Medicare For Ssi Recipients
Do you get Medicare coverage if you were approved for SSI? Claimants who are approved for SSI only typically receive Medicaid coverage in most states. And like SSI, Medicaid is subject to income and asset limitations. Medicaid is a needs-based, state- and county-administered program that provides for a number of doctor visits and prescriptions each month, as well as nursing home care under certain conditions.Can you ever get Medicare if you get SSI? Medicare coverage for SSI recipients does not occur until an individual reaches the age of 65 if they were only entitled to receive monthly SSI disability benefits. At the age of 65, these individuals are able to file an uninsured Medicare claim, which saves the state they reside in the cost of Medicaid coverage. Basically, the state pays the medical premiums for an uninsured individual to be in Medicare so that their costs in health coverage provided through Medicaid goes down.
For people with limited income and assets, Medicare offers Extra Help for prescription drug costs. This Extra Help covers the costs of a Medicare prescription drug plan including monthly premiums and prescription co-pays. The application is online at www.socialsecurity.gov/prescriptionhelp. For more information, see Nolos article on the Extra Help subsidy.
What If Im Turned Down By Medicaid
- You may be able to buy a private health plan through the Marketplace instead for the 2018 plan year in the fall. You may qualify for savings based on your income through a premium tax credit and savings on out-of-pocket costs.
- If you don’t qualify for either Marketplace or Medicaid savings, you still have options. Learn more here.
Special Enrollment Periods For Unemployed Persons
Losing coverage because of losing a job is a life event under the Affordable Care Act that creates a special enrollment period. Those who lose employment-based coverage can get new coverage with a special enrollment period of sixty days. This life event exception applies to those that lose coverage as a dependent too.
They can get a special enrollment period to buy new insurance coverage. The items below are among the life events that can help the unemployed get a special enrollment period.
- Losing employer-sponsored health insurance as an employee
- Losing employer-sponsored health insurance as a dependent
- Losing employer-sponsored coverage on the 26th birthday
- Losing employer-sponsored coverage by divorce
Dont Miss: Medicaid Long Term Care Virginia
You May Like: How To Apply For Medicaid In Las Vegas Nevada
Medicaid Eligibility In Texas
You may be eligible for Medicaid in Texas if you fit the following requirements.
- You are a legal resident of Texas, i.e., a U.S citizen, legal alien or permanent resident, and need health insurance/care assistance.
- Your financial situation falls under the low or very low-income bracket.
- You are responsible for a child who is 18 or younger or blind
- You are pregnant
- You or a family member suffers from a disability
- You are 65 years or older
- If you live with an underage uninsured child. This includes your grandparents, parents or stepparents, legal guardians, adult brothers, and sisters.
- If you are a young adult who is 19 years of age or younger and lives on your own.
Apply For Benefits In Person
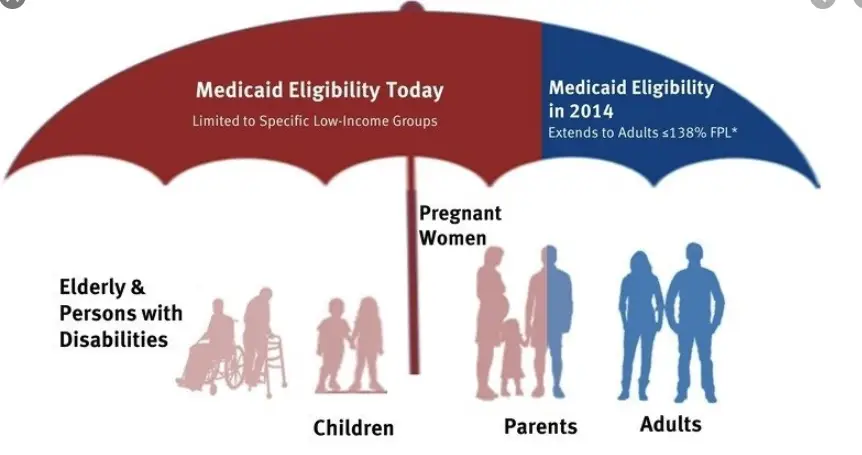
Also Check: Why States Should Not Expand Medicaid
Also Check: New York Department Of Social Services Medicaid
What Information Will I Need To Have Ready To Apply
You will need to provide information such as name, date of birth, and gender for all members of the household. You will need to provide information about all sources of income received by household members and whether individuals have other insurance. For more on what counts as income, read this blog by Tricia Brooks. You will also need to provide Social Security numbers for anyone applying for coverage.
Make Sure Youre Eligible
The Medi-Cal eligibility requirements have expanded, which means individuals and families that previously didnt qualify, may now be approved. If you are a citizen or legal resident of the state of California and you earn less than 138 percent of the Federal Poverty Level, you probably qualify. Mybenefitscalwin.org has an online questionnaire you can fill out to quickly determine whether or not you meet the requirements for the program.
Donât Miss: Does Medicaid Cover Wisdom Teeth Removal In Florida
Also Check: How To Get Help With Medicaid
What You Need To Know About Medicaid
- Eligibility is based on family size, assets, and income
- Generally, once a person is eligible for Medicaid coverage, coverage starts on the date of application or on the first day of the month of application. Sometimes, benefits for up to three months before the month of application might be covered. Coverage usually stops at the end of the month in which a person is no longer eligible for coverage. Be sure to check with your state to find the exact start and end date for coverage for you or your loved one.
- Medicaid benefits can be different depending on the state in which you live. Check with your state to find out what benefits are available to you. A list of mandatory and optional Medicaid benefits can be found here.
- Medicaid is a type of health insurance, but the caseworkers may know of other helpful resources for people with low incomes
- Check if your health care provider accepts Medicaid
What Age Can I Get Medicare
If you are 65 years old or more, you are eligible for full Medicare benefits if:
- You are a U.S. citizen or a permanent legal resident who has lived in the United States for at least five years.
- You are getting Social Security or Railroad Retirement benefits or have worked long enough to be qualified for those benefits but are not yet collecting them.
- You or your husband/wife is a government employee or retiree who has not paid into Social Security but has paid Medicare payroll taxes while working.
If you are younger than 65, you may still be qualified. You are eligible for full Medicare benefits if you are less than 65 years old if:
- You have been getting to Social Security Disability benefits for at least 2 years
- You get a disability pension from the Railroad Retirement Board and meet specific conditions
- You have Lou Gehrigs disease, also called amyotrophic lateral sclerosis , which makes you immediately eligible
- You have permanent kidney failure for which you need regular dialysis or a kidney transplant and you or your spouse has paid Social Security taxes for a certain period, based on your age.
Don’t Miss: If You Have Medicaid Do You Need Medicare Part B
Effective Date Of Coverage
Once an individual is determined eligible for Medicaid, coverage is effective either on the date of application or the first day of the month of application. Benefits also may be covered retroactively for up to three months prior to the month of application, if the individual would have been eligible during that period had he or she applied. Coverage generally stops at the end of the month in which a person no longer meets the requirements for eligibility.
How To Qualify For Medicaid
May 15, 2020, 12:00 AM
It can be expensive to pay for health insurance when you lose your job, but many people dont realize that theyre eligible for Medicaid coverage. If you live in one of the 36 states that expanded Medicaid coverage for low-income adults, you can qualify for coverage if your monthly income is less than $1,467 for an individual or $3,013 for a family of four even if you earned a lot more than that during the first few months of the year.
This type of Medicaid has different eligibility requirements than the version that provides nursing home coverage for people over age 65 there is no asset test for this type of Medicaid. Instead, eligibility is based on your family size and your modified adjusted gross income .
Many people dont know that theyre eligible for Medicaid, says Robin Rudowitz, co-director of the Program on Medicaid and the Uninsured at the Kaiser Family Foundation. Medicaid is based on monthly income, so people who have significant drops in income could become eligible. There is no open enrollment period for Medicaid, so when people experience a change in their circumstances, they dont have to wait for a special open enrollment period to enroll.
Heres more information about how to qualify for Medicaid, how the coverage works and what you can do if your state hasnt expanded coverage.
Who Is Eligible for Medicaid?
Read Also: Hearing Aids Covered By Medicaid
How Do I Apply
There are two ways you can apply for Medicaid. First, you can enroll through the HealthCare.gov marketplace by creating an account and filling out the application. The second option is applying directly through your states Medicaid agency. Its that easy!
Medicaid is there to ensure that people on limited incomes can still attain quality health care, but since the program is managed by each state, the different requirements can be confusing. Luckily, the number of states that are expanding their eligibility of coverage is growing, creating a standardization across the country. This makes it easier to know what to expect if your considering looking into Medicaid as a health care coverage option!
Q How Much Income Can I Receive And Still Be Eligible For Medicaid

A. Income is money that you get from working, or money that someone gives you, or checks that you receive, such as a Social Security check, unemployment benefits, child support, retirement benefits, or sick pay. Whether your income level qualifies you or your family for Medicaid depends on the size of your family and the Medicaid program for which you are applying.
Income limits are set each year by the federal government to define the Federal Poverty Level for different family sizes. In general, if your household income is at or below the current 100% Federal Poverty Level for your household size, your family is likely to be eligible for Medicaid. Children from age 1 to under age 6 can qualify for Medicaid benefits when household income is at or below 133% of the Federal Poverty Level. Pregnant women and infants under age 1 qualify for Medicaid with family income at or below the 200% Federal Poverty Level, and pregnant women count as 2 family members.
See our tables of income limits for applying for DMMA programs to find out where your family income is, in relation to these income benchmarks.
Medical assistance programs other than Medicaid have different income level requirements. For example, uninsured children under age 19 who live in families with incomes at or below the 200% Federal Poverty Level are eligible for low cost health insurance under the Delaware Healthy Children Program.
Also Check: Medicaid Nevada Provider Phone Number
Policy Basics: Introduction To Medicaid
In 2018, Medicaid provided health coverage for 97 million low-income Americans.
In 2018, Medicaid provided health coverage for 97 million low-income Americans over the course of the year. In any given month, Medicaid served 32 million children, 28 million adults , 6 million seniors, and 9 million people with disabilities, according to Congressional Budget Office estimates.
Children account for more than two-fifths of Medicaid enrollees but only one-fifth of Medicaid spending. Only one-fifth of Medicaid enrollees are seniors or people with disabilities, but because they need more health care services, they account for nearly half of Medicaid spending.
Medicaid is sometimes confused with Medicare, the federally administered, federally funded health insurance program for people over 65 and some people with disabilities. And there is overlap between the two programs: nearly 10 million low-income seniors and people with disabilities so-called dual eligibles are enrolled in both Medicare and Medicaid.
Do I Qualify For Medicaid
Medicaid provides free or low-cost health coverage to some low-income people, families and children, pregnant women, the elderly, and people with disabilities. Many states have expanded their Medicaid programs to cover all people below certain income levels. Medicaid qualifications depend partly on whether your state has expanded its program.
Also Check: Medicaid Office Great Falls Mt
I Have Pregnancy Only Coverage What Does Medicaid Cover
Pregnancy-only coverage only covers services related to or caused by the pregnancy. Please talk to your PCP or South Dakota Medicaid about whether a service will be covered if you are unsure.
Routine dental and vision services are not covered in this program. If you feel you have a health issue that may put you and your baby at risk, contact your PCP.
Q How Long Will My Medicaid Benefits Remain Active
A. Medicaid is based on month to month eligibility. However, your benefits are redetermined on a yearly basis by DMMA to confirm whether you still remain eligible for the program you are receiving. Certain Medicaid programs require you to report changes in your situation within 10 days of the change. One example of a change that must be reported is new employment.
Recommended Reading: Blue Shield Of California Medicaid
Person Who Is Aged Blind And/or Disabled
Apply if you are aged , blind, or disabled and have limited income and resources. Apply if you are terminally ill and want to get hospice services. Apply if you are aged, blind, or disabled live in a nursing home and have limited income and resources. Apply if you are aged, blind, or disabled and need nursing home care, but can stay at home with special community care services. Apply if you are eligible for Medicare and have limited income and resources.
Special Home And Community
The Special Home and Community-Based Services Waiver Group eligibility pathway allows states to extend Medicaid eligibility to individuals receiving HCBS under a waiver program87 who require the level of care provided by a nursing facility or other medical institution.88 This eligibility pathway is sometimes referred to as the 217 Group in reference to the specific regulatory section for this group, 42 C.F.R. Section 435.217. States use the highest income and resource standard of a separate eligibility group covered by the state plan under which an individual would otherwise qualify if institutionalized. For example, states that offer the Special Income Level pathway described above can extend eligibility to waiver program participants with income up to 300% of the SSI FBR. States must use the income- and resource-counting methodologies used to determine eligibility for this same eligibility group. States may also apply Section 1902s more liberal income-counting rules to this group.
Also Check: Keystone First Medicaid Phone Number
What Happens If You Are No Longer Eligible For Medicaid
- Learn where to turn when you are no longer eligible for Medicaid. Depending on your state and situation, there may be other health care options available at an affordable price.
If you are no longer eligible for Medicaid, there are other options that can help you maintain health insurance for you and your family. Before you can apply for them, you need to determine why you became ineligible for Medicaid benefits and what alternative health care options might pertain to your specific situation.
Spousal Impoverishment Prevention Coverage

This coverage applies to couples where one needs Nursing Care Services in a facility or at home.
The spouse receiving the nursing care services is allowed $3,000. The spouse who remains in the community is entitled to keep half of the couple’s countable assets, but not less than $27,480 and not more than $137,400 for calendar year 2022.
The spouse receiving the nursing care services may keep up to $65 of their monthly income and may deem income to bring the income of the spouse in community up to $2,550 per month and any dependent household members up to $726.
Read Also: Is It Hard To Get Medicaid In Florida
Who Is Eligible For Medicare And Medicaid
Medicare and Medicaid are two different government-run programs. They are operated and funded by various parts of the government and primarily serve different groups.
- Medicare is a federal program that provides health coverage if you are more than 65 years old or are under 65 and have a disability, regardless of your income.
- Medicaid is a state and federal program that gives health insurance if you have a very low income.
- If you are qualified for both Medicare and Medicaid , you can have both. They will work together to provide you with health coverage and lower your costs.
Moreover, keep in mind that while Medicare and Medicaid are both health insurance programs that are federally supported, there are differences in covered services and cost-sharing. You can call 1-800-MEDICARE or get in touch with your local Medicaid office to learn more about Medicare and Medicaid costs and coverage, especially if you are dual-eligible.
Do Disability Recipients Automatically Qualify For Medicare And Medicaid
Posted on behalf of Sigman, Janssen, Sewall, Pitz & Burkham on in Social Security
If the Social Security Administration grants you disability benefits, you may at some point qualify for Medicare or Medicaid health care coverage. Individuals receiving disability benefits are either unable to work or are not working enough hours to be eligible for health insurance from their employer.
Qualifying for Medicare or Medicaid will depend on whether you are approved for Social Security Disability insurance or Supplemental Security Income . If you have questions about receiving or retaining your disability benefits, a Social Security Disability attorney in Green Bay is here to assist you. An initial consultation is completely free and confidential.
Recommended Reading: Medicaid Albany Ny Phone Number
You May Like: Is Amerihealth Caritas Medicaid Or Medicare
