Medicaid Mental Health Benefits Explained
Medicaid is a public insurance plan that was established in 1965 along with Medicare. Its original purpose was to expand access to healthcare for people receiving public financial assistance.
Before Medicaid, people who couldnt afford to go to the doctor could usually only receive medical and mental health care at charitable organizations or state facilities.
Medicaid allowed many people with lower incomes to choose their providers for the first time.
Medicaid has expanded and contracted in different ways over time, but it has ultimately grown. Medicaid now covers more people than ever before, including people with disabilities, pregnant women, and people who work low-income jobs but dont have access to insurance through their employers.
Not only does Medicaid link millions of Americans with primary medical care, it has also become the single largest payer of mental health care in the United States.
Read on to learn whos eligible for Medicaid, how it works, and which mental health services it covers.
On This Page
- BetterHelp makes starting therapy easy.
- At OpenCounseling we have used BetterHelp and think they are a great option.
- Sign up today and get matched to a licensed therapist online.
- Get 20% off your first month with the link below.
How To Get Mental Illness Disability
People can investigate SSI and SSDI on their own. Each website has information about the program, benefit eligibility screening tools, and links to sections explaining how to apply .
The Social Security Administration tries to make the process straightforward and easy. Still, though, navigating the disability programs system can be nightmarish for anyone and especially for those frustrated by thechallenges of mental illness.
Help is available for people trying to secure disability benefits for mental illness. The following resources are good starting points on the journey of wading through the process of completing long applications, providing extensive documentation, and restarting the process if the benefits application is denied.
- Social workers and case managers are agents that advocate for their mentally ill clients in many ways, including helping them through the benefits application process.
- Social Security offices in local communities exist so people can receive human assistance with the process.
- Socialsecuritylaw.com is an organization of dedicated disability lawyers that efficiently and quickly help people secure disability benefits.
APA ReferencePeterson, T. . How To Get Disability Benefits For Mental Illness, HealthyPlace. Retrieved on 2022, January 7 from https://www.healthyplace.com/other-info/mental-illness-overview/how-to-get-disability-benefits-for-mental-illness
Is Depression Treatment Covered By Medicaid
Yes, depression has been recognized as one of the significant yet silent assassins of modern society, and it is one of the things for which you can seek counseling and be covered with Medicaid.
Each state has its own set of laws and restrictions, so make sure to consult your local Medicaid agents or health insurance reps for further information.
Don’t Miss: Dentist In Madisonville Ky That Accept Medicaid
The Barriers People On Medicaid Face
Mental health care is a chronically underfunded sector of the healthcare system, explained Dr. Amal Trivedi, MPH, professor of health services, policy and practice at Brown University School of Public Health.
Payment rates are so much lower for mental health care than they are for other types of care especially specialty care, in general. Many mental health providers do not accept Medicaid coverage and that is often driven by the lower payment rates.
Medicaid is a program that is often confused and conflated with Medicare in discussions about U.S. health coverage.
For reference, Medicare is meant to offer medical insurance coverage to people who are age 65 and older. Medicaid, on the other hand, offers health coverage to individuals and families with low incomes.
For most adults under 65, eligibility for a Medicaid program is having an income that is lower than 133 percent of the federal poverty line, according to the governments official Medicaid website.
The Childrens Health Insurance Program extends coverage to children.
For 2021, this would stand at $12,880 for a single person and ranges from $17,400 up to $44,660 for families of 2 to 8, respectively, according to Healthcare.gov.
The 2010 Affordable Care Act, so-called Obamacare, made it possible for states to cover virtually all lower-income people under 65.
Currently, 39 states, as well as Washington, D.C., have adopted some form of Medicaid expansion to cover more of their populations, according to KFF.
Disability Benefits For Mental Illness

Generally, governments establish assistance programs for people who live with a disability, either physical or mental, that renders them unable to work. In the U.S., the federal government operates over 40 programs that serve people of all ages with mental illness. States have their own disability programs, too, such as state Medicaid. Such programs vary from state to state.
The federal government operates two main disability programs for with people with mental illness if they qualify. These large benefits programs are the Supplementary Security Income program and Social Security Disability Insurance .
SSI, sometimes simply called Social Security, exists in order to help people with little or no income, including many people living with mental illness. The financial benefits provided are for basic needs like housing, food, and clothing. A serious mental illness alone doesn’t qualify someone for SSI, even if they can’t work. To receive SSI disability benefits for mental illness, one must live below the poverty line and have minimal access to financial resources.
Read Also: Blue Cross Blue Shield Nevada Medicaid
Parity Protections For Mental Health Services
This generally means limits applied to mental health and substance abuse services cant be more restrictive than limits applied to medical and surgical services. The limits covered by parity protections include:
- Financial like deductibles, copayments, coinsurance, and out-of-pocket limits
- Treatment like limits to the number of days or visits covered
- Care management like being required to get authorization of treatment before getting it
Coverage Expansion Contributes To Positive Mental Health
Being uninsured can create and compound stress by causing people to worry about medical bills and the cost of care, including behavioral health care. These financial concerns can lead people to delay seeking treatment until they are in crisis. Low-income people who are newly insured often experience improved mental health. For example, among low-income parents, Medicaid expansion meaningfully contributed to reductions in severe psychological distress as well as reduced difficulty paying medical bills. There is also evidence of improved mental health among low-income childless adults, who report fewer poor mental health days and fewer depression diagnoses.
Also Check: Can I Change Medicaid Plan
How Do I Find A Provider
Your primary care provider or regional organization can help you find a behavioral health provider.
Every Health First Colorado member has a primary care provider. Members and primary care providers belong to a regional organization that helps make sure Health First Colorado members get the health care and services they need. Regional organizations can also help members understand and manage physical and behavioral health benefits, find specialists or other providers, and connect members with transportation, food assistance or other social services, if needed.
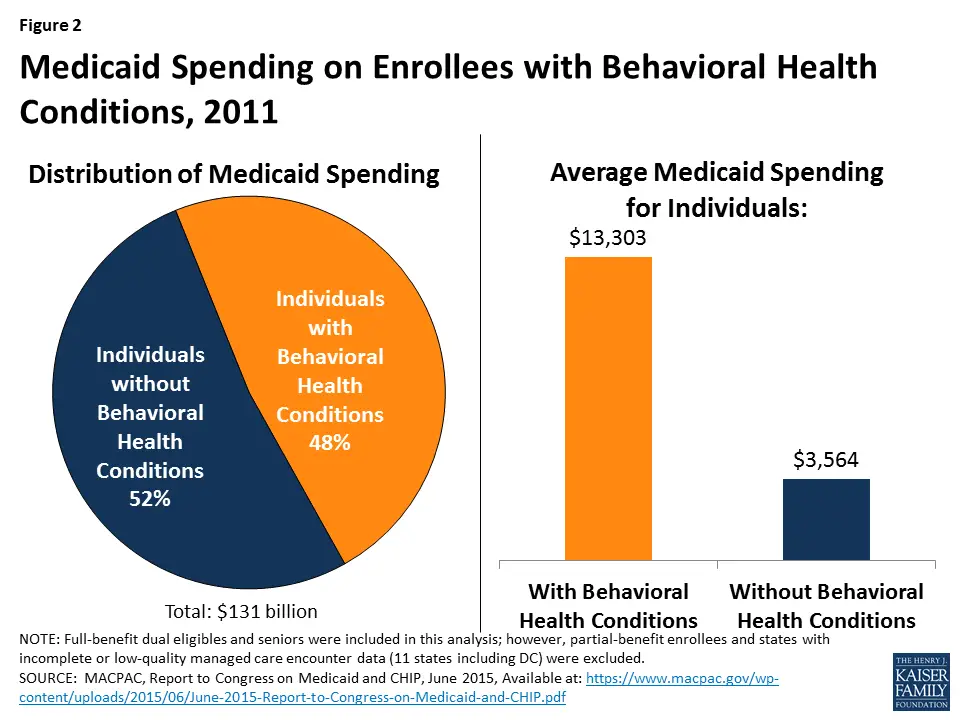
Medicaid Is The Single Largest Payer Of Mental Health Care In The United States
Medicaid is an essential link to mental health care for millions of Americans. It accounts for 25 percent of spending on mental health services in America every year, making it the largest single payer of mental health care in the country.
About 21 percent of adults with mental health conditions have Medicaid, compared to 14 percent of the general population.
Don’t Miss: Medicaid Health And Human Services
Dont Give Up The Resources Are Out There Possibly On Your Smartphone
Experts concur that it make take some time and effort to find a mental health provider, but your search will likely pay off. In the interim, you might want to turn to your smartphone.
Tele-mental health in all forms has become a huge resource and there are great resources online offered by large health systems, says Harry Nelson, managing partner of Nelson Hardiman, head of the Behavioral Health Association of Providers and co-author of From ObamaCare To TrumpCare: Why You Should Care. The challenge there is that you need to be licensed in the state where the patient lives, but that said, we’ve seen a flourishing growth in treatment of all mental health by telemedicine and I expect it to grow exponentially. Reach out to your local hospital system to ask if they offer these services.
Who Is Eligible For Medicaid
Until recently, you were only eligible for Medicaid when you had income below a certain level and were also a member of one or more of the following vulnerable groups:
- Pregnant women
- Low-income adults aged 65 or older
- Low-income parents of Medicaid-eligible children
- Disabled adults receiving SSI or Social Security Disability
The 2010 Patient Protection and Affordable Care Act expanded Medicaid to anyone whose income was at or below 138% of the Federal Poverty Level regardless of their membership in any of these groups.
While the law originally made Medicaid expansion a requirement for all states, in 2012, the Supreme Court ruled that states could elect whether to expand Medicaid. This means some states retain categorical eligibility requirements for Medicaid while others do not.
Where to Apply for Medicaid
If you think you might be eligible for Medicaid, you can apply for coverage at your local Social Services office.
Another way to learn whether you are eligible is to apply for an individual insurance plan through the federal Health Insurance Marketplace on HealthCare.gov. As part of the application process, you will be evaluated for Medicaid eligibility and allowed to apply online if you are eligible.
Read Also: How Do I Get My Medicaid Number
Taking Away Medicaid For Not Meeting Work Requirements Harms People With Mental Health Conditions
Medicaid is the nations largest payer of mental health services, providing health coverage to 26 percent of adults with a serious mental illness, many of whom obtained coverage through the Affordable Care Acts Medicaid expansion.
Now, however, the Trump Administration is allowing states to take away Medicaid coverage from people who dont document that they work a specified number of hours each month. This will harm people with mental health conditions, threatening their coverage and access to treatments including medications, therapy, and case management services.
The Administrations policy requires states to exempt people deemed medically frail and recommends exempting those with an acute medical condition that keeps them from working. But many people with mental health conditions likely wont qualify for an exemption or wont be able to prove they do. Thats what seems to have happened in Arkansas, the first state to implement such a policy, where the number of people who lost Medicaid coverage exceeded the work requirements presumed target population people who are neither working nor qualify for an exemption. More than 18,000 people in the state lost coverage in 2018 due to the new requirements.
Q: What Is The Health Insurance Marketplace
The Health Insurance Marketplace is designed to make buying health coverage easier and more affordable. The Marketplace allows individuals to compare health plans, get answers to questions, find out if they are eligible for tax credits to help pay for private insurance or health programs like the Childrens Health Insurance Program , and enroll in a health plan that meets their needs. The Marketplace Can Help You:
- Look for and compare private health plans.
- Get answers to questions about your health coverage options.
- Get reduced costs, if youre eligible.
- Enroll in a health plan that meets your needs.
Learn more at HealthCare.gov.
Also Check: Does Anthem Medicaid Cover Dental
Coverage Expansion Increases Behavioral Health Provider Capacity
Coverage expansion also contributes to increased access to behavioral health services by increasing behavioral health provider capacity. The more likely providers are to receive adequate reimbursement for their services, the greater their capacity to accept various forms of coverage. For example, providers of specialty mental health treatment were more likely to accept Medicaid after their states expanded eligibility under the ACA. And while much work remains to be done to ensure adequate reimbursement rates for providers of SUD treatment, evidence from states that increased Medicaid rates in recent years shows that these increases also contributed to greater provider participation in Medicaid. The more providers that accept Medicaid, the easier it is for enrollees to get the services they need when and where they need them. Closing the Medicaid coverage gap would benefit not only low-income patients but also the under-resourced providers that support them.
The Demand For Mental Health Services Is High
Earlier this year, KFF reported that about 4 in 10 adults in the United States reported symptoms of depressive disorder or anxiety over the course of the pandemic.
Similarly, a July 2020 tracking poll from the foundation discovered that U.S. adults were experiencing a range of negative symptoms that indicated a downturn in mental health from 36 percent reporting trouble sleeping to 12 percent revealing they increased the consumption of alcohol and other substances.
In short, the pandemics drastic, traumatic shifts to the ways we work, socialize, and ensure the health and safety of ourselves and those around us dramatically affected our mental health.
While the demand is there for mental health services right now, nationwide shortages in providers offering that kind of care underscores a large problem, especially for underserved, economically disadvantaged populations.
In just one example, many of New Hampshires 10 community health centers have 25 to 40 clinical staff vacancies, unable to fill needed positions, according to the New Hampshire Bulletin.
When it comes to reaching the mental health needs of their residents, rural and frontier counties in the United States have an average of just 1.8 and 1.5 licensed behavioral health providers, respectively, per every 1,000 Medicaid enrollees.
This compares to an average of 6.4 providers in urban counties, reports Health Affairs.
Also Check: Who Is Eligible For Medicaid In Nebraska
People Who Qualify For Medicaid Typically Require More Intensive Services
People on Medicaid have higher rates of mental illness than people in the general population and use mental health services at a higher rate than people who have other types of insurance. They also have high rates of comorbid medical disorders.
Medicaid Statistics
The following statistics are all provided by the Medicaid and CHIP Payment and Access Commission . According to MACPAC:
- About 10 percent of people on Medicaid have serious mental illness, relative to 3 percent of people with private insurance and 5 percent of people with no insurance.
- About 24 percent of people on Medicaid received mental health treatment in the past year, relative to 14 percent of people with private insurance and 10 percent of people with no insurance.
- About 44 percent of people on Medicaid had fair or poor health status in the past year, compared to 13 percent of people with private insurance and 24 percent of people without insurance.
This means that Medicaid is an important link that connects essential medical and mental health services with the people who need them most.
To Improve Behavioral Health Start By Closing The Medicaid Coverage Gap
Jennifer Sullivan, Miriam Pearsall, and Anna Bailey
Closing the Medicaid coverage gap is a critical step toward addressing the nations behavioral health crisis. In 2019, 2.2 million uninsured adults with incomes below the poverty line, which is too low to qualify for subsidized health insurance coverage in the Affordable Care Act marketplaces, were left without a pathway to coverage, because their states didnt expand Medicaid. Most of these adults live in the South, 60 percent are people of color, and more than 1 in 4, about 600,000 people, are estimated to have a behavioral health condition.
Improved access to coverage has been shown to increase access to behavioral health services by reducing financial barriers to care and increasing the number of behavioral health providers that accept Medicaid. Having health coverage has also been shown to improve mental well-being and reduce stress and anxiety among low-income people. For those without a pathway to coverage, closing the coverage gap would expand access to critically needed behavioral health services which include services to treat mental health conditions and substance use disorders at a time when the need for these services is high and increasing.
Policymakers have an opportunity to address the coverage gap in recovery legislation, which would help millions of currently uninsured people, many with behavioral health needs that can have fatal consequences when neglected, access the care they need.
Read Also: Montefiore Medicaid Office Bronx Ny
Office Of Mental Health
The Office of Mental Health provides a way for people to get the mental health treatment they need in a variety of settings, depending on age and conditions. However, several of our programs are limited to children under age 21. Some services are not covered, while others may require a specific diagnosis to be covered. Additionally, some services require prior authorization for coverage. Geriatric psychiatric services are not covered. The Office of Mental Health is comprised of three divisions: Mental Health Programs, Special Mental Health Initiatives, and Mental Health Services.
The Mental Health Programs division oversees the following programs:
- Intermediate Care Facilities for Individuals with Intellectual Disabilities
The Special Mental Health Initiatives division oversee the following programs:
- Autism Spectrum Disorder Services
- Community Support Program 1915
- Intellectual Disabilities/Developmental Disabilities Waiver
- Mississippi Youth Programs Around the Clock
- Substance Use Disorder Services
The Mental Health Services division oversees the following programs:
- Acute Freestanding Psychiatric Facilities
- Community/Private Mental Health Centers
- Federally Qualified Health Centers and Rural Health Clinics
- Outpatient Mental Health Hospital Services
- Psychiatric Residential Treatment Facilities
- Psychiatric Units at General Hospitals
- Psychiatric Services by Physicians or Nurse Practitioners
- Therapeutic and Evaluative Mental Health Services for Children
