Help For Adults And Seniors To Stay Safely In Their Homes
DHS has several programs that are designed to help adults with physical disabilities and seniors stay in their homes and communities rather than go to s skilled nursing facility. To apply for the programs below, please reach out to your local county office. If you would like to talk to a counselor about your options, call the Choices in Living Resource Center at 1-866-801-3435 or email .
ARChoices in Home Care provides attendant care, home-delivered meals, personal emergency response systems, adult day services, and respite care. Independent Choices is like ARChoices in Home Care, but the client is responsible for hiring, training, and supervising his or her in-home workers from Medicaid funds the client or his/her representative control.
Living Choices Assisted Living is a Medicaid program that pays for apartment-style housing for people who need extra care and supervision. Its for people who are at risk of being placed in a nursing home or who are in a nursing home and want more independence.
Program of All-Inclusive Care for the Elderly is for people age 55 and older who have been determined by the state, based on specific criteria, to need nursing home care. PACE allows them to live as independently as they can.
Eligibility For Medicaid For Aged Or Disabled
Aged or disabled individuals can receive benefits through Medicaid program. SSI related Medicaid has a simple application process and it covers most medical requirements of such individuals.
BenefitsApplication.com is not a government website or a government agency. You typically must work directly with the government to qualify for your program or benefits. This website and its contents are for informational purposes only. We do not claim responsibility for its accuracy.
Family Planning Only Coverage
You’re eligible to receive 10 months of Family Planning Only coverage after your pregnancy coverage ends, regardless of how it ends . This includes all forms of birth control, permanent methods to stop having children, and health checkups related to receiving birth control. This coverage is automatic.
Also Check: Dentist In Louisiana That Accept Medicaid For Adults
Do I Qualify For Insurance If Im Pregnant
As a result of the Affordable Care Act, all Marketplace plans must cover pre-existing conditions. Healthcare reports that. The government does not consider pregnancy to be a pre-existing condition. In other words, if you were pregnant at the time you applied for new health coverage: You are not eligible for coverage if you were pregnant.
Current Medicaid Access And Barriers
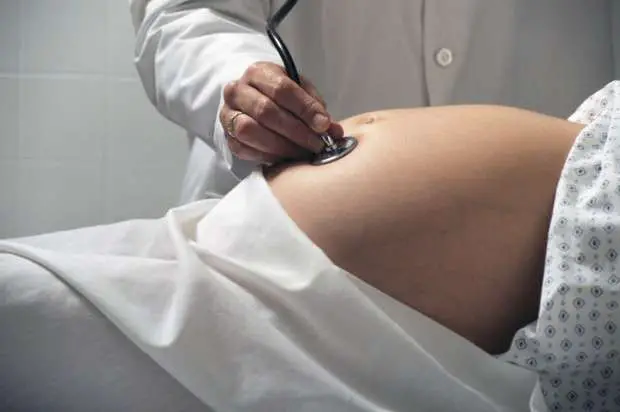
Women of reproductive age and pregnant women often rely on Medicaid to access health services ranging from prenatal to postpartum care. Only pregnant women with extremely low incomesapproximately $9,000 annually for a 4-person householdcan access Medicaid with all of its benefits. This full Medicaid coverage has the strictest qualifications of any form of Medicaid coverage in the state, limiting eligibility by income, family size, additional resource availability, citizenship status, and residency. If a woman’s finances improve, coverage can and often is revoked through the process of redetermination.
TABLE 1.
Medicaid Eligibility for Pregnant Women in North Carolina, 2019
Pregnancy coverage options are especially limited for North Carolina’s undocumented immigrant women, who are often low-income but do not qualify for either full Medicaid coverage or MPW. Many of these women must seek care at free clinics or Federally Qualified Health Centers. Understandably, this creates barriers to pre- and post-natal care. The Emergency Medicaid program covers the cost of births for undocumented immigrants, but program benefits do not extend to prenatal coverage or postpartum health care. Claims data for these services point to a significant level of unmet need. Nearly all of North Carolina’s Emergency Medicaid claims are to undocumented immigrants, and 4 in every 5 claims paid by the program are for obstetric diagnoses .
Recommended Reading: Denture Places That Accept Medicaid
Work Requirement Took Effect In June 2018 And 18000 People Had Lost Coverage By The End Of 2018
Arkansas received federal approval in March 2018 to make some modifications to the states Medicaid expansion program, including the implementation of a work requirement and the unconditional elimination of Medicaids three-month retroactive eligibility, replacing it with a 30-day retroactive eligibility provision instead. The waiver amendment was submitted in June 2017, and Arkansas had hoped to implement the changes by January 2018. But the waiver approval noted that the work requirement could be implemented no earlier than June 1, 2018.
The state wasted no time, however, and implemented it as of June 5, 2018. The work requirement was delayed until 2019 for people under the age of 30, but applied as of June 5 to people between the ages of 30 and 49 who werent otherwise exempt. They had to work or participate in other community engagement activities at least 80 hours per month in order to maintain access to Medicaid coverage. After three months of non-compliance, Medicaid eligibility would terminate.
So people began losing coverage as of the end of August for failure to comply with the work requirement including failure to comply with the onerous reporting requirements, detailed below. By the end of 2018, more than 18,000 people had lost their Medicaid coverage in Arkansas under the new work requirement. A beneficiary who lost coverage due to non-compliance with the work requirement was locked out of Arkansas Works until the end of the year.
Can A Pregnant Woman Receive Medicaid Or Chip Services Prior To An Eligibility Decision
Maybe. States may elect, but are not required, to provide some categories of Medicaid enrollees, including pregnant women, with presumptive eligibility. This allows pregnant women to receive immediate, same-day Medicaid services, typically at the clinic or hospital where they submit an application for Medicaid presumptive eligibility. Currently, 30 states provide presumptive eligibility to pregnant women.
Don’t Miss: Michigan Medicaid Nursing Home Application
Lawsuit Over Arkansas Medicaid Work Requirement Was Slated For Scotus But Hearing Was Canceled And Work Requirement Waiver Was Then Rescinded By Hhs
The Trump administration appealed the case, as expected, and a panel of three judges on the U.S. Court of Appeals for DC heard oral arguments in the appeal in October 2019. During the arguments, all three judges expressed concerns about the coverage losses that stem from Medicaid work requirements, which was the crux of Boasbergs ruling earlier in the year that suspended the work requirement. And in February 2020, the three-judge panel unanimously ruled that it was arbitrary and capricious for HHS to approve the Arkansas Works waiver, and upheld Boasbergs ruling to overturn the states Medicaid work requirement. So the work requirement has remained suspended.
In July 2020, however, the Trump administration asked the Supreme Court to intervene and allow Arkansas to reinstate its work requirement once the COVID-19 situation is under control enough to allow the unemployment rate to return to normal levels. The Supreme Court justices agreed to hear the case, and oral arguments in the lawsuit, Arkansas v. Gresham, were scheduled for March 29, 2021 at the Supreme Court.
But the Biden administration does not support Medicaid work requirements, and asked the Supreme Court to cancel the hearing. That request was granted, and Arkansas v. Gresham was not heard by the Supreme Court.
Dont Miss: Lasik During Pregnancy
Apply For Medicaid For Aged Or Disabled
Applying online: Individuals can apply for Medicaid electronically. All they have to do is to go to ACCESS Florida website and fill out the application forms there. The entire process can be completed online. You will automatically qualify for Medicaid if you are eligible for SSI. You can apply for SSI using this LINK. However, if you need nursing services, you will have to make sure that you are checking the box that asks for HCBS or Nursing Home on benefit information page. This program will provide services for assisted living so that individuals do not have to be institutionalized.
Recommended Reading: Does Walmart Vision Center Accept Medicaid For Contacts
Read Also: Find A Ob Gyn Who Takes Medicaid
Benefits Of Medicaid For Pregnant Women
First, you will be given a list of medical providers who accept Medicaid or given a website to look for a provider in your area.
Second, pregnant women are covered for all care related to the pregnancy, delivery and any complications that may occur during pregnancy and up to 60 days postpartum.
Third, as long as you receive care from a Medicaid provider, your health care costs will be submitted through Medicaid and will be covered, in accordance with Medicaid regulations and guidelines.
Finally, Medicaid usually gives Pregnant women priority in determining Medicaid eligibility. Most offices try to qualify a pregnant woman within about 2-4 weeks.
If you need medical treatment before then, talk with your local office about PE Medicaid as explained above.
Get Important News & Updates
Sign up for email and/or text notices of Medicaid and other FSSA news, reminders, and other important information. When registering your email, check the category on the drop-down list to receive notices of Medicaid updates check other areas of interest on the drop-down list to receive notices for other types of FSSA updates.
Don’t Miss: Guidelines To Qualify For Medicaid
Option 2 Apply At Medicaid Application Center Near You
You can apply in person at a Medicaid Application Center near you. to locate an office.
Option 3 Download Application
You can an application, complete it, and mail it to your county Medicaid Application Center or submit it in person.
For assistance with your Medicaid application, or to ask questions about programs or services, please call toll free 1.888.342.6207.
Do I Qualify For Medi

In order to qualify for Medi-Cal managed care health plans, pregnant women must remain with their physician in Fee-for-Service during their pregnancy and postpartum period, unless they opt to enroll in Medi-Cal managed care. In addition to providing all medically necessary services, the expansion of coverage will ensure that pregnant women are covered.
Don’t Miss: What Benefits Do You Get With Medicaid
How To Apply For Medicaid In Arkansas
The Arkansas Medicaid application process is an opportunity for residents who cannot afford health insurance to obtain medical coverage. Learning how to apply for Medicaid in AR is beneficial for families who meet the eligibility requirements to receive Medicaid benefits. It is important for prospective applicants to understand what will be on the AR Medicaid application form and where to apply for Medicaid insurance in the state. If you are wondering, Can you apply for Medicaid online? or Where do you sign up for Medicaid in Arkansas? continue reading the outlined information below.
Where do you sign up for Medicaid in Arkansas?
While many states allow applicants to apply for Medicaid online, the state of Arkansas does not have a way to sign up for Medicaid via web. However, you may print the Medicaid form from the internet and fax it to 870-534-3421 or mail the form to:
DHS Jefferson County
P.O. Box 5670
Pine Bluff, AR 71611
If you are enrolled in the program, workers at the county office will provide you with more information on what health care services Medicaid covers and which medical providers are available to you. They will also ask you to pick a primary care physician.
Find out more about the requirements to receive benefits from Medicaid in our free guide.
Information Required on the Medicaid Application Form in Alabama
- Your name, birth date and Social Security Number
- Your before-tax income
You May Like: Is Vagisil Safe To Use While Pregnant
Does Pregnancy Medicaid Cover Dental
Although pregnant women enrolled in Medicaid and CHIP are entitled to ?pregnancy-related services,? dental care is not explicitly included as a pregnancy-related service, and federal Medicaid law leaves dental care for adult enrollees as a state option.3 CHIP requires coverage of dental care for youth, including
Also Check: Free Cell Phone Through Medicaid
You May Like: What Is The Best Medicaid Plan In Michigan
Arkansas Medicaid Expansion Enrollment Has Declined Significantly Since 2016
By September 30, 2016, total enrollment in expanded Medicaid in Arkansas had reached 324,000 . And by December 2016, there were 331,000 people enrolled in the states expanded Medicaid. The states total Medicaid enrollment grew by 70 percent from the end of 2013 to December 2016, reaching 948,181.
But as of January 1, 2017, enrolled in expanded Medicaid dropped to 310,951, following the states efforts to remove people from Medicaid who were no longer eligible from the program. 21,280 non-eligible people were removed from the states expanded Medicaid rolls at the start of 2017. Enrollment had climbed to over 320,000 by March 31, 2017, but it had declined to 285,000 by January 2018, in line with the decline in the states overall Medicaid enrollment from 2017 to 2018.
As of January 2019, enrollment in Arkansas Works stood at 234,400 people , although it had grown to . Thats more than 27% lower than it had been in 2016. Although that would be a positive change if the individuals in question had transitioned to employer-sponsored plans or other private health insurance options, Judge Boasbergs ruling makes it clear that there are certainly a number of people who have lost Medicaid coverage and simply become uninsured.
Dont Miss: Can I Drink Breakfast Essentials While Pregnant
Lawfully Present Immigrants And Marketplace Savings
If youre a lawfully present immigrant, you can buy private health insurance on the Marketplace. You may be eligible for lower costs on monthly premiums and lower out-of-pocket costs based on your income.
- If your annual income is between 100% and 400% of the federal poverty level : You may qualify for premium tax credits and other savings on Marketplace insurance.
- If your annual household income is above 400% FPL: You may still qualify for premium tax credits that lower your monthly premium for a 2021 Marketplace health insurance plan.
- If your annual household income is below 100% FPL: If youre not otherwise eligible for Medicaid youll qualify for premium tax credits and other savings on Marketplace insurance, if you meet all other eligibility requirements.
Recommended Reading: Walk In Clinic Takes Medicaid
What Services Are Covered
Medicaid covers breast pumps and breast feeding support during your pregnancy and after your baby is born.
You will get health care services through health plans. The health plans all have special programs for high-risk pregnancies. To learn more, go to Health Plan Information. Or call your health plan.
Early Periodic Screening Diagnostic & Treatment
Early and Periodic Screening, Diagnostic, and Treatment benefit includes a comprehensive array of preventive, diagnostic, and treatment services for Medicaid eligible infants, children and adolescents under age 21, as specified in Section 1905 of the Social Security Act . The EPSDT benefit is also available to PeachCare for Kids® members up to 19 years of age. The EPSDT benefit is designed to assure that children receive early detection and care, so that health problems are averted or diagnosed and treated as early as possible. The goal of the EPSDT benefit is to assure that individual children get the health care they need when they need it.
The EPSDT benefit also covers medically necessary diagnostic services. When a screening examination indicates the need for further evaluation of a childs health, the child should be appropriately referred for diagnosis without delay. States are required to arrange for and cover under the EPSDT benefit any Medicaid covered service listed in Section 1905 of the Act if that treatment or service is determined to be medically necessary to correct or ameliorate defects and physical and mental illnesses or conditions for children through age 20 years of age.
Reviewing your Health Check Record
Billing Tips for Health Check
Health Check Referral Codes
Read Also: Medicaid Fraud Cases In Louisiana
What Is Medicaid For Pregnant Women
With Medicaid for pregnant women, you get full health care benefits during your pregnancy and for two months after your babys birth. Medicaid may also cover your medical bills for the three months before you enroll. You also get dental benefits during your pregnancy. Dental services are through the Smiles for Children program. For help finding a dentist or to learn more, call Smiles For Children at 1-888-912-3456. Also read the Guide to Dental Coverage.
What Is The Highest Income To Qualify For Medicaid
According to the 2020 FPL, a family of three can expect to earn $21,330 in all 48 contiguous states plus the District of Columbia, increasing to $26,100 in Alaska. Families with three members can get by on $24,540 from Hawaiis FPL. Every American within the contiguous United States is subject to the Internal Revenue Code of 1988. Based on this figure, the FPL will be $12,490 in 2019.
Also Check: Medicaid Texas Income Limits 2020
Health Care Programs Eligibility
Health care coverage is available to individuals and families who meet certain eligibility requirements. The goal of these health care programs is to ensure that essential health care services are made available to those who otherwise do not have the financial resources to purchase them.
It is very important that individuals and families obtain health care coverage. In Michigan, there are many health care programs available to children, adults, and families. Specific coverages may vary depending on the program and the applicant’s citizenship status . The Michigan Department of Health and Human Services determines eligibility for most of the health care programs that are administered by the State of Michigan).
All of the health care programs in Michigan have an income test, except Children’s Special Health Care Services, and some of the programs also have an asset test. These income and asset tests may vary with each program. For some of the programs, the applicant may have income that is over the income limit and still be able to obtain health care benefits when their medical expenses equal or exceed their deductible amount.
