Medicaid Expansion With A Ballot Initiative
In Maine, Utah, Idaho, Nebraska, Oklahoma, and Missouri, Medicaid expansion came about as a result of ballot initiatives passed by voters.
So far, Medicaid expansion ballot initiatives have passed in 100% of the states that have had them on the ballot .
A Medicaid expansion measure might be on the ballot in South Dakota in 2022. Medicaid expansion advocates in Mississippi had been working to gather signatures for a 2022 ballot measure, but suspended their campaign after a Mississippi Supreme Court decision that currently makes it impossible for a signature-gathering campaign to be successful in the state.
What Was The Income Eligibility
The minimum federal level to cover these individuals:
- Children and pregnant women up to 133% FPL
- Parents varies from 25%-200% FPL by state
- Severely disabled, blind, or low-income elderly are covered through Social Security
- Non-disabled adults without dependent children were generally excluded from Medicaid unless the state obtained a waiver for them
Federal Action Needed To Cover Those Left Out
Millions of uninsured people with low incomes have experienced none of the gains of expansion simply due to where they live. The differences in health outcomes between expansion and non-expansion states are stark. While, as noted above, Medicaid expansion has saved the lives of at least 19,200 adults aged 55 to 64 from 2014 to 2017, non-expansion has cost the lives of another 15,600 such adults. The impact of expansion on racial disparities is particularly salient, because more than half of those who remain uninsured due to their states refusal to expand are people of color, most of whom live in the South.
About 2.2 million adults with incomes below the poverty line are uninsured in the 12 states that havent expanded Medicaid . They have no pathway to affordable coverage because their incomes are too low to qualify for subsidies in the marketplace and they dont qualify for their states underlying Medicaid programs, which generally provide coverage for adults without a disability only for parents with very low incomes. Those who lack coverage are mostly people of color 28 percent are Black and 28 percent are Hispanic .
Read Also: Medicaid Texas Income Limits 2020
The Cost Of Not Expanding Medicaid Eligibility
Because the federal government funds nearly all of the cost of Medicaid expansion, the 14 states that havent yet taken action to expand Medicaid have been missing out on significant federal funding more than $305 billion between 2013 and 2022.
Just five states Florida, Texas, North Carolina, Georgia, and Tennessee would have received nearly 60% of that funding if they had expanded Medicaid to cover their poorest residents starting in 2013. The good news is that although the federal government is no longer funding the full cost to expand Medicaid, theyll always pay at least 90% of the cost, making the state Medicaid expansion a good deal for states regardless of when they implement it .
For residents of states that havent expanded Medicaid, their federal tax dollars are being used to pay for Medicaid expansion in other states, while none of the Medicaid expansion funds are coming back to their own states. From 2013 to 2022, $152 billion in federal taxes will be collected from residents in states not expanding Medicaid, and will be used to fund Medicaid expansion in other states.
Medicaid Expansion Is Needed To Protect Our Communities Particularly The Most Vulnerable
Expanding Medicaid has been proven to protect the health of our communities, our frontline workers, and our economy. And yet 12 states continue to refuse to expand Medicaid, even though their residents are already paying for it with their federal tax dollars. These states continue to deny residents affordable access to the care they deserve even in the face of considerable federal incentives and ample evidence that doing so saves money, saves lives, and helps keep rural hospitals open.
These 12 states failure to expand Medicaid has had catastrophic effects, preventing roughly 4 million people in those states from accessing life-saving health services. Residents of those 12 states also now carry a medical debt burden nearly 2 times that of states that expanded Medicaid in 2014. As communities become unable to pay their bills, the rural hospitals that serve them are at increasing risk of closing, leaving many without access to emergency rooms and basic healthcare services at times when they need them most.
Fortunately, these hospitals would be greatly aided through Medicaid expansion. Medicaid expansion has been proven to lower levels of uncompensated care and increase financial stability for rural hospitals as more of the population they serve will be insured, ensuring that hospitals will be paid for their services and will be better able to keep their doors open.
Recommended Reading: Ent In Lafayette La That Accept Medicaid
Michigan: Full Offset Required
Michigan expanded Medicaid under the Social Welfare Act, which included a provision that automatically sunsets the program whenever annual state savings are insufficient to cover the costs. As a result, Michigan closely tracks the fiscal impacts of expansion. In its most recent estimates, Michigans House Fiscal Agency estimated that it would generate sufficient savings to offset expected costs through at least 202728 . The estimated net savings generated by expansion are substantial, amounting to more than $160 million per year.19
Michigans official estimates likely understate the savings within traditional Medicaid. The House Fiscal Agency includes the elimination of its Adult Benefits Waiver, but it does not include any other potential savings within Medicaid as described above.
Michigans official estimates also do not account for increased revenues attributable to increased economic activity. Levy et al. argue that Michigan likely enjoys nearly $140 million per year in additional tax revenue because of expansion. While some of this revenue may be offset by the costs associated with providing services to a larger economy, the net effect is still large.
Summary of Fiscal Impacts of Medicaid Expansion in Michigan| $771.9 | 169% |
Data: All estimates for FY2021 from Koorstra except taxes on increased economic activity, which comes from Levy et al. .
What Is Medicaid Expansion
A provision in the Affordable Care Act called for the expansion of Medicaid eligibility in order to cover more low-income Americans. Under the expansion, Medicaid eligibility is extended to adults up to age 64 with incomes up to 138% of the federal poverty level .
Pre-ACA, Medicaid was generally never available to non-disabled adults under age 65 unless they had minor children. And even then, the income caps to qualify as a parent/caretaker were very low. By expanding Medicaid, the ACA created a viable pathway to coverage for millions of low-income adults.
You May Like: What Is Straight Medicaid In Florida
Apply For Medicaid Coverage Even If Your State Hasnt Expanded
Even if your state hasn’t expanded Medicaid and it looks like your income is below the level to qualify for financial help with a Marketplace plan, you should fill out a Marketplace application.
Each state has coverage options that could work for you particularly if you have children, are pregnant, or have a disability. And when you provide more detailed income information you may fall into the range to save.
Changes In The Uninsured By Income
Exhibit 2 and Table 4 show the reduction in the uninsured by income level.
Option 1 opens the ACA marketplace to people below the poverty level and reduces the number of uninsured below 138 percent of FPL by 2.9 million. There are small reductions in the uninsured above 138 percent of FPL because of reductions in premiums as the risk pool improves. Overall, the number of uninsured falls by 3.0 million.
Option 2 is like option 1 but with enhanced premium subsidies. It reduces the number of uninsured by 3.2 million among people with incomes below 138 percent of FPL in nonexpansion states. There are also sizable reductions in the number of uninsured at higher income levels. Overall, the number of uninsured falls by 4.6 million.
Option 3 has both enhanced premium and cost-sharing subsidies and reduces the number of uninsured below 138 percent of FPL by 3.3 million in nonexpansion states. Overall, the number of uninsured falls by 5.0 million, more than in option 2 because the cost-sharing subsidies are more generous. Both options 2 and 3 have dual objectives: filling the gap and improving subsidies.
Medicaid expansion reduces the number of uninsured below 138 percent of FPL by 4.1 million. This option increases coverage the most for low-income adults. There is a slight reduction in the uninsured above 138 percent of FPL. Overall, the number of uninsured people falls by 4.1 million.
Also Check: Does Medicaid Give You A Free Breast Pump
Weighing Costs And Benefits
Wisconsin, Alabama, Wyoming and South Dakota are also taking different approaches to considering broader Medicaid eligibility, although none is a sure bet for expansion.
Wisconsin Gov. Tony Evers, a Democrat, signed an executive order last week calling for a special session starting Tuesday in an uphill battle to expand Medicaid.
Were not just missing out on the opportunity to expand access to quality, affordable health care. We are also missing out on an additional $1 billion under the American Rescue Plan that is available to states like us that have not expanded, Evers said at a news conference, referring to the March law.
Evers said the savings would be invested to pay for economic development and increase providers pay.
Wisconsins hospitals, doctors, nursing homes, and behavioral health providers will see needed rate increases, Wisconsin Department of Health Services Secretary-designee Karen Timberlake said in a statement. Expanding Medicaid is the most effective way to protect the health of Wisconsin.
In Wyoming, state lawmakers had built momentum to pass an expansion bill earlier this year, but the House-passed bill died in a Senate committee vote. The state is expected to hold a special legislative session in July, when expansion may be back on the table.
South Dakota advocates hope to put expansion to a vote in 2022.
Still, Adams acknowledged, No one has expanded outside of ballot initiatives in a very long time.
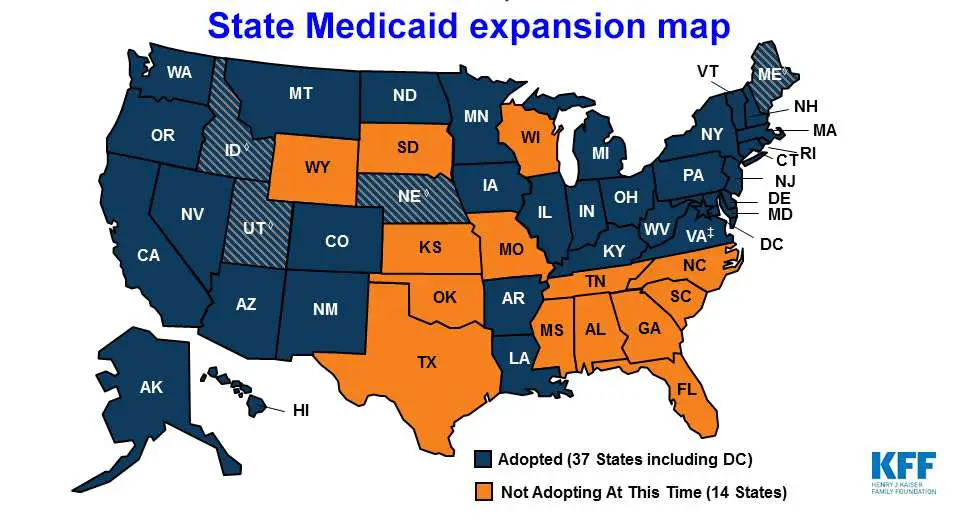
Status Of State Medicaid Expansion Decisions: Interactive Map
The Affordable Care Acts Medicaid expansion expanded Medicaid coverage to nearly all adults with incomes up to 138% of the Federal Poverty Level and provided states with an enhanced federal matching rate for their expansion populations.
To date, 39 states have adopted the Medicaid expansion and 12 states have not adopted the expansion. Current status for each state is based on KFF tracking and analysis of state expansion activity.
These data are available in a table format. The map may be downloaded as a PowerPoint slide.
Key States with Expansion Activity
This table tracks state actions related to adoption of the ACA Medicaid expansion. For non-expansion states, we include actions toward potential adoption. These include legislative actions , executive actions , and voter-led actions . We also mention some limited coverage expansions that would not qualify as full ACA Medicaid expansions and would not qualify for enhanced federal matching funds. For expansion states, we include summaries of when and how late-adopting states took up the expansion as well as notes on state attempts to place limits or requirements on the expansion population, especially through Section 1115 waivers.
Read Also: Dentists In Logan Utah That Accept Medicaid
The Rationale For Expanding Medicaid In 2021
1. Significant Economic Benefits. The cost of expansion is often cited as a reason for states rejecting it. Although the federal government pays for 90 percent of expansion costs, non-expansion states point to the burden of the 10 percent state share. However, a review of the direct and indirect impact of expansion on state budgets demonstrates that expansion pays for itself. We need only look at the experience of the 36 states that have already expanded Medicaid, where federal dollars from Medicaid expansion have offset state spending and fueled economic growth.
Non-expansion states are today spending state general funds to underwrite the program costs of health care services for their uninsured residents. With expansion, many, if not most, of these residents would become eligible for Medicaid, permitting states to underwrite all but 10 percent of the cost of these services with federal dollars, rather than with state-only funds. Expansion states have realized savings on mental health and substance use disorder services as well as inpatient hospital services for prisoners. Recently, several of these states have also begun to pursue Section 1115 waiver authority to use federal Medicaid funds for health care services and supports for prisoners prior to release and, more generally, to address underlying social factors, further reducing state spending, recidivism, and attendant financial and human costs.
The impact of Medicaid expansion on states budgets
Expansion Has Improved Coverage Access To Care Financial Security And Health Outcomes
While all states have seen uninsured rates fall since the ACAs major coverage provisions took effect in 2014, states that expanded Medicaid have made the greatest progress in increasing health coverage. In 2018 the uninsured rate among low-income, non-elderly adults in expansion states was 17 percent, compared to 32 percent in non-expansion states, a 52 percent versus a 24 percent decline from 2013. Prior to the onset of the pandemic and recession, over 12 million newly eligible people had health coverage through the Medicaid expansion. Another 4 million uninsured people would gain eligibility for Medicaid coverage if all states expanded.
Medicaid expansion is also a powerful anti-poverty tool: it reduces the medical debt of low-income Americans, improves access to credit, and significantly reduces housing evictions for renters.
Don’t Miss: How To Get Medicaid To Cover Tummy Tuck
Wyoming More Debate But No Movement
A Medicaid expansion bill passed in the Wyoming House last year, but subsequently failed in the states Senate. Last month, both the states House and the Senate tried to amend the 2023-2024 budget to expand Medicaid, given the substantial increase in federal funding from the American Rescue Plan. Despite a heartfelt plea by a state senator to expand health care coverage based on his own past experiences being uninsured while having stage-three cancer the proposed expansion failed. The Senate Rules Committee deemed it unconstitutional, as it was not an ordinary expenditure of the legislature.
Why Are There Some States That Havent Implemented Medicaid Expansion
The ACA called for Medicaid expansion nationwide. But in June 2012, the Supreme Court ruled that states could not be forced to expand their Medicaid programs, so it was left to each state to determine whether to participate or not.
When Medicaid expansion first took effect in 2014, it was only available in 26 states and DC. In the ensuing years, there has been a slow but steady increase in the number of states implementing Medicaid expansion. As of 2022, Medicaid had been expanded in 38 states and the District of Columbia . Oklahoma and Missouri are the most recent states to have expanded Medicaid, both doing so in 2021.
But Wisconsin is not counted among the Medicaid expansion states. It has implemented what essentially amounts to a partial expansion of Medicaid, and has no coverage gap because Medicaid is available to low-income adults with income below the poverty level.
But because Wisconsin has not fully expanded Medicaid as called for in the ACA , the state does not receive the enhanced federal Medicaid funding that it would receive if it fully expanded Medicaid.
You May Like: Medicaid Office In Corpus Christi
History Of Medicaid Expansion
As noted at the start of this summary, Medicaid was a cornerstone of ACA lawmakers efforts to expand access to healthcare. The idea was that everyone with household incomes up to 133% of the federal poverty level would be able to enroll in Medicaid .
People above that threshold would be eligible for premium tax credits in the exchanges to make their coverage affordable, as long as their income didnt exceed 400% of the poverty level. The idea was that people with income above 400% of the poverty level would be able to afford coverage without subsidies, but that has not proven to be the case. So the American Rescue Plan temporarily eliminated the income cap for subsidy eligibility, for 2021 and 2022. Congress could extend that for future years, but had not done so as of April 2022.
Because Medicaid expansion was expected to be a given in every state, the law was written so that premium subsidies in the exchange are not available to people with incomes below the poverty level. They were supposed to have access to Medicaid instead.
Expansion Push In Florida
An effort to bring a Medicaid expansion ballot measure to Florida for the 2020 election failed after the Legislature made changes to the ballot initiative process that drove up the cost of collecting signatures and raised the number of signatures needed for early stage review by the state Supreme Court.
The Legislatures interventionapparently a direct response to the Medicaid expansion measureunderscores the importance of the ballot initiative process as a tool to enact expansion in Florida, according to JoNel Newman, a professor at the University of Miami School of Law.
Whats unclear about the Legislatures action is whether the Medicaid ballot measure can be revived under at least some of the old rules or must begin again under the new rules, Newman said.
I do believe that theyre going to be able to restart this and get the funding to do it for the 2022 election, Newman said.
The Florida Hospital Association expressed support for Medicaid expansion in a statement that fell short of saying it would back a ballot measure.
We will always be on the front lines advocating for efforts that improve access to coverage, maintain appropriate funding for the cost of healthcare and services through state and federal safety net programs, and improve the quality of healthcare for everyone, Mary Mayhew, the associations president and CEO, said.
Don’t Miss: Does Medicaid Cover Breast Lift
