Nc Medicaid Transformation: The Basics
The Medicaid Transformation plan will move most of NC Medicaids services for adults and children into a managed care model, such that:
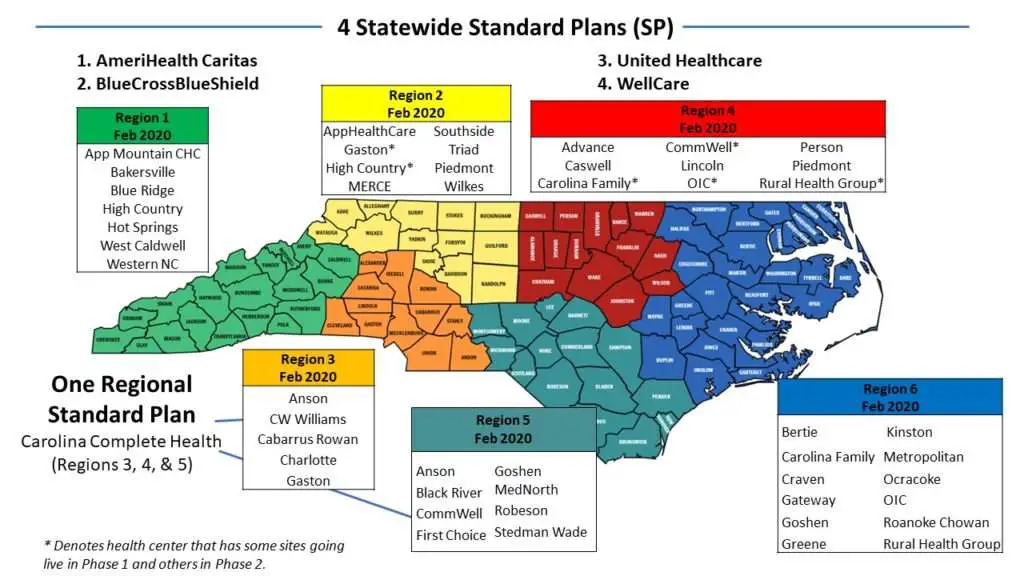
- Beneficiaries will select or be assigned to a Prepaid Health Plan which will offer a Standard Plan through which beneficiaries will access health care services from the companys network of providers.
- Providers will contract with Standard Plans to serve Medicaid beneficiaries through Plan networks and will bill Plans for those services
- NC DHHS will pay Standard Plans a set rate for each beneficiary that elects into/is assigned to the Standard Plan, and Standard Plans will have to managed beneficiary health care costs within that provided amount
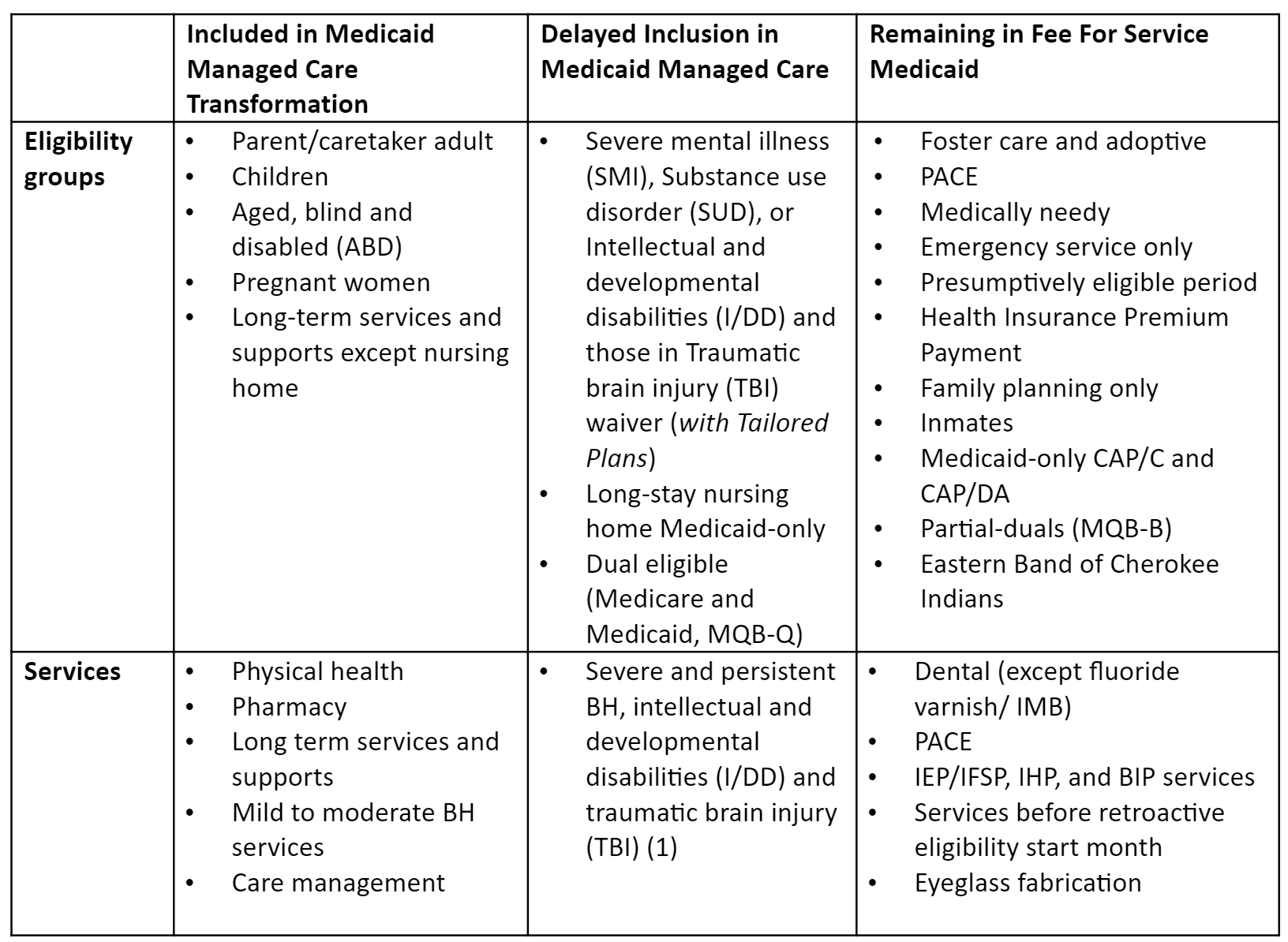
Table 1: NC Medicaid Eligibility Groups and Services, by status of inclusion status in Medicaid Transformation to Standard and Tailored Plans
Tips For A Successful Transition
- Start learning early about the new Medicaid changes and make sure that your DSS Caseworker has your most updated address, phone number and email address.
- Contact the Enrollment Broker at 1-833-870-5500 with any questions related to enrolling in NC Medicaid Managed Care.
Sobre el Cuidado Administrado de NC Medicaid El Cuidado Administrado de NC Medicaid es una buena manera de recibir los mismos servicios de Medicaid que tiene en el presente y le ayuda a recibir lo máximo de sus beneficios de Medicaid.
En vez de un programa de Medicaid, hay muchos planes a escoger. Todos los planes de salud están requeridos a tener los mismos servicios de Medicaid tales como visitas a oficina, exámenes de sangre y radiografías.
Los planes de salud también pueden ofrecer servicios adicionales tales como programas para dejar de fumar, comer más saludablemente y mantener un embarazo saludable.
Cada plan tiene su propia red de doctores calificados y profesionales de la salud.
Para mantener a su doctor, clínica u otro proveedor, averigüe con que planes ellos trabajan. Entonces elija uno de esos planes.
Tailored Plans Will Start December 1 2022
On December 1, 2022, NC Medicaid will have a new type of health plan. It is called the Behavioral Health and Intellectual/Developmental Disabilities Tailored Plan . People who need certain services to address a mental health disorder, substance use disorder, intellectual/developmental disability or traumatic brain injury may qualify for the Tailored Plan that serves their county.To learn more, go to Tailored Plan services.
Meetings and events
You can schedule rides to medical appointments. Learn more about transportation services.
Get the free mobile app
To get the app, search for NC Medicaid Managed Care on or the App Store.
Use the app to find and view primary care providers and health plans for you and your family. Learn more about the free mobile app at .
You May Like: Where Can I Apply For Medicaid In Florida
About Nc Medicaid Managed Care
NC Medicaid Managed Care is a new way to get the same Medicaid services that you have right now and it helps you get the most out of your Medicaid benefits.
Instead of one Medicaid program, there are many health plans to choose from. All health plans are required to have the same Medicaid services, such as office visits, blood tests and X-rays.
Health plans may also offer added services such as programs to help you quit smoking, eat healthier, and have a healthy pregnancy.
Each plan has its own network of qualified doctors and health care professionals.
To keep your doctor, clinic or other provider, find out which plans they work with. Then choose one of those plans.
Ncdhhs Begins Mailing Enrollment Packets And Launches Call Center In Preparation For Nc Medicaid Managed Care Open Enrollment
Link to Original Release:
The North Carolina Department of Health and Human Services has begun mailing enrollment packets statewide and launched new resources for beneficiaries as it prepares for NC Medicaid Managed Care Open Enrollment which begins on Mar. 15, 2021. Beneficiaries can now call the NC Medicaid Enrollment Call Center to learn more about NC Medicaid Managed Care and can download a free beneficiary enrollment mobile app.
These new tools, as well as the NC Medicaid enrollment website, will assist beneficiaries in choosing a primary care provider and a health plan for their families care. Some people will not need to choose a health plan because of the type of health services they need.
The NC Medicaid Enrollment Call Center number is 833-870-5500 . The free mobile app, called NC Medicaid Managed Care, is available on Google Play or the App Store. Mailings of enrollment packets are being done in batches and should arrive at beneficiary homes by Monday, Mar. 15, 2021.
Health plans also have added services such as educational assistance and programs to have a healthy pregnancy. The Eastern Band of Cherokee Indians Tribal Option is an additional managed care option for federally recognized tribal members and other individuals eligible to receive services through Indian Health Service.
Also Check: How Much Does Medicaid Pay
Will I Lose My Medicaid With These New Changes
No. The eligibility for Medicaid will remain the same.
Union County DSS will continue to process Medicaid applications and recertify individuals and families for Medicaid just as they do now.
Individuals and families that use Medicaid will now have the opportunity to choose from five health plans instead of just one.
Reminder: Open Enrollment Period For Nc Medicaid Managed Care Ends May 14
The statewide open enrollment period for NC Medicaid Managed Care will end May 14, 2021. Most people in NC Medicaid must choose a health plan as part of the States transition to NC Medicaid Managed Care.
Some people will stay in NC Medicaid Direct, and others will be able to choose whether they move to a health plan or not. This Fact Sheet outlines who must choose a health plan, who may choose a health plan, and who cannot choose a health plan.
You may receive information from your health care provider encouraging you to choose a health plan they are contracted with in NC Medicaid Managed Care so you can continue being their patient. Communication from providers is not an official enrollment notice. Depending on your current eligibility, you may not be required to choose a health plan. For questions, including whether you need to enroll, please call the NC Medicaid Enrollment Broker Call Center at 833-870-5500 or visit ncmedicaidplans.gov.
Beneficiaries can now enroll through one of four channels:
For more information, beneficiaries can reference the enrollment packets that were mailed to them, visit the NC Medicaid Managed Care website or call the NC Medicaid Managed Care Call Center at 833-870-5500 .
Also Check: What Does Medicaid Cover In Ny
Consejos Para Una Transicin Exitosa
- Empiece a aprender temprano sobre los nuevos cambios de Medicaid y asegúrese de que su trabajador de caso de Servicios Sociales tenga su dirección, número de teléfono y correo electrónico más recientes.
- Comuníquese con su Agente de Inscripción al 1-833-870-5500 con cualquier pregunta relacionada a la matrícula del Cuidado Administrado de NC Medicaid.
Nc Medicaid Managed Care Launches
Starting July 1, nearly 1.6 million Medicaid beneficiaries in North Carolina began receiving the same Medicaid services in a new way through NC Medicaid Managed Care health plans.
Starting July 1, 2021, most Medicaid beneficiaries began receiving the same Medicaid services in a new way. Called “NC Medicaid Managed Care,” beneficiaries choose a health plan and get care through a health plan’s network of doctors. Some beneficiaries are remaining in traditional Medicaid, which is called NC Medicaid Direct.
Don’t Miss: Dual Enrollment Medicare And Medicaid
Nc Medicaid Managed Care
In 2015, the NC General Assembly enacted legislation directing DHHS to transition Medicaid and NC Health Choice from fee-for-service to managed care. Under managed care, the state contracts with insurance companies, which are paid a predetermined set rate per enrolled person to provide all services.
In July 2020, legislation authorized NC Medicaid Managed Care to begin July 1, 2021, for Standard Plans and Dec. 1, 2022, for Behavioral Health I/DD Tailored Plans.
Medicaid Managed Care Webinar Series
The North Carolina Department of Health and Human Services Division of Health Benefits and North Carolina AHEC are offering an evening webinar series to help providers, practice managers, and quality managers succeed with Medicaid Managed Care.
Hosted by Shannon Dowler, MD, Chief Medical Officer of the NC Division of Health Benefits, the Medicaid Managed Care webinars on the 3rd Thursday of the month are dedicated to bringing you late breaking information and guidance on NC Medicaids transition to Managed Care.
Topics will vary, but each session will include an open question and answer period. Upcoming topics will include: pharmacy and durable medical equipment, behavioral health, transitions of care, specialized therapies, quality measures, network adequacy, provider directory, billing, incentive payments, clinical coverage policy updates, and more.
Also Check: Medicaid Texas Income Limits 2020
Unitedhealthcare Dual Complete Plans
Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
Unitedhealthcare Senior Care Options Plan
UnitedHealthcare SCO is a Coordinated Care plan with a Medicare contract and a contract with the Commonwealth of Massachusetts Medicaid program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is a voluntary program that is available to anyone 65 and older who qualifies for MassHealth Standard and Original Medicare. If you have MassHealth Standard, but you do not qualify for Original Medicare, you may still be eligible to enroll in our MassHealth Senior Care Option plan and receive all of your MassHealth benefits through our SCO program.
Recommended Reading: Does Immediate Care Take Medicaid
What Is A Tailored Plan
A Tailored Plan is a North Carolina Medicaid and NC Health Choice health plan. It offers physical health, pharmacy, care management and behavioral health services. It is for members who may have significant mental health needs, severe substance use disorders, intellectual/developmental disabilities or traumatic brain injuries . Tailored Plans offer added services for members who qualify.
Tailored Plan auto-enrollment begins . If you are auto-enrolled in a Tailored Plan or have the option to choose a Tailored Plan, you will receive a notice in the mail. Tailored Plans will start
Who qualifies for a Tailored Plan?
- People who get Innovations Waiver services
- People who get Traumatic Brain Injury Waiver services
- People who may have a mental health disorder,substance use disorder, intellectual /developmental disability or traumatic brain injury .
Nc Medicaid Managed Care Plans And Nccra
As you may be aware the NC Medicaid Managed Care plans kicked off on July 1st. We wanted to share some information about cardiovascular and pulmonary rehab coverage for these plans but encouraged you to contact your business office regarding your organizations participation with each plan.
In contacting United Healthcare Community Care for a patient we were told that both Cardiac and Pulmonary Rehabilitation allow up to 15 sessions of therapy and no pre-authorization was needed.
In contacting Healthy Blue we were told that Cardiac rehabilitation must be pre-authorized and that we could suggested the number of therapy sessions we think are needed and that Clinical Review would either except or indicate the number of sessions allowed. We were told there is no coverage for Pulmonary or Respiratory therapy.
In contacting WellCare we were told that Cardiac Rehabilitation and Pulmonary Rehabilitation must be pre-authorized but Respiratory Therapy did not require pre-authorization.
In contacting AmeriHealth Caritas they tell us that Cardiac Rehabilitation does not require pre-authorization for participating providers but would require pre-authorization for non-participating providers. They could find no information for either Pulmonary Rehabilitation or Respiratory Therapy and suggested that those services would require pre-authorization.
We did not check with Carolina Complete Health or EBCI Tribal Option.
Below is are the links to the Health Plans.
Don’t Miss: Is Wisdom Teeth Removal Covered By Medicaid
Vaya Total Care Tailored Plan For Medicaid Members
For Medicaid and NC Health Choice beneficiaries with serious mental illness, serious emotional disturbance, severe substance use disorder, intellectual/ developmental disabilities , or a traumatic brain injury :
- Physical health care services
- Traumatic Brain Injury services
- Long-term services and supports
- Dedicated care manager
Unitedhealthcare Connected For Mycare Ohio
UnitedHealthcare Connected® for MyCare Ohio is a health plan that contracts with both Medicare and Ohio Medicaid to provide benefits of both programs to enrollees. If you have any problem reading or understanding this or any other UnitedHealthcare Connected® for MyCare Ohio information, please contact our Member Services at from 7 a.m. to 8 p.m. Monday through Friday for help at no cost to you.
Si tiene problemas para leer o comprender esta o cualquier otra documentación de UnitedHealthcare Connected® de MyCare Ohio , comuníquese con nuestro Departamento de Servicio al Cliente para obtener información adicional sin costo para usted al de lunes a viernes de 7 a.m. a 8 p.m. .
This is not a complete list. The benefit information is a brief summary, not a complete description of benefits. For more information contact the plan or read the Member Handbook. Limitations, copays, and restrictions may apply. For more information, call UnitedHealthcare Connected Member Services or read the UnitedHealthcare Connected Member Handbook. Benefits, List of Covered Drugs, pharmacy and provider networks and/or copayments may change from time to time throughout the year and on January 1 of each year.
Recommended Reading: Amerigroup Medicaid Texas Breast Pump
Is A Tailored Plan The Right Option For Me
The right option for you will depend on your eligibility and your unique health needs. If you are currently enrolled in Medicaid or NC Health Choice and want to learn more about choosing the right plan for you, call the NC Medicaid Enrollment Broker Call Center at , Monday through Sunday from 7 a.m. to 8 p.m. The Enrollment Broker can answer your questions when the Tailored Plan enrollment period begins in August 2022.
If you are not enrolled in Medicaid or NC Health Choice, you can find out if you are eligible by contacting your countys Department of Social Security office. A list of DSS offices is available on the NCDHHS website.
Nd Annual Virtual Statewide Quality Forum
The North Carolina Department of Health and Human Services Division of Health Benefits and North Carolina AHEC, in conjunction with the five Medicaid managed care health plans, will host the 2nd Annual Virtual Statewide Quality Forum on from 12:30-1:30 p.m. to help providers, practice managers, and quality managers succeed with Medicaid Managed Care quality initiatives. This information session will cover the following topics:Statewide Medicaid Standard Plan Metric OutcomesAMH Metrics: Maximizing Data CaptureAMH Support
Access the October 12, 2021 Recording, Slides and Transcript.
Recommended Reading: What’s The Income Level For Medicaid
Nc Medicaid Managed Care To Launch Statewide On July 1
Starting July 1, nearly 1.6 million Medicaid beneficiaries in North Carolina will begin receiving the same Medicaid services in a new way through NC Medicaid Managed Care health plans. Most beneficiaries will continue to get care from the same doctors they see today but will now be a member of a health plan. Some beneficiaries will not enroll with health plans and will remain in NC Medicaid Direct.
NCDHHS has leveraged the move to managed care to build an innovative health care delivery system that puts the health of beneficiaries at the forefront. Features of the states program include establishing a payment structure that rewards better health outcomes, integrating physical and behavioral health, and investing in non-medical interventions aimed at reducing costs and improving the health of Medicaid beneficiaries. “July 1 marks a significant milestone with the official launch of Medicaid Managed Care in North Carolina,” said North Carolina Department of Health and Human Services Secretary Mandy K. Cohen, M.D. “From the start of this process, our goal has been to improve the health of North Carolinians through an innovative, whole-person centered, and well-coordinated system of care. Today moves us closer to that goal as we begin to implement this important program.”
Additionally, for issues that cannot be resolved with their health plans, beneficiaries can contact the NC Medicaid Ombudsman at 877-201-3750.
Which Health Plans Do I Get To Choose From
| Plan | |
|---|---|
| Carolina Complete Health** | 1-833-552-3876 |
* EBCI Tribal Option is only available in Cherokee, Graham, Haywood, Jackson and Swain counties. Eligible members in the following counties may opt in: Buncombe, Clay, Henderson, Macon, Madison and Transylvania.
** Carolina Complete Health is only available in these counties: Alamance, Alexander, Anson, Bladen, Brunswick, Cabarrus, Caswell, Catawba, Chatham, Cleveland, Columbus, Cumberland, Durham, Franklin, Gaston, Granville, Harnett, Hoke, Iredell, Johnston, Lee, Lincoln, Mecklenburg, Montgomery, Moore, Nash, New Hanover, Orange, Pender, Person, Richmond, Robeson, Rowan, Sampson, Scotland, Stanly, Union, Vance, Wake, Warren, and Wilson.
Recommended Reading: Doctors In San Antonio That Accept Medicaid
Choosing A Health Plan
Open Enrollment ended May 21, 2021. If you did not choose a health plan by this date, you were auto-enrolled in a health plan to ensure you could continue to get care. Most people were able to keep their same doctors.
Each health plan works with a network, or group of doctors, hospitals and other health care providers. You should choose a health plan that will let you keep going to your doctors and other health care providers. All health plans offer the same basic benefits and services. Some may also offer added services. When choosing a health plan, you may want to ask:
You can learn more about what health plans are available to you and the services they provide by visiting ncmedicaidplans.gov or calling 833-870-5500.
If you are new to Medicaid, you can get help in plan selection/change in one of the following ways:
- Complete and return a paper enrollment form by fax or mail
- Use the NC Medicaid Managed Care mobile app
AmeriHealth Caritas
