Which Medicaid Recipients Are Excluded From Participation In The Managed Care Plans
The populations that are excluded from participation in the Managed Care Plans and who will receive all their services in the regular Medicaid program are
- Recipients over age 21 who are residents of an intermediate care facility for the developmentally disabled .
- Recipients with limited eligibility periods of 3 months or less
- Recipients receiving a limited benefit package
Health Plans And Program
In Florida, most Medicaid recipients are enrolled in the Statewide Medicaid Managed Care program. The program has three parts: Managed Medical Assistance, Long-Term Care, and Dental. People on Medicaid will get services using one or more of these plan types:
Managed Medical Assistance : Provides Medicaid covered medical services like doctor visits, hospital care, prescribed drugs, mental health care, and transportation to these services. Most people on Medicaid will receive their care from a plan that covers MMA services.
Long-Term Care : Provides Medicaid LTC services like care in a nursing facility, assisted living, or at home. To get LTC you must be at least 18 years old and meet nursing home level of care .
Dental: Provides all Medicaid dental services for children and adults. All people on Medicaid must enroll in a dental plan.
What Is Heritage Health
Heritage Health is a new healthcare delivery system that combines Nebraskas current physical health, behavioral health, and pharmacy programs into a single comprehensive and coordinated system for Nebraskas Medicaid and CHIP clients.
For Heritage Health enrollment information, please call 1-888-255-2605, or visit the Heritage Health website.
Nebraska Total Care offers the services you and your family want and need. Our services include:
- Primary Care Visits
- Wellness and Healthy Rewards Programs
- Prescriptions
- Care and Disease Management Services
- Behavioral Health and Substance Use Services and Programs
- Hearing and Vision Services
You May Like: How Does Emergency Medicaid Work
Medicaid Is Jointly Financed By States And The Federal Government
Medicaid is financed jointly by the federal government and states. The federal government matches state Medicaid spending. The federal match rate varies by state based on a federal formula and ranges from a minimum of 50% to nearly 75% in the poorest state. Under the ACA, the federal match rate for adults newly eligible was 100% for 2014-2016, phasing down gradually to 90% in 2020 and thereafter . The federal matching structure provides states with resources for coverage of their low-income residents and also permits state Medicaid programs to respond to demographic and economic shifts, changing coverage needs, technological innovations, public health emergencies such as the opioid addiction crisis, and disasters and other events beyond states control. The guaranteed availability of federal Medicaid matching funds eases budgetary pressures on states during recessionary periods when enrollment rises. Federal matching rates do not automatically adjust to economic shifts but Congress has twice raised them temporarily during downturns to strengthen support for states.
Total federal and state Medicaid spending was $577 billion in FY 2017. Medicaid is the third-largest domestic program in the federal budget, after Social Security and Medicare, accounting for 9.5% of federal spending in FY 2017. In 2017, Medicaid was the second-largest item in state budgets, after elementary and secondary education .
Figure 8: Medicaid is a budget item and a revenue item in state budgets.
The Majority Of The Public Holds Favorable Views Of Medicaid
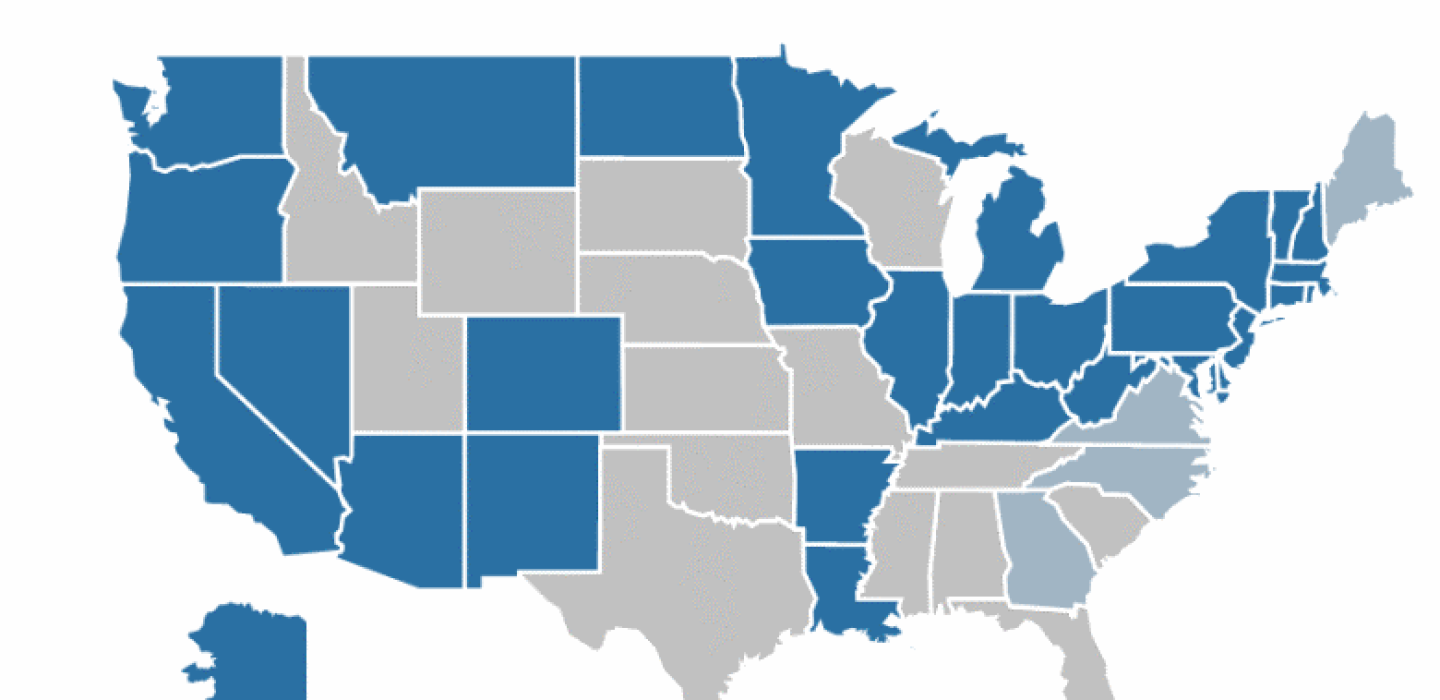
Public opinion polling suggests that Medicaid has broad support. Seven in ten Americans say they have ever had a connection with Medicaid including three in ten who were ever covered themselves. Even across political parties, majorities have a favorable opinion of Medicaid and say that the program is working well . In addition, polling shows that few Americans want decreases in federal Medicaid funding. In addition to broad-based support, Medicaid has very strong support among those who are disproportionately served by Medicaid including children with special health care needs, seniors, and people with disabilities.
Figure 10: Large Shares Across Parties Say They Have a Favorable Opinion of Medicaid
Recommended Reading: Priority Health Medicaid Find A Doctor
Feds Approve Arkansas Plan To Overhaul Medicaid Expansion
LITTLE ROCK, Ark. Arkansas Gov. Asa Hutchinson said Tuesday that the federal government has approved the states proposal to overhaul its Medicaid expansion.
This will allow 300,000 low-income Arkansans to continue to receive health care under our qualified insurance plans that have been very successful in Arkansas in expanding health care, Hutchinson said.
The state Department of Human Services submitted the overhaul proposal to the federal government over the summer after the programs previous requirement that some recipients work was blocked by the courts.
As with the current program, the overhauled expansion would continue using Medicaid funds to place recipients on private health insurance.
Arkansas unveiled the proposal after the Biden administration moved to roll back Medicaid work requirements in Arkansas and several other states. A federal judge blocked the Arkansas work requirement.
Hutchinson said Tuesday that the federal government didnt approve the states request to continue to require individuals with income above 100% of the federal poverty level to pay a share of premiums for their coverage. He said the current premium amount of $13 per month will continue for calendar year 2022 but not beyond.
To report a correction or typo, please email
Most Read
How To Choose A Health Plan
When picking a plan, think about the following:
- Are doctors you already use and like covered by the plan?
- How is the plan rated on issues that are important to you and your family?
- What value-added services are available through the plan?
We also provide tools to help you choose the best plan for you and your family.
You May Like: How To Obtain Medicaid In Florida
Who Pays For Medicaid
Medicaid does not pay money to individuals but sends payments directly to healthcare providers.
States make these payments according to a fee-for-service agreement or through prepayment arrangements, such as health maintenance organizations . The federal government then reimburse each state for a percentage share of their Medicaid expenditures.
This Federal Medical Assistance Percentage changes each year and depends on the states average per capita income level.
The reimbursement rate begins at 50% and reaches 77% in 2020. Wealthier states receive a smaller share than states with less money.
In the states that chose to expand their coverage under the Affordable Care Act, more adults and families on low incomes are eligible with the new provision allowing enrolment at up to 138% of the FPL. In return, the federal government cover all expansion costs for the first 3 years and over 90% of the costs moving forward.
Medicare is a federal health insurance program that funds hospital and medical care for older people in the U.S. Some people with disabilities also benefit from Medicare.
The program consists of:
- Part A and Part B for hospital and medical insurance
- Part C and Part D that provide flexibility and prescription drugs
Medicaid Facilitates Access To Care
A large body of research shows that Medicaid beneficiaries have far better access to care than the uninsured and are less likely to postpone or go without needed care due to cost. Moreover, rates of access to care and satisfaction with care among Medicaid enrollees are comparable to rates for people with private insurance . Medicaid coverage of low-income pregnant women and children has contributed to dramatic in the U.S. A growing body of research indicates that Medicaid eligibility during childhood is associated with reduced teen mortality, improved long-run educational attainment, reduced disability, and lower rates of hospitalization and emergency department visits in later life. Benefits also include second-order fiscal effects such as increased tax collections due to higher earnings in adulthood. Research findings show that state Medicaid expansions to adults are associated with increased access to care, improved self-reported health, and reduced mortality among adults.
Figure 7: Nationally, Medicaid is comparable to private insurance for access to care the uninsured fare far less well.
Also Check: Michigan Pregnancy Medicaid Income Limits
Chapter 1an Overview Of Medicaid Managed Care
Medicaid plays an integral role in financing health care services in the United States, accounting for 16 percent of total health spending and providing coverage for one out of every six Americans. Among the more than 60 million citizens who rely on Medicaid are about 9 million nonelderly people with disabilities, including 1.4 million children. While people with disabilities constituted 16.5 percent of Medicaid enrollees in fiscal year 2008, expenditures on their behalf represented 44 percent of total Medicaid outlays.
The Medicaid program serves a diverse array of people with disabilities, ranging widely in age and type and severity of disability, and has an extraordinary impact on the health and quality of life of beneficiaries with disabilities. The program rolls include children with physical, sensory, intellectual, and developmental disabilities working-age adults with spinal cord and traumatic brain injuries children and adults with severe and persistent mental illnesses and low-income adults with other serious, chronic illnesses and disorders such as diabetes and cardiac and pulmonary diseases.
White House Nixes Work Requirement In Georgia Medicaid Plan
ATLANTA The Biden administration has rejected Georgia’s plan to expand Medicaid coverage on the condition that recipients meet a work requirement.
The U.S. Centers for Medicare & Medicaid Services said Thursday that it was revoking the state’s authority to require work activities or charge Medicaid recipients higher premiums. The Trump administration had approved the work provision.
CMMS cited the ongoing coronavirus pandemic in part for its decision, saying work requirements would significantly compromise the effectiveness of Georgia’s plan to boost coverage.
The decision was a blow to Georgia Republican Gov. Brian Kemp, who had promoted Georgia’s Medicaid plan as a fiscally responsible alternative to a full expansion of Medicaid services under the Affordable Care Act. The plan sought to add an estimated 50,000 poor and uninsured Georgia residents to the Medicaid rolls in its first two years.
The Kemp administration said it planned to fight Thursday’s decision in court.
Georgia proposed and received approval to implement an innovative waiver that would expand coverage and access in a fiscally conservative way,” spokeswoman Katie Byrd said in a statement. We are disappointed the Biden Administration chose to turn its back on a bipartisan group in the Georgia General Assembly that came together to help create a fair and balanced healthcare framework that increases options and lowers costs.
Read Also: Does Medicaid Cover Incontinence Pads
In Fy 2019 Payments To Comprehensive Risk
In FY 2019, state and federal spending on Medicaid services totaled nearly $604 billion.7 Payments made to MCOs accounted for about 46% of total Medicaid spending . The share of Medicaid spending on MCOs varies by state, but about three-quarters of MCO states directed at least 40% of total Medicaid dollars to payments to MCOs . The MCO share of spending ranged from a low of 0.4% in Colorado to 87% in Kansas.8 State-to-state variation reflects many factors, including the proportion of the state Medicaid population enrolled in MCOs, the health profile of the Medicaid population, whether high-risk/high cost beneficiaries are included in or excluded from MCO enrollment, and whether or not long-term services and supports are included in MCO contracts. As states expand Medicaid managed care to include higher-need, higher-cost beneficiaries, expensive long-term services and supports, and adults newly eligible for Medicaid under the ACA, the share of Medicaid dollars going to MCOs will continue to increase.
Figure 6: Payments to comprehensive MCOs account for almost half of total national Medicaid spending
Figure 7: In most MCO states, spending on MCOs makes up at least 40% of total Medicaid spending
The Meaning And Origins Of Managed Care
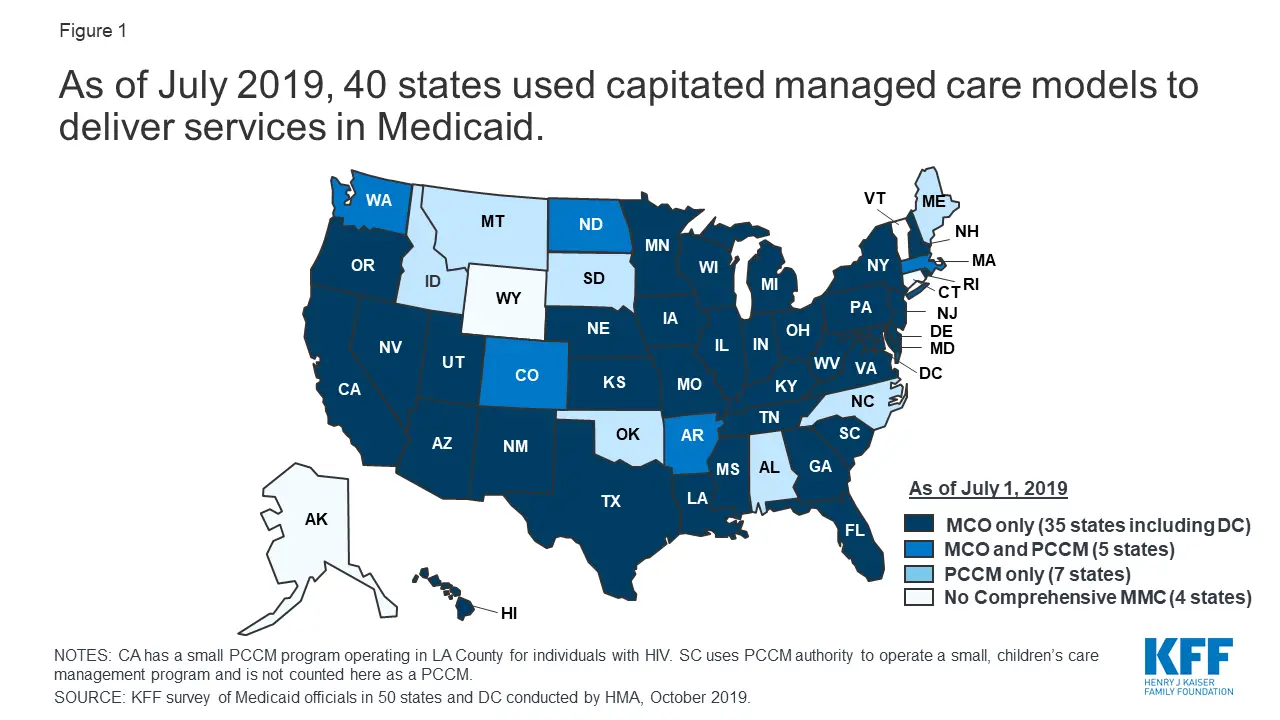
The term managed care has different meanings depending on the context in which it is used. These multiple meanings can be confusing, especially to those who are not well versed in the terminology of health care delivery systems. Reduced to its fundamentals, however, managed care involves efforts to coordinate, organize, and rationalize the delivery of health care services and supports in a manner designed to improve service access and quality while avoiding unnecessary expenditures.
Managed health care emerged in the 1930s in response to the growing cost of medical services in the United States. Physicians and hospitals banded together in local or area-wide cooperatives to provide primary and acute care services to individual subscribers in exchange for the payment of a fixed monthly fee, or premium. As employer-based health insurance became the norm in the United States, commercial insurers and large employers came to recognize the advantages of a managed care approach to controlling the costs and quality of health services. By the early 1990s, a majority of American workers were enrolled in some type of managed care arrangement.
Don’t Miss: Dentist In Montgomery Al That Accept Medicaid
Medicaid Is The Nations Public Health Insurance Program For People With Low Income
Medicaid is the nations public health insurance program for people with low income. The Medicaid program covers 1 in 5 Americans, including many with complex and costly needs for care. The program is the principal source of long-term care coverage for Americans. The vast majority of Medicaid enrollees lack access to other affordable health insurance. Medicaid covers a broad array of health services and limits enrollee out-of-pocket costs. Medicaid finances nearly a fifth of all personal health care spending in the U.S., providing significant financing for hospitals, community health centers, physicians, nursing homes, and jobs in the health care sector. Title XIX of the Social Security Act and a large body of federal regulations govern the program, defining federal Medicaid requirements and state options and authorities. The Centers for Medicare and Medicaid Services within the Department of Health and Human Services is responsible for implementing Medicaid .
Figure 1: Medicaid plays a central role in our health care system.
Services That Medicare Does Not Provide
If Medicare does not cover a medical expense or service, a person may wish to take out a Medigap plan for supplemental coverage.
Private companies also offer Medigap plans. Depending on the individual plan, Medigap may cover:
- copayments
- deductibles
- care outside of the U.S.
If a person has a Medigap policy, Medicare will first pay their eligible portion. Afterward, Medigap will pay the rest.
To have a Medigap policy, a person must have both Medicare Parts A and B and pay a monthly premium.
Medigap policies do not cover prescription drugs, which a Part D plan covers.
An individual must be one of the following to be eligible for Medicare:
- age over 65 years
- age under 65 years and living with a disability
- any age with end stage renal disease or permanent kidney failure needing dialysis or transplant
They must also be:
- a U.S. citizen or permanent legal resident for 5 years continuously
- eligible for Social Security benefits with at least 10 years of contributing payment
Also Check: I Am Pregnant And Need To Apply For Medicaid
Medicare Vs Medicaid: Whats The Difference
Fact checkedReviewed by: Leron Moore, Medicare consultant –
Understand the differences between Medicare and Medicaid and find out if you can qualify for both.
What you should know
- 1Medicare and Medicaid are both government programs to help Americans afford health care.
- 2Medicaid is funded jointly by federal and state governments and is available if you meet your states income eligibility and other standards.
- 3Medicare is health care coverage available if youre at least 65 or have a qualifying disability.
- 4Its possible to be eligible for both Medicaid and Medicare at the same time.
Have you wondered about the difference between Medicare and Medicaid? Theyre very different programs. Although both are government-run health care programs, the similarities end there. Medicaid is available if you have low income, while Medicare eligibility kicks in when you turn 65 or have a qualifying disability.
If you meet income eligibility, Medicaid can be an essential resource for covering health care expenses that Medicare does not. But not everyone can qualify for Medicaid, so you can enroll in Medicare when you reach retirement age.
Both programs are designed to offset the costs of health care services. Medicaid offers additional coverages that Medicare does not. If youre dual-eligible, you can qualify for Medicaid and Medicare and get coverage from both.
Learn more about the differences between Medicaid and Medicare.
Each Year States Develop Mco Capitation Rates That Must Be Actuarially Sound And May Include Risk Mitigation Strategies
States pay Medicaid managed care organizations a set per member per month payment for the Medicaid services specified in their contracts. Under federal law, payments to Medicaid MCOs must be actuarially sound. Actuarial soundness means that the capitation rates are projected to provide for all reasonable, appropriate, and attainable costs that are required under the terms of the contract and for the operation of the managed care plan for the time period and the population covered under the terms of the contract. Unlike fee-for-service , capitation provides upfront fixed payments to plans for expected utilization of covered services, administrative costs, and profit. Plan rates are usually set for a 12-month rating period and must be reviewed and approved by CMS each year. States may use a variety of mechanisms to adjust plan risk, incentivize plan performance, and ensure payments are not too high or too low, including risk sharing arrangements, risk and acuity adjustments, medical loss ratios , or incentive and withhold arrangements.
Figure 2: CMS has provided guidance to states to address MCO payment issues in response to the COVID-19 pandemic
Recommended Reading: Molina Medicaid Michigan Prior Authorization Form
What Is Healthy Louisiana
Healthy Louisiana is the way most of Louisiana’s Medicaid and LaCHIP recipients receive health care services. The state contracts with Health Plans that deliver these services through their provider networks. Recipients are given the chance to choose the Health Plan that best fits their family’s needs.
