How Does Medicaid In Colorado Work
To access medicaid dental benefits in Colorado, an application can be fill out at the Health First Colorado website or at a local office. The application will be reviewed to determine if you can qualify for medicaid dental benefits. Once approved for benefits, a member identification number will be issued much like a private insurance plans. Provider locations and contact info can be accessed through the Health First Colorado website or through common search engines.
Does Medicaid Cover Invisalign Braces
Medicaid is supposed to serve as a health insurance safety net. It is government-provided health insurance for people who cant afford insurance on their own. Its available to low-income individuals and to families who meet certain eligibility requirements. Payments are made directly to health care providers and sometimes a small copay is required from the patient.
How Can You Determine If You Qualify For Braces With Medicaid
In 2019 the AAO sought to clarify what is a medically necessary orthodontic procedure.
However, individual states still have a lot of say in what their Medicaid plans will cover and wont cover
A free consolation with a Medicaid-approved orthodontist can help you better understand if you should get braces and whether your Medicaid plan will pay for all the expenses or a fraction of them.
If Medicaid decides to pay for the cost of your braces partially, no need to panic that dental insurance isnt as expensive as Medical insurance, and you can get one to pay for as much as 1500 USD, about 25% of the cost.
But considering that the out-of-pocket costs for braces range from around 5000 USD to 7000 USD 3rd party dental insurance plan saves you a lot of money.
There are other options you should consider to manage dental expenses if Medicaid doesnt pay, and they include:
1. Getting your dental services from university dental school clinics
2. No-interest financing
3. Cash discounts
4. Tax-exempt saving accounts
Also, non-profit programs such as Smiles for a Lifetime and Smiles Change Lives can also offer you cut-price braces if you are a low-income individual who needs braces and cant afford the entire cost of orthodontic treatment.
Recommended Reading: Ohio Medicaid Customer Service Phone Number
Does Medicaid Cover Crowns
Have you ever wondered what your Medicaid would cover if you require dental work? Dont worry, you are not alone.
This is one of the reasons why we will go over all of the crucial aspects of Medicaid and dental coverage, with a specific emphasis on crowns. Because this procedure is so crucial for preserving a healthy and beautiful smile, you should discover all of the fascinating facts about it.
So, without further ado, lets get started with todays topic.
Does Texas Medicaid Cover Braces
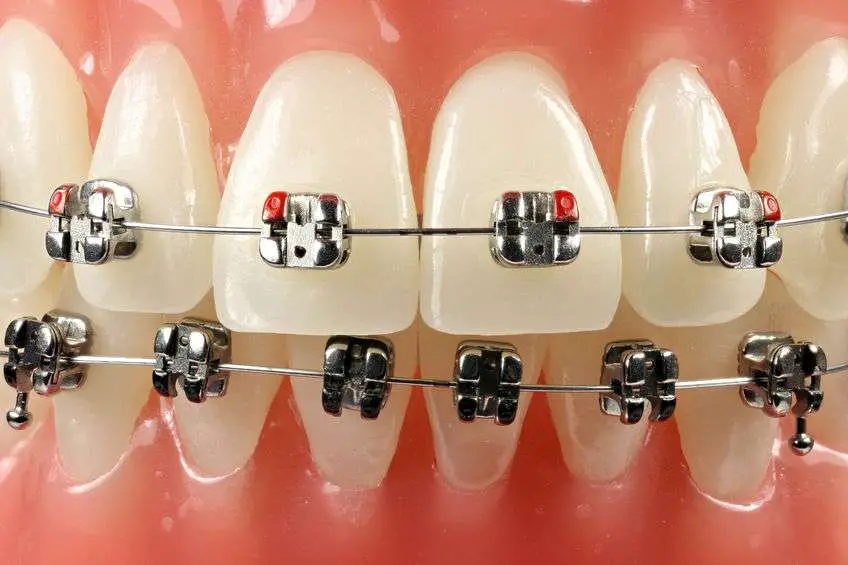
Texas Medicaid members with a severely handicapping malocclusion or particular medical disorders such as cleft palate, post-head trauma injury involving the oral cavity, and/or skeletal deformities impacting the oral cavity are covered for comprehensive medically required orthodontic therapy. Orthodontics includes the diagnosis of dental problems and the application of specialized treatments designed to correct misaligned teeth and improve overall facial appearance.
Orthodontists are doctors who specialize in treating irregularities in the way your teeth grow into place by using gentle pressure waves from an electric toothbrush and special tools called implants. They work closely with your dentist to develop an individual treatment plan for you that involves both surgical and non-surgical options. Non-surgical treatments include rubber bands, clear aligners, and other devices used to move teeth quickly without surgery. Surgical treatments include tooth extraction, bone grafting, and other procedures used to correct severe cases of malocclusion.
Recommended Reading: Medicaid Office In Vicksburg Mississippi
Does Medicaid Cover Braces For Adults
Yes. While certain Medicaid plans now include orthodontic braces for adults and other dental benefits, only a few people over 21 get their braces covered .
Medicaid covers medically necessary treatments to prevent disease or injury, like broken jaws or dislocated teeth requiring orthodontic treatment.
Some may ask, does Medicaid cover dental implants for adults? Dental implants could be a medical necessity covered by Medicaid if the patient needs them to fix a functional impairment affecting basic oral activities.
Is It Ok To Have Dental Work While Pregnant
Dental work while pregnant, such as cavity fillings and crowns, should be treated to reduce the chance of infection. If dental work is done during pregnancy, the second trimester is ideal. It is best to avoid this dental work while pregnant and avoid exposing the developing baby to any risks, even if they are minimal.
You May Like: Can I Put Braces While Pregnant
Also Check: Does West Virginia Have Expanded Medicaid
Early And Periodic Screening Diagnostic And Treatment
8.280.4.E Other EPSDT Benefits
Other health care services may include other EPSDT benefits if the need for such services is identified. The services are a benefit when they meet the following requirements:
Dates Of Service After The Death Of A Health First Colorado Member
Health First Colorado will reimburse supply providers for durable medical rental equipment, oxygen, and bulk supplies that are drop-shipped to the member’s home for services rendered during the month of the member’s death, only if the claims date of service is before the members date of death. Health First Colorado will make recoveries for all DMEPOS services following the date of the member’s death.
The interChange operationalizes this policy in the following ways:
- If the claim’s ‘date of service’ occurs before the member’s ‘date of death’ within the same month, the claim will be paid and not recouped.
- If the claim’s ‘date of service’ occurs on/after the member’s ‘date of death’ within the same month, and for all following months, the claim will be denied or eventually recouped.
Span Billing for Certain Supplies
The following items may have a date span of up to 30 calendar days on claims submitted to the Department:
- Diabetic testing supplies
- Continuous passive motion devices
- Parenteral and enteral nutrition
- Parenteral and enteral administration kits
- External infusion pump supplies
- Over the Counter, at-home COVID-19 tests
You May Like: Dental Surgeon That Accepts Medicaid
Does Medicaid Cover Orthotics Without A Copay
State Medicaid programs are allowed to charge nominal copays for some services, including orthotics. In most states, the copay is a flat fee, but some states require enrollees to pay for a certain percentage of the cost. For example, South Dakota requires enrollees to pay 5% of the Medicaid-approved amount. Some states set their copays based on each enrollee’s financial situation. In Montana, enrollees who are at or below 100% of the Federal Poverty Level pay a $4 copay, while enrollees above the Federal Poverty Level pay 10% of the cost. Many states require no copays for orthotics, including Arizona, California, Connecticut, Hawaii, Louisiana, Massachusetts and Vermont.
What Dental Treatments Does Medicaid Cover
Medicaid coverage varies from state to state, but in most states basic preventive dental services are covered. These services include x-rays, exams, cleanings, fillings, and extractions. Many states also offer orthodontic care and denture coverage as well. Restorative and cosmetic services are not covered by Medicaid except in rare circumstances.
Read Also: Florida Medicaid Income Limits 2020
Medicaid Dental Coverage By State
| States that provide extensive Medicaid dental coverage | States that provide limited Medicaid dental coverage | States that only cover emergency Medicaid dental services | States that dont provide any Medicaid dental coverage | States who expanded Medicaid under the Affordable Care Act |
|---|---|---|---|---|
| Alaska, California, Connecticut, Iowa, Massachusetts, Montana, New Jersey, New Mexico, New York, North Carolina, North Dakota, Ohio, Oregon, Rhode Island, Washington, Wisconsin | Arkansas, Colorado, Ilinois, Indiana, Kansas, Kentucky, Lousiana, Michigan, Minnesota, Montana, Nebraska, Pennsylvannia, South Carolina, South Dakota, Vermont, Virginia, Wyoming | Arizona, Florida, Georgia, Hawaii, Idaho, Maine, Maryland, Mississippi, Nevada, New Hampshire, Oklahoma, Texas, Utah, West Virginia | Alabama, Delaware, Tenessee | Arizona, Hawaii, Maryland, Nevada, Hew Hampshire, West Virginia, Arkansas, Colorado, Illinois, Indiana, Kentucky, Louisiana, Michigan, Minnesota, Pennsylvania, Vermont, Alaska, California, Connecticut, Iowa, Massachussets, Montana, New Jersey, New Mexico, New York, Ohio, Orgegon, Rhode Island, Washington |
As you can see from this table that shows Medicaid dental coverage by state, different benefits are given to those in the Medicaid base population and Medicaid expansion population.
People who fall into the Medicaid base population are those who were receiving Medicaid before the Medicaid Expansion Program under the Affordable Care Act.
Colorado Access Child Health Plan Plus
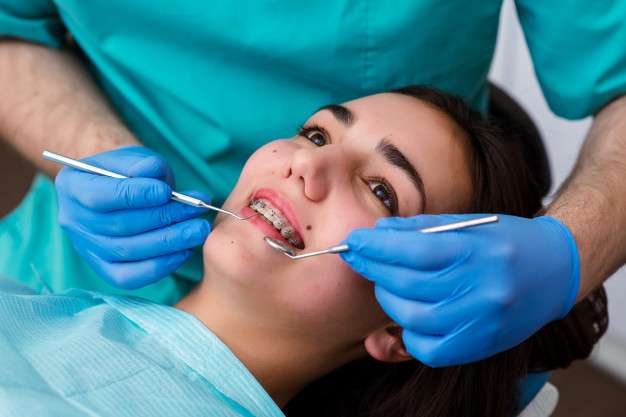
We participate in the Health First Colorado Dental program! To use your benefit, this program requires a records submittal before treatment can be started. Click Schedule Pre-Authorization Records to schedule your first visit with our records tech. We will take 2 digital radiographs, photos, and 3D scan of your teeth. Records will be reviewed and submitted to see what coverage you will qualify for under your insurance plan.
Medicaid/DentaQuest will cover the cost of this records appointment. Please note: Coverage must be active on appointment date.
Child Health Plan Plus / Colorado Access: A non-refundable copay of $250 is due at the time of this records appointment. Please note: CHP+ does not supply a benefit for Phase I orthodontic treatment. It is recommended to Schedule A New Patient Consultation if your child has baby teeth, you are unsure if they have baby teeth, or if you are interested in our flexible, interest-free monthly payment plans.
You May Like: How Does Someone Get Medicaid
Contact Your Metro Denver Coorthodontic Specialists
Have more questions about our financial policies or want to learn more about how to pay for braces? Were here to help. Feel free to call us with any questions, or use our easy online form to schedule an appointment at one of our six Colorado office locations. We cant wait to hear from you, and we look forward to helping you achieve a beautiful, healthy smile affordably!
Dme Safety Equipment Policy
As part of the Prior Authorization Request process, Health First Colorados PAR vendor reviews requests for safety of the member. It is the members responsibility to ensure safe installation of any safety equipment that modifies the home and or their environment. This would refer to items such as rails that attach to a wall, toilet, or other part of the home. The department refers to these items as permanently affixed safety equipment. Due to substantial risk of safety for the member, the department will not approve of safety items that are not permanently affixed. This includes but is not limited to items attached by means of a suction cup or tension mechanism.
However, PARs are still reviewed for safety on an individual basis and this policy should not be used to assume that all permanently affixed items are safe for every member.
DME most commonly impacted by this policy: E0241 Bathtub wall rail, eachE0242 Bathtub rail, floor base, eachE0243 Toilet rail, each
You May Like: Does Medicaid Work Out Of State
The Average Cost Of Orthotics
Custom orthotics are much more expensive than the over-the-counter kind, but they’re also more effective. Without insurance, it may cost anywhere from $200 to $800 to have custom orthotics made. It could cost even more if your doctor orders a foot X-ray or performs other services before deciding that wearing orthotics is the best course of action. Over-the-counter orthotics may cost as little as $10 per set, but remember that they’re not customized for your feet, so they may not help with proper foot alignment.
Dental Care For Children Ages 0
- Dental Exams
- Problem focused
- Pain management
Some Services may require permission from a dental plan before the dentist performs the service. This is called a prior authorization. Services must be medically necessary in order for dental plans to pay for them. For more details about dental services, contact the recipientâs dental plan starting December 1, 2018.
- Additional dental exams
Also Check: Can You Get Lasik Eye Surgery While Pregnant
Read Also: Dc Medicaid Customer Service Number
How To Apply For Medicaid
Because Medicaid is administered through the state and states determine eligibility, you will need to visit your states Medicaid office or website to apply. When applying you will need proof of income, residency, age, citizenship and/or immigration status for every member of your household.
Contact your state Medicaid office . Getting approved for Medicaid can take time, so start the application process as soon as there is a clear need. Most offices allow you to apply or at least start your request online. You may need to go into one of their offices for an interview as part of the application process. Have all your needed verification documents ready.
Medicaids Eligibility factors include income, residency, age, citizenship, immigration status, household composition, and pregnancy.
The exact verification documents you will need will vary based on what state you are in. However, be prepared to have any proof of income, proof of residency, your social security card, and immigration status confirmation documents on hand . Generally, household composition and pregnancy status do not require formal verification.
Who Is Eligible For Apple Health
People of all ages may be eligible for coverage under Apple Health, including yourself, your parents, and your children. The Washington State Health Care Authoritys website details all the ways you may be eligible for Apple Health. Click the link below that best describes you and/or your family to learn more.
Dont Miss: Can I Use Vagisil Wash While Pregnant
Don’t Miss: Pediatricians In Austin Tx That Accept Medicaid
How Can I Enroll In Apple Health
You can enroll in Apple Health at any point during the year on the Washington Healthplan Finder. If you do not qualify for Apple Health, the Washington Healthplan Finder has many other insurance options for you to choose from.
About 7-10 days after applying for Apple Health coverage, a ProviderOne services card will be mailed to you. This is a plastic ID card that looks like other health insurance ID cards. Take this card with you to your doctor and dentist appointments. Providers use this card to make sure your service is covered.
You May Like: Is It Safe To Take Tums While Pregnant
When Does Medicaid Cover Adults Braces
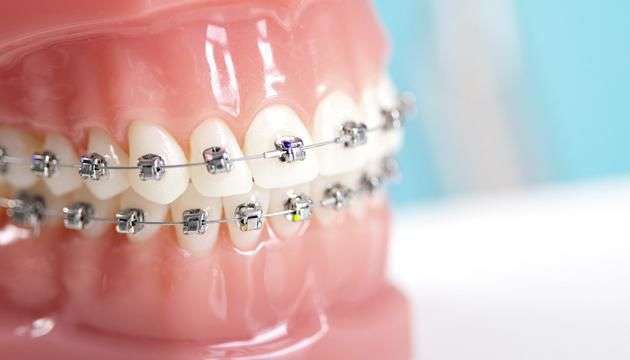
Although Medicaid, for the most part, only pays for childrens orthodontic procedures, in recent times, it has expanded its coverage to include indigent or low-income adults, pregnant women, or disabled persons.
However, in the case of braces, adults rarely qualify for Medicaid.
Medical necessity is a critical factor in determining whether Medicaid will pay for braces in adults.
For instance, Medicaid can pay for braces for adults who have dislodged teeth or broken jaws as a result of an accident.
Adults who have ailments that affect the jaw and neck also have a valid reason to lay claim to dental coverage by Medicaid.
Medicaid will also pay for teeth repositioning procedures to correct the following conditions:
1. TMD or TMJ .
2. Sleep Apnea.
3. Handicapping Malocclusions.
When presenting your case for Medicaid to pay for your braces, ensure the data is detailed about a medical condition thats impacted by problems with the mouth or jaws.
Braces can be approved without treatment if youre experiencing pain, youre ill, or you have an infection.
Also, if the condition impacts the normal functioning of your body or your ability to go about your routines, then braces can also be approved by Medicaid.
Read Also: Molina Medicaid Michigan Prior Authorization Form
Medicaid At Kids Choice Dental
At Kids Choice Dental, we understand the importance of dental hygiene and how critical it is for your child to receive the appropriate dental care to avoid bigger problems in the future. Thats why we provide care through Medicaid for those families that need a helping hand. We are always excited to help your child get the best dental care they can in Colorado. Contact our staff today and schedule your appointment or, if you have any questions, please dont hesitate to ask them well be more than happy to answer them!
What Does Medicaid Cover at Kids Choice Dental?
At Kids Choice Dental in Colorado, Medicaid often covers the entire procedure or dental service your kid would need. We are happy to work with you and your child to get you the best solution for their dental needs and ensure that they can leave our dentist clinic with a beautiful smile. Set up an appointment today to learn more about the dental needs of your child, what Medicaid covers, and how to move forward with your childs dental care. We look forward to hearing from you!
Adult Medicaid Including Medallion And Ccc+
Effective January 1, 2019 adults in Virginia with household incomes up to 138% of the federal poverty level are eligible for Medicaid. Medicaid covers dental extractions and related costs. HOWEVER, the Managed Care Organizations administering the program have added additional benefits such as comprehensive exams and cleanings. Some even offer money towards other dental care. If you wish to change Managed Care Organizations so you get different dental benefits, call the Managed Care Helpline at 1-800-643-2273 . The helpline is available Monday through Friday from 8:30 am to 6:00 pm.
If you are disabled and have both Medicaid and Medicare you also have additional benefits
Cover Virginia is your best source for information if you are new to Medicaid. Their website is
Also Check: How To Add A Baby To Medicaid
