Ohio Medicaid Changes To Prescription Drug Coverage Take Effect Today
About 1.5 million Ohioans enrolled in the state’s Medicaid managed care plans will be forced to change the way they get their prescriptions starting today.
The move, which is expected to save about $243 million in the state’s budget, affects more than 193,000 residents in Cuyahoga County. Local community activists are concerned that the switchover will confuse people and lead to not getting their medications on time.
“Hopefully, it will go seamless. … but there’s a lot of detail work and who knows?” said Gail Long, a community health advocate.
The Ohio Department of Jobs and Family Services, which oversees the state’s Medicaid program, has sent letters to managed care enrollees describing the switchover, according to Ohio Medicaid Program Director Tracy Plouck.
Below are some common questions and answers on the changes:
Who will be affected?
Anyone enrolled in one of Ohio’s seven Medicaid managed care plans and getting prescriptions. That includes members of AmeriGroup Community Care Buckeye Community Health Plan CareSource Molina Healthcare of Ohio Paramount Advantage Unison Health Plan of Ohio and WellCare.
What will change for members of those plans?
Will prescriptions continue as normal and uninterrupted?
Yes.
Will there now be a charge for prescriptions?
Is there a requirement to switch to generics? Possibly. In most cases, Ohio Medicaid requires that a generic drug be used if it is available.
What Documentation Do You Need For Blood Pressure Monitors
When it comes to obtaining your Medicaid to fund any DME, you must supply all of the necessary papers.
This includes the following:
- Official diagnosis from your doctor as to why you require the blood pressure monitor
- A treatment plan, which may include medication
- If the patient is under the age, a pediatricians prescription is required.
The documents required may differ from state to state, since each state has the authority to govern Medicaid as they see suitable. This is why you should check with your Medicaid or health insurance provider to see whether you are qualified for a blood pressure monitor.
Unitedhealthcare Dual Complete Plans
Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
You May Like: Does Medicaid Cover Home Birth In Texas
Unitedhealthcare Connected For Mycare Ohio
UnitedHealthcare Connected® for MyCare Ohio is a health plan that contracts with both Medicare and Ohio Medicaid to provide benefits of both programs to enrollees. If you have any problem reading or understanding this or any other UnitedHealthcare Connected® for MyCare Ohio information, please contact our Member Services at from 7 a.m. to 8 p.m. Monday through Friday for help at no cost to you.
Si tiene problemas para leer o comprender esta o cualquier otra documentación de UnitedHealthcare Connected® de MyCare Ohio , comuníquese con nuestro Departamento de Servicio al Cliente para obtener información adicional sin costo para usted al de lunes a viernes de 7 a.m. a 8 p.m. .
Does Medicaid Cover All Expenses
Medicaid generally covers all expenses for covered care, but there may be circumstances in which small monthly premiums, deductibles or copayments are required. These include people with incomes above a certain amount in some states or when non-emergency services are administered in an emergency room.
Higher-risk groups such as children and pregnant women are typically exempt from any expenses
Also Check: Does Medicaid Pay For Retainers
Unitedhealthcare Connected Benefit Disclaimer
This is not a complete list. The benefit information is a brief summary, not a complete description of benefits. For more information contact the plan or read the Member Handbook. Limitations, copays and restrictions may apply. For more information, call UnitedHealthcare Connected® Member Services or read the UnitedHealthcare Connected® Member Handbook. Benefits, List of Covered Drugs, pharmacy and provider networks and/or copayments may change from time to time throughout the year and on January 1 of each year.
You can get this document for free in other formats, such as large print, braille, or audio. Call , TTY 711, 8 a.m. – 8 p.m., local time, Monday – Friday . The call is free.
You can call Member Services and ask us to make a note in our system that you would like materials in Spanish, large print, braille, or audio now and in the future.
Language Line is available for all in-network providers.
Puede obtener este documento de forma gratuita en otros formatos, como letra de imprenta grande, braille o audio. Llame al , TTY 711, de 08:00 a. m. a 08:00 p. m., hora local, de lunes a viernes correo de voz disponible las 24 horas del día,/los 7 días de la semana). La llamada es gratuita.
Puede llamar a Servicios para Miembros y pedirnos que registremos en nuestro sistema que le gustaría recibir documentos en español, en letra de imprenta grande, braille o audio, ahora y en el futuro.
Los servicios Language Line están disponibles para todos los proveedores dentro de la red.
Rehabs That Accept Ohio Medicaid
More than 2.7 million individuals were receiving Ohio Medicaid as of September 2018. Medicaid is a state- and federally-funded insurance plan which provides free and low-cost healthcare coverage for individuals who meet income and other requirements.
Ohio Medicaid makes it possible for these individuals to secure necessary medical care, including addiction treatment, for little to no cost.
Because the cost of treatment can keep many individuals from receiving the care they need to enter recovery, Ohio Medicaid can provide a great advantage in helping people make lasting changes in their lives.
For those looking to use Ohio Medicaid to pay for an alcohol or drug rehab program, it may be a good idea to first research which rehab centers accept their Medicaid plan.
Recommended Reading: When Does Medicaid End For A Child In Nc
Does Medicaid Cover Vivitrol
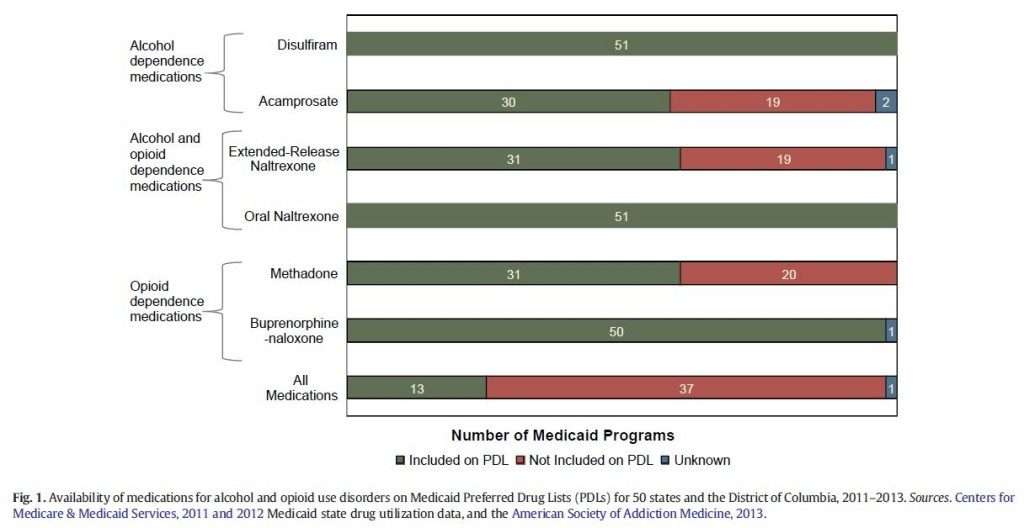
Vivitrol is a long-acting, injectable medication that is covered by Medicaid in all 50 states and the District of Columbia . Eligibility requirements, including an FDA-approved diagnosis, may apply in order to receive insurance coverage for Vivitrol.
Vivitrol is a prescription medication for alcohol and opioid use disorder. It is covered by Medicaid health plans in all 50 U.S. states and the District of Columbia.
Eligibility requirements for receiving Medicaid coverage for Vivitrol may vary according to your state of residence and the type of Medicaid coverage plan you have.
Nova Behavioral Health Dayton Ohio
Residential programs through Nova are specialized to meet the needs of a specific group and include:
- womens treatment program: short-term, gender-specific program for women which focuses on exploring their emotional, social, and life issues
- mens residential program: short-term, gender-specific program for men focuses on helping men overcome their issues
- dual disorder treatment: involves a combination of mental health counseling and therapy and substance use treatments
- Morningstar program: a program for individuals with a prominent mental health disorder and a minor substance use problem
Due to the variation of programs offered at Nova Behavioral Health, programs are highly customized and may include a number of the following treatments:
- 12-step group involvement
253-1680
You May Like: Medicaid And Other Health Insurance
American Disabilities Act Notice
In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
Member Advisory Council And Connected Advisors
UnitedHealthcare Care Managers for Member’s Unique Needs
Every UnitedHealthcare MyCare Ohio member receives a personal representative. These Care Managers are licensed professionals providing education and coordination of UnitedHealthcare Connected® for MyCare Ohio benefits, tailored for each member’s unique needs.
to watch a video on how these Care Managers are helping current members.
We recently mailed you a letter that included some information on benefit changes. Some of the information did not pertain to members that only have their Medicaid covered benefits through our plan. Please disregard that letter. The letter also had an incorrect number for the Ohio Medicaid Hotline. The correct number for the Hotline is 1-800-324-8680. We are sorry for any confusion this may have caused you. Please view the Member Clarification Letter for additional information.
Use the documents below to learn more about each important health topic.
-
PDF 180.50KB – Last Updated: 11/12/2020
UnitedHealthcare Member Advisory Council and “Connected Advisors”
UnitedHealthcare Member Advisory Council and “Connected Advisors” is an advisory council to ensure that UnitedHealthcare actively engages consumers, families, advocacy groups, and other key stakeholders as partners in the program design and delivery system.
Who is involved?
They will advise and guide the UnitedHealthcare Community Plan of Ohio on:
How is it organized?
What will they do?
-
PDF 26.62KB – Last Updated: 11/12/2020
Read Also: Does Medicaid Cover Weight Loss Pills
Unitedhealthcare Senior Care Options Plan
UnitedHealthcare SCO is a Coordinated Care plan with a Medicare contract and a contract with the Commonwealth of Massachusetts Medicaid program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is a voluntary program that is available to anyone 65 and older who qualifies for MassHealth Standard and Original Medicare. If you have MassHealth Standard, but you do not qualify for Original Medicare, you may still be eligible to enroll in our MassHealth Senior Care Option plan and receive all of your MassHealth benefits through our SCO program.
Can I Use My Medicaid Coverage In Any State
You can’t take it with you: If you’re relocating, you’ll need to reapply for Medicaid in the state where you’re planning to reside.
Q. Can I use my Medicaid coverage in any state?
A: No. Because each state has its own Medicaid eligibility requirements, you cant just transfer coverage from one state to another, nor can you use your coverage when youre temporarily visiting another state, unless you need emergency health care.
Medicaid offers health coverage to millions of Americans, and in many states, that coverage matches or even surpasses that of private health insurance. Medicaid is jointly funded by the federal government and state governments, but each state has the option to set its own rules and requirements for eligibility. As such, transferring your Medicaid coverage from one state to another isnt always possible.
Recommended Reading: Dentist In Brookhaven Ms That Accept Medicaid
Traveling To Another State
If youre traveling to another state and fall ill, you may be out of luck Medicaid wont cover the cost of services in a state that isnt your home state. Generally, you can only use your Medicaid coverage out-of-state if you encounter a true life-threatening emergency that requires immediate care .
That said, sometimes, pre-approved treatment at an out-of-state facility is covered by Medicaid, but only when proper authorization is obtained. Similarly, Medicaid coverage may kick in if you receive treatment in an out-of-state facility that borders yours, and in which residents of your state routinely seek care. Again, you must make sure Medicaid will cover such care before pursuing it, or you risk getting stuck with the associated bills.
Maurie Backman has been writing professionally for well over a decade, and her coverage area runs the gamut from healthcare to personal finance to career advice. Much of her writing these days revolves around retirement and its various components and challenges, including healthcare, Medicare, Social Security, and money management.
Why Did I Get Denied For Medicaid
Theres a multitude of reasons why someone may get denied for Medicaid coverage. Aside from not meeting the financial or demographic requirements, some common reasons for a denied Medicaid application include:
- Incomplete application or documents
- Failure to respond to a request within a timely manner
- Late filing
- Disability not proven or otherwise not medically qualified
Dont forget that mistakes can be made on behalf of Medicaid, and you have a right to appeal Medicaids decision concerning your coverage. Contact your state Medicaid program for instructions about how to appeal a decision if you are denied benefits.
Don’t Miss: Problems With Medicare And Medicaid
Medicare Cover Prescription Drugs Under Original Medicare
Most Americans with Medicare choose to get their benefits through the Original Medicare program, which is administered by the federal government. Original Medicare splits its coverage into three parts, known as Parts A, B, and D. Medicare Part A pays for hospital and other inpatient costs, while Part B assists with outpatient expenses, such as medical office visits. Prescription drugs administered while in the hospital, such as surgical anaesthetics, are generally paid for under Part A, while vaccines and other provider-administered medications usually fall under Part B.
Part D is the main prescription drug benefit under Original Medicare. This element pays for some of the cost of the drugs beneficiaries pick up from the pharmacy and take at home. Part D coverage levels vary by state and by a specific plan, but participants are generally expected to pay a monthly premium for their Part D plan and cover the listed copayment amounts. Out-of-pocket costs go as high as $5,100 per calendar year in 2019.
Do I Need A Prescription To Get My Catheters Covered By Ohio Medicaid
Yes, catheters are a prescription-only item. Ohio Medicaid will require a prescription from your doctor for the supplies you need.
Also, Ohio Medicaid may request more supporting documentation, such as medical progress notes.
In addition, if you need coudé catheters, Ohio Medicaid will request a process of Prior Authorization to approve this type of catheter. This is because coudé catheters are typically only approved for use in cases when straight tip catheters are not able to be passed normally.
Dont worry about all these requirements though. Once youve seen your doctor, 180 Medical is happy to do the groundwork to get any documentation from your physician. Also, well handle contacting Ohio Medicaid to verify your coverage and eligibility.
Recommended Reading: How To Get Both Medicare And Medicaid
Learn More About Medicare
Join our email series to receive your free Medicare guide and the latest information about Medicare and Medicare Advantage.
Medicaid coverage can vary a bit from state to state, so a service or item that is covered in one state may not be covered in another. Optional benefits that may or may not be covered depending on the state include:
- Prescription drugs
- Physical and occupational therapy
- Respiratory care
- Speech, hearing and language disorder services
Again, coverage rules vary by state. If you would like to know if Medicaid will cover a particular service or item, contact your state Medicaid program for assistance.
Does Medicaid Cover Blood Pressure Monitors
Over 100 million Americans suffer from high blood pressure, which is one of the most serious long-term illnesses. It can lead to a heart attack, a brain aneurysm, or a stroke, and controlling your blood pressure is one of the best methods to avoid it.
Because this entails prescription medicine and blood pressure monitoring, many people ask if Medicaid will pay the expenses of blood pressure monitors.
If you were wondering the same thing, youve come to the correct spot since we have all of the answers in one place. This will assist you in making the most of your Medicaid resources and determining the best effective therapy for you.
You May Like: Medicaid Ga Number Customer Service
Preferred And Preventive Drugs
In recent years, drug costs have increased dramatically. The rise in prices for medications can be a source of frustration for your patients. At the same time, we understand that harshly limiting the medications our physicians can prescribe in order to cut costs would only lead to frustration for our providers.
With such concerns in mind, our employer groups, physicians and members challenged us to develop a prescription benefit that helps reduce drug benefit costs while maintaining physicians’ freedom to select the most appropriate drugs. We rose to the challenge by introducing our innovative Four-Tier Preferred Drug prescription benefit with the following copay structure:
- Generic drugs at the lowest copay
- Preferred brand name drugs at a mid-level copay
- Non-preferred brand name drugs at a higher brand copay
- Multi-Source brand name drugs at the highest copay
Drug Coverage Through Medicare Supplemental Plans

People who receive Original Medicare often find that their plans have certain gaps in coverage. Because these spaces can fall on the beneficiaries shoulders, many Medicare participants opt into a gap supplemental plan, or Medigap plan.
Medigap plans are offered by private insurance companies to fill the spaces left by traditional Medicare coverage. They are not, by law, intended for Part C beneficiaries, but for people enrolled in Original Medicare. Though Medigap plans are issued by private insurers in each state, both state and federal law require authorized plans to include minimum coverage levels and to meet other mandates, such as charging acceptable group rates and accepting applicants with preexisting conditions.
Policies offered under Medigap can help pay for some of the prescription drug costs that are not included under traditional Part D policies. Details of this coverage vary by state, as well as by individual provider within each state, so there is no national standard for how much of the cost of prescriptions must be covered. Fortunately, most states have several authorized Medigap providers, and many Medicare plan representatives can offer advice about choosing a supplemental plan that offers acceptable drug benefits.
Read Also: Apply For Sc Medicaid Online
