get Health First Colorado coverage and dont need to worry about the rules discussed here. Learn more in DB101s SSI article.
- Have low income, low resources, and a disability, but don’t get SSI. Disability-based Health First Colorado is explained on this page.
- Have a disability and work, even if your income is higher and you have lots of resources. Learn more about the Health First Colorado Buy-In Program For Working Adults With Disabilities .
Answer the questions on this page to see if you might qualify for disability-based Health First Colorado . If you do, its probably your best health coverage option because:
- It doesnt usually have a premium and copayments are low
- It covers more services than most private insurance, and may help you qualify to get Home and Community-Based Services Waivers, and
- If you qualify for Health First Colorado , you cannot get government help paying for an individual plan on Connect for Health Colorado.
See If You Can Sign Up For Health First Colorado
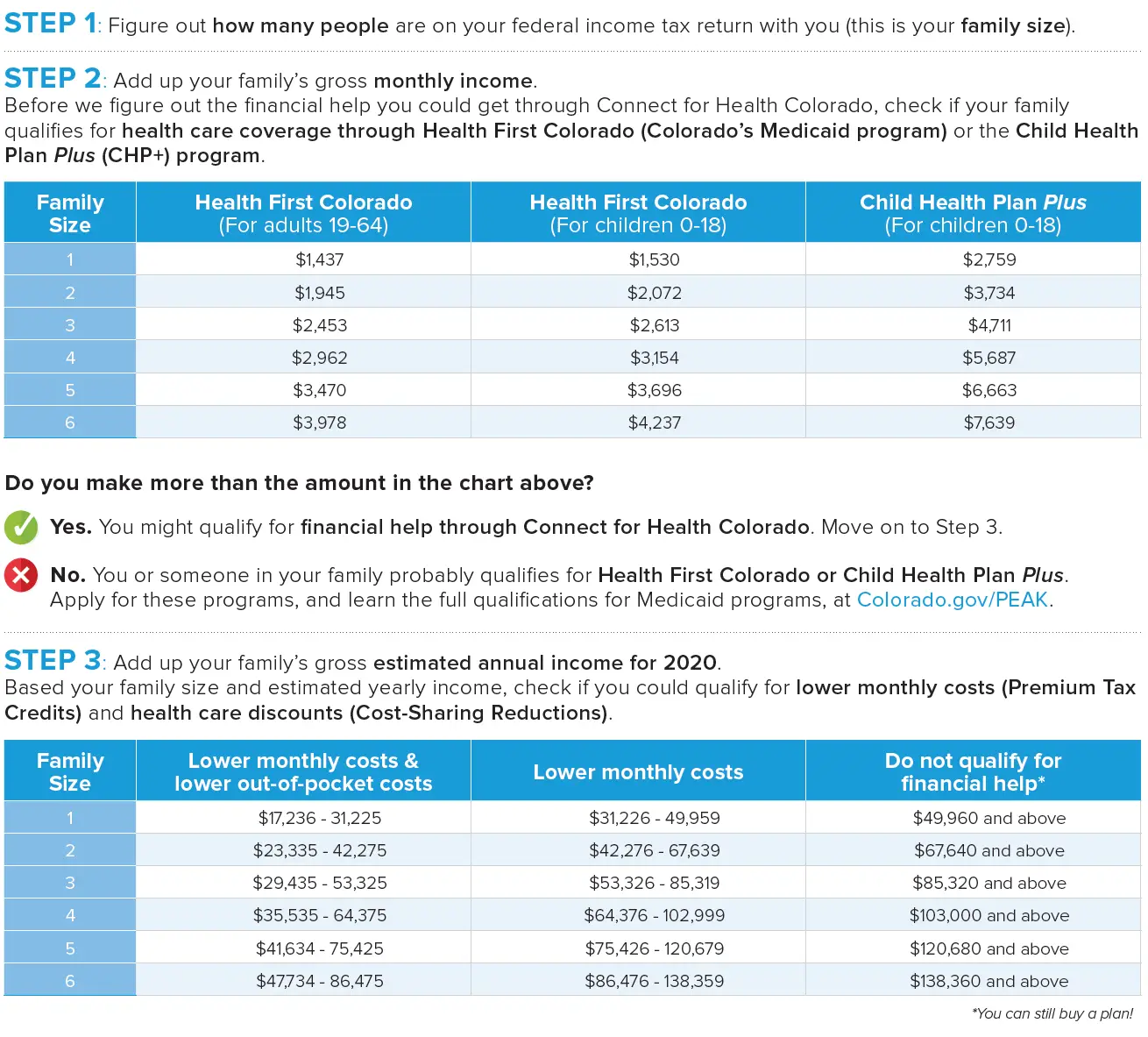
You may qualify for Health First Colorado if you meet the monthly income guidelines:
| Family Size |
Can I still sign up for a plan through Connect for Health Colorado if I qualify for Health First Colorado?
- Yes. You can still purchase a private health insurance plan at full price if you qualify for Health First Colorado.
- NOTE: If you qualify for Health First Colorado or CHP+, you will not qualify for financial help to lower the cost of your health insurance plan through Connect for Health Colorado. You will pay full price for your health insurance plan.
I applied through Connect for Health Colorado and was told that my application was sent to Health First Colorado. Whats next?
- Watch your mail or email. You will get a notification from the State of Colorado with your application results. You will also receive a letter or email if more information is needed to complete the process.
- You may also check the results of your application through your PEAK account.
- If you do not have a PEAK account, you can create one at Colorado.gov/PEAK.
- You can use your Connect for Health Colorado log-in and password information to sign into PEAK.
- You can also use PEAK to manage your Health First Colorado or CHP+ benefits, print benefit cards, report changes and more.
Also Check: Income For Medicaid In Michigan
Batch Electronic Claims Submission
Batch billing refers to the electronic creation and transmission of several claims in a group. Batch billing systems usually extract information from an automated accounting or patient billing system to create a group of claim transactions. Claims may be transmitted from the provider’s office or sent through a billing vendor or clearinghouse.
All batch claim submission software must be tested and approved by the Department’s fiscal agent. Any entity sending electronic transactions through the Health First Colorado file delivery and retrieval system secure website for processing or the Provider Web Portal where reports and responses will be delivered must complete an EDI Trading Partner enrollment. This provides EDI the information necessary to assign a Logon Name, Logon ID, and Trading Partner ID, which are required to submit electronic transactions, including claims.
If the file contains syntactical error, the segment and element where the error occurred will be reported.
Testing and Vendor Certification
Completion of the testing process must occur prior to submission of electronic batch claims to the Colorado interChange. The EDI testing packet and Companion Guides are available on the EDI Support web page.
Do You Get Supplemental Security Income
If you get SSI benefits, or qualify for SSIs 1619 rule, which helps people who used to get SSI, you automatically get Health First Colorado coverage and dont need to worry about the other rules discussed here. Learn more in DB101s SSI article.
If you get SSI or qualify for 1619, you have Health First Colorado coverage!
If not, keep reading this page to see if disability-based Health First Colorado might be right for you.
You May Like: Medicaid Brooklyn Ny Phone Number
Other Health Care Options
If you are denied Health First Colorado coverage, you may be eligible for other health care programs.
- Connect for Health Colorado is a new online health insurance marketplace that opened on October 1, 2013. This marketplace is sometimes referred to as the health insurance exchange. Individuals, families and small employers can shop for and buy health insurance through the Connect for Health Colorado website. Boulder County is a Certified Connect for Health Colorado Assistance Site and has trained Health Coverage Guides to help residents enroll in health insurance. Call 303-441-1000 or email for more information or to make an appointment with a Health Coverage Guide.
- Child Health Plan Plus a low-cost health insurance program for uninsured Colorado children ages 18 and under whose families earn too much to qualify for Health First Colorado.
- Colorado Indigent Care Program is a discount rate offered at some clinics and hospitals for eligible Colorado residents.
There are several ways to apply for benefits. Once you apply, we will contact you for a required interview.
Select the one option that is best for you:
Electronically:
- Apply online at Colorado PEAK
Paper:
Breast And Cervical Cancer Program
The Breast and Cervical Cancer Program is for uninsured or underinsured women who have been diagnosed with breast or cervical cancer. BCCP also covers breast and cervical conditions that may lead to cancer if not treated.
Who Qualifies?
In order to apply for this program you must:
- be diagnosed with breast or cervical cancer or conditions that may lead to cancer if left untreated
- be between the ages of 40 and 64
- have an income less than 250% of the Federal Poverty Level
- not have health insurance that covers breast or cervical cancer treatments
- not be currently enrolled in Health First Colorado and are not eligible for Medicare
- be a U.S. citizen or a qualified non-citizen
Top Benefits:
- access to all Health First Colorado covered services
- breast reconstruction after breast cancer surgery
Co-pay Costs:
Co-pay costs vary depending on the service. View the co-pay amounts per service in the Health First Colorado Benefits and Services Overview.
| Program Information Page |
Recommended Reading: What’s The Income Level For Medicaid
Health First Colorado Member Billing
Providers agree to accept Health First Colorado payment as payment in full for benefit services. Colorado law ) provides that no Health First Colorado member shall be liable for the cost, or the cost remaining after payment by Health First Colorado, Medicare, or a private insurer, of medical benefits authorized under Title XIX of the Social Security Act. This law applies whether or not Health First Colorado has reimbursed the provider, whether claims are denied by Health First Colorado due to provider error, and whether or not the provider is enrolled in Health First Colorado. This law applies even if a Health First Colorado member agrees to pay for part or all of a covered service. This law also prohibits providers from billing Health First Colorado members or the estates of deceased Health First Colorado members for Health First Colorado benefit services. Refer to the Health First Colorado policy on Member Billing.
Old Age Pension Health And Medical Care Program
The Old Age Pension Health and Medical Care Program provides limited medical care for Coloradans getting Old Age Pension. If you get Old Age Pension and make too much to qualify for Health First Colorado , you may qualify.
The OAP Health and Medical Care Program is also known as the Modified Medical Plan, State Medical Program, Limited Medicaid and OAP State Only Program.
Who Qualifies?
- You must get Old Age Pension,
- You do not qualify for Health First Colorado , and
- You are not a patient in an institution for tuberculosis or mental disease.
If you do not qualify for the OAP Health and Medical Care Program you may have other coverage options.
| Program Information Page |
You May Like: Which Of The Following Services Are Mandated Medicaid Basic Benefits
Applying For Colorado Medicaid Long Term Care Programs
The first step in applying for Health First Colorado Long Term Care coverage is deciding which of the three Medicaid programs discussed above you or your loved one wants to apply for Nursing Home Medicaid, Home and Community Based Service Waivers or Aged Blind and Disabled Medicaid / Regular Medicaid.
The second step is determining if the applicant meets the financial and functional criteria, also discussed above, for that Long Term Care program. Applying for Health First Colorado when not financially eligible will result in the application, and benefits, being denied.
During the process of determining financial eligibility, its important to start gathering documentation that clearly details the financial situation for the Health First Colorado applicant. These documents will be needed for the official Medicaid application. Necessary documents include five years of quarterly bank statements from all accounts the most recent monthly or quarterly statements from all investments, IRAs, 401Ks, annuities and any other financial accounts a letter from the Social Security Administration showing the applicants gross Social security income and deductions tax forms to verify income streams including wages, pensions, royalties and interest lists of items of any trusts proof life insurance and a list of beneficiaries Power of Attorney documentation.
Choosing a Colorado Medicaid Nursing Home
What Does Medicaid Cover
If you are age 65 or older and eligible for Supplemental Security Income and/or Old Age Pension state supplemental payments, you will be eligible for Medicaid. Medicaid covers some of the same kinds of services as Medicare and also covers a number of medical services Medicare does not. It covers most long-term care, including long-term skilled nursing care, and nonmedical personal care such as adult day care and at-home assistance with the activities of daily living.
Additionally, if you are found to be eligible, Medicaid may cover some of these bills retroactively. Retroactive eligibility can go back to the beginning of the third month before the date you filed your application. In order to be covered by Medicaid, the client must make sure that the care was prescribed by a doctor, administered by a provider who participates in Medicaid, and determined to be medically necessary.
Read Also: What Does Nc Family Planning Medicaid Cover
What You Need To Apply
- Social security numbers for applicants who have them
- Immigration document numbers for non-citizens
- The name, address, contact info, and birth date for applicants
- Employer and income information for everyone in your household. Examples include pay stubs or W2 forms.
- Other income information including Social Security Administration or Supplemental Security Income payments and mentions
- Information and policy numbers for health insurance plans covering members of your household, including Medicare
We may ask for more information if we cant verify what you tell us through our electronic data sources.
Apply now
What Are The Income Rules In Colorado On Medicaid
Do you think you have too many assets to qualify for Medicaid assistance with nursing home costs? Think again.
At The Hughes Law Firm, P.C., in Denver, we help people just like you qualify for Medicaid benefits as well as provide assistance with many issues of elder law, VA benefits and estate planning. Let our lawyers help you understand how Colorados Medicaid income rules work.
You May Like: Walk In Clinic Takes Medicaid
Eligibility Requirements For Medicaid In Colorado
Every state has a Medicaid program, and Colorado is no exception to this rule. You can find out a lot about the eligibility requirements for Medicaid in Colorado by reading over the Colorado Department of Health Care Policy and Financing. Colorado is one of the states that will expand its Medicaid program.
Medicaid is a public, or government run, form of health insurance. It is designed to provide health insurance coverage to people who are low-income and who cannot afford to purchase a health plan from a private insurance company. Medicaid is funded, in part, by the federal government. It is also funded by an individual state.
In April of 2012, Colorado made the decision to expand its Medicaid program. There is a provision in the Affordable Care Act that extends the federal dollar-for-dollar match that already exists within Medicaid funding to cover adults who do not have children. States can receive funding to expand their Medicaid program in this way.
The Medicaid program in Colorado is administered by the Colorado Department of Health Care Policy and Financing. People who live in Colorado can go to that website to learn more about the eligibility requirements for Medicaid and how to apply for the coverage through this program.
Image by BrianSwan on Flickr
How Does Medicaid Provide Financial Assistance To Medicare Beneficiaries In Colorado
Many Medicare beneficiaries receive Medicaid financial assistance that can help them with Medicare premiums, lower prescription drug costs, and pay for expenses not covered by Medicare including long-term care.
Our guide to financial assistance for Medicare enrollees in Colorado includes overviews of these programs, including Medicaid nursing home benefits, Extra Help, and eligibility guidelines for assistance.
Don’t Miss: Will Medicaid Pay For Nose Surgery
How Do I Enroll In Medicaid In Colorado
If you think you may qualify for Medicaid, you can apply a number of ways:
- Online at Colorado PEAK. Colorado PEAK is a website for applying for food, cash, and medical assistance programs. Colorados state-run health insurance exchange connects with PEAK, so youll be able to enroll in Medicaid or CHIP if you start at the exchange website, too.
What Are The Different Types Of Care Available
The Medicaid programs available in each state are: regular Medicaid, Medicaid for long-term nursing home care, and Medicaid for home-based nursing care.
Regular Medicaid is the health care benefits program available to all of a states residents, providing they meet the eligibility requirements. Some of the eligibility requirements include:
- Legal status on the United States
- Resident of the state of application
Those who meet these criteria are able to use their regular Medicaid benefits for their doctors visits, hospital care, laboratory testing, and transportation for medical purposes.
The income limit for regular medicaid will be a set amount, depending on state and marital status. Some states allow one lump sum for a married couple and others have an income limit per spouse.
Medicaid for long-term nursing home care is for those who are elderly and can no longer live independently, those with chronic illness, and people with disabilities. At the facility, the residents receive 24/7 supervision and medical care, as well as lodgings and meals.
All state residents who meet the eligibility criteria and require long-term nursing home care are entitled to and will receive the care. There are no waitlists or lotteries for this benefit and you cant be denied if you meet the eligibility requirements.
Also Check: Does Medicaid Cover Lap Band Surgery
Health First Colorado Program Who Might Be Eligible
- Individuals and families who meet income limits
- Children under 19For information about childrens Medicaid benefits see Healthy Communities.
- Children with a disability
- People ages 16-64 who are working and have a disability
- Health First Colorado Buy-in Program for Working Adults with Disabilities provides adults with disabilities, who earn too much income or have too many resources the opportunity to purchase Health First Colorado benefits. Clients will pay a monthly premium based on their income. For more information see, HCPF:Adult Buy-In.
If you need nursing home or home and community based services , please see below for information about Long-term Care Medicaid.
People Age 65 and Over: People age 65 or older who are eligible for Supplemental Security Income and/or Old Age Pension state supplemental payments are eligible for Health First Colorado.
Recommended Reading: Therapists Baton Rouge Accept Medicaid
Aca Medicaid Eligibility Expansion In Colorado
One of the Affordable Care Acts primary strategies for reducing the uninsured rate is Medicaid expansion to cover low-income adults under the age of 65.
Medicaid expansion was a required element of the ACA as originally written. However, a coalition of states challenged Medicaid expansion and several other provisions of the ACA, and the case ended up before the Supreme Court in 2012. While the Court rejected most of the challenges, it did rule that Medicaid expansion was optional.
Fortunately for Colorados uninsured residents, the state opted to expand Medicaid. Then-Governor John Hickenlooper signed the legislation authorizing Medicaid expansion in May 2013.
As of 2022, Medicaid expansion enrollment in Colorado was 547,571, accounting for more than a third of the states total Medicaid enrollment.
Medicaid enrollment in Colorado grew by 72% in the first two years of Medicaid expansion implementation. Medicaid enrollment growth had largely leveled off by 2016/2017, but it spiked again in 2020, due to the COVID pandemic, and has continued to grow every since.
The Families First Coronavirus Response Act, enacted in March 2020, provides states with additional federal Medicaid funding. But as a condition of receiving that funding , states are prevented from disenrolling anyone from Medicaid unless they move out of state or request a coverage termination. This means that the normal eligibility redetermination process has not been happening since early 2020.
Also Check: Medical Supplies That Accept Medicaid