Asset Limits And Requirements
To qualify for Medicaid in Florida, a person must not have enough resources or income to pay for their care costs. Medicaid evaluates a persons ability to pay by looking at the monetary value of their resources. If an applicant makes too much income per month, or their assets are too valuable according to Medicaids guidelines, they must participate in a spend-down period with Medicaid or pay for their care privately.
Medicaid considers assets and income separately when they evaluate a persons financial need. Homes, vehicles, spending accounts, and burial plots are among the many types of assets Medicaid evaluates. Assets are divided into countable assets, which Medicaid considers towards a persons asset limit, and exempt assets, which are not considered.
Its common for Medicaid applicants to posses exempt assets, which do not count toward their asset limits if they meet certain criteria. For example, a persons home is considered exempt by Medicaid, provided the applicant or their spouse uses it as a primary residence and its value does not exceed Floridas Home Equity Limit.
The Home Equity Limit determines how much a home can be worth before Medicaid will count it toward a persons asset limits. In Florida, the Home Equity Limit is $840,000 if a home is valued beyond this limit, Medicaid has the right to deny an applicant from receiving benefits until theyve liquidated the asset and put it toward their care costs.
Florida Medicaid Income Limits Summary
We hope this post on Florida Medicaid Income Limits was helpful to you.
If you have any questions about Medicaid in the state of Florida, you can ask us in the comments section below.
Help us spread the word! If you found this post on Florida Medicaid Income Limits helpful, help us spread the word by sharing it using the Share this button below.
Be sure to check out our other articles about Medicaid.
What Our Clients Say About Our Services
Ive had the pleasure to work with Mr. Daily for over 20 years, and he has always found the time to counsel and explain the best course of action.
JG | Tax Law Assistance And Counsel
Mr. Daily helped me get out of a tax situation that could have forced the dissolution of my business and ruined my credit.
Anonymous | Representation And Defense In Front Of The IRS
Fred assisted us through a multi year audit with ease and professionalism. His guidance was excellent and it was obvious he knew exactly how to handle the IRS
Richard | Multiyear Tax Audit Defense
Don’t Miss: Will Medicaid Pay For Portable Oxygen Concentrator
Florida Medicaid Eligibility Guidelines
To qualify for Medicaid in Florida, an individual must meet the eligibility requirements of the program.
There are several Medicaid programs that people in Florida can be eligible for. Each program has its own income and asset requirements.
However, all applicants must meet the general requirements below in order to qualify for Florida Medicaid.
Are There Options If I Make More Than The Limit
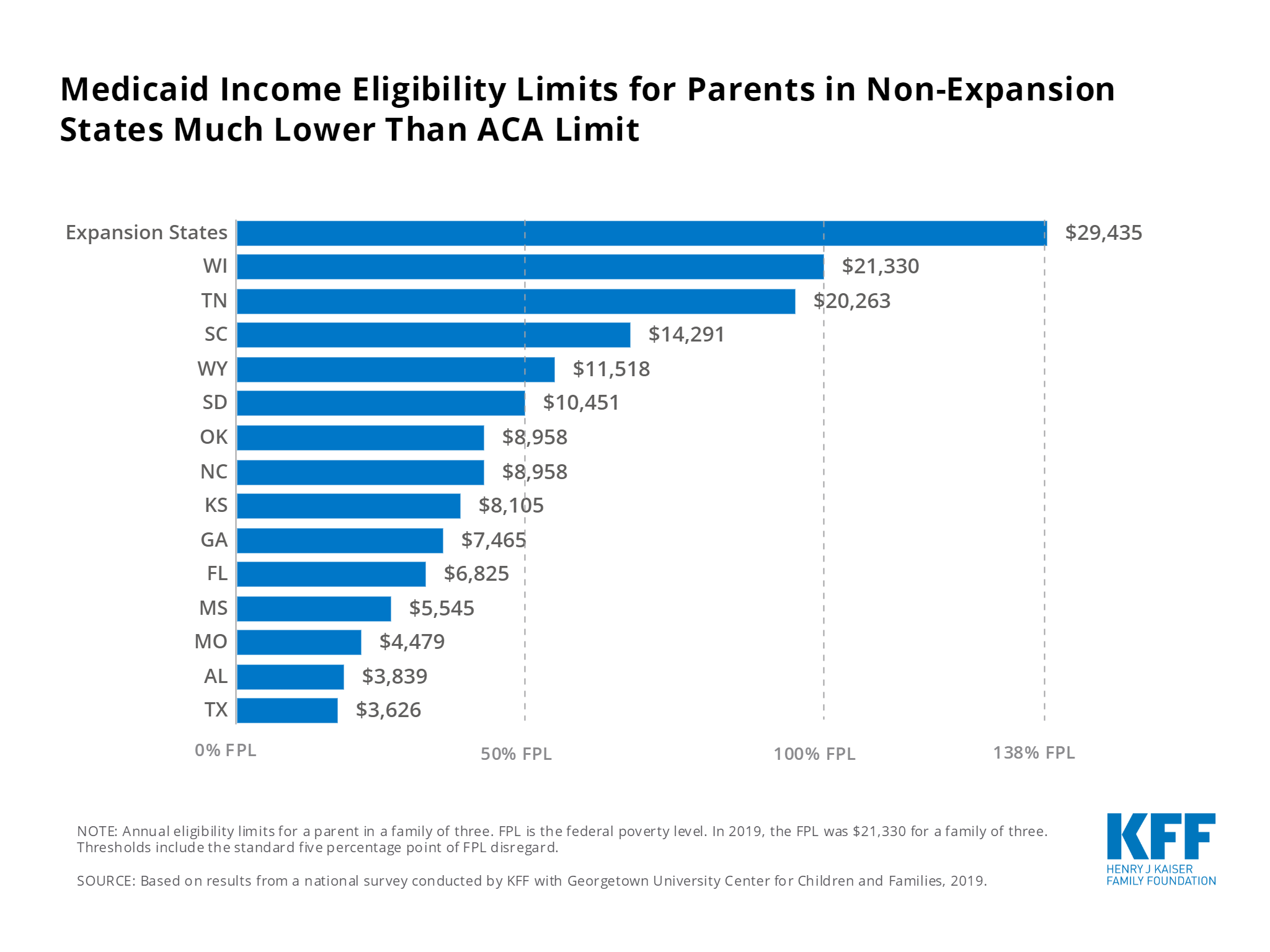
There might be some options to still receive Medicaid benefits if you make more than the income limit in your state.
The options do differ from state to state, but the majority do offer a pathway for those who would be considered medically needy and have high medical expenses.
If someone who requires a lot of medical care has too high of an income, they might be able to spend that income on their medical costs and then have that count against their income.
For example, if someone was $500 over the income limit in their state and that state has a program for the medically needy, they might be permitted to spend that excess income on their medical expenses and then receive Medicaid benefits after. This helps those with high than average medical costs be put on more equal footing for income eligibility requirements.
Not every state offers this particular program, however. For a great resource on the sorts of waivers, exceptions, and other eligibility information, visit this website. Once you click on your state of residence, you should be able to see which waivers are available in your state for those who exceed the income limit.
Recommended Reading: Who Gets Medicaid In Florida
How To Apply To Medicaid In Florida
Medicaid applications are reviewed by the Department of Children and Families in Florida. There are three primary ways to apply to Medicaid:
- In-person, at a local DCF branch
- Online, using the MyACCESS portal
- Over the phone, by calling 866-762-2237
If a person is moving from another state to Florida, they must re-apply for benefits regardless of any Medicaid coverage they had in their previous location. SSI recipients are automatically considered for Medicaid coverage in Florida, however they must submit a separate ACCESS application if they are applying for long-term care benefits.
How Does Medicaid Provide Financial Help To Medicare Beneficiaries In Florida
Many Medicare beneficiaries receive Medicaid financial assistance that can help them with Medicare premiums, lower prescription drug costs, and pay for expenses not covered by Medicare including long-term care.
Our guide to financial assistance for Medicare enrollees in Florida includes overviews of these programs, including Medicaid nursing home benefits, Extra Help, and eligibility guidelines for assistance.
Read Also: Does Medicaid Cover Gastric Bypass In Michigan
New Hampshire Medicaid Eligibility
Eligibility for Medicaid services in New Hampshire is generally based on your Modified Adjusted Gross Income . In some cases, MAGI wont be used to determine if you qualify for special programs in these instances, the Department of Health and Human Services will review your family size, home situation, and other financial resources.
Which Medicaid plan is best in New Hampshire?
Medicaid plans and programs in New Hampshire are based on specific needs and other factors, such as age, ability level, and health condition. You or your family may qualify for some services, such as Childrens Medicaid, coverage for pregnant women, or services for seniors.
You can learn more about applying for assistance here.
New Hampshire Medicaid Application:
Why Is The Income Test Important
The Income Test is important in Florida because this is a means test that allows eligible applicants to receive Medicaid. The importance of Medicaid cant be stated enough. Healthcare costs are growing each year, and can easily eat into a persons savings fast. The inheritance that many were hoping to leave for their loved ones may have to one day be used for nursing care, assisted living, or other forms of expensive care. This is why we recommend to all of our clients that they take advantage of every resource available, which includes receiving Medicaid benefits.
The problem is that not everyone can qualify for Medicaid benefits because they do not pass The Income Test or The Asset Test. This is why we often recommend clients use a Qualified Income Trust in order to take full advantage of their Medicaid benefits. Follow this link for more information on Qualified Income Trusts.
If you have questions about Medicaid or would like more information about Medicaid in Jacksonville or other areas of Florida, contact a Jacksonville Medicaid Eligibility Lawyers by email or call us at 904-685-1200 to discuss your situation today.
Also Check: How To Find Your Medicaid Number
How Many People Are On Medicaid
According to the Centers for Medicare & Medicaid Services, as of July 2020, here are the number of people enrolled in Medicaid and Chip in the entire United States:
- 75,521,263 individuals were enrolled in Medicaid and CHIP
- 68,826,573 individuals were enrolled in Medicaid
- 6,694,690 individuals were enrolled in CHIP
Medicaid Eligibility Information By State
Medicaid is a government-funded program designed to provide health care coverage for low-income households. This program receives funding from both the state and federal government. The federal government designed the program and maintains program regulations that states are required to follow. States, in turn, are allowed to make decisions regarding eligibility and benefits within the state. Each state maintains its own Medicaid website, which is used as a resource and portal for those applying for and receiving Medicaid.
Don’t Miss: Does Disability Count As Income For Medicaid
Florida Medicaid Income Limit Charts
The FL Medicaid eligibility income limit charts are divided by groups.
For example, the first chart is focused on income limits for children who qualify for Medicaid.
Similarly, the second chart below focuses on the Medicaid income limits for adults in Florida who qualify for Medicaid.
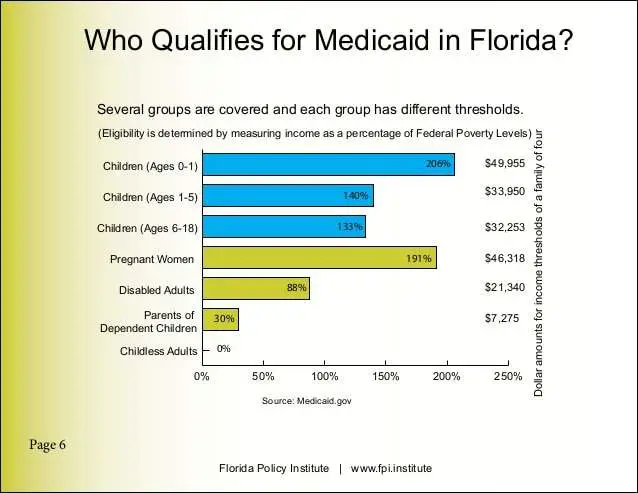
Florida Medicaid Income Limit for Children
Below is the income limit for children by age category. Find the age category your child falls into and you will see the income limit by household size.
| Florida Medicaid Income Limit Children |
| Children Medicaid Ages 0-1 |
| N/A |
How to Read the Florida Medicaid Income Limits Charts Above
You cannot have an income higher than the Federal Poverty Level percentage described for your group to be eligible for Medicaid.
Similarly, when you identify the income group that applies to you, the income limit you see refers to the maximum level of income you can earn to qualify for benefits.
For example, if you are pregnant, to qualify for Medicaid, you cannot have an income higher than 191% of the Federal Poverty Level which for a family of two is $33,272 as shown in the chart above.
Whos Eligible For Medicaid For The Aged Blind And Disabled In Florida

Medicaid for the aged, blind, and disabled can pay for Medicare cost sharing expenses, and cover some services not covered by Original Medicare. Beneficiaries whose incomes and assets make them eligible for Medicaid can receive coverage for those additional services if theyre enrolled in Medicaid for the Aged, Blind and Disabled .
This program is called Medicaid for the Aged and Disabled in Florida.
In Florida, Medicaid ABD covers dental services in emergencies. According to this website, Medicaid may also cover non-emergency dental benefits for some enrollees.
Medicaid ABD also covers eyeglasses , contact lenses, eyeglasses repairs, and will pay for prosthetic eyes.
Medicaid spend-down for Medicaid ABD in Florida
If an individuals income is over the eligibility limit for Medicaid for the aged, blind and disabled but their assets are below the resource limit, they can enroll in the Medicaid spend-down, which is also called the Medically Needy Program.
You May Like: Nursing Homes In Huntsville Al That Take Medicaid
Medicaid In 2021 For Aged And Disabled
- The MEDS-AD Program entitles eligible aged or disabled individuals to receive full Medicaid coverage.
- This program does NOT cover blind individuals unless they are considered disabled.
- Individuals cannot receive Medicare Part A or B unless the individual receives ICP, Hospice, or Home and Community Based Services Waiver.
Florida Medicaid Phone Number
Heres how to contact Florida Medicaid:
To reach Florida KidCare, call 1-800-821-5437.
For Medicaid Applicant & Member Services, call 1-877-711-3662, TDD 1-866-467-4970.
Customer Service is available Monday through Thursday from 8 a.m. to 8 p.m. Friday from 8 a.m. to 7 p.m.
If you are not enrolled in a health plan, call the Medicaid Helpline at 1-877-254-1055.
Also, if you need help finding contact information for your Medicaid plan, call ourMedicaid Helpline at 1-877-254-1055. You can get help with:
- Locating a doctor
- The services your plan covers
- Transportation to access covered services
- Other general questions you may have
Also Check: How To Apply For Medicaid In Houston
Asset Limits For Florida Long
Itâs important to note that there are different Medicaid programs in Florida. Some of which have higher asset limits. This article is only focused on the asset limits for those who need nursing home, ALF or home-health care.
Below, Iâll discuss a few different scenarios: the asset limit test for a single person applying for Florida long-term care Medicaid benefits the amount of assets a married couple can have if both are applying for ICP or Medicaid Waiver benefits and the asset limits a married couple can have if only one needs either of the above-referenced long-term care Medicaid benefits.
Floridas Requirements For Medicaid Qualification
In order to get Medicaid in Florida, you have to meet certain eligibility requirements. You have to be a certain type of patient for one thing. These include:
- Pregnant women
- Parents or relatives who are caretakers
- Families who might have lost Medicaid because of an increase in income or alimony
- Florida residents who receive SSI through the Social Security Administration
- Patients who are disabled or over the age of 65
- Children under 21
- Those who are eligible to receive Temporary Cash Assistance
- People under age 26 who were in a foster home
- People in nursing homes or those who receive community or home-based care.
You also have to be a Florida resident who has a valid social security number and a citizen of the U.S.
Don’t Miss: Florida Medicaid In Home Care
What Happens After I Apply For Medicaid In Florida
After you submit your Florida Medicaid application, you may be required to attend an interview with a Department of Children & Families case worker.
Whether you will required to attend an interview depends on your situation:
If you are applying for Medicaid for your child alone, then no interview will likely be required.If you are applying for any other benefits at the same time, then an interview will likely be required.
During this interview, you will be required to bring documents that prove the information that you provided on your initial Florida Medicaid application.
See above for the list of documents that may be required during the interview.
Once you complete this interview, you will receive a call or a letter in the mail that will tell you whether you were approved or denied.
If you are denied benefits, you have the right to appeal but that appeal must be filed within a certain timeframe. As your caseworker for details.
Emergency Medical Assistance For Non
Non-citizens may be eligible for Medicaid coverage in emergency situations including childbirth as long as they meet the other eligibility requirements.
To receive Medicaid coverage a non-citizen must do the following:
Complete a Medicaid application and provide the necessary verifications and
- Provide proof from a medical professional that the treatment was for an emergency, meaning it was due to a medical condition of sufficient severity that could result in placing the persons health in serious jeopardy.
- Medicaid can only be approved for the date of the emergency, and in case of childbirth there is no postpartum coverage.
- Non-citizens in the United States for a temporary reason, such as tourists or those traveling for business or pleasure, are not eligible for any Medicaid benefits with the exception of lawfully residing children , who are potentially Medicaid eligible.
Don’t Miss: Eye Doctors In Traverse City That Accept Medicaid
What Health Care Services Florida Medicaid Covers
Medicaid was enacted to provide better access to health care for those who might otherwise not be able to get the medical treatment they need. Because of this, the range of services Medicaid covers can be as diverse as the people who qualify for it. Medicaid coverage includes everything from dental work to dialysis, but due to what coverage group or plan you belong to your Medicaid coverage may be different than someone elses.
To see everything Medicaid includes and find out if you are eligible for coverage for certain services, head to the Agency for Health Care Administrations comprehensive Florida Medicaids Covered Services page here: .
Confirm with doctors and other health care providers before receiving treatment to make sure that Medicaid coverage applies.
Income Limits For Florida Icp Or Medicaid Waiver Program
The income test for long-term care Medicaid eligibility is the same regardless of whether the applicant is married or single. In any of the above-permutations, the Medicaid applicant can earn no more than the income cap amount, which changes from time-to-time in Florida. As of January 1, 2022, the Florida Income Cap is $2,523.00 per month. DCF will ask for statements from all income sources and if the total gross amount from all sources exceeds $2,523.00, then a Miller Trust will be required. Click the link to an article that further describes how a Medicaid Income Trust works.
Recommended Reading: How Many Levels Of Medicaid Are There
Institutional Care Program For 2021
- The Institutional Care Program helps people in nursing facilities pay for the cost of their care and provides general medical coverage.
- Must need of nursing facility services and appropriate placement as determined by the Department of Elder Affairs , must meet requirements as defined by the Comprehensive Assessment and Review for Long-Term Care Services .
Florida Medicaid Eligibility Requirements
Created by FindLaw’s team of legal writers and editors
There are many people in Florida who may qualify for medical care or nursing home treatment under Medicaid. Usually, those people are in a lower income bracket, and may have issues like disabilities or age that prevent them from working. If you would like to know more about eligibility for Medicaid in Florida, the following article provides the basics.
Recommended Reading: How To Apply For A Replacement Medicaid Card
Medicaid Eligibility For Persons With Disabilities
Individuals that are unable to work due to a disability may receive cash assistance through the Supplemental Security Income program. Qualifying for SSI automatically qualifies you for Medicaid in most states, but not all. The federal government requires all states to offer Medicaid to low-income disabled individuals. However, states are still allowed to set their own income eligibility requirements. Ten states, referred to as the 209 states have set income requirements that are more restrictive than SSI requirements. This means that individuals receiving SSI are not guaranteed Medicaid. They have to apply separately and be approved. These ten states are Connecticut, Hawaii, Illinois, Minnesota, Missouri, New Hampshire, North Dakota, Ohio, Oklahoma, and Virginia.
For individuals with a disability that have not been qualified for SSI, there are still options to qualify for Medicaid. Most states allow individuals with an impairment to prove that their impairment has prevented them from being able to work for at least one year. Once this is proven, the individual will be able to apply under the income and asset requirements for people with disabilities.
