Medicaid For Infants And Children
Through the Medicaid for Infants and Children program, medical needs for infants and children within a certain age range, and who meet income criteria, are met through the Medicaid program.
The income limits under MIC are higher than the MAF limits, and there are no reserve limits for this program. In addition, children who qualify for assistance under this program can receive Medicaid without meeting a deductible.
Medicaid Or Medicare Savings Programs
Medicare beneficiaries with limited income or very high medical costs may be eligible to receive assistance from the Medicaid program. There are also Medicare Savings Programs for other limited-income beneficiaries that may help pay for Medicare premiums, deductibles, and coinsurance. There are specified income and resources limits for both programs. Contact your local county Department of Social Services or SHIIP to apply for one of these programs.
Action Steps For States
- States must add counseling and pharmacotherapy benefits for pregnant women, which under Section 4107 of the Affordable Care Act are now mandatory benefits under Medicaid. This coverage is defined as diagnostic, therapy, counseling services, and pharmacotherapy for cessation of tobacco use by pregnant women. For more information, please see State Medicaid Director Letter #11-007 and contact your regional CMS office.
- Promote cessation benefits to pregnant women and all women of reproductive age.
- Make use of the many resources available to the public and to health care providers to help women quit smoking. See this Resource Guide for a list of highlighted resources.
For technical assistance and additional resources, contact .
Recommended Reading: How Long Does It Take To Get Accepted For Medicaid
Food And Nutrition Services
The Food and Nutrition Program is a federal food assistance program that provides low-income families a monthly supplemental allotment of benefits issues via Electronic Benefit Transfer cards . The Food stamp program is an entitlement program, so all eligible individual and households can receive assistance.
You may be eligible for Food and Nutrition Services if your total income falls below the appropriate gross income limits for your household size. Eligibility workers determine which income limit applies to your household.
Eligible individuals will receive Food and Nutrition benefits no later than thirty days from the date of application. Individuals with special circumstances will be given an opportunity to receive Food and Nutrition benefits within seven days of the application. View more information apply through the North Carolina Health and Human Servicess online program.
Family & Childrens Medicaid
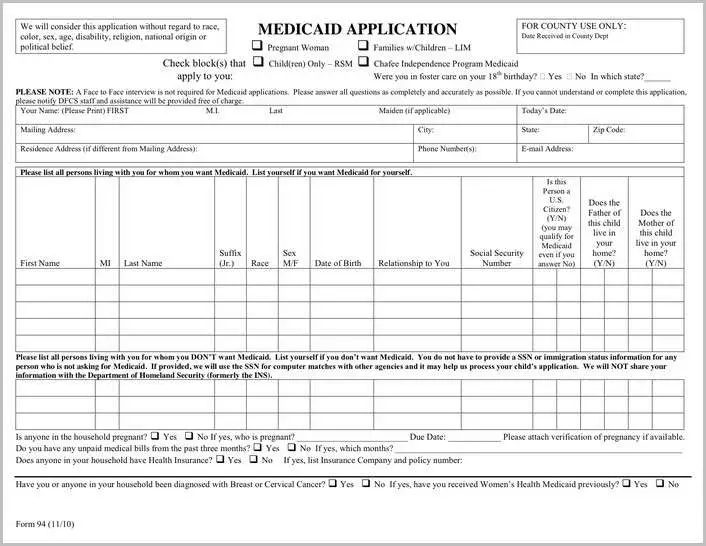

Is a health insurance program that serves low-income individuals, children, and parents. For information regarding the different types of Medicaid in North Carolina and to see if you are potentially eligible, visit the Division of Medical Assistance web site at
Also Check: Does Medicaid Cover Incontinence Pads
How To Enroll In Medicaid
To enroll in Medicaid, you must apply with the North Carolina Department of Health and Human Services.
North Carolina Medicaid programs may offer coverage for children, pregnant women, and families with children, the elderly, adults with disabilities, and children with disabilities.
You can apply for Medicaid services and enroll in a health plan in several ways:
How Much Can A Family Make To Qualify For Medicaid
In the 36 states that expanded coverage to low-income adults after the Affordable Care Act was passed, you can generally qualify for Medicaid if your monthly modified adjusted gross income is less than 138% of the federal poverty level. Thats $1,467 per month for an individual or $3,013 for a family of four.
You May Like: Can I Sell My House While On Medicaid
Learn About Requirements For Medicaid In North Carolina
What are the requirements for Medicaid in North Carolina? is a crucial question for applicants, because understanding how to qualify for Medicaid assistance is the first step toward receiving benefits. Whether or not an applicant meets Medicaid eligibility requirements in NC is determined by a local county Division of Social Services caseworker based on various established Medicaid benefits eligibility criteria involving age, health needs, income and resources. To find out who is eligible for Medicaid in North Carolina and to learn more about the states established qualifications, review the sections below.
What are the requirements for Medicaid in North Carolina?
North Carolina Medicaid eligibility is based on a number of factors. In order to meet the basic eligibility requirements for Medicaid assistance, you must satisfy one of the following criteria:
- You require long-term care.
- You are a low-income individual or family.
- You are younger than 21 years of age.
- You are blind or disabled .
- You are 65 years of age or older.
- You are/were recently pregnant
Medicaid benefits are available for pregnant women before or after the baby is delivered, and in cases where women experience pregnancy loss.
What are the income requirements for Medicaid in North Carolina?
- Stocks and bonds.
Medicaid For Pregnant Women
We can provide Medicaid to help with the cost of prenatal and postpartum care, up to 60 days following termination of pregnancy, either due to delivery or miscarriage. Must meet eligibility requirements.
Free viewers are required for some of the attached documents.They can be downloaded by clicking on the icons below.
You May Like: Dental Surgeon That Accepts Medicaid
What Benefits Does Pregnancy Medicaid Provide
Similar to other health care assistance programs, Medicaid does not pay monetary benefits directly to covered participants. Certain health care providers and health care facilities have a contract with Medicaid to treat those who are covered by Medicaid insurance.
When receiving Medicaid benefits, you should be given a list of medical providers who accept Medicaid or given a website to look for a provider in your area. As long as you receive care from a Medicaid provider, your health care costs will be submitted through Medicaid and will be covered. Pregnant women are covered for all care related to the pregnancy, delivery and any complications that may occur during pregnancy and up to 60 days postpartum.
Additionally, pregnant women also may qualify for care that was received for their pregnancy before they applied and received Medicaid. Some states call this Presumptive Eligibility and it was put in place so that all women would start necessary prenatal care as early in pregnancy as possible.
Talk with your local office to find out if you qualify for presumptive eligibility.
Pregnant women are usually given priority in determining Medicaid eligibility. Most offices try to qualify a pregnant woman within about 2-4 weeks. If you need medical treatment before then, talk with your local office about a temporary card.
Family & Childrens Medicaid Recertifications And Changes:
When information is required to complete your FCH Medicaid Recertification, documents must be returned by the due date on the request sent to you. Documents can be mailed in, dropped off using the DSS drop boxes located outside of the DSS building, or dropped off at the scanning area on the 1st floor of the DSS building.
to turn in information on the floor at the receptionist desk.)
For more information contact: 910-323-1540
You May Like: Are There Any Assisted Living Facilities That Accept Medicaid
Extra Help To Pay For Medicare Prescription Drug Costs
Extra Help is a Medicare program to help people with limited income and resources pay Medicare prescription drug costs. You may qualify for Extra Help if your yearly income and resources are below these limits in 2021:
- Single person yearly income less than $19,320 and less than $13,290 in other resources per year
You may qualify even if you have a higher income . Resources include money in a checking or savings account, stocks, bonds, mutual funds, and Individual RetirementAccounts . Resources dont include your home, car, household items, burial plot, up to $1,500 for burial expenses , or life insurance policies.
If you qualify for Extra Help and join a Medicare drug plan, youll:
- Get help paying your Medicare drug plans costs.
- Have no late enrollment penalty.
You automatically qualify and will receive Extra Help if you have Medicare and meet any of these conditions:
- You have full Medicaid coverage.
- You get help from your state Medicaid program paying your Part B premiums .
- You get Supplemental Security Income benefits.
Drug costs in 2021 for people who qualify for Extra Help will be no more than $3.70 for each generic drug and $9.20 for each brand-name drug.
Recommended Reading: Does Sc Medicaid Cover Breast Pumps
Where Do I Apply For Medicaid
Applications are taken daily Monday through Friday from 8:00 am to 5:00 pm and no appointment is needed. You may apply at The Department of Social Services.
741 North Highland Avenue Winston-Salem, NC 27101
The process of making an application for Medicaid can be complex and require a considerable amount of information.
If you have questions, please call 703-3800. We are here to answer your questions!
Recommended Reading: How To Become Medicaid Certified
Personal Needs Allowance In North Carolina
If you receive Medicaid and live in a nursing home, you will be expected to spend almost all of your income on your care. North Carolina allows nursing home residents receiving Medicaid to keep just $30/month as a personal needs allowance.
Read on to find out about when Medicaid will pay for assisted living or home health care in North Carolina.
Self-help services may not be permitted in all states. The information provided on this site is not legal advice, does not constitute a lawyer referral service, and no attorney-client or confidential relationship is or will be formed by use of the site. The attorney listings on this site are paid attorney advertising. In some states, the information on this website may be considered a lawyer referral service. Please reference the Terms of Use and the Supplemental Terms for specific information related to your state. Your use of this website constitutes acceptance of the Terms of Use, Supplemental Terms, Privacy Policy and Cookie Policy. Do Not Sell My Personal Information
If You Currently Have Marketplace Coverage
- If you want to keep your current Marketplace coverage, dont report your pregnancy to the Marketplace. When filling out your application for Marketplace coverage, select the Learn more link when we ask if youre pregnant to read tips to help you best answer this question.
- If you report your pregnancy, you may be found eligible for free or low-cost coverage through Medicaid or the Childrens Health Insurance Program . If you are found eligible for Medicaid or CHIP, your information will be sent to the state agency, and you will not be given the option to keep your Marketplace plan.
- If you keep your Marketplace coverage, be sure to update the application after you give birth to add the baby to the plan or enroll them in coverage through Medicaid or CHIP, if they qualify.
Recommended Reading: Eye Doctors In Las Vegas That Accept Medicaid
Don’t Miss: Does Medicaid Pay For Dental Work
Who Is Eligible For Medicaid
The general guidelines for eligibility for Medicaid are set by the Federal government however, each state sets up their own specific requirements for eligibility and these can differ from state to state.
All States are required to include certain individuals or groups of people in their Medicaid plan.
The state eligibility groups are:
- Categorically needy
- Medically needy
- Special groups
In the categorically needy group, this will cover pregnant women whose income level is at or below 133% of the Federal Poverty level.
In the medically needy group, this will cover a pregnant woman who makes too much money to qualify in the categorically needy group. This means that women, who may have been denied Medicaid before, may be able to qualify now.
Option 1 Apply Online
You can apply online through the North Carolina ePASS Portal as shown in the image below.
If you have an account, you can log in or create your North Carolina ePASS Account. to be taken to the website.
The video below, from the North Carolina Department of Health and Human Services does a great job of walking you through how to apply for Medicaid online.
We highly encourage you to watch it if you are planning to apply for NC Medicaid online.
Donât Miss: Can I Get Dental Insurance With Medicaid
Recommended Reading: Does Medicaid Cover Cortisone Shots
Adult Medicaid And Long Term Care Medicaid
ADULT MEDICAID AND LONG TERM CARE MEDICAID PROGRAMS
Adult Medicaid is health insurance for low-income individuals, seniors, and people with disabilities. Eligibility is based on your familys monthly income and resources that are owned. To receive Medicaid for disability or blindness, you must meet Social Securitys definition of disability or blindness. Adult Medicaid covers individuals living at home in a Private Living Arrangement or individuals in Long Term Care living arrangements. The Medicare Savings Program is a limited assistance Adult Medicaid program for individuals enrolled in Medicare Part A and/or Part B. The Medicare Savings Program can help pay for Medicare premiums, coinsurance, and deductibles.
APPLYING FOR ADULT MEDICAID & LONG TERM CARE PROGRAMS:
- Apply online at or print here to mail in the application.
- You may also request that an application be mailed to you by calling 919-580-4034.
- Applications can be dropped off in the Social Services mail drop box located in the parking lot of Wayne County Social Services at 301 N Herman St, Goldsboro, NC 27530.
- Apply in person at the Wayne County Dept. of Social Services located on the 2nd floor at 301 N. Herman St, Goldsboro NC. Applications are taken between 8:00 am to 5:00 pm, Monday Friday .
ADULT MEDICAID & LTC RECERTIFICATIONS AND CHANGES:
Report changes by calling 919-731-1022
RELATED LINKS:
You May Like: How Can I Check The Status Of My Medicaid
What Happens To My Medicaid If I Move
North Carolina Medicaid recipients must report changes that can influence their eligibility status, including relocating to a new address.
If you move to a new residence within North Carolina, you can update your address with the North Carolina Division of Social Services in the following ways:
- By phone at 1 662-7030.
- In person at a local Division of Social Services office. Find contact information for local DSS offices in North Carolina here.
Note: Medicaid benefits do not transfer. If you move to a new state, you must reapply for Medicaid in your new location. If you have further questions about moving with Medicaid, visit the national Medicaid Contact Us here.
Donât Miss: Pros And Cons Of Expanding Medicaid
Recommended Reading: Dentist In Southaven Ms That Take Medicaid
Medicaid And Health Choice Programs
Medicaid is a federal program designed to assist families and children with the cost of health care. Health Choice is North Carolinas free or low-cost health insurance plan for children ages 6-18 whose families cannot pay for private insurance and who do not qualify for Medicaid.
Medicaid also offers assistance to the uninsured with breast and cervical cancer. Other programs offered are Medicaid for pregnant women, family planning Medicaid, and emergency Medicaid for undocumented aliens.
Also Check: Louisiana Medicaid Dental Coverage For Adults
North Carolina Medicaid Expansion Update
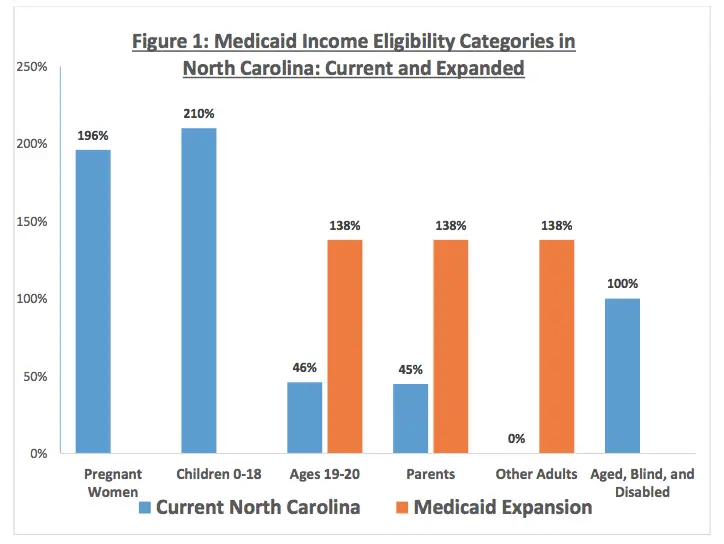
North Carolina is one of 12 states that has not yet expanded Medicaid under the Affordable Care Act .
If Medicaid is expanded in North Carolina, it is estimated that 624,000 residents would become newly eligible for coverage.
Governor Cooper has long pushed for Medicaid expansion, but GOP lawmakers oppose expansion.
North Carolinas Medicaid program is transitioning to a managed care model in 2021 after several delays.
You May Like: Does Medicaid Pay For Tubal Ligation Reversal
Information You May Need When Applying For Services
To assist you with the Medicaid and Food and Nutrition Services applications, listed below are verifications you may be asked to provide in order to determine your eligibility. If you do not have any of this information you may still complete an application and interview for services. Individuals can apply at or in person at the Social Service building, no appointment is necessary.
To submit required verification electronically, email them to:
Name/Identity:
- Mail received at your address
Earned Income:
You May Like: What Is The Income Limit For Arkansas Medicaid
Who Can Get Medicaid In North Carolina
You should apply for Medicaid if your income is low and you match one of the descriptions below:
- You think you are pregnant
- The parent or caretaker of a child and/or teenager under the age of 19.
- You are a child or teenager age 18 or under.
- An adult age 65 or older.
- You are legally blind.
- Living with a disability or disabled.
- You are in need of nursing home care.
Don’t Miss: Eye Doctors In Lynchburg Va That Accept Medicaid
Medicaid Coverage And State
Private health insurance covers the cost of substance-use disorder treatment and services to varying degrees. Each insurer has its own policy, and insured individuals will need to refer to the policy of their respective insurance companies to determine the extent of services that are covered. Many women needing treatment, including pregnant women, may have once had private insurance but have lost that insurance. This section presents information for women who are uninsured, women who may qualify for Medicaid insurance, and women who are currently insured with Medicaid.
Medicaid Services for Women and Children
- Medicaid for Infants and Children
Medicaid for Infants and Children provides medical coverage for children younger than 19 years old. The income limits are determined by the family size and the age of the child or children applying for benefits. There is no limit on resources.
- Medicaid for Families with Dependent Children
Medicaid for Families with Dependent Children provides medical coverage for parent or other caretaker/relative with a child 18 years or younger in the household and for children under age 21. A pregnant woman may also qualify.
The family cannot have more than $3,000 in assets such as savings in the bank.
If the family income is above the cut-off and the child and/or family has high medical bills, the family might still qualify for Medicaid .
- Medicaid for Pregnant Women
Medicaid for Pregnant Women covers only services related to pregnancy:
