How To Find Texas Family Doctors Near Me That Accept Medicaid
Start by visiting the TMHP website. If you land on a page that looks like the one below you are in the right place.
As you can see you can search for doctors according to:
- Health Plan Medicaid has multiple different plans. Some are for adults, some for children, others for pregnant women, or those with a disability. If you are unsure which coverage you have, simply check your insurance card or refer to this section in the article that explains what each Medicaid health plan covers.
- Provider Type This is the section where you can choose a mental health provider, primary care physician, or specialist doctor.
- Zip Code Enter the zip code where you live or work to find a Medicaid doctor near you.
- Distance From Zip Code If you want a doctor close to you select 5 miles away. That being said, if you do have adequate transportation you can broaden your search and this will give you access to more primary care doctors in Texas who take Medicaid insurance.
I Have Breast Or Cervical Cancer And I Don’t Have Health Insurance
Medicaid for Breast and Cervical Cancer provides health care services for low-income women who have breast or cervical cancer.
Services include cancer treatment, lab tests, hospital care and service coordination provided by a nurse.
You must contact a Breast and Cervical Cancer Services provider who can help you apply.
How Do I Make Referrals To Other Providers And Programs
Primary care referrals
If a woman covered by Healthy Texas Women does not want to pay out-of-pocket for services not covered by the program, providers must refer the woman to another physician or clinic. Providers should make referrals when health issues are identified and necessary services related to those health issues are not covered under the program.Texas Health and Human Services prefers referrals to local indigent care services, but 2-1-1 can assist with locating other primary care providers, if needed.
Breast and cervical cancer screening
The Breast and Cervical Cancer Services program offers breast and cervical cancer screening and diagnostic services and cervical dysplasia treatment throughout Texas for free or at low cost to eligible women.
You May Like: What Benefits Do You Get With Medicaid
You May Like: Oral Surgeons Columbus Ohio Accept Medicaid
How To Find Fqhcs That Accept Medicaid In Texas
If you are wondering are there clinics that accept Medicaid near me the answer is yes. These are called FQHC or federally qualified health centers.
An FQHC is a clinic that receives federal funding to provide healthcare to low income neighborhoods. In order to receive federal funding, these clinics have to accept coverages like Medicaid and Medicare.
To find these low cost clinics that take Medicaid health insurance you can use the HRSA Find a Health Center tool. Once there type your zip code in the search and you will be presented with a listing and map of Texas clinics near you that most likely accept Medicaid.
Who Can Provide Healthy Texas Women Services

Providers who meet certain criteria might qualify to provide services. These criteria include:
- Must deliver the types of services available through the program.
- Have completed the Medicaid enrollment process through the Texas Medicaid & Healthcare Partnership.
- Can certify that they do not perform or promote elective abortions or affiliate with an entity that performs or promotes elective abortions in accordance with the Healthy Texas Women program rules located in the Texas Administrative Code Title 1, Part 15, Chapter 382, Subchapter A, §§382.1 382.29.
Visit the Healthy Texas Women page on the Texas Medicaid & Healthcare Partnership website to learn more about the requirements and find links to the certification documents.
Read Also: Dentists In Grand Island Ne That Accept Medicaid
Philosophical Resistance To Medicaid
In April 2021, Toni Rose, a Democratic state representative from Dallas, went before the 150-member Texas House to lay out her bill to expand Medicaid to a full year after pregnancy. Within three minutes, the bill passed the chamber with bipartisan support. Some lawmakers applauded its passage.
The ease with which the measure sailed through the House inspired advocates to hope that the 12 months of coverage stood a chance to become law in Texas. Of the 14 members of the public who testified on the bill during a House committee hearing, not one spoke against the measure. And not a single representative publicly raised concerns about the bill before it eventually passed by a 121-24 vote.
More than a month later, on the same day that Abbott signed into law the Texas Heartbeat Act, which banned most abortions after about six weeks of pregnancy, the state Senate took a different approach.
During a hearing that month, Lois Kolkhorst, the Senate sponsor for the postpartum Medicaid bill, ticked off a list of states that had applied to the federal government to extend coverage for new parents to 12 months or that were considering passing legislation to do so.
Certainly, Texas would be on the cutting edge of this if we were to pass this bill in any form, extending past the 60 days, Kolkhorst said.
After the May hearing, Kolkhorst accepted an amendment by Sen. Dawn Buckingham, a Republican from Austin and an eye surgeon, that slashed the Houses proposed postpartum coverage in half.
Different Types Of Medicaid Insurance Plans
Below is a listing of Medicaid insurance plans. As we mentioned before, Medicaid has several insurance coverages. The coverage that you qualify for will depend on factors like your age, whether you have a disability, and if you are pregnant.
- STAR Most people who have Medicaid in Texas get their coverage through the STAR managed care program. STAR covers low-income children, pregnant women, and families. STAR members get their services through the private health insurance companies who manage their care.
- STAR Plus This is a Texas Medicaid managed care program that offers treatment to adults 65 and older or adults with disabilities.
- STAR Kids Children and young adults 20 years or younger who have disabilities receive care under the Texas Medicaid STAR Kids program.
- Traditional Medicaid
- Healthy Texas Women This coverage offers help paying for well womens services like mammograms, breast, and cervical cancer screenings.
You can learn more about Texas Medicaid managed care programs by visiting the Texas Health and Human Services website.
Recommended Reading: Fertility Doctor That Takes Medicaid
Examples Of Proof We Need
Proof showing how much money you receive:
- Paycheck stub or copy of a check from the last 60 days.
- A letter from an employer.
- Court papers, divorce decree or separation agreement that show you get alimony
- Unemployment benefit award letter or pay stubs.
- Supplemental Security Income award letter or pay stubs.
Proof showing how much you pay:
Court papers, divorce decree or separation agreement that shows how much you pay for alimony. Proof showing your citizenship and identity:
- A U.S. passport.
- A certificate of naturalization.
- A certificate of U.S. citizenship.
- The three items above prove both citizenship and identity. If you dont have one of these documents, you will need to show two documents, one from each list below:
|
Proof of Citizenship |
|
|---|---|
|
Affidavit from 2 adults establishing the date and place of birth in the United States |
An example of an item that shows proof of immigration status is an alien registration card or document from the Bureau for Citizenship and Immigration Services .
You have to prove citizenship, immigration and identity only one time. You dont need to send these items again if you reapply.
Texas Incentives For Physicians And Professional Services
TIPPS is a value-based directed payment program for certain physician groups providing health care services to children and adults enrolled in the STAR, STAR+PLUS and STAR Kids Medicaid programs. Eligible physician groups include health-related institutions, indirect medical education physician groups affiliated with hospitals and other physician groups.
CMS approved TIPPS on March 25, 2022. The program must be approved annually by CMS.
Read Also: Best Medicaid Plans In South Carolina
Performance And Reporting Requirement Adjustments Due To Covid
QIPP Y3 and Y4 were impacted by the COVID-19 Public Health Emergency . The CMS waived certain reporting requirements for nursing facilities effective March 1, 2020, including timeframe requirements for Minimum Data Set assessments and transmission.
- On June 9, 2020 HHSC waived the performance requirements connected to all MDS quality measures effective March 1, 2020 to August 31, 2020. To help relieve the administrative burden on facilities, reporting requirement for Component One-Submission of monthly Quality Assurance and Performance Improvement Validation reports was also waived.
- On December 23, 2020, HHSC extended the waiver effective September 1, 2020, to the rest of fiscal year 2021.
- CMS reinstated MDS reporting requirements effective May 10, 2021. HHSC reinstated performance requirements for the fourth quarter of QIPP Y4, spanning June 1, 2021 to August 31, 2021.
During both waivers, while HHSC suspended the reporting requirements for Component One, NSGOs were required to continue holding monthly Quality Assurance and Performance Improvement meetings. If a facility was randomly selected for a Quality Assurance review, HHSC reserved the rights to require supporting documentation for all monthly meetings.
How Do I Know If An Applicant I Have Treated Is Enrolled In Healthy Texas Women And Her Claim Will Be Paid
To see if a woman is enrolled in the program:
- Check in the Texas Medicaid Provider section of the Texas Medicaid & Healthcare Partnership website. .
Providers should make sure that a woman is enrolled in the program before billing. Claims received before enrollment will be denied, but providers can resubmit claims once a woman is enrolled. Providers have 95 calendar days from service delivery to bill the program.
You May Like: Keystone First Medicaid Phone Number
Where Do I Get My Birth Control
You can get your birth control at a clinic or doctor’s office that works with the Healthy Texas Women program. If your doctor gives you a prescription, you can fill it for free at a drug store if you show the Your Texas Benefits ID card.
Find a Pharmacy – If you need to find a drug store that serves Healthy Texas Women members, use this search feature.
Accessing Care: Medicaid And Chip Members
To choose a doctor or Primary Care Provider , call Superior Member Services. They can give you the name, address and phone number of a doctor or specialist. They can also help you get a providers:
- Professional qualifications
- Demographics
More information on how to choose a PCP can be found in your member handbook.
To find out which nursing facilities are in Superiors network, you can call us at 1-877-277-9772 or search our Find a Provider online tool.
If you are a STAR Kids or STAR+PLUS member and are dual eligible, Medicare pays your doctor. That means you do not need to choose a PCP in STAR Kids or STAR+PLUS. You can keep seeing the Medicare doctor you have been seeing for your health care.
You May Like: Medicaid For Non Us Citizens
Read Also: How To Get Medicaid For Mental Illness
Finding Specialty Doctors That Take Texas Medicaid
To find specialists that take Medicaid in Texas you will need to use the Advance Search Filters. After clicking Advanced Search Filters you will then need to select Provider Options. This will give you the chance to choose a specialist that accepts Medicaid.
The Medicaid specialist that you will find include doctors like:
- Pediatricians
- Internal Medicine
- Physician Assistants and more
If there is a specific doctor that you would like you can also search for them by name on this screen.
Once you have selected a zip code and type of provider, you will see a list of Medicaid doctors that accept your insurance coverage. The listing will offer the Medicaid doctors name, office address, and phone number.
W111 Type Of Assistance 41 Ma Healthy Texas Women
Revision 21-3 Effective July 1, 2021
To be eligible for HTW, applicants must:
- be female, 15 through 44
- a parent or legal guardian must apply on behalf of applicants 15-17
Notes:
- A legal guardian is a person appointed by a judge to care for a child younger than 18.
- Deny applications received for minors, 15-17, without a parent or legal guardian signature if they are not eligible for full coverage Medicaid or CHIP. Use the denial reason, Denied 15-17 without parent or legal guardians signature.”
Related Policy
Revision 21-3 Effective July 1, 2021
Applicants can use any Texas Works medical benefits application form to apply for HTW.
Related Policy
Application Requests and Submissions, A-113
Also Check: United Healthcare Medicaid Dental Plan
American Disabilities Act Notice
In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
Does Enrollment In Healthy Texas Women Affect Other Texas Health And Human Services Benefits
A woman’s enrollment in Healthy Texas Women does not make a household ineligible for other program benefits such as Medicaid, TANF or SNAP. But the information reported when applying for Healthy Texas Women might affect the household’s other benefits if it’s different than what was previously reported for other programs.
Read Also: Medicaid Indiana Provider Phone Number
Can Women Who Have Medicaid For Pregnant Women Transition To Healthy Texas Women To Avoid A Gap In Coverage
Yes. At the end of a womans Medicaid for Pregnant Women coverage, she will be automatically enrolled in Healthy Texas Women. The woman will get a notification letter in the mail about her auto-enrollment into Healthy Texas Women and she will have the option to opt out of the program. To be auto-enrolled, a woman must:
- Be 1844 years of age
- Not be receiving active third-party resources at the time of auto-enrollment
- Be unable to get any other Medicaid or CHIP programs
If a woman cannot be auto-enrolled in Healthy Texas Women, she can apply for the program in the last month she is eligible for pregnancy coverage. If she meets the eligibility criteria, her Healthy Texas Women coverage will begin the first day of the month following the end of her Medicaid or CHIP Perinatal coverage.
Promoting Continuity Of Care
When families are faced with unemployment or loss of employer-based health coverage, they turn to Texas Medicaid or another health-care program to provide the health care they and their loved ones need. Providers who enroll as Texas Medicaid and other state health-care programs providers can continue to see existing patients during those times of change.
Providers may also render service to families with mixed coverage .
Read Also: Does Medicaid Cover Copays From Primary Insurance
You May Like: New York Department Of Social Services Medicaid
How Does Texas Health And Human Services Protect A Womans Confidentiality
The application allows women to list a separate mailing address where all correspondence can be sent. The woman must list her home street address on the application but she can list a P.O. box as a mailing address.If the woman has private health insurance coverage, providers do not bill the private insurance first because this could risk her confidentiality.
What Information And Documents Need To Be Submitted With An Application
Documentation is needed for:
- Social Security number
- Household expenses
Note: Documentation of household expenses is not required, but Texas Health and Human Services recommends that women send the following, if available:
- Expenses for dependent care .
- Expenses for child support paid by the household .
Recommended Reading: Does Medicaid Pay For Assisted Living In Washington State
Please Tell Us A Little More About You
We appreciate you taking the time to help Americas Health Rankings better understand our audiences. Your feedback will allow us to optimize our website and provide you with additional resources in the future. Thank you.
Please select one option which best describes your profession or field of expertise
Can Women With Health Insurance Coverage Enroll
Women enrolled in Medicaid, CHIP or Medicare Part A or B are not able to get Healthy Texas Women. A woman who has private health insurance is not eligible for the program unless:
- her private insurance does not cover family planning services or
- filing a claim on her health insurance would cause physical, emotional or other harm from her spouse, parents or other person.
You May Like: Dentist In Great Falls Mt That Take Medicaid
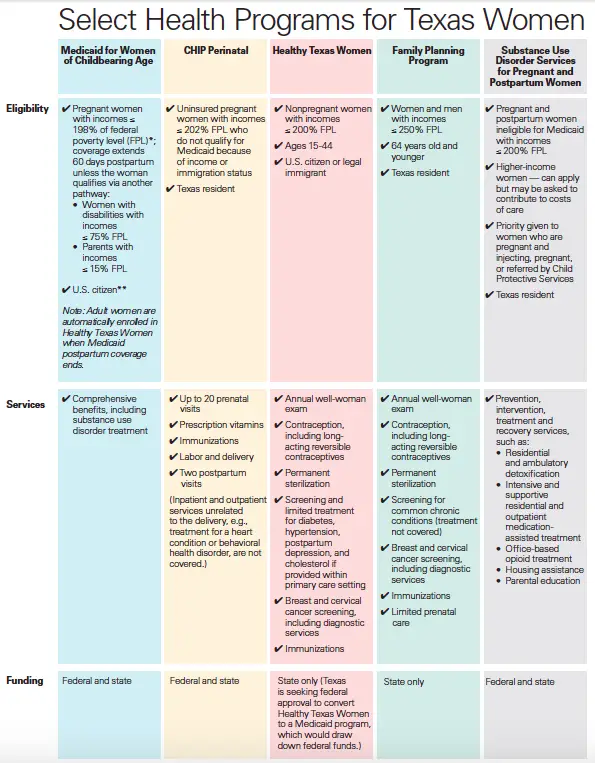
Medicaid For Pregnant Women & Chip Perinatal
Need Services?
SNAP, TANF and Lone Star Card Information
Pregnant women without health insurance might be able to get free health coverage during their pregnancy through Medicaid for Pregnant Women or the CHIP Perinatal program.
Medicaid provides health coverage to low-income pregnant women during pregnancy and up to two months after the birth of the baby.
CHIP Perinatal provides similar coverage for women who cant get Medicaid and dont have health insurance.
To get Medicaid for Pregnant Women or CHIP Perinatal, you must be a Texas resident and a U.S. citizen or qualified non-citizen.
When you apply, well ask about your familys monthly income to see if you can get Medicaid or CHIP Perinatal.
When Does Coverage Start
The enrollment effective date is the first day of the month that Texas Health and Human Services receives the application. For example, if we receive a woman’s application on Jan. 20 and she is determined eligible for the program, her coverage begins Jan. 1. Call 866-993-9972 if you have questions about the enrollment effective date or think there might be an error.
Read Also: Is Neurofeedback Covered By Medicaid
