Medicaid Income Eligibility Chart State By State
The following is each of the states, listed alphabetically. Under your state of residence, you will find all of the relevant information regarding the Medicaid Income Eligibility Chart for each of three programs available: regular, in-home nursing care, and institutional nursing care.
Additionally, each of these programs will have additional information about the income limits for those who are single, married with both spouses applying, and married with only one spouse applying.
Does West Virginia Help With My Medicare Premiums
Many Medicare beneficiaries who struggle to afford the cost of Medicare coverage are eligible for help through a Medicare Savings Program . In West Virginia, these programs pay for Medicare Part B premiums, Medicare Part A and B cost-sharing, and in some cases Part A premiums.
- Qualified Medicare Beneficiary : The income limit is $1,063 a month if single and $1,437 a month if married. QMB pays for Part A and B cost sharing, Part B premiums, and if a beneficiary owes them it also pays their Part A premiums.
- Specified Low-Income Medicare Beneficiary : The income limit is from QMB levels up to $1,276 a month if single and $1,724 a month if married. SLMB pays for Part B premiums.
- Qualified Individuals : The income limit is from SLMB levels up to $1,436 a month if single and $1,940 a month if married. QI pays for Part B premiums.
- Qualified Disabled and Working Individuals : The income limit is $2,127 a month if living alone and $2,874 a month if living with one other person. QDWI pays for Part A premiums owed by certain disabled beneficiaries who have returned to work.
MSP asset limits: The asset limit for QMB, SLMB or QI is $7,860 if single and $11,800 if married. QDWI has an asset limit of $4,000 if living alone and $6,000 if living with others.
The Wv Medicaid Formulary And Prescription Drug Coverage
The West Virginia Medicaid program has a comprehensive prescription drug program. The drugs on the preferred drug list will act as your formulary. Youll also find information about prior authorization, meaning that there are certain drugs that you will need to have Medicaid approve before you retrieve your prescription at the Medicaid rate.
Recommended Reading: North Carolina Managed Medicaid Plans
How To Qualify For Medicaid
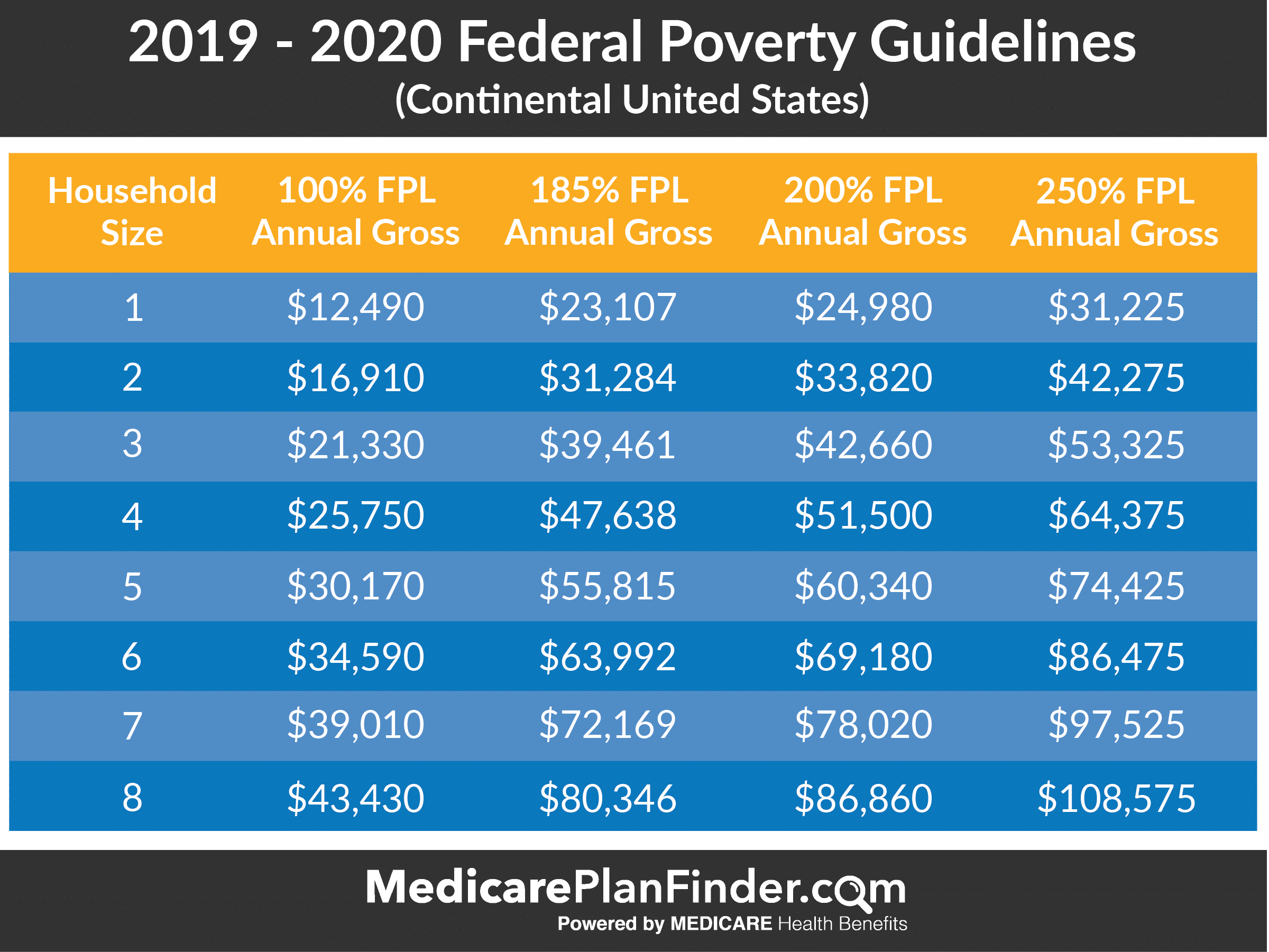
Almost every state has multiple Medicaid programs. But, as a good rule of thumb, if you make less than 100% to 200% of the federal poverty level and are pregnant, elderly, disabled, a parent/caretaker or a child, theres likely a program for you. And if you make less than 133% of the FPL**, theres possibly a program for you, depending on whether your state expanded Medicaid under Obamacare. In 2021, the federal poverty levels range from $12,880 to $44,660 .
In 2021, the federal poverty level in Alaska ranges from $ $16,090 to $55,850 . The federal poverty level in Hawaii ranges from $14,820 to $51,360 .
West Virginia Medicaid Benefits
Services include but are not limited to inpatient and outpatient hospital care, nursing home care, physician services, laboratory and x-rays, immunizations and other early and periodic screening, diagnostic, and treatment services for children, family planning, health centers and rural health clinics.
Also Check: Louisiana Medicaid Dental Coverage For Adults
Previous And Current Governor Support Medicaid Expansion
West Virginias former Governor, Earl Ray Tomblin, was instrumental in West Virginias acceptance of Medicaid expansion but was term-limited and could not seek re-election in 2016.
Governor Jim Justice took office in January 2017. He campaigned and was elected as a Democrat, but in the summer of 2017, during his first year in office, he switched to the Republican party. Justice reiterated his support for Medicaid expansion in the weeks leading up to his party switch, stating in late June 2017 that it would be beyond catastrophic if the people who had gained coverage under Medicaid expansion were to lose it. But Justice also vetoed a supplemental appropriation for the states Medicaid program in 2019, saying that the Medicaid program already had enough funding.
West Virginia Medicaid Income Limit Charts
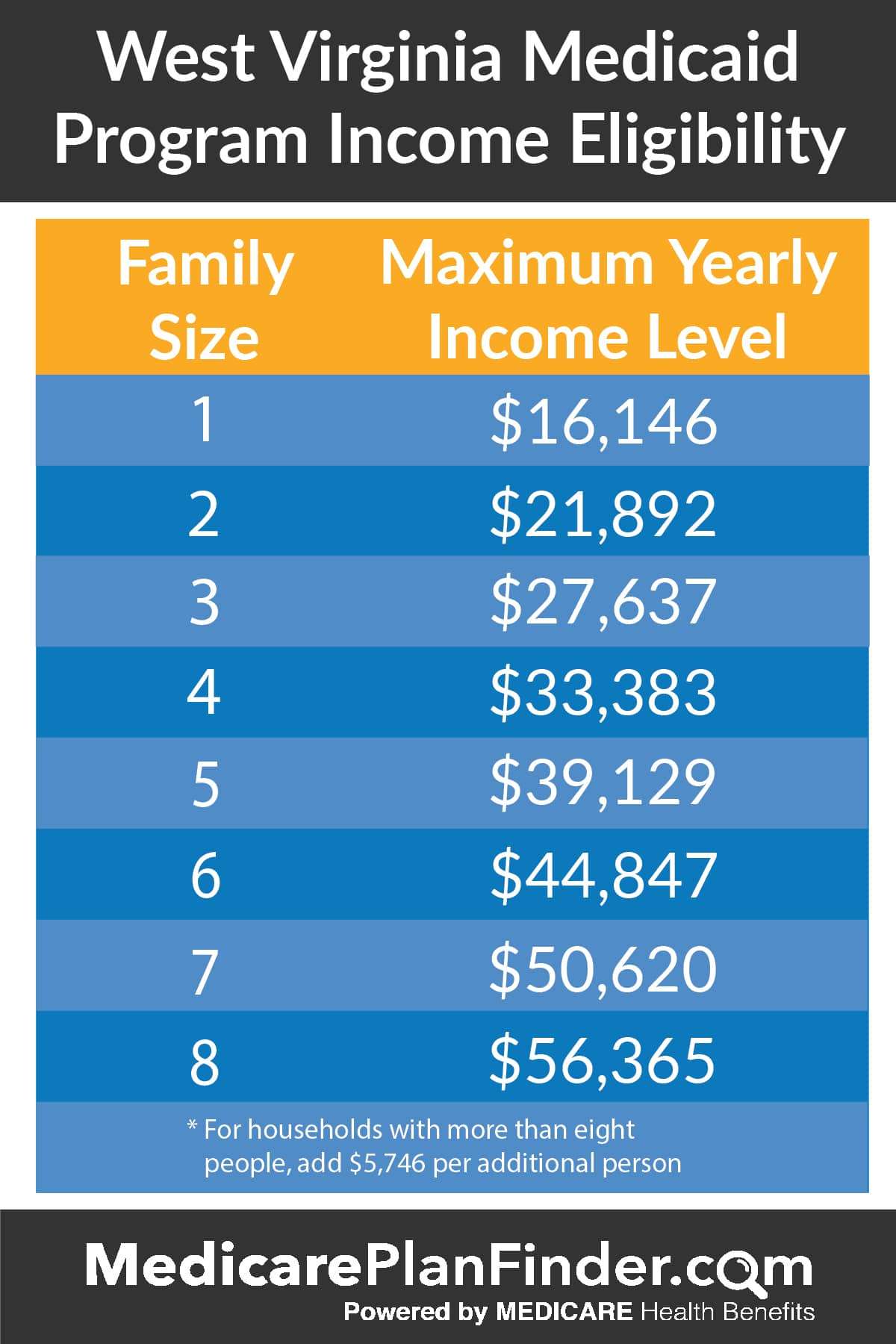
The West Virginia Medicaid eligibility income limit charts are divided by groups.
For example, the first chart is focused on income limits for children who qualify for Medicaid.
Similarly, the second chart below focuses on the Medicaid income limits for adults in West Virginia who qualify for Medicaid.
West Virginia Medicaid Income Limit for Children
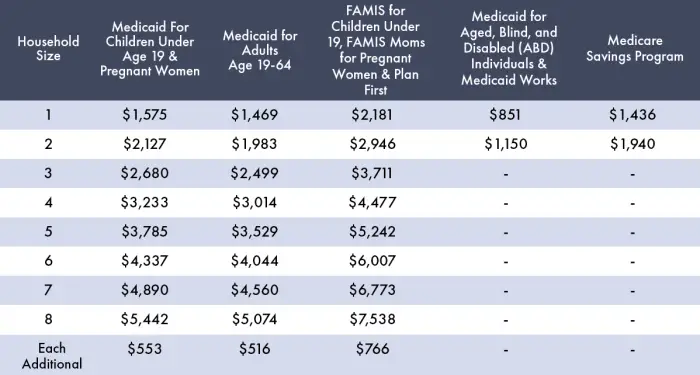
Below is the income limit for children by age category. Find the age category your child falls into and you will see the income limit by household size.
| West Virginia Medicaid Income Limit Children |
| Children Medicaid Ages 0-1 |
| $59,398 |
How to Read the West Virginia Medicaid Income Limits Charts Above
You cannot have an income higher than the Federal Poverty Level percentage described for your group to be eligible for Medicaid.
Similarly, when you identify the income group that applies to you, the income limit you see refers to the maximum level of income you can earn to qualify for benefits.
For example, if you are pregnant, to qualify for Medicaid, you cannot have an income higher than 185% of the Federal Poverty Level which for a family of two is $32,227 as shown in the chart above.
Don’t Miss: How To Qualify For Medicaid In Oregon
Find A $0 Premium Medicare Advantage Plan Today
For California residents, CA-Do Not Sell My Personal Info, .
MedicareAdvantage.com is a website owned and operated by TZ Insurance Solutions LLC. TZ Insurance Solutions LLC and TruBridge, Inc. represent Medicare Advantage Organizations and Prescription Drug Plans having Medicare contracts enrollment in any plan depends upon contract renewal.
The purpose of this communication is the solicitation of insurance. Callers will be directed to a licensed insurance agent with TZ Insurance Solutions LLC, TruBridge, Inc. and/or a third-party partner who can provide more information about Medicare Advantage Plans offered by one or several Medicare-contracted carrier. TZ Insurance Solutions LLC, TruBridge, Inc., and the licensed sales agents that may call you are not connected with or endorsed by the U.S. Government or the federal Medicare program.
Plan availability varies by region and state. For a complete list of available plans, please contact 1-800-MEDICARE , 24 hours a day/7 days a week or consult www.medicare.gov.
Medicare has neither reviewed nor endorsed this information.
What Are The Medicaid Income Limits For 2022
Finding out if you are eligible for Medicaid can be quite a headache. Since Medicaid is jointly funded by federal and state governments, there are different eligibility criteria for each state! One of the biggest factors for Medicaid eligibility are the income limits.
If you are trying to learn more about whether your income is within the Medicaid income limit for your state of residence, then you are reading the right article!
I will be explaining which sources of monthly incoming money are considered income, how each state decides their income limit, and providing an easy-to-use list of each states income limits for the year 2022.
Read on to learn more about Medicaid income limits and determine if your income would be considered within the limit set by your state of residence!
Recommended Reading: Best Way To Apply For Medicaid
What Counts As Income
The monthly financial amount that you receive from employment wages, benefits from Social Security, payments from a pension plan. Alimony, and payouts from stocks, IRAs, and other investment returns.
Mostly likely, if it is a form of money that you receive monthly, then it would count as income. However, if you are not sure about one of your sources of money, it is always better to err on the side of caution and check with your Medicaid program coordinators.
For applicants who are single or divorced, these monthly amounts are simply added up and the total number is the amount you can compare to the income eligibility limits in your state of residence. If it matches or is less than the limit for your state, you should be able to receive Medicaid health care benefits.
For applicants who are married, the protocol for evaluating income limit can differ depending on which state you reside in.
Most states have either one limit amount that each spouse can contribute to asymmetrically or a limit amount where each spouse can only make up one half of the total. Also, there are a few states where you are considered a single applicant, regardless of marital status.
There are also cases where you are married, but only one spouse is applying for Medicaid benefits. Again, the protocol will differ depending on the state of your residence. Most states will either treat the spouse applying as a single applicant or will consider their income limit as a married applicant.
What Is West Virginia Medicaid
West Virginia Medicaid is an entitlement program thats financed by the state and federal governments. The program is administered by the Department of Health and Human Resources and provides quality health care for low income residents. West Virginia uses private health insurance companies to provide services for some groups of Medicaid recipients. This is called Mountain Health Trust and is provided by Managed Care Organizations .
You May Like: What Benefits Do You Get With Medicaid
How Much Is The Federal Poverty Level
The federal poverty level in 2021 is equal to an income of $12,880 per year for an individual adult, plus $4,540 for each additional household member. Alaska and Hawaii have different benchmarks because of their differing costs of living.
|
Number of people in home |
48 states and Washington D.C. |
Alaska |
|---|
Medicaid Income Eligibility Chart For 2022
If you are looking into applying to receive Medicaid, whether it is for the first or hundredth time, your eligibility is decided based on your income. However the income eligibility can change from year to year, depending on the economy and what sort of care you require.
The Medicaid Income Eligibility chart is a tool for determining if your income falls under the limit, depending on if you need regular medicaid or Medicaid for long-term nursing care. All you need to do is find the listings for your state, line that up with the care you need, and then you will see the income limit for both single and married applicants.
If you are looking for an overview of the Medicaid Income Eligibility Chart regarding your situation, this is the article you need to read. Here, I will be providing all of the information for each state, type of care, and marital status for those who are trying to learn the facts. Read on to get more information about the benefits that are available to you!
You May Like: Ga Medicaid Income Limits 2020
West Virginia Medicaid Expansion Update
West Virginia opted to expand Medicaid under the Affordable Care Act starting on January 1, 2014.
Medicaid expansion significantly exceeded the 93,000 people that West Virginia had initially projected to enroll in by 2020.
Nearly 157,000 people enrolled under Medicaid expansion in West Virginia as of November 2019.
Additionally, the West Virginia CHIP program now covers maternity care as of July 2019
West Virginias uninsured rate dropped to 6.4% in 2018, thanks in large part to Medicaid expansion.
Maximum Out Of Pocket
Each calendar year quarter, West Virginia Medicaid members will have a maximum out-of-pocket payment. The OOP is the most the member will ever be required to pay in any given quarter, regardless of the number of health care services received.
The following table shows the maximum out of pocket costs based on poverty level:
| Federal Poverty Level |
Also Check: Medicaid And Other Health Insurance
West Virginia Has Accepted Federal Medicaid Expansion
- 581,329 Number of West Virginians covered by Medicaid/CHIP as of May 2021
- 226,785 Increase in the number of West Virginians covered by Medicaid/CHIP fall 2013 to May 2021
- 54% Reduction in the uninsured rate from 2010 to 2019
- 64% Increase in total Medicaid/CHIP enrollment in West Virginia since Medicaid expansion took effect
West Virginia Medicaid Asset Limits 2019
Individuals in West Virginia are allowed to keep $2,000 when they apply to Medicaid for long term care. If they are over this amount, they must spend down on care. It is important to note, that individuals are not allowed to give gifts of any amount for a period of 5 years prior to applying to Medicaid. If an individual’s assets are more than $2,000, they should learn about Medicaid Planning strategies. This asset limit only applies to assets that are considered countable assets. Some examples of countable assets include savings accounts, bank accounts, retirement accounts and a second home. If you have multiple assets and are looking to access Medicaid, it may make sense to speak with a Medicaid Planner or Elder Law attorney in West Virginia.
Couples that both require Medicaid for long term care in West Virginia are allowed to keep $3,000 in assets. If there is one spouse that requires care, and one that does not, the spouse that does not receive care is referred to as the Community Spouse. The Community spouse is allowed to keep 50% of their assets up to $123,600 in countable assets which is known as the Community Spouse Resource Allowance. The Community Spouse is allowed to keep 100% of their marital assets up to $24,720 .
You May Like: Does Medicaid Pay For Vyvanse
Contact A Knowledgeable Cabell County Lawyer For Assistance With Medicaid Planning
Herrenkohl Law Office assists West Virginia clients who are seeking to establish and maintain eligibility for Medicaid benefits. Please call 304-948-5860 or contact me online to make an appointment with an experienced attorney serving the Huntington area. My offices are in Barboursville and Beckley.
Who Can Get Medicaid In West Virginia
You should apply for Medicaid if your income is low and you match one of the descriptions below:
- You think you are pregnant
- The parent or caretaker of a child and/or teenager under the age of 19.
- You are a child or teenager age 18 or under.
- An adult age 65 or older.
- You are legally blind.
- Living with a disability or disabled.
- You are in need of nursing home care.
You May Like: Does Medicaid Cover Vasectomy Reversal
Where Can I Apply For Medicaid In West Virginia
West Virginias Medicaid program is administered by the Department of Health and Human Resources . Individuals can apply for Medicaid or an MSP using this website or by visiting a local DHHR office.
An in-person interview is always required when applying for long-term care benefits, and some states also require one for Medicaid ABD. However, interviews are not required for applicants who are only seeking an MSP.
Josh Schultz has a strong background in Medicare and the Affordable Care Act. He coordinated a Medicare ombudsman contract at the Medicare Rights Center in New York City, and represented clients in extensive Medicare claims and appeals. In addition to advocacy work, Josh helped implement federal and state health insurance exchanges at the technology firm hCentive.
What To Do If You Don’t Qualify For Medicaid
If you don’t qualify for Medicaid, you can possibly get subsidized health care through the Obamacare marketplaces during a special enrollment or open enrollment period. Americans who making more than 100% of the FPL qualify for a premium tax credit that can significantly lower the cost of a plan.
Federal open enrollment for 2022 health care plans runs until Jan. 15, 2022, though some state exchanges are open longer. Learn 2022 open enrollments dates by state. Healthcare.gov, the federal exchange, usually opens from November 1 to December 15 each year.
If you can’t find affordable health care on your marketplace during open enrollment, you have a few back-up options.
These include:
Short-term health insurance: Originally designed to prevent short-term health insurance gaps, these plans are cheaper, but much less comprehensive than traditional coverage. They don’t have to cover Obamacare’s 10 essential benefits or pre-existing conditions. Following changes by the Trump administration, short-term health plans can last from three months to potentially three years, though som estates have stricter limits.
Limited benefit plans: These plans cover a very small portion of the costs associated with certain “medical events,” like a doctor’s visit or ambulance ride. Both the number of events and dollar amounts covered are capped.
Prescription discount cards: While these cards won’t help you pay for inpatient or outpatient care, they do help you get medication at discounted rates.
Read Also: Spartanburg South Carolina Medicaid Office
Dedicated Attorney Takes Steps So Seniors Can Qualify For Nursing Home Care
Low-income individuals who believe they will require Medicaid to pay for serious expenses such as in-home care or residence in a nursing facility should take steps to maximize the likelihood of receiving benefits. Many people must shift ownership of some property in order to move below the $2,000 asset limit. This process is sometimes referred to as a spend down. My elder law firm conducts a thorough review of clients financial circumstances and advises on how gifts, trusts and other methods of asset reduction can help them qualify for benefits. I also show clients how using available funds for healthcare-related expenses might also serve their long-term interests.
How Many People Are On Medicaid
According to the Centers for Medicare & Medicaid Services, as of November 2020, here are the number of people enrolled in Medicaid and Chip in the entire United States:
- 78,521,263 individuals were enrolled in Medicaid and CHIP
- 72,204,587 individuals were enrolled in Medicaid
- 6,695,834 individuals were enrolled in CHIP
Don’t Miss: How To Apply For Medicaid In Houston
Mountain Health Trust And The West Virginia Health Bridge Alternative Benefit Plan
Mountain Health Trust and the West Virginia Health Bridge Alternative Benefit Plan are the managed care organizations for the West Virginia Medicaid program. Once accepted into the program, you will receive a packet in the mail which will tell you which MCO program you are in. The main differences between the two programs are a few coverage limits. For example, the Health Bridge program does not include nursing home coverage and has a limit of 24 chiropractic treatments per year. On the other hand, the Health Bridge program allows for 30 physical and occupational therapy visits per year instead of the traditional 20, and 100 home health visits instead of 60. Whichever program you qualify for, you will receive detailed information about your coverage limits in the mail upon your acceptance.
