A More Active Enrollment
When it was looking at ways to revamp the system, the department took the position of wanting participants to be more actively involved in choosing a plan.
“Our goal was to try to help everyone make a choice,” said Corcoran. “We want to try to educate and provide information about available services, so that we could improve the overall health literacy of everyone on the program, rather than sort of default.”
Automatic enrollment into one’s original plan would be taken away. Almost all applicants would be required to actively select a plan, and if they didn’t, then they would go through the quality-based assessment process, which would also get an updated algorithm.
The underlying idea was that the more people know about their own plan, the better the health outcomes.
“There were people on the program who didn’t even realize some of those simple things about transportation being available to your doctor, or that your management people can help coordinate your care,” the director said.
But some have worried such changes would pose barriers for the Medicaid population, who tend to be difficult to reach and in disadvantaged communities. Therefore, they’re less likely to successfully navigate the additional red tape and actively enroll.
But the department acknowledged Crawley’s arguments and is reevaluating.
Leaderships Opposition To The Aca
In June 2013, the Ohio Department of Insurance issued a press release announcing that 14 insurers filed plans to offer more than 200 options for individual insurance, and seven insurers would offer 84 options for small businesses . Then-Lt. Gov. Mary Taylor, who also directed the states insurance department until 2017, stated in the press release that consumers will have fewer choices and pay much higher premiums for their health insurance starting in 2014.
Both opponents and supporters of the Affordable Care Act jumped on the press release. Opponents claimed Ohio was the latest example of rate shock. Supporters dismissed the announcement for making apples-to-oranges comparisons and pointed out that both Kasich and Taylor had been outspoken about their opposition to the ACA.
Laws were enacted in Ohio to make it more difficult for navigators to be certified, which means that the state has fewer people available to assist applicants, and there was a delay in getting them started as navigators after the exchange opened in October 2013.
Medicaid Expansion In The Buckeye State
Former Ohio Governor John Kasich was not an ACA proponent, but he actively pushed for Medicaid expansion in Ohio, which was approved in late October 2013. Eligible residents were able to begin enrolling in expanded Medicaid on December 9, 2013. Net enrollment in Ohios Medicaid program has grown by 43% since the fall of 2013.
However, opponents of Medicaid expansion brought a lawsuit against the Ohio Department of Medicaid and the states Controlling Board because the General Assembly was bypassed in the decision to expand Medicaid. The plaintiffs hoped to block the state from expanding Medicaid, but on December 20th, 2013 the Ohio Supreme Court sided with Governor Kasich and kept Ohio Medicaid expansion on track. The Courts ruling came less than two weeks before expanded Medicaid took effect.
You May Like: Pregnancy Medicaid Texas Phone Number
Exchange History In Ohio
In November 2012, Governor Kasich formally announced that Ohio would not implement a state-run health insurance exchange. In the same letter, Kasich indicated that Ohio would retain control of plan management activities and determining eligibility for the states Medicaid and Childrens Health Insurance Plan . Ohio is one of five states that use the marketplace plan management model.
Ohio residents can compare plans, determine subsidy eligibility and enroll in coverage at Healthcare.gov.
What Rural Ohio Stands To Lose If Proposed Change To Medicaid Open Enrollment Moves Forward

People from Columbus and Ohios other big cities may not fully understand the importance of Medicaid for rural and less-populated counties across Ohio. Medicaid, which is the second largest health insurance provider in Ohio, covers just over a quarter of our states entire population. In many rural counties, particularly in southern and southeast Ohio, the percentage of people covered by Medicaid is significantly higher than the state average, and higher or on par with Cuyahoga, Franklin and Hamilton Counties which are home to Cleveland, Columbus and Cincinnati.
Medicaid assists in covering rural health clinics and federal qualified health centers, prescription drugs, nursing home and home health care, and drug addiction treatment among many other services vital to people across our state but particularly in more rural communities.
Since Ohio expanded Medicaid in 2013, our state has seen a nearly 50% reduction in its uninsured rate. A major reason for Medicaids success in providing quality health insurance to such a significant percentage of our population is the open enrollment process. Through open enrollment, Medicaid members can change their plan if they want to or keep it if they like it. Its a relatively straightforward, accessible process that limits confusion and works well on the large scale required to manage such a robust and complex system.
Recommended Reading: Medicaid Eligibility For Nursing Home Care
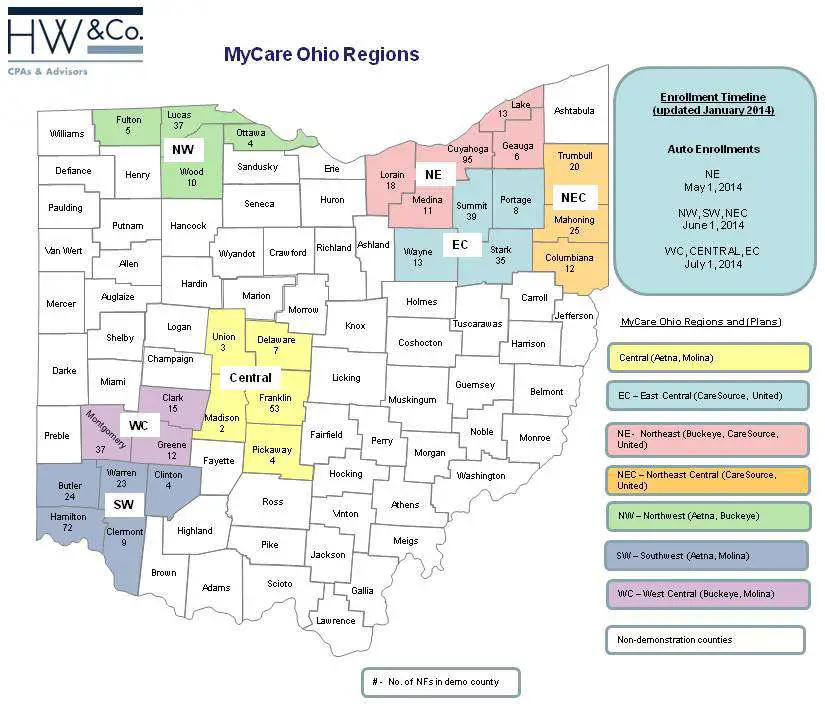
Learn More About Mycare Ohio
Read the MyCare Ohio: What You Need to Know fact sheet to learn more about how this new managed care program might work for you or watch this MyCare Ohio Overview presentation.
For more specific information and frequently asked questions, click the link to the fact sheet that best describes your current care arrangement.
- Live in a Nursing Facility
Is My Virtual Visit Covered By Insurance
Cleveland Clinic provides virtual visits for your convenience and health. Virtual visits are not covered by all insurance plans. In order to fully understand your benefits and potential cost, contact your insurance company and ask if virtual visits are included in your plan and if not, what it may cost you.
You May Like: How Can I Check If I Still Have Medicaid
Initially 20 Counties Had No Plans Filed For 2018 But Other Insurers Agreed To Cover Them
When Anthem announced that they would exit the exchange at the end of 2017, there were 20 rural counties which had more than 11,000 exchange enrollees in 2017 that did not have any insurers slated to offer exchange coverage. But on July 31, 2017, Ohios Department of Insurance announced that five existing exchange insurers had agreed to offer coverage in 19 of the 20 bare counties. Buckeye Health Plan, CareSource, Medical Mutual, Molina, and Paramount Health Care agreed to offer coverage in those counties.
Only Paulding County, in northwest Ohio, was still without any insurers slated to offer coverage at that point. State regulators continued to work with insurers to devise a solution for Paulding County, and On August 24, the Ohio Department of Insurance announced that CareSource had agreed to offer coverage in Paulding County. CareSource offered plans in 51 Ohio counties in 2017, and their 2018 rate filing indicated that they would expand to offer coverage in 59 counties in 2017, although the recent additional expansion further increases that number CareSource agreed in late July to cover eight of the bare counties, and added a ninth with Paulding.
This happened in other states too, and insurers stepped in to fill the bare spots. Previously bare counties in Tennessee, Washington, Kansas, Missouri, Indiana, Wisconsin, and Nevada were all ultimately filled, and all areas of the country had plans available in the exchange in 2018.
Choosing Your Managed Care Organization
Most people are automatically selected for Medicaid managed care coverage. Shortly after you enroll in Medicaid, you will get a letter asking you to choose a Medicaid MCO. Visit the websites below for each to learn more and find one that is right for you. If you dont choose a plan, we will choose one for you. You can change plans up to 90 days from your date of initial enrollment, or during our annual open enrollment period.
A helpful way to enroll in managed care is online through the Medicaid MCO Member Service Website. With help from the MCO Member Service, you can compare plans additional benefits and view plans provider networks. You may want to consider: what services you might need, which health plan is accepted by the doctors you use, which plan was found to meet the highest quality for your health care needs, and which extra benefits are most beneficial to you.
Once you are enrolled with an MCO, you will get a new card in the mail. MCOs send one permanent card when you enroll. Keep this card for as long as you are on the plan. If you need to replace your managed care ID card, please contact your MCO, or use their online member portal. The plan will also send you information on your doctors, health services, and the scope of coverage from your plan.
Recommended Reading: Does Medicaid Pay For Dentures In Nc
Member Advisory Council And Connected Advisors
UnitedHealthcare Care Managers for Member’s Unique Needs
Every UnitedHealthcare MyCare Ohio member receives a personal representative. These Care Managers are licensed professionals providing education and coordination of UnitedHealthcare Connected® for MyCare Ohio benefits, tailored for each member’s unique needs.
to watch a video on how these Care Managers are helping current members.
We recently mailed you a letter that included some information on benefit changes. Some of the information did not pertain to members that only have their Medicaid covered benefits through our plan. Please disregard that letter. The letter also had an incorrect number for the Ohio Medicaid Hotline. The correct number for the Hotline is 1-800-324-8680. We are sorry for any confusion this may have caused you. Please view the Member Clarification Letter for additional information.
Use the documents below to learn more about each important health topic.
-
PDF 180.50KB – Last Updated: 11/12/2020
UnitedHealthcare Member Advisory Council and “Connected Advisors”
UnitedHealthcare Member Advisory Council and “Connected Advisors” is an advisory council to ensure that UnitedHealthcare actively engages consumers, families, advocacy groups, and other key stakeholders as partners in the program design and delivery system.
Who is involved?
They will advise and guide the UnitedHealthcare Community Plan of Ohio on:
How is it organized?
What will they do?
-
PDF 26.62KB – Last Updated: 11/12/2020
Where Do I Get Started
We know that it can be stressful to navigate the insurance coverage process, but we strive to make it as smooth as possible.
We accept a variety of plans from insurance companies at all of our locations. To verify if your insurance plan is accepted for services across our health system, please review our list of accepted insurance companies below.
If your insurance company is accepted by Cleveland Clinic: Please contact your insurance company to confirm what care is covered by your plan as well as information on copayments, deductibles and coinsurance amounts. See what your out-of-pocket expenses will be using our cost estimator.
If your insurance company is not accepted by Cleveland Clinic: This means your insurance plan is considered out-of-network which can lead to greater out-of-pocket expenses for your care. Please contact your insurance company for more information about what your financial responsibility may be if you choose to receive care at Cleveland Clinic. Find more information about Cleveland Clinics out-of-network insurance process.
You May Like: Tens Unit Covered By Medicaid
Unitedhealthcare Connected For Mycare Ohio
UnitedHealthcare Connected® for MyCare Ohio is a health plan that contracts with both Medicare and Ohio Medicaid to provide benefits of both programs to enrollees. If you have any problem reading or understanding this or any other UnitedHealthcare Connected® for MyCare Ohio information, please contact our Member Services at from 7 a.m. to 8 p.m. Monday through Friday for help at no cost to you.
Si tiene problemas para leer o comprender esta o cualquier otra documentación de UnitedHealthcare Connected® de MyCare Ohio , comuníquese con nuestro Departamento de Servicio al Cliente para obtener información adicional sin costo para usted al de lunes a viernes de 7 a.m. a 8 p.m. .
How To Appeal An Application Denial
Medicaid applications will be denied if applicants do not meet the eligibility requirements. Also, beneficiaries can have their benefits terminated or reduced if their eligibility status changes while they are enrolled.
If your Medicaid application is denied or your benefits amount is reduced, you have the right to file an appeal. If you would like to submit an appeal request, review your determination letter for step by step instructions on the appeal process. Alternatively, you can contact the Ohio Medicaid Consumer Hotline at 1 324-8680 for assistance.
You May Like: Does Medicaid Pay For Retainers
Big Step Forward For Ohio Medicaid But More To Come
On April 9, Ohio Department of Medicaid Director Maureen Corcoran made a long-awaited announcement revealing the names of the Medicaid managed-care insurance companies that would get to share in a 20 billion dollar, five-year contract to provide health care services for 3 million Ohioans.
Director Corcoran said repeatedly that she wanted to focus on people and not just the business of managed care.
The announcement had been delayed likely because of a lawsuit that Ohio Attorney General David Yost had filed against Centene accusing the company of a conspiracy to wrongfully and unlawfully obtain tens of millions of dollars in Medicaid payments. Its not clear how this situation will resolve itself, but it seems likely that Centene has a strong incentive to settle this case.
The announcement of the winning plans was the culmination of a process that began a little more than two years ago. In fact, Governor Mike DeWine signaled early that he wanted to re-procure Ohios Medicaid managed-care contracts. Director Corcoran said repeatedly that she wanted to focus on people and not just the business of managed care.
Insurance Companies That Responded To Ohio Medicaid Request For Proposals
| Score | |
|---|---|
| UnitedHealthcare Community Plan of Ohio, Inc. | 1 |
| Humana Health Plan of Ohio, Inc. | 2 |
| Molina Healthcare of Ohio, Inc. | 3 |
| Anthem Blue Cross and Blue Shield | 5 |
| Buckeye Community Health Plan | Defer |
Any final decision related to Buckeye Community Health Plan is subject to additional consideration by Medicaid under sections 5.13 and 5.14 of the RFA, based on the claims by the Ohio Attorney General, Medicaid, and the State of Ohio in litigation recently filed in the Franklin County Court of Common Pleas and other factors. At this time, Medicaid is neither issuing nor denying an award to Buckeye Community Health Plan.
You May Like: Can You Get Plan B For Free With Medicaid
See What Unitedhealthcare Has To Offer
Its your health. Its your choice.
Everyone deserves affordable health care, including you.
Working adults, people with disabilities, pregnant women, and children who qualify for Medicaid should check out UnitedHealthcare Community Plan.
We have the Medicaid benefits and extras that can make a real difference in your life. All at no cost to you.
Find a doctor you trust in our network
- Dental coverage
- Transportation to and from doctor appointments
- 24/7 NurseLine to answer your health questions
- No copays
Sometimes, you might need a little extra help. Get extras not covered by Medicaid.
- Earn rewards for keeping you and your baby healthy
- Earn gift cards for getting preventive services
- Doctor Chat chat with a doctor wherever you are
- Wellhop for Mom & Baby
We also offer resources to help you make the most of your plan, including:
- Member Services
Helping you live a healthier life. We are here for you, OHIO. Remember to choose UnitedHealthcare Community Plan.
To learn more about UnitedHealthcare Senior Care Options, visit UHCCommunityPlan dot com forward slash OH.
Looking for the federal governments Medicaid website? Look here at Medicaid.gov.
Unitedhealthcare Dual Complete Plans
Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
Also Check: Can Medicaid Be Transferred To Another State
Ohio Health Insurance Exchange Links
HealthCare.gov800-318-2596
State Exchange Profile: Ohio The Henry J. Kaiser Family Foundation overview of Ohios progress toward creating a state health insurance exchange.
About our health insurance quote forms and phone lines
We do not sell insurance products, but this form will connect you with partners of healthinsurance.org who do sell insurance products. You may submit your information through this form, or callto speak directly with licensed enrollers who will provide advice specific to your situation. Read aboutyour data and privacy.
The mission of healthinsurance.org and its editorial team is to provide information and resources that help American consumers make informed choices about buying and keeping health coverage. We are nationally recognized experts on the Affordable Care Act and state health insurance exchanges/marketplaces.Learn more about us.
If you have questions or comments on this service, pleasecontact us.
How Medicaid Enrollment Is Currently Done
As it’s done now, a Medicaid participant already enrolled in a plan gets automatically assigned back to the same plan.
If a person is newly eligible, the applicant is first checked if he can be put on a family member’s same plan, as the case is for newborns. If not, the department looks at the doctors that an applicant has used to see which plan most of the providers are associated with. Any remaining people are then put through a “quality-based assessment assignments process” based on plan performance in areas such as payment and quality measures.
The member gets notified that he or she has been assigned to a plan, and within 90 days, the member can voluntarily choose to make a different selection instead.
Overall, it’s a mostly hands-off process for the individual.
Recommended Reading: Assisted Living In New Jersey That Accepts Medicaid
