Stick To The Colorado Medicaid Formulary
Health First Colorado includes a comprehensive prescription drug benefit. Most adults will pay $3 per prescription, but pregnant women and children will not have a co-pay. In most cases, you will receive the generic version of whatever prescription you need. To receive the brand-name drug, you will need prior authorization. Generic drugs almost always have the same effect as their brand-name counterparts.
This Colorado Medicaid Formulary , or preferred drug list, is what your doctors and other providers should stick to when prescribing your medication. If they attempt to prescribe you a drug that is not on the list, remind them that you are a Medicaid beneficiary and will either need a different drug or their authorization for coverage of the other drug. Youll notice that you will not find fertility drugs, cosmetic drugs, weight-loss drugs, or any DESI drugs on the list. Those items will not be covered by Health First Colorado.
When Medicaid Covers Eye Exams
Medicaid sometimes covers eye exams for adults. The reasons for the visual testing and your state of residence determine whether your plan will honor claims and how frequently.
Finding a local eye doctor that accepts Medicaid could prove challenging due to the low reimbursement rates and varying levels of coverage.
- Medicaid acts as health insurance with relatively uniform benefits across the country for medically necessary eye care.
- Medicaid acts as vision insurance with widely varying benefits state-by-state when measuring refractive errors.
What Is A Prior Authorization And How Do I Get One
A Prior Authorization is a request from your provider for Health First Colorado to cover a drug not listed on the Preferred Drug List or otherwise listed on Appendix P of the Preferred Drug List. Your provider will submit the prior authorization request for you. After your prior authorization request is reviewed you and your provider will find out Health First Colorado’s decision. If the criteria are not met, the doctor can re-submit with updated information, or appeal the decision to Health First Colorado’s Pharmacy Benefits section for further review.
Each request is processed within 24 hours, and most phone requests are given the approval/denial decision immediately upon submission. If you have an emergency, your provider can get a 72-hour emergency supply of the drug you need.
Colorado Pharmacy Call Center phone number: | Colorado Pharmacy Call Center Fax Number: 800-424-5881
Don’t Miss: Does Maryland Medicaid Cover Abortions
Does Medicaid Cover Prescription Eye Exams
Eye exams are an important part of vision health and therefore covered by Medicaid. Some types of eye exams may be covered under your standard health insurance plan.
Medicaid covers many types of eye exams, including exams for vision prescriptions. Eye exams covered by Medicaid include:
- Routine exams.
- Glaucoma screening.
What Is Not Covered By Medicaid If You Need Glasses

While the rules and regulations vary by state, you are generally not covered for:
- Transition lenses
- Oversized lenses
- No-line bifocals or trifocals
As usual, check with your doctor or the Medicaid representative in your state and locality to see if these particular lenses are covered by Medicaid. Sometimes they are just partially insured, and you simply need to cover the difference in cost.
Don’t Miss: When Does Medicaid End For A Child In Nc
What Exactly Is Medicaid
Medicaid is one of the government-created financial support programs in the United States for low-income households. This program, unlike others, concentrates on medical requirements and covers the bulk of expenditures for those in need and their family members.
However, as fantastic as this program is, there are a few ambiguities that leave consumers wondering what is and is not covered by this medical insurance.
There are some standard and obligatory treatments that are covered in all states, but the amount that Medicaid will fund in most circumstances is determined by the state in which you live. Because each country has the authority to implement the Medicaid program as it sees suitable, there are numerous laws and regulations.
Differences Between Medicaid And Medicare
Both Medicaid and Medicare cover medical costs, but theyre different government programs and have different regulations. Medicare pays medical bills from the money contributed to a trust fund by its beneficiaries.
Regardless of income, Medicare primarily pays medical bills for those who are:
- 65 years old and older
- Disabled, regardless of age
- On dialysis
Patients pay part of their medical expenses through deductibles and other expenses.
In contrast, Medicaid is an aid program meant for those who earn below a certain income level and serves people across all ages. With Medicaid, patients do not pay a part of their costs, though sometimes, a small co-payment is needed.
Don’t Miss: Does Medicaid Pay For Prescription Glasses
How Will You Know If You Have Medicaid
If you want to know whether you have Medicaid and can use it to pay for your eyeglasses, consult your plan provider. You can get his/her contacts on one of the online directories that show you where to get eyewear providers who accept Medicaid.
You can also visit your states Medicaid site to check if you qualify for the program then apply to join. Remember that the qualification rules change, so check regularly to know when you are eligible.
What Is Medicaids Stance On Contact Lenses
Where contact lenses are concerned, its important to know the following:
1. All contact lenses must be approved beforehand by Medicaid.
2. Medicaid doesnt pay for contact lenses meant for cosmetic purposes.
3. Medicaid covers both soft and rigid contact lenses .
4. If the recipient can wear both soft and rigid contact lenses, Medicaid will pay for the least expensive alternative.
Don’t Miss: Medicaid Assisted Living Austin Texas
Where Can You Use Medicaid To Get Glasses
The next step in getting new glasses is to choose an eye doctor. This implies you should verify your insurance card and call the business in charge of your Medicaid plan.
They will be able to give you a list of available doctors who take Medicaid at their offices, from which you can select the finest one for you.
What Addiction Treatment Services Does Colorado Medicaid Cover
Treatment for mental health, substance use disorder, or behavioral services are covered by the Colorado Medicaid program. Coverage includes:
- Alcohol and drug assessment
- Physical assessment of detoxification progression
- Alcohol and/or drug services, including targeted case management and group counseling by a clinician
- Drug screening and monitoring
- Behavioral health counseling and therapy for individuals and groups
- Safety assessment, including suicide ideation
- Family therapy
- Emergency and crisis services
- School-based mental health services
The Health First website states that these services do not require co-pays or have limits to the amount of their coverage. Some authorization by a medical provider or other sources may be required for some of the treatment options.
Recommended Reading: Annual Income Eligibility For Medicaid
What Are Medicaid And Medicare
Medicaid and Medicare are health insurance programs funded by federal and state funds. When Title XIX of the Social Security Act was signed into law in 1965, this act created Medicaid and Medicare. Both programs are available in all fifty states, the District of Columbia, and the U.S. territories. Medicaid is intended as assistance for low-income families in need of a public insurance program.
In 2010, the Affordable Care Act , sometimes known as Obamacare, designated that Medicaid must cover basic tenets of treatment for drug and alcohol addiction. This means that Colorado Medicaid for addictiontreatment may be the assistance you need to take advantage of our world-class program.
Chp+ Colorado And Family Planning
For the Family Planning program, There are no co-pays for family planning office visits, counseling, sterilization, and contraceptives. Limits include one exam per year and up to three months worth of contraceptives at one time. Sterilization is only available to those over the age of 21. There are no co-payments for prenatal and postpartum care, child delivery, newborn health care , or substance abuse treatment for pregnant women.
CHP+, the kids program, is slightly different. Kids get added benefits like blood work, specialist visits, x-rays, and full dental and vision. Emergency care co-pays can range from $3 to $50, medical visits can be up to $10, inpatient hospital stays can reach up to $50, therapy services can reach up to $10, and prescriptions can range from $0 to $15.
Read Also: How To Qualify For Medicaid In Oregon
What Information Will I Be Asked To Submit With My Application
The application will ask you to submit your income information or any other proof for your eligibility category. You will not be asked to show proof of immigration or citizenship status. You also do not need to submit a written statement from your physician proving that you experienced an emergency.
What Is A Preferred Drug List
The Health First Colorado Preferred Drug List includes clinically effective medications that you can get without needing prior authorization or approval. This list is updated regularly. You may still be able to get drugs not on the Preferred Drug List. To get drugs that are not preferred on the Preferred Drug List, your provider will need to get prior authorization from Health First Colorado.
If you are already taking a drug not on the Preferred Drug List or your drugs gets removed from the Preferred Drug List, you may be able to keep taking the same drug. Talk to your provider about staying on your same drug.
Also Check: Where Can I Apply For Medicaid In Florida
Can You Get Bifocal Transition Lenses
Transitions VI® lenses are compatible with virtually all frame styles and they’re available in most types of lens materials and designs, including plastic and thinner materials like polycarbonate and Trivex®. Transitions are available in single-vision lenses, bifocals, multi-focals and progressive lenses.
Are Transition Lenses Covered By Insurance
Photochromic lenses, sometimes referred to as “transition lenses” after the well-known brand name, Transitions, are eyeglass lenses that can change from clear to dark, depending on the environment. Typical costs: … Photochromic lenses typically are covered, at least partially, by vision insurance.
Recommended Reading: How To Get Medicaid For Child
Who Is Eligible For Emergency Medicaid
To be eligible for Emergency Medicaid, applicants must meet the same eligibility requirements as all other Health First Colorado applicants, except for immigration or citizenship requirements. Applicants also must have a qualifying life- or limb-threatening medical emergency covered by Emergency Medicaid. Emergency Medicaid benefits are limited to the treatment of medical emergencies only. Health First Colorado recognizes that all situations are unique, so please apply to see if you are eligible.
While all applicants for Health First Colorado or Child Health Plan Plus will be asked to provide a social security number, you do not need a social security number to receive emergency services under Emergency Medicaid.
People who may qualify for Emergency Medicaid include, but are not limited to:
- Deferred Action for Childhood Arrivals recipients
- Undocumented people
- Non-immigrant visa holders such as tourists and students
- Individuals granted Temporary Protected Status
- Adult legal permanent residents who have not been in the U.S. lawfully for at least five years
- This does not apply to children and pregnant people who qualify for Medicaid with full benefits
We encourage all uninsured people to apply for Health First Colorado to see if they qualify, even if they are unsure of their immigration status.
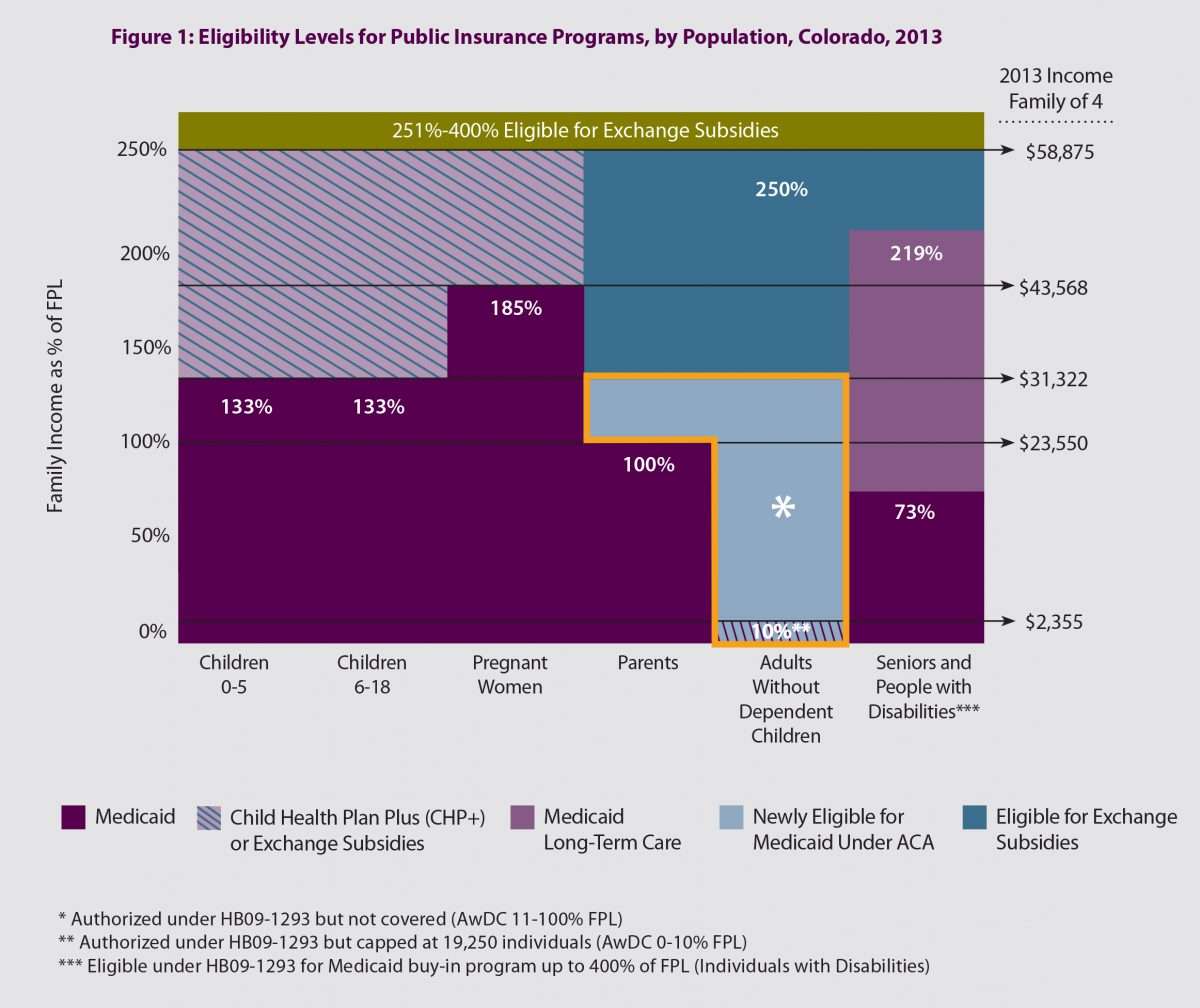
Medicaid Income Limits Colorado
To qualify for Health First Colorado, you must be a Colorado resident, U.S. citizen or legal alien, and your income must* fall at or below the following income limits .
*If your annual earnings are higher than these numbers but you spend enough on your medical expenses to fall below these numbers, you may still qualify for medical assistance. Additionally, older adults who do not qualify based on income may still qualify for the Old Age Pension Medicaid or Old Age Pension Health Care programs. Fill out the Medicaid application to find out if you qualify.
- Rehabilitative services
Don’t Miss: How To Become A Medicaid Provider In Texas
How To Get Cgm For Medicaid Patients
Medicaid in Colorado has certain eligibility requirements that must be met in order to provide coverage for personal CGM. If the patient does not meet them, Professional CGM may be an option for intermittent use. This resource will help you navigate Colorado Medicaids eligibility requirements for coverage, ordering and insurance authorization, and documentation. To download this resource as a PDF, .
For a comparison guide on helping your patient choose a CGM and tips on navigating common problems, .
Colorado Medicaid Eligibility Requirements for personal CGM
In order to be eligible for Colorado Medicaid coverage of personal CGM, the followingrequirements must be met:
Example Documentation
Chart note example: The following is an example of text that you can add to your chart notes for patients meeting Colorado Medicaids eligibility criteria. You can copy/paste, add to your EHRs macro library , and/or modify as needed:
How to Order a Dexcom
- Complete the Byers CGM Order Form .pdf?sfvrsn=ad9d8fba_2″ rel=”nofollow”> printable form or fillable form)
- Email or Fax: chart notes, Byers CGM Order Form, and patient contact information to:
Dental Coverage Under Medicaid
Medicaid dental benefits are one of the most contentious issues surrounding this insurance since some states provide full coverage while others do not.
The good news is that children under the age of 21, pregnant women, and the elderly are normally covered for all medical expenditures without having to make a co-payment.
In terms of adults, different states will enable Medicaid to cover a variety of services. In general, Medicaid covers everything that is deemed medically essential. Does this, however, include crowns?
Continue reading to learn more.
Don’t Miss: How Long Does It Take For Medicaid To Start
Does Medicaid Replace Glasses
Medicaid typically replaces glasses, but the frequency with which you may do so is determined by your age and the state in which you live.
Children and young people under the age of 21 can often get two replacements each year. The remainder of Medicaid patients typically receives one replacement each year.
This covers scenarios in which the glasses are broken, stolen, or misplaced. Furthermore, in many jurisdictions, Medicaid will pay for the cost of fixing spectacles.
Who Does Medicaid Provide Vision Coverage For
Federal law requires that vision care be provided through Medicaid to children and adults under the age of 21. Regular well visits that include vision screenings help to reduce the occurrence of eye conditions later in life. The idea is that prevention is the best way to keep costs down overall.
There are no federal regulations, however, that require Medicaid to provide vision care for adults over the age of 21. Standard vision coverage options are offered by each state, though the specific services can vary greatly. Its important to confirm the specifics of coverage with your state.
Optometry services and eyeglasses are optional benefits under Medicaid. Optional medical services may come with a small copay for the individual. Again, the amount will vary by state.
In order to qualify for Medicaid coverage, you must meet certain requirements. You can qualify for Medicaid based on the following factors:
- Income
- State residency
If you have questions regarding your eligibility status, you can contact Medicaid directly.
As of October 2019, over 71 million people were enrolled in Medicaid across the country. Over 35 million of those individuals were children enrolled in Medicaids Childrens Health Insurance Program .
Medicaid provides affordable and essential health care services to individuals and families who may otherwise not be able to afford it.
Also Check: How To Cancel Medicaid In Virginia
What States Allow Medicaid To Cover Glasses
We said that most states enable Medicaid to pay your glasses and related expenditures, however, this is not the case in all states.
The following states DO NOT allow Medicaid to cover glasses:
- Arizona
- Routine and comprehensive eye exams
- Safety frames
- Prosthetic eyes
All of the above-mentioned examinations and products are considered optional, and just a few states permit them. As usual, the best thing you can do is contact your plan assistant and request further information.
How To Take Advantage Of Your Medicaid Vision Benefits
If you have Medicaid for vision coverage, it is likely that you will need a referral from your primary care provider in order to see an ophthalmologist
Ophthalmologist visits are usually covered through your standard Medicaid insurance, as care from a specialty doctor. By getting connected with an ophthalmologist, you can take advantage of the eye care benefits offered through Medicaid. This includes exams and assessments for eye diseases and conditions.
To get in touch with a local Medicaid office, visit the federal governments website at Benefits.gov. From there, you can filter information by state and subcategory to find the contact information for a Medicaid office near you.
You can also ask a specific eye care provider for assistance on using your Medicaid coverage. Some providers dont take Medicaid, but they may be able to refer you to another provider who does.
Recommended Reading: Does Medicaid Pay For Hospice Room And Board
Does Medicaid Pay For Contacts
Asked by: Mrs. Kali Ritchie
Medicaid can pay for prescriptions under most circumstances, as well as contact lenses. They handle the financial reimbursement of frames in a similar fashion to their policy on eye exams, wherein your prescription must be prescribed by an optometrist for a medically necessary cause.
Lenses Covered By Medicaid
If you need new glasses through Medicaid, it is important to be aware of which types of lenses are covered. Regular single vision lenses are covered by Medicaid, for near and distance vision correction.
If you need bifocals or trifocals, Medicaid will also usually cover the cost. It will generally cover the cost of one pair of bifocals or trifocals, or two pairs of single vision glasses.
Lenses that are not covered by Medicaid include:
- Oversized lenses.
- Progressive multifocals.
- Transition lenses.
If you would like to have any of the above lenses, you can still get them with your Medicaid coverage. You will just have to pay the difference in cost for such specialty lenses.
Additionally, contact lenses are not typically covered by Medicaid. If you want contacts, you will probably have to pay for them out of pocket or with a different supplemental insurance plan. In some cases, contact lenses are covered, but only when they are deemed to be medically necessary.
Also Check: Florida Medicaid Managed Care Organizations
