Louisiana Hhs Director Pushes To Keep Medicaid Expansion
On January 5, 2016, Edwards named Dr. Rebekah Gee to be the director of Louisianas Department of Health and Hospitals, which is the agency that oversees the states Medicaid program. Edwards said that Medicaid expansion would be one of Gees primary tasks, and Gee noted that the state would need to hire almost 250 people to process enrollments and manage the expansion of Medicaid.
Gee also said that Edwards administration would focus on working with doctors to ensure that there would be an adequate network of providers willing to work with the influx of new Medicaid patients gaining coverage under Healthy Louisiana.
Gee noted that in addition to the states portion of the cost of coverage for the newly eligible population, the state also had to pay 25% of the cost of hiring the 248 new state employees to handle the additional volume in the Medicaid program. The federal government would pay 75% of that cost, but the states portion was expected to be $2 million. Gee said that she was aware of the budget problems that were inheriting, calling them humbling but noting that the new administration had plans to deal with the budget issues.
Unitedhealthcare Connected General Benefit Disclaimer
This is not a complete list. The benefit information is a brief summary, not a complete description of benefits. For more information contact the plan or read the Member Handbook. Limitations, copays and restrictions may apply. For more information, call UnitedHealthcare Connected® Member Services or read the UnitedHealthcare Connected® Member Handbook. Benefits, List of Covered Drugs, pharmacy and provider networks and/or copayments may change from time to time throughout the year and on January 1 of each year.
You can get this document for free in other formats, such as large print, braille, or audio. Call Member Services, 8 a.m. – 8 p.m., local time, Monday – Friday . The call is free.
You can call Member Services and ask us to make a note in our system that you would like materials in Spanish, large print, braille, or audio now and in the future.
Language Line is available for all in-network providers.
Puede obtener este documento de forma gratuita en otros formatos, como letra de imprenta grande, braille o audio. Llame al Servicios para los miembros, de 08:00 a. m. a 08:00 p. m., hora local, de lunes a viernes correo de voz disponible las 24 horas del día,/los 7 días de la semana). La llamada es gratuita.
Puede llamar a Servicios para Miembros y pedirnos que registremos en nuestro sistema que le gustaría recibir documentos en español, en letra de imprenta grande, braille o audio, ahora y en el futuro.
How Do I Replace My Medicaid Id Card
Call Medicaid Customer Service at 1-888-342-6207 to request a new card or visit the online Medicaid Self-Service Portal. You can create an online account at any time. Until you receive your new card you should call your health care provider before your appointment to make sure they can verify your coverage.
If you need a new Healthy Louisiana plan ID card, call the member services department for a replacement card.
You May Like: How To Qualify For Medicaid In Utah
Mental Health Coverage Through Magellan Of Louisiana
Depending on your plan, you can get some mental health services covered by Healthy Louisiana. Some examples of covered services are mental illness, substance abuse, addictive disorders, drug and alcohol misuse, and mental disorders like autism.
Magellan of Louisiana is the MCO for LaCHIP. The MCO has mental health, substance abuse, and therapy providers. to find a Magellan provider near you.
How To Get Both Medicare And Medicaid In Louisiana
If you are eligible for Medicaid but you are also over the age of 65 or have been diagnosed with ALS or ESRD, you can ALSO get Medicare coverage. When you have both Medicare and Medicaid coverage, you are considered dual-eligible and can enroll in a Medicare Advantage dual-eligible special needs plan.
To get more information about saving money on health care by enrolling in Medicare Advantage, set up an appointment with a licensed agent in your area or call us at 833-438-3676.
Read Also: Texas Healthy Women’s Medicaid Coverage
Exciting New Dental Benefits For You
Date:01/16/19
Starting February 1, 2019, our members ages 21 and older will get up to $500 per year in dental benefits, including:
- Dental exams and cleanings
- One whole mouth set of x-rays
- Fillings
- Simple tooth extractions
And you will leave your appointments with a new toothbrush, toothpaste and floss so you can keep your smile healthy at home!
The Long Path To Medicaid Expansion
On November 21, 2015, Democrat John Bel Edwards won the runoff gubernatorial election in Louisiana. Edwards supported Medicaid expansion as called for in the ACA, and his win immediately made Medicaid expansion much more likely in Louisiana.
Former Governor Bobby Jindal was emphatically opposed to Medicaid expansion, but was not eligible to run in the 2015 gubernatorial race due to term limits. There was a primary election in October 2015, but none of the four candidates received a majority of the vote. So a runoff election was scheduled for November 21, 2015, with voters deciding between the two candidates who garnered the most votes in the first election .
All four of the primary candidates had previously expressed at least some degree of willingness to accept federal funds to expand Medicaid, although all but Edwards had called for using a section 1115 waiver to craft Medicaid expansion in a state-specific way. Edwards support for Medicaid expansion was unequivocal.
In addition, lawmakers in Louisiana passed House Concurrent Resolution 75 in June 2015, which helped pave the way for the expansion of Medicaid. HCR75 allowed hospitals to implement a fee that would generate the revenue needed to pay the states portion of the cost of expanding Medicaid . HCR75 gave Edwards until April 1, 2016 to propose a plan to expand Medicaid, but he wasted no time in issuing the Medicaid expansion executive order the day after taking office.
Recommended Reading: Can You Enroll In Medicaid Anytime
Doctor Visits & Screenings
Preventative care visits are covered by Louisiana Healthcare Connections. This means visiting the doctor for a regular check-up, rather than waiting until you are sick.
Louisiana Healthcare Connections covers an annual physical for adults.
Regular child check-ups are also covered for those under the age of 21. These doctor visits should occur at the below ages. Children also need a blood lead test at 12 and 24 months of age. We cover this. After that, if they are high risk, they need the blood lead test each year age 3 to 6.
- Birth or neonatal exam
Louisiana Medicaid Expansion Update
On January 12, 2016, then-Governor John Bel Edwards signed his first executive order to start the process of Medicaid expansion in Louisiana.
Prior to June 1, 2016, Medicaid eligibility for adults in Louisiana was unchanged from 2013, and childless adults were ineligible for coverage, regardless of how low their incomes were.
Expansion has made Medicaid available to more than 400,000 people living in Louisiana who did not previously qualify for full Medicaid coverage and could not afford to buy private health insurance.
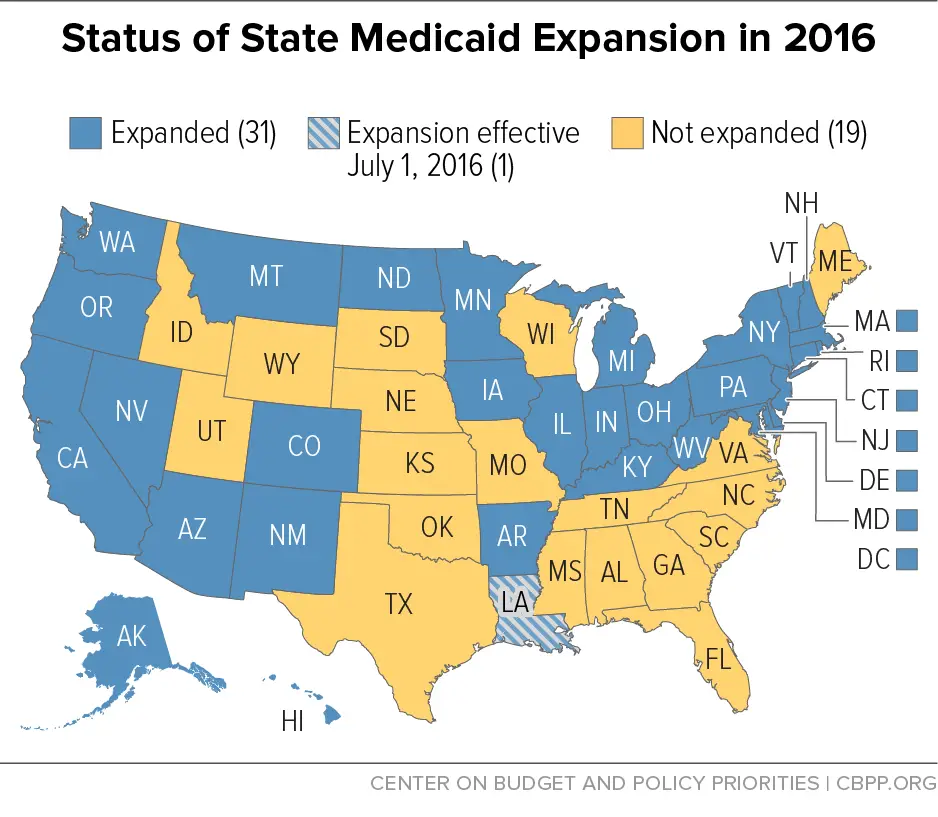
Louisiana Medicaid expansion took effect June 1, 2016.
Healthy Louisiana is Louisianas name for its new expanded Medicaid program.
Eligibility and enrollment system updates allow for real-time eligibility determinations based on state and federal data.
Work requirement was considered by lawmakers in 2018 but did not pass.
Also Check: How To Qualify For Kansas Medicaid
Will Louisiana Medicaid Cover Dental Care And Orthodontics
Medicaid is a federal program administered by states to ensure low-income Americans can access health care coverage. To qualify, you must have limited income and resources. In compliance with federal rules, each state determines the financial threshold and other eligibility requirements applicable to state residents. People enrolled in Medicaid include:
- Adults with limited means
- Children
Dental care for children with Medicaid
The Childrens Health Insurance Program is a low-cost health insurance program for children in families where the household income exceeds the level that would qualify them for Medicaid but falls below the level needed to purchase private insurance. CHIP is available in every state and partners with the Medicaid program.
Every state must provide access to dental coverage for every child covered by Medicaid and CHIP. All children enrolled in Medicaid get the comprehensive dental benefit known as Early and Periodic Screening, Diagnostic and Treatment . At minimum, states must provide dental services that include:
- Pain and infection relief
- Dental health maintenance
Orthodontics
Orthodontia falls under restorative services. However, coverage applies only if the braces are medically necessary. States can decline coverage for braces requested for cosmetic reasons.
Dual-eligibles
- Qualified Disabled and Working Individuals
Dental care for adults with Medicaid
Who Among The Four Eligibility Groups Would Benefit From Our Instruction To Apply For Ssi
Anyone who is 65 or older or have a disability with income below $750. There could even be some in the special long-term care income limit program who have income less than $750 and never applied for SSI, or have resources over the SSI limit. Medicaid also has provisions for spousal impoverishment considerations.
Recommended Reading: Does Medicaid Cover Gastric Bypass In Colorado
What If I Have Questions About My Healthy Louisiana Plan
If you have questions about your Healthy Louisiana plan, contact your plans customer service department.
- Aetna Better Health 1-855-242-0802 TTY: 711 Available 24 hours a day, 7 days a week
- AmeriHealth Caritas 1-888-756-0004 Available 24 hours a day, 7 days a week.
- Healthy Blue 1-844-521-6941 Available Monday Friday, 7:00 a.m. – 7:00 p.m.
- Louisiana Healthcare Connections 1-866-595-8133 Available Monday Friday, 7:00 a.m. – 7:00 p.m.
- UnitedHealthcare Community 1-866-675-1607 Available Monday Friday, 7:00 a.m. 7:00 p.m
Medicaid / Healthy Louisiana
Louisiana Receives Approval for Unique Strategy to Enroll SNAP Beneficiaries in Expanded Medicaid CoverageWednesday, June 1, 2016 Contact: Samantha Faulkner 225.342.9010,
Baton Rouge, La. Yesterday, the U.S. Department of Health and Human Services announced that Louisiana has received final federal approval to enroll residents in Medicaid using data from the Supplemental Nutrition Assistance Program , more commonly known as food stamps. With this approval, Louisiana has become the first state in the country to receive approval to both determine Medicaid income eligibility and enroll people receiving SNAP benefits using this special fast-track enrollment process.
The authority granted by the Centers for Medicare and Medicaid Services allows the state to enroll individuals who are certain to be eligible for Medicaid without the need for a full Medicaid application because the financial eligibility requirements for Medicaid and SNAP are nearly identical and non-financial eligibility requirements are also already met.
Governor John Bel Edwards thanked CMS for expediting the approval of the state plan amendment, the formal request to make a change to the Medicaid program, to allow for the automatic enrollment of SNAP enrollees, as it will allow more people to get health care coverage as soon as July 1.
Questions and Answers
You May Like: Is Amerihealth Caritas Medicaid Or Medicare
What Is Healthy Louisiana
Healthy Louisiana is the way most of Louisiana’s Medicaid recipients receive health care services. As soon as you or family members are eligible for Medicaid, you need to choose a Healthy Louisiana Health Plan to manage your or your family members health care. If you do not choose a health plan, Healthy Louisiana will choose one for you or your family. Compare health plans to find the best plan for you. If you have questions, call Healthy Louisiana at 1-855-229-6848 .
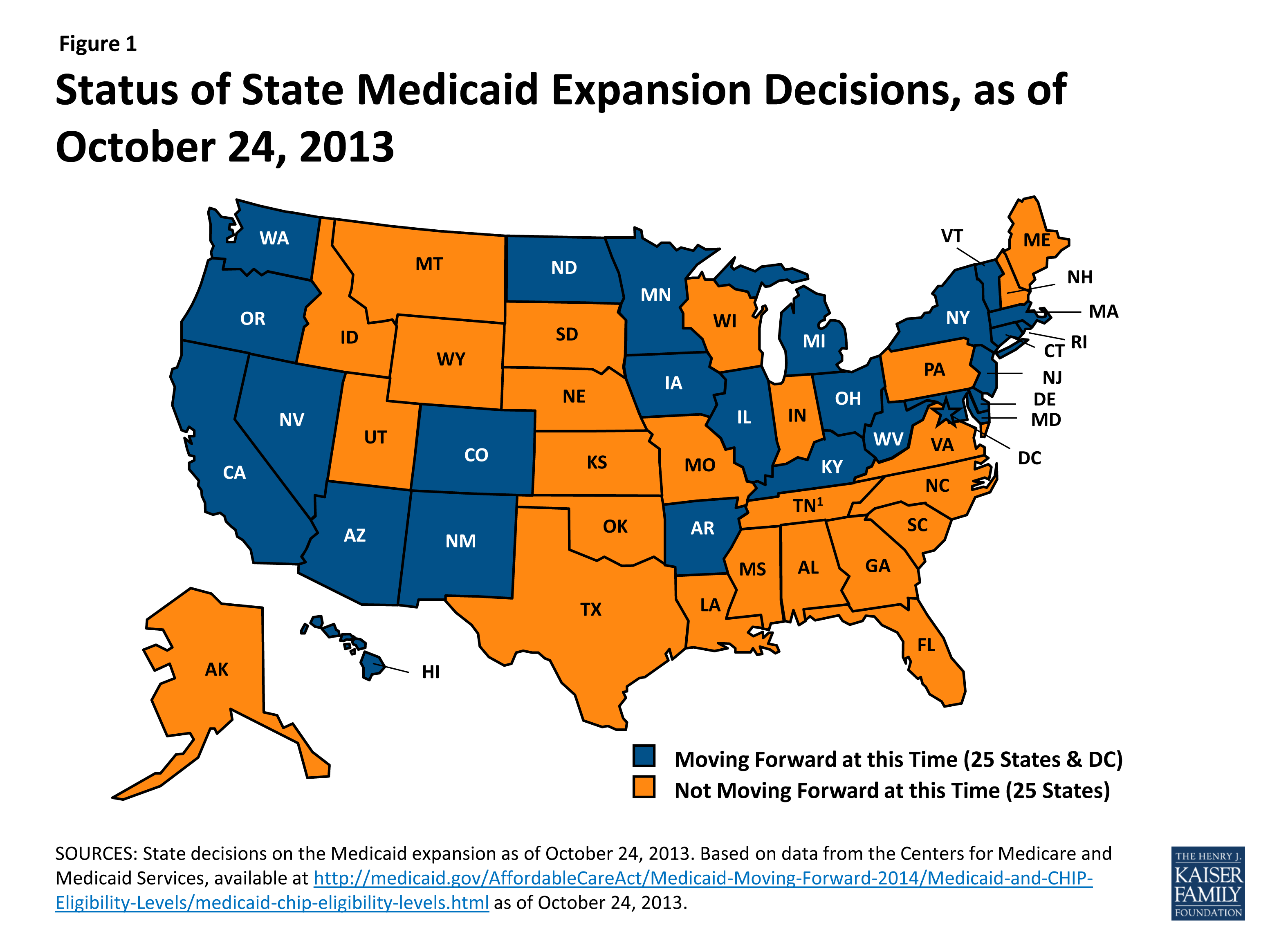
Louisiana Has Accepted Federal Medicaid Expansion
- 1,825,285 Number of Louisianans covered by Medicaid/CHIP as of February 2022
- 732,243 Number of Louisianans covered under Medicaid expansion as of May 2022
- 801,299 Increase in the number of Louisianans covered by Medicaid/CHIP fall 2013 to January 2022
- 50% Reduction in the uninsured rate from 2010 to 2019
- 79% Increase in total Medicaid/CHIP enrollment in Louisiana since late 2013
Recommended Reading: Does Medicaid Pay For Prescription Glasses
Which States Have Limited Adult Dental Coverage
When Medicaid has limited coverage for dental, this usually means one of two things. Either there is a financial cap to the dental care you can have covered, or there is a fixed list of services that will be covered.
If it is a financial cap, the range is usually somewhere between $500 to $1000. Once that amount is met, dental wont be covered unless it is an emergency.
If it is a fixed list, your Medicaid dental benefits will typically include preventative care such as cleanings and restorative care such as fillings, as well as emergency care.
States with limited adult dental care:
- Arkansas
- Washington
- Wisconsin
Something that is not typically covered even in comprehensive plans is adult orthodontic care or braces. If this is something that you require, you may need to pay out-of-pocket. Luckily, this is not something that would be an emergency, so you will still have all the care that you need to maintain good dental health.
Data Variables And Covariates
We used the electronic medical records, Epic and Cerner , to obtain information on patients who completed a UC appointment, PC appointment, or ED visit. Data related to the encounter included date of clinic appointment or date of ED visit. International Classification of Diseases 9/10 codes were abstracted for ED discharge diagnoses. Visits from patients without a Louisiana address were excluded from the analysis.
ED visits for which ICD-9 or ICD-10 codes were available were classified according to the NYU algorithm. This algorithm is based on the probability of each ICD-9 or ICD-10 code falling into 2 categories: emergent or nonemergent. Following Ballard et al, if the added probability of a nonemergent visit and PC-treatable visit was > 50%, the visit was classified as nonemergent. If the sum of the preventable emergency probability and the nonpreventable probability was > 50%, the visit was classified as emergent. Visits that had equal probability of being classified as nonemergent and emergent, those that were classified into the remaining categories , and those that did not have an ICD-9/10 code were excluded from the analysis.
Don’t Miss: Does Medicaid Work Out Of State
Does Louisiana Medicaid Cover Braces
Good oral health involves the usual brushing and flossing, but it may also require corrective procedures in order to reduce the potential for structural problems. For some people, including those in Louisiana, structural concerns in the mouth are a matter of cosmetics, but for others, these issues can lead to problems chewing food, the development of pain and the worsening of tooth decay and gum disease. Ultimately, dental health concerns may go on to severely impact other parts of the body, including the heart, liver and lungs. While there are plenty of surgical procedures available to address structural dental problems, one of the most common first lines of defense is to fit a patient with braces.
In most cases, braces will be ordered for a dental patient who is still young and has a changing and developing bone structure. Addressing oral health concerns early provides a high likelihood of success as opposed to using braces to correct dental problems in adults. Unfortunately, braces are often expensive and may need to be adjusted over the course of months or even years. This makes it difficult for many low-income families to afford however, Medicaid may pay for dental treatment with braces in Louisiana.
Does Louisiana Medicaid Cover Braces?
Are Children Covered for Braces Under Louisiana Medicaid?
Are All Types of Braces Covered by Medicaid in Louisiana?
Related articles:
Members Age 21 And Over
Members age 21 and over get up to $750 in dental benefits per calendar year.
Covered dental services include:
- Simple tooth extractions
- Deep cleaning and plaque removal
And you will leave your appointment with a new toothbrush, toothpaste and floss so you can keep your smile healthy at home.
To find an in-network dental provider in your area, use our Find a Provider tool. Or call Member Services at 1-866-595-8133 , Monday Friday, 7 a.m. to 7p.m.
Also Check: How To Obtain Medicaid In Florida
Dental Vision And Hearing Care
We help you keep your smile, sight and hearing at their best. Benefits include:
- Dental. Covered cleanings, checkups and dental work are provided by MCNA Dental for members under the age of 21. We also offer coverage for adults.
- Vision. Exams and eyeglasses or an allowance for lenses are covered for members under the age of 21. We also offer coverage for adults.
- Hearing. Tests, exams and hearing aids for members to age 21.
Get the medical care and equipment you need to live safely at home. Benefits may include:
- Equipment and Supplies. In-home medical and safety equipment are covered for medically necessary equipment.
- Home Health Care. Medical and personal care at home, if necessary.
Recommended Reading: Does Kelsey Seybold Accept Medicaid
What Is The Maximum Income For Medicaid In Louisiana
The income limits for Louisiana Medicaid vary depending on whether the applicant is a child, pregnant woman, parent of a minor child, childless non-elderly adult, or aged/blind/disabled. For the groups that qualify based on income alone, eligibility is determined as a percentage of the federal poverty level . As of 2021, Louisianas Medicaid eligibility standards are:
- Children ages 0-18: 212% of the federal poverty level
- Children with family income between 212% and 250% of FPL are eligible for the Louisiana Childrens Health Insurance Program
Don’t Miss: Is Oregon Health Plan Medicaid
Who Would Be Impacted By The Loss Of These Eligibility Categories
People who are impacted get their Medicaid from four eligibility categories:
- Provisional Medicaid covers individuals who are either age 65 and older or disabled with monthly income less than $750.
- The Medically Needy and Medically Needy Spend Down Programs cover some individuals whose medical expenses exceed their income.
The Long Term Care Special Income Level program covers individuals who are aged, blind or disabled who qualify for institutional level of care because of their medical needs and who have monthly income between $750 and $2,250.
