Q If I Dont Qualify For Medicaid Is There Any Other Help For Me Or My Children
A. Yes. Many organizations in Delaware are dedicated to the principle that health care should never be beyond the reach of those who need it. If you need health care, but do not have insurance coverage, the people at the Delaware HelpLine have a wealth of information about organizations that provide health care at reduced rates for uninsured individuals. Call the Delaware HelpLine toll-free at 1-800-464-HELP from Monday Friday from 8:00 a.m. to 5:00 p.m. The Delaware Helpline service is also available in Spanish. Additional information about the support provided by the Delaware Helpline can also be found by visiting www.delawarehelpline.org.
For example, you may qualify to receive discounted medical services through the Community Healthcare Access Program . CHAP helps connect uninsured individuals with affordable health care from primary care doctors, medical specialists, and other health providers including prescription programs, laboratory and radiology services. To find out more about this program, visit the website for the Community Healthcare Access Program, or call 1-800-996-9969 for eligibility guidelines.
You can read about CHAP and other healthcare resources for uninsured individuals in the Delaware Healthcare Resource Guide. This guide is also available in Spanish: Guía de Recursos de Salud.
Under 18:
Over 65:
Coverage Changes By Income
Table 3 shows the changes in nongroup and Medicaid coverage by income.
Option 1 extends marketplace coverage to people earning less than the poverty level but does not improve premium and cost-sharing subsidies. It brings new nongroup or Medicaid coverage to an additional 3.1 million individuals with incomes below 138 percent of FPL. There are small increases in coverage at higher incomes, because the expansion of coverage for people below the poverty level positively affects the nongroup market risk pools, causing a small reduction in premiums that attract some additional enrollees.
Option 2 extends new nongroup or Medicaid coverage to 3.5 million people below 138 percent of FPL in nonexpansion states. This reflects the extension of coverage to people below the poverty level as well as the improvement in premium subsidies. The improvement in subsidies at higher income levels results in an increase in new nongroup or Medicaid coverage of 221,000 between 138 percent and 200 percent of FPL, 809,000 between 200 percent and 400 percent of FPL, and 475,000 above 400 percent of FPL. This option has large coverage gains both because of the expansion of subsidized coverage below the poverty level and the increased generosity of subsidies above 138 percent of FPL.
Prior Medicaid expansions have led to a modest increase in enrollment among those already eligible. These results show slightly higher Medicaid and CHIP coverage above 138 percent of FPL for the same reason.
Q Can I Have Both Medicaid And Medicare At The Same Time
A. It depends. If you receive Supplemental Security Income from the Social Security Administration, you are automatically eligible for Medicaid and often receive Medicare as well. If you receive both Medicaid and Medicare, Medicaid will pay your Medicare premium, co-payments and deductibles. If you have both Medicare and Medicaid, you should show both cards to your medical care provider each time you receive services. Resources for Those Who Have Medicare and Full-Benefit Medicaid
Don’t Miss: Psychiatrist That Accept Medicaid In Houston Tx
People Who Have Both Medicare & Medicaid
People who have both Medicare and full Medicaid coverage are dually eligible. Medicare pays first when youre a dual eligible and you get Medicare-covered services. Medicaid pays last, after Medicare and any other health insurance you have.
You can still pick how you want to get your Medicare coverage: Original Medicare or Medicare Advantage . Check your Medicare coverage options.
If you choose to join a Medicare Advantage Plan, there are special plans for dual eligibles that make it easier for you to get the services you need, include Medicare coverage , and may also cost less, like:
- Special Needs Plans
- Medicare-Medicaid Plans
- Program of All-Inclusive Care for the Elderly plans can help certain people get care outside of a nursing home
Please Answer A Few Questions To Help Us Determine Your Eligibility
Medicaid is a health insurance program for low-income individuals that is operated by the states, according to guidelines established by the federal government.
The federal government requires all states to offer Medicaid coverage to some groups of people and allows the states to cover certain additional groups. One group required to be covered by Medicaid is disabled individuals with low incomes. But states are allowed to have eligibility requirements, particularly regarding income and asset limits, that are different from the SSI disability program.
Whether SSI recipients are automatically eligible for and enrolled in Medicaid depends on the state that a recipient lives in.
Read Also: Anthem Medicaid Ky Dental Providers
How Effective Is Medicaid
Medicaid is very effective in providing health insurance coverage to the most vulnerable. Since the ACAs major coverage expansions took effect in 2014, Medicaid has helped to reduce the number of uninsured from 45 million to 29 million. If Medicaid did not exist, most of the tens of millions of Medicaid enrollees would be uninsured. This is because private health insurance is generally not an option for Medicaid beneficiaries: many low-income workers do not have access to coverage for themselves and their families through their jobs and cannot afford to purchase coverage in the individual market. The creation of Medicaid, subsequent expansions of Medicaid coverage to children and pregnant women in the 1980s and 1990s, and the most recent expansion of Medicaid coverage to low-income adults under the ACA all have led to significant drops in the share of Americans without health insurance coverage.
Medicaid is also effective in improving access to care, in supporting financial stability among low-income families, and in improving health outcomes. Some of the clearest evidence comes from the ACA expansion of Medicaid coverage to low-income adults, which provides a recent natural experiment, letting researchers compare outcomes in states that did and did not adopt the expansion.
Does My State Guarantee Medicaid Eligibility For Ssi Recipients
Most states automatically grant Medicaid when you get approved for SSI based on disability. In fact, most states let the Social Security Administration handle Medicaid enrollment for SSI recipients when they’re approved for SSI. Individuals in those states will receive information about their Medicaid enrollment along with the SSI award letter that they get when they’re approved for SSI.
You May Like: Medicaid Blue Cross Blue Shield Nevada
What Is A Dual Special Needs Plan
A Dual Special Needs Plan is a type of health insurance plan for people who have both Medicaid and Medicare. These people are dual-eligible because theyre eligible to receive Medicaid benefits as well as Medicare benefits.
Dual Special Needs Plans provide extra help to those who need it. That may be because of income, disabilities, age and/or health conditions. A Dual Special Needs Plan works together with your Medicaid health plan. Youll keep all your Medicaid benefits. Most dual health plans also give you more benefits and features than you get with Original Medicare. All with as low as a $0 plan premium. Learn more about dual health insurance plan benefits.
See UnitedHealthcare plans in your area.
Dual-eligible or Medicaid plan benefits can change depending on where you live. Search using your ZIP code to find the best plan to meet your health care needs.
Were here to help
Contact us at:
Were here to help
Contact us at:8 a.m. to 8 p.m. local time, 7 days a week.
Still have questions
Were here to help
Contact us at:
Were here to help
Contact us at:8 a.m. to 8 p.m. local time, 7 days a week.
Looking for the federal governments Medicaid website? Look here at Medicaid.gov.
If Your Income Is Low And Your State Hasnt Expanded Medicaid
If your state hasnt expanded Medicaid, your income is below the federal poverty level, and you don’t qualify for Medicaid under your state’s current rules, you wont qualify for either health insurance savings program: Medicaid coverage or savings on a private health plan bought through the Marketplace.
- Find out why
-
- When the health care law was passed, it required states to provide Medicaid coverage for all adults 18 to 65 with incomes up to 133% of the federal poverty level, regardless of their age, family status, or health.
- The law also provides premium tax credits for people with incomes between 100% and 400% of the federal poverty level to buy private insurance plans in the Health Insurance Marketplace®.
- The U.S. Supreme Court later ruled that the Medicaid expansion is voluntary with states. As a result, some states havent expanded their Medicaid programs.
- Adults in those states with incomes below 100% of the federal poverty level, and who dont qualify for Medicaid based on disability, age, or other factors, fall into a gap.
- Their incomes are too high to qualify for Medicaid in their states.
- Their incomes are below the range the law set for savings on a Marketplace insurance plan.
-
States are continuing to make coverage decisions. They could expand Medicaid in the future.
Don’t Miss: Breast Reduction Doctors That Accept Medicaid
Expansion Under The Affordable Care Act
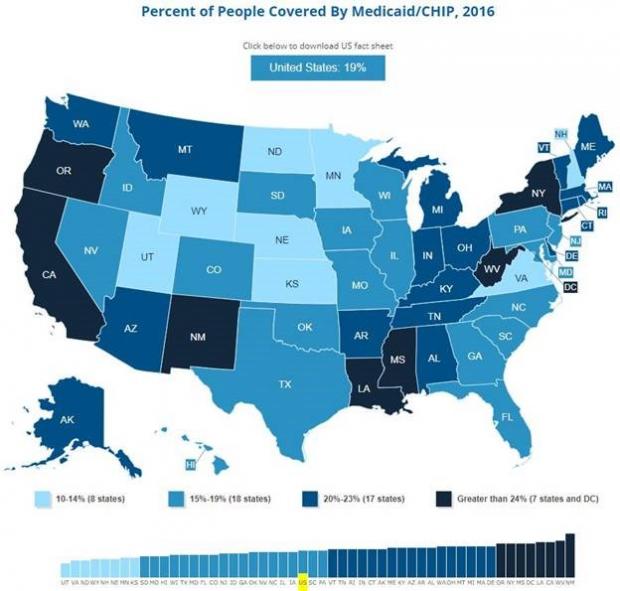
As of March 2022, 38 states and the District of Columbia have accepted the Affordable Care Act Medicaid extension 12 states have not. Among adults aged 18 to 64, states that expanded Medicaid had an uninsured rate of 7.3% in the first quarter of 2016, while non-expansion states had a 14.1% uninsured rate. Following a 2012 Supreme Court ruling, which held that states would not lose Medicaid funding if they did not expand Medicaid under ACA, several states rejected the option. Over half the national uninsured population lives in those states.
The Centers for Medicare and Medicaid Services estimated that the cost of expansion was $6,366 per person for 2015, about 49 percent above previous estimates. An estimated 9 to 10 million people had gained Medicaid coverage, mostly low-income adults. The Kaiser Family Foundation estimated in October 2015 that 3.1 million additional people were not covered in states that rejected the Medicaid expansion.
Studies of the impact of Medicaid expansion rejections calculated that up to 6.4 million people would have too much income for Medicaid but not qualify for exchange subsidies. Several states argued that they could not afford the 10% contribution in 2020. Some studies suggested that rejecting the expansion would cost more due to increased spending on uncompensated emergency care that otherwise would have been partially paid for by Medicaid coverage,
Medicaid And Former Foster Youth
For young adults formerly in foster care, there are special provisions. Medicaid is available until age 26 for those who:
- exit foster care at age 18
- were on Medicaid while in foster care
- are not eligible for other Medicaid coverage
No income is counted towards eligibility, and the young adult is eligible even if they have another offer of coverage through an employer. Children who were adopted or placed in guardianship at age 18 are not eligible for Medicaid under the former foster care coverage group.
Don’t Miss: How To Get Medicaid Card Online
Most Medicaid Enrollees Get Care Through Private Managed Care Plans
Over two-thirds of Medicaid beneficiaries are enrolled in private managed care plans that contract with states to provide comprehensive services, and others receive their care in the fee-for-service system . Managed care plans are responsible for ensuring access to Medicaid services through their networks of providers and are at financial risk for their costs. In the past, states limited managed care to children and families, but they are increasingly expanding managed care to individuals with complex needs. Close to half the states now cover long-term services and supports through risk-based managed care arrangements. Most states are engaged in a variety of delivery system and payment reforms to control costs and improve quality including implementation of patient-centered medical homes, better integration of physical and behavioral health care, and development of value-based purchasing approaches that tie Medicaid provider payments to health outcomes and other performance metrics. Community health centers are a key source of primary care, and safety-net hospitals, including public hospitals and academic medical centers, provide a lot of emergency and inpatient hospital care for Medicaid enrollees.
Figure 6: Over two-thirds of all Medicaid beneficiaries receive their care in comprehensive risk-based MCOs.
How Did The Affordable Care Act Change Medicaid
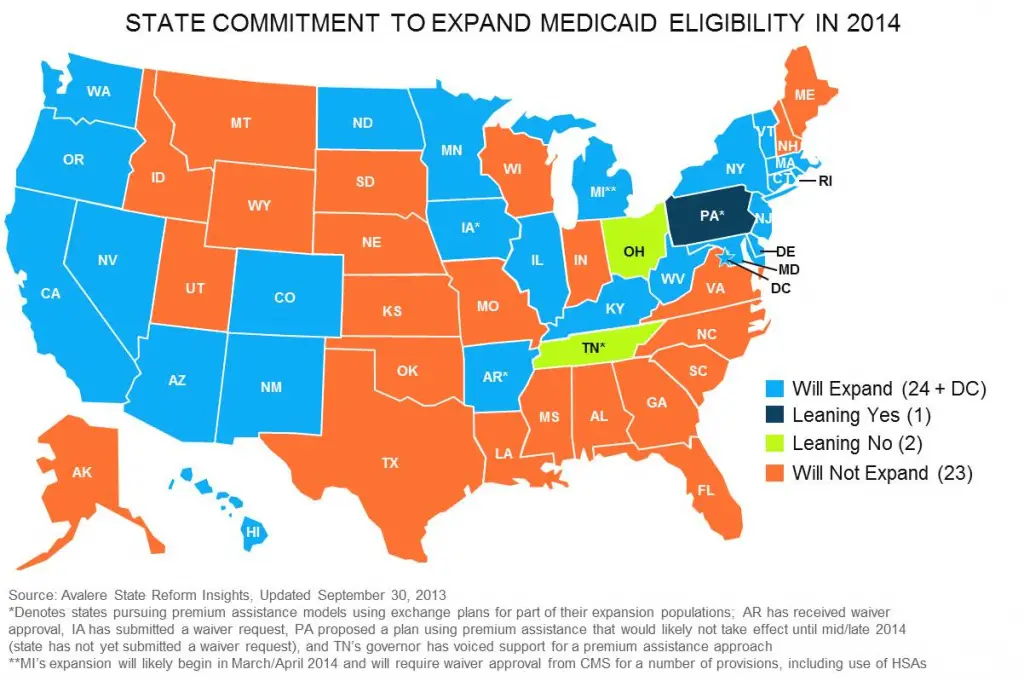
Medicaid plays an even more important role in insuring low-income Americans due to the Affordable Care Act. As noted, the ACA provides coverage for poor and low-income adults by expanding eligibility for Medicaid to 138 percent of the poverty line. As of April 2020, 35 states plus the District of Columbia have implemented the Medicaid expansion to serve poor and low-income adults. By 2029, 14 million more low-income adults will have enrolled in Medicaid and gained access to affordable comprehensive health coverage due to the ACA, CBO estimates.
The expansion is a very good financial deal for states. After picking up all expansion costs for the first three years, the federal government now pays 90 percent of expansion costs on a permanent basis. And by greatly reducing the number of uninsured, the expansion will save states and localities substantial sums on uncompensated care for the uninsured. Some expansion states have also experienced savings in mental health programs, criminal justice systems, and other budget areas.
You May Like: Dentist In Vidalia Ga That Takes Medicaid
What Medicaid Helps Pay For
If you have Medicare and qualify for full Medicaid coverage:
- Your state will pay your Medicare Part B monthly premiums.
- Depending on the level of Medicaid you qualify for, your state might pay for:
- Your share of Medicare costs, like deductibles, coinsurance, and copayments.
- Part A premiums, if you have to pay a premium for that coverage.
A Look At Medicaid Programs In Calfornias Neighboring States
Similarly to California, five states expanded Medicaid access to include low-income adults also. Those states are Illinois, North Dakota, Ohio, Oregon and Pennsylvania. Many of Californias neighboring states also expanded access to their programs, including:
- Oregon: Oregon expanded access to low-income adults but also has programs for normal populations. The state also has medical marijuana and programs to help with substance drug and alcohol abuse.
- Nevada: Nevada expanded access for all households below the 138% FPL threshold.
- Washington: Washington grants access to adults with financial hardships regardless if they have children or other dependents. Income levels vary by household size.
- Arizona: Arizona expanded access to adults whose income levels make them ineligible for other programs, but they must earn less than 133% of the FPL. The program also offers low premiums and coinsurance rates for adults who earn more than 106% of the FPL.
Don’t Miss: Get My Medicaid Id Number
What Services Does Medicaid Cover
Medicaid covers more than 60 percent of all nursing home residents and roughly 50 percent of costs for long-term care services and supports.
Federal rules require state Medicaid programs to cover certain mandatory services, such as hospital and physician care, laboratory and X-ray services, home health services, and nursing facility services for adults. States are also required to provide a more comprehensive set of services, known as the Early and Periodic Screening, Diagnostic, and Treatment benefit, for children under age 21.
States can and all do cover certain additional services as well. All states cover prescription drugs, and most cover other common optional benefits include dental care, vision services, hearing aids, and personal care services for frail seniors and people with disabilities. These services, though considered optional because states are not required to provide them, are critical to meeting the health needs of Medicaid beneficiaries.
About three-quarters of all Medicaid spending on services pays for acute-care services such as hospital care, physician services, and prescription drugs the rest pays for nursing home and other long-term care services and supports. Medicaid covers more than 60 percent of all nursing home residents and roughly 50 percent of costs for long-term care services and supports.
How Much Does Medicaid Cost? How Is It Financed?
The Marginal Cost Of Filling The Gap
The results presented above reflect the effects of joint policies of expanding subsidies and filling the Medicaid coverage gap. An alternative way to analyze this issue is to estimate the cost of filling the gap for those below 100 percent of FPL, building on an existing policy that has previously expanded subsidies. In option 1 above, federal spending for people in the Medicaid gap increases by $16.6 billion as they become eligible for subsidies. However, spending on health grows somewhat less $15.1 billion largely because the cost of premium tax credits falls for people already in the subsidized nongroup market. Premium tax credits are smaller, because the new enrollees have lower expected health costs than the currently insured population, and those lower costs are spread among all participants in the nongroup market, lowering premiums across the board. These lower premiums lead to a small increase in enrollment among those not eligible for premium tax credits.
As shown in Exhibit 5, the 10-year costs of just filling the gap, building on existing subsidies, are $199 billion, $207 billion, and $217 billion, respectively. The cost of increasing the federal match in expansion states increases these amounts to $344 billion, $352 billion, and $362 billion, respectively.
Also Check: Dentist In Newport News Va That Accept Medicaid
Q How Will I Receive My Medical Care
A. In Delaware, Medicaid benefits are provided mainly through a managed care organization, or MCO, under contract with the state. Managed care is an organized way to ensure that people receive the quality medical care they need in the most cost-effective manner. Some Medicaid recipients in Delaware those who also receive Medicare and those in Long Term Care Medicaid programs such as the Nursing Facility program do not receive their medical care through a managed care organization.
DMMA provides a choice of managed care organizations so you can select the MCO plan that is best for you and your family. Delaware contracts with two managed care plans AmeriHealth Caritas and Highmark Health Options.
The Medicaid MCO provides almost all of the care for Medicaid members who join their plan. Prescription and non-emergency medical transportation services are covered directly by Medicaid, not through the MCO. Medicaid recipients need to show their Medicaid card to pharmacies and transportation providers when receiving these services.
