How To Apply For Medicaid
If youâre eligible for Medicaid, you can apply all year round through your state’s Medicaid website or HealthCare.gov, the federal health insurance marketplace. If you apply for Medicaid through Healthcare.gov and it looks like you qualify, the federal government will notify your state agency, which will contact you about enrollment. States also generally let you print out paper applications you can mail, fax or return directly to your local government office.
To complete your Medicaid application, you will likely need to provide documentation that you meet your state’s requirements. This documentation may include:
-
Your birth certificate or driver’s license to serve as proof of age and citizenship
-
Recent pay stubs or tax returns to serve as proof of income
-
Copies of bank statements
-
Proof of address, which could include a lease, utility bill statements or a copy of your mortgage
-
Medical records to serve as proof of disability
States have 45 days to process your Medicaid application. They have 90 days if eligibility is tied to a disability . Processing can take longer if applicants do not supply all of the required documentation. If you don’t qualify for Medicaid, you might be able to get subsidized health insurance through Healthcare.gov. However, only certain life events allow you to apply for a marketplace health care plan outside of open enrollment, which takes place from Nov. 1 to Jan. 15.
Free in your inbox each Friday.
Sign up now
Health Care With Heart
There is a reason more Ohioans choose CareSource for their Medicaid plan than all other plans combined. Its because CareSource is more than just quality health care. We care about you and your familys health and wellbeing. CareSource members get access to a large provider network, reward programs like Kids First and Babies First®, free rides to health care appointments, pharmacies and more. Plus, we never charge a copay for any medical or behavioral health service!
Choose CareSource for your Ohio Medicaid health care plan and join over 1.2 million members who trust us with their health and well-being.
Sign Up For Our Weekly Newsletter
Portland, Maine Office:
Phone: 202-903-0101
State Goals
- Make more effective use of data, data matching, and demonstrating return on investment :
- Review Medicaid data on individuals with intellectual and/or developmental disabilities to identify those eligible for additional housing supports.
- Create data sharing agreementsto share data among Medicaid, I/DD, mental health, and housing
- Illinois Department of Human Services
- Illinois Department of Healthcare and Family Services
- Illinois Housing Development Authority
- Illinois Council on Developmental Disabilities
State Successes
Next Steps
- Continue review of health and hospital projects for potential state system data matching and housing initiative opportunities.
- Continue work on pre-tenancy and tenant supports for Illinois residents.
- Explore expansion or new avenues for services typically covered through Medicaid Section 1115 waivers for other populations, especially I/DD populations.
Sessions:
Closing Remarks
From 2016 to 2018, she was the Chief Health Policy Advisor in the Office of Lt. Governor Nancy Wyman, coordinating the states health reform initiatives.
Recommended Reading: How Do I Apply For Medicaid Over The Phone
Ohio Medicaid Expansion Update
Governor Kasich announced in early 2013 that Ohio would expand Medicaid under the ACA.
Ohio lawmakers who were opposed to Medicaid expansion brought a lawsuit against the Kasich administration in an effort to block expansion.
Ultimately, in late 2013, the Ohio Supreme Court ruled in favor of Governor Kasich, and Medicaid expansion took effect as scheduled in 2014.
As of June 2019, there were 526,100 Ohio residents enrolled in expanded Medicaid.
Additionally, during the 2015 legislative session, lawmakers agreed to allow Medicaid expansion to continue as a part of a budget agreement.
Therefore, there was no separate legislation on Medicaid expansion.
Ohios Medicaid work requirement waiver was approved in 2019 but has been delayed due to COVID.
Where Can Medicare Beneficiaries Get Help In Ohio
Ohio Senior Health Insurance Information Program
You can access free counseling about Medicare benefits through the Ohio Senior Health Insurance Information Program at 800-686-1578.
The OSHIIP can help you enroll in Medicare, compare and change Medicare Advantage and Part D plans, and answer questions about state Medigap protections. OSHIIP counselors may also be able to provide referrals for local home care or long-term care services. This website has more information about the services OSHIIP offers.
Elder law attorneys
Elder law attorneys can help individuals plan for Medicaid long-term care benefits. You can use this National Academy of Elder Law Attorneys search feature to find an elder attorney locally.
Also Check: Find Primary Care Doctor Medicaid
Who’s Eligible For Medicaid For The Aged Blind And Disabled In Ohio
Medicare covers a great number services including hospitalization, physician services, and prescription drugs but Original Medicare doesnt cover important services like vision and dental benefits.
Medicare can also leave its enrollees with large co-pays, coinsurances and deductibles. Some beneficiaries those whose incomes make them eligible for Medicaid can receive coverage for Medicare cost sharing and services only Medicaid covers if theyre enrolled in Medicaid for the aged, blind and disabled .
In Ohio, Medicaid ABD covers extensive dental benefits, including cleanings, x-rays, extractions, fillings, and dentures. Medicaid ABD also covers one eye exam and a pair of eyeglasses every 12 months for adults 60 and older.
Asset limits: The asset limit is $2,000 if single and $3,000 if married.
Help with prescription drug costs in Ohio
Medicare beneficiaries who have limited incomes and assets can apply for Extra Help a federal program that lowers prescription drug expenses under Medicare Part D. The income limit is $1,615 a month for singles and $2,175 a month for couples, and the asset limit is $14,610 for individuals and $29,160 for spouses.
How Do I Become Eligible For Medicaid In My State
Most states have multiple pathways to Medicaid eligibility. Furthermore, many states allow the use of Miller Trusts or Qualified Income Trusts to help person who cannot afford their care costs to become Medicaid eligible. There are also Medicaid planning professionals that employ other complicated techniques to help person become eligible.
Don’t Miss: What Is The Income Limit For Arkansas Medicaid
How To Choose Caresource
Medicaid health care coverage is available for eligible Ohioans with low income, pregnant women, infants and children, older adults and individuals with disabilities.
| Choose CareSource |
|---|
| When you apply for Ohio Medicaid, you can choose CareSource as your managed care plan. Whether you apply online, by mail, over the phone or at your local Department of Job and Family Services , tell them you want to choose CareSource. |
| Switch to CareSource |
|---|
| If you were assigned to another managed care plan and want to switch to CareSource, call the Ohio Medicaid hotline, complete a change request within 90 days and tell them you want to switch to CareSource. If you have been on your plan more than 90 days, you can switch to CareSource during your next open enrollment period. |
Medicaid Eligibility In Ohio
Funded by both the federal and state government, the health insurance program known as Medicaid was designed with low-income families in mind. Children, elderly, and disabled members of society are often first among the list of eligible applicants in the state of Ohio. Before applying, it is important to note the states specific criteria for getting approved and accepted into the program to receive coverage.
Read Also: How Do I Qualify For Medicare And Medicaid
Are There Options If I Make More Than The Limit
There might be some options to still receive Medicaid benefits if you make more than the income limit in your state.
The options do differ from state to state, but the majority do offer a pathway for those who would be considered medically needy and have high medical expenses.
If someone who requires a lot of medical care has too high of an income, they might be able to spend that income on their medical costs and then have that count against their income.
For example, if someone was $500 over the income limit in their state and that state has a program for the medically needy, they might be permitted to spend that excess income on their medical expenses and then receive Medicaid benefits after. This helps those with high than average medical costs be put on more equal footing for income eligibility requirements.
Not every state offers this particular program, however. For a great resource on the sorts of waivers, exceptions, and other eligibility information, visit this website. Once you click on your state of residence, you should be able to see which waivers are available in your state for those who exceed the income limit.
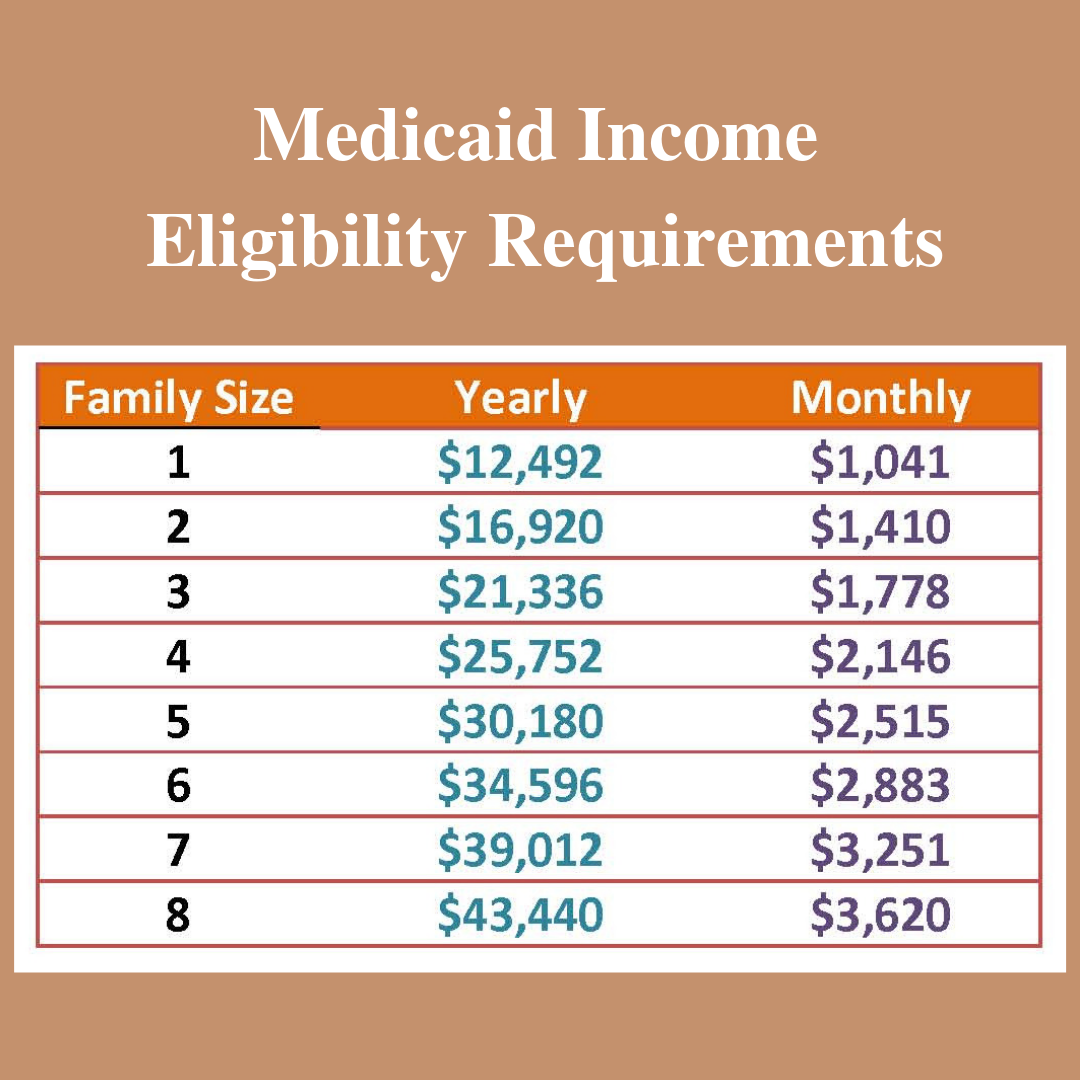
What Are The Medicaid Income Limits For 2022
Finding out if you are eligible for Medicaid can be quite a headache. Since Medicaid is jointly funded by federal and state governments, there are different eligibility criteria for each state! One of the biggest factors for Medicaid eligibility are the income limits.
If you are trying to learn more about whether your income is within the Medicaid income limit for your state of residence, then you are reading the right article!
I will be explaining which sources of monthly incoming money are considered income, how each state decides their income limit, and providing an easy-to-use list of each states income limits for the year 2022.
Read on to learn more about Medicaid income limits and determine if your income would be considered within the limit set by your state of residence!
Don’t Miss: Apply For Emergency Medicaid Utah
Does Ohio Help With My Medicare Premiums
Many Medicare beneficiaries who struggle to afford the cost of Medicare coverage are eligible for help through a Medicare Savings Program . In Ohio, these programs pay for Medicare Part B premiums, Medicare Part A and B cost-sharing, and in some cases Part A premiums.
- Qualified Medicare Beneficiary : The income limit is $1,063 a month if single and $1,437 a month if married. QMB pays for Part A and B cost sharing, Part B premiums, and if a beneficiary owes them it also pays their Part A premiums.
- Specified Low-Income Medicare Beneficiary : The income limit is from QMB levels up to $1,276 a month if single and $1,724 a month if married. SLMB pays for Part B premiums.
- Qualified Individuals : The income limit is from SLMB levels up to $1,436 a month if single and $1,940 a month if married. QI pays for Part B premiums.
MSP asset limits: The asset limits for QMB, SLMB and QI are $7,860 if single and $11,800.
What Are The Medicaid Programs In Ohio
The Ohio Medicaid Schools Program. The Medicaid School Program has been developed to include federal Medicaid matching funding for medically necessary therapy services, certain administrative activities, and specialized transportation associated with accessing therapy services. Direct MSP providers include traditional school districts
You May Like: Who Is Eligible For Medicaid In Nebraska
What Are The Different Types Of Care Available
The Medicaid programs available in each state are: regular Medicaid, Medicaid for long-term nursing home care, and Medicaid for home-based nursing care.
Regular Medicaid is the health care benefits program available to all of a states residents, providing they meet the eligibility requirements. Some of the eligibility requirements include:
- Low-income
- Legal status on the United States
- Resident of the state of application
Those who meet these criteria are able to use their regular Medicaid benefits for their doctors visits, hospital care, laboratory testing, and transportation for medical purposes.
The income limit for regular medicaid will be a set amount, depending on state and marital status. Some states allow one lump sum for a married couple and others have an income limit per spouse.
Medicaid for long-term nursing home care is for those who are elderly and can no longer live independently, those with chronic illness, and people with disabilities. At the facility, the residents receive 24/7 supervision and medical care, as well as lodgings and meals.
All state residents who meet the eligibility criteria and require long-term nursing home care are entitled to and will receive the care. There are no waitlists or lotteries for this benefit and you cant be denied if you meet the eligibility requirements.
Medicaid If You Are 19 Or Older
If you are 19 or older, you may qualify for income-based Medicaid if your familys income is 138% of FPG or less . If you are pregnant, you can have income up to 205% FPG . It doesn’t matter how much your family has in resources or whether you have a disability.
Check whether your income is low enough for you to get income-based Medicaid:
Your family size:If you have a disability, don’t get SSI, and make too much for income-based Medicaid, you may qualify for disability-based Medicaid or for MBIWD.
You may see the income limit for income-based Medicaid listed as 133% of the Federal Poverty Guidelines in some places. However, when Medicaid counts your income, theyll knock 5% of FPG off your income if you make more than 133% of FPG. That’s why we say that you can make up to 138% of FPG, because it more accurately shows how much income you could have and still get Medicaid. For pregnant women, this means we show 205% of FPG as the limit, rather than 200%.
Learn more about income-based Medicaid for adults in DB101’s How Health Benefits Work article.
If you dont qualify for Medicaid or MBIWD, look into other health coverage options on Healthcare.gov. Learn more about private health insurance.
Don’t Miss: Medicaid Change Plan Phone Number
What Do I Need For Proof Of Income
In order to prove that you fall within the limit for income eligibility, you will need to provide documentation of all sources of income that you have.
Documents to include are things like pay stubs from wages, copies of social security deposits, copies of alimony checks, and award letters from any other monthly financial benefit that you may receive.
It would also be helpful to have all of your most recent income tax returns and any other tax forms that would be relevant to verifying your income.
Some states are able to electronically gather the resources to verify your income, which does simplify the process as well as eliminate fraud. To find out if your state has this technology for your application, click here to learn more about the application process in your state of residence.
How Much Does Medicaid Cost In Ohio
More than $21 billion gets spent on Ohio Medicaid costs. The federal government shares these expenses with the state, with Ohio allocating over 37 percent of their budget to its funding. This amount will only grow over time, as there are plans to expand the program to ensure more people who need coverage can receive it.
You May Like: How To Apply For Pregnancy Medicaid Ga
Income Requirements For Ohio Medicaid
Household size and total amount of income versus outgoing bills plays a part in determining the income limit for each family. Single-family households can make up to $15,800 per year, while a four-person family can bring in $32,319 per year to qualify. Those who fall well below the poverty line, as well as children and pregnant women, qualify most often.
B Gift And Medicaid Compliant Annuity
Individuals often require long-term care without having engaged in any prior planning. They desire to apply for Medicaid, but have assets greatly in excess of the $2,000 limit, which they would like to preserve for their family. In such situations, it may be possible to save a significant portion of a persons assets, while still allowing them to qualify for Medicaid. This requires dividing the individuals assets into two shares: the Gifted Share and the Medicaid-Compliant Annuity Share. The Gifted Share is generally given to the individuals children or to an irrevocable trust for their benefit. The Medicaid-Compliant Annuity Share is used to purchase a special annuity that is not counted as an asset for Medicaid purposes. The annuity produces a monthly stream of payments. The objective is to preserve the assets gifted to the children by using the Medicaid-Compliant Annuity to pay through the penalty period created by the improper transfer.
Dividing Assets into “Gifted Share” and “Medicaid-Compliant Annuity Share”:
Also Check: Medicaid Breast And Cervical Cancer Program Texas
Submit Your Application Online
The quickest and easiest way to apply for health care benefits is to call 1-844-640-6446 and follow the prompts. You may also apply online at www.benefits.ohio.gov. There you will answer a series of questions and your answers will direct you to the correct application for health care.
- If your income is within the new legal limit implemented by Medicaid Expansion , you will be directed to the citizens self-service portal.
- If your income is above 205 percent of the Federal Poverty Level, you will be directed to the Federally Facilitated Health Insurance Marketplace to shop for health care.
After you submit your application online, you may be asked to send verification documents to Hamilton County Job and Family Services. The best way to return documents is to fax them to 946-1076. You can fax documents for free from any Public Library of Cincinnati and Hamilton County branch.
Visit www.healthcare.gov or www.benefits.ohio.gov to learn more or call the Medicaid Consumer Hotline at 1-800-324-8680. Representatives are available to answer questions related to eligibility for Medicaid due to the Affordable Care Act and Medicaid Expansion and answer questions about where to apply.
How Does Ohio Regulate Long
Medicare beneficiaries increasingly rely on long-term services and supports or long-term care which is mostly not covered by Medicare. In fact, 20 percent of Medicare beneficiaries who lived at home received some assistance with LTSS in 2015. Medicaid fills this gap in Medicare coverage for long-term care, but its complex eligibility rules can make qualifying for benefits difficult. Whats more eligibility rules vary significantly from state to state.
Medicaid nursing home coverage
In past decades, most Americans received long-term care services in nursing homes. Medicaid covers these services for an unlimited number of enrollees in each state who meet income and resource limits.
Income limits: The income limit is $2,349 a month if single and $4,698 a month if married .
When only one spouse needs nursing home care, the income limit for single applicants is used and usually only the applying spouses income is counted. Non-applying spouses are allowed to keep a portion of their Medicaid spouses income.
This income limit doesnt mean nursing home enrollees can keep all of their income up to the limit. Nursing home enrollees have to pay nearly all their income toward their care, other than a small personal needs allowance and money to pay for health insurance premiums .
Assets limits: The asset limit is $2,000 if single and $3,000 if married . If only one spouse has Medicaid, federal rules allow the other spouse to keep up to $128,640.
Estate recovery in Ohio
You May Like: Is There A Copay With Medicaid
