How To Choose A Health Plan
When picking a plan, think about the following:
- Are doctors you already use and like covered by the plan?
- How is the plan rated on issues that are important to you and your family?
- What value-added services are available through the plan?
We also provide tools to help you choose the best plan for you and your family.
Unitedhealthcare Connected For Mycare Ohio
UnitedHealthcare Connected® for MyCare Ohio is a health plan that contracts with both Medicare and Ohio Medicaid to provide benefits of both programs to enrollees. If you have any problem reading or understanding this or any other UnitedHealthcare Connected® for MyCare Ohio information, please contact our Member Services at from 7 a.m. to 8 p.m. Monday through Friday for help at no cost to you.
Si tiene problemas para leer o comprender esta o cualquier otra documentación de UnitedHealthcare Connected® de MyCare Ohio , comuníquese con nuestro Departamento de Servicio al Cliente para obtener información adicional sin costo para usted al de lunes a viernes de 7 a.m. a 8 p.m. .
Helping You Save Money With*:
- SAMS CLUBTM membership
- Gym membership
- No-cost or discount services like haircuts
- VISA® gift cards for certain wellness visits and immunizations
- Up to $60 in VISA® gift cards for healthy pregnancy rewards
- Healthy Food for You
- Rides to medical and behavioral health appointments, pharmacy and social services
- Free cell phone with 1,000 free minutes or 1.5 GIGS of data and unlimited texting from Lifeline
- MyHPN Essentials for Baby
- Boys & Girls Club membership for kids ages 5-18
You May Like: Tens Unit Covered By Medicaid
Recipients Should Consider The Following When Choosing A Long
- What services do I think I need? Assisted Living? Home Health?
- Which plan has the providers I currently use or think I will need?
- Are the providers I need a part of the plan?
I Would Like To Change My Health Or Dental Plan

Change Health or Dental Plans Online
Log in to the FL Medicaid Member Portal to change your Health or Dental Plan. We will walk you through the process of changing your plan.
Why should you sign up for a FL Medicaid Member Portal account?
- You can check your Medicaid eligibility and enrollment status
- View and update your address
- Request help using secure messaging
- Enroll in a plan or change plans
- File complaint and see what is happening with your complaint
- Go paperless. Choose to only get letters from Medicaid electronically
- Receive email or text message alerts
Other Ways to Change Your Health or Dental Plan
If you are unable to change Health or Dental Plans online at this time, there are several other options available to you.
Recommended Reading: Does Medicaid Cover Glasses In Texas
We Know Youre Going To Have Questions
Ohio Medicaids new approach to managed care is based on extensive feedback we received from providers, patients, and other key stakeholders about the way the system was working for them.
It is designed to make access to care simpler, more personal, and more effective. But, we know youll still have questions. Feel free to contact us at with suggestions, questions and guidance on the changes ahead.
For information related to the next generation of managed care, please visit managedcare.medicaid.ohio.gov.
Health Plan Report Cards
People across Texas shared their thoughts about their health plan, and rated them, one to five stars, on the services their plan provided.You can compare plans using the overall ratings or by looking at the services that matter the most for you and your family.
You can view the report cards on the Managed Care Report Cards page. Click the program you are enrolled in and find your service area to see plans available to you.
Recommended Reading: Vision Care That Accepts Medicaid
Do The Worst Case Scenario Math
Some employers offer software that allows workers to upload their claims history from the past year and uses that to recommend a health care plan. I wish that were available to everyone. The closest Ive seen is HealthSherpa, which helps people winnow their ACA marketplace options based on how they generally use health care.
The plan that may have been a good fit for your past claims, though, may not be the best choice for the future especially if you become seriously ill or injured. To protect against worst-case scenarios, you also need to consider the out-of-pocket limits. These are the maximum amounts youd have to pay in addition to your premiums. Out-of-pocket limits typically range from $2,000 to $6,000, although there may be different maximums for in-network versus out-of-network costs, and not all policies have these caps.
Some plans give you only a small break in premiums while exposing you to much larger potential costs, says Alan Silver, senior director of benefits delivery and administration at Willis Towers Watson, a benefits consultant.
Before signing up for any policy, add your annual premiums to the out-of-pocket limit to see the potential costs you could face. If the total scares you, look for a plan with a limit that lets you sleep at night.
This article was written by NerdWallet and was originally published by The Associated Press.
Unitedhealthcare Dual Complete Plans
Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
Don’t Miss: Montefiore Medicaid Office Bronx Ny
Get Important News & Updates
Sign up for email and/or text notices of Medicaid and other FSSA news, reminders, and other important information. When registering your email, check the category on the drop-down list to receive notices of Medicaid updates check other areas of interest on the drop-down list to receive notices for other types of FSSA updates.
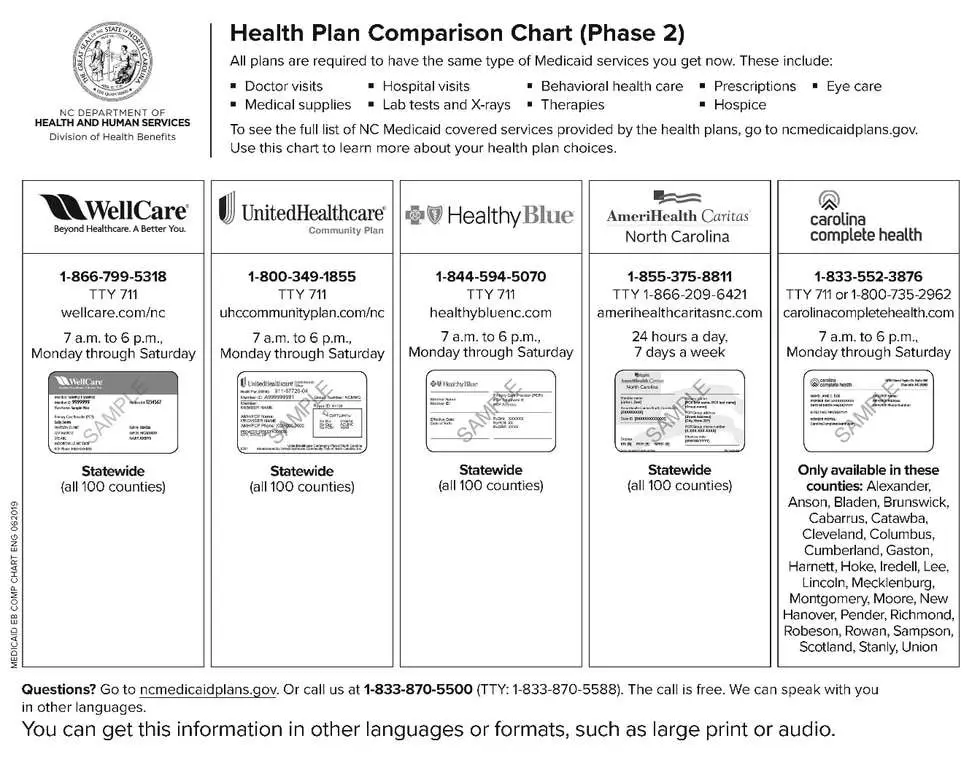
Nc Medicaid Managed Care Started July 1 2021
NC Medicaid Managed Care health plans are now active. This means that you will now get care through your health plan. If you have questions about benefits and coverage, call your health plan. You can find the number on your new Medicaid ID card or visit View health plans.
You can also contact the NC Medicaid Ombudsman if you have questions or problems your health plan or provider could not answer. Call 1-877-201-3750 or visit ncmedicaidombudsman.org.
Meetings and events
You can schedule rides to medical appointments. Learn more about transportation services.
Get the free mobile app
To get the app, search for NC Medicaid Managed Care on or the App Store.
Use the app to find and view primary care providers and health plans for you and your family. Learn more about the free mobile app at Get answers.
You May Like: Family Doctors In Charleston Wv That Accept Medicaid
Match Your Consumption To Your Deductible
Many experts recommend high-deductible plans for healthy people who rarely visit the doctor, since premiums for these plans are lower. But high-deductible plans also can be a good fit for people who need a lot of health care, says Carolyn McClanahan, a physician and certified financial planner in Jacksonville, Florida.
Parents of young children or people who have chronic health conditions often spend so much on care that they can easily meet a higher deductible, McClanahan says. Many high-deductible plans qualify for tax-advantaged health savings accounts, as well.
These plans arent a good fit, however, for people who would put off necessary care rather than pay out of pocket. If you dont have enough savings to cover medical costs until the deductible is satisfied, consider spending more for a lower-deductible plan.
Just dont pay an extra $500 to lower your deductible by $250, as many people did in that first study. If youre allowed to choose different deductibles for the same plan, multiply the difference in premiums by 12 to get your yearly cost and compare that to the difference in deductibles.
Famis Or Famis Moms Members
FAMIS or FAMIS MOMS members can choose their health plan when they apply. If they did not choose a plan when they applied, they can join a plan by calling Cover Virginia at 833-5CALLVA. If they do not choose a plan, one will be chosen for them.
Read about FAMIS health plan choices and covered services:
You May Like: Washington State Medicaid Residency Requirements
Get The Free Mobile App
To get the app, search for Healthy Louisiana on or the App Store.
Use the app to choose a health plan and provider.Available now: A new version of the app with updates and new tools. Now you can:
- Use the app in Spanish
- Find providers based on your current location
- Get directions to providers
Learn more about the free mobile app on the .
How And When Do I Choose A Health Plan
Open Enrollment ended May 21, 2021. If you did not choose a health plan by this date, you were auto-enrolled in a health plan to ensure you could continue to get care. Most people were able to keep their same doctors.
Each health plan works with a network, or group of doctors, hospitals and other health care providers. You should choose a health plan that will let you keep going to your doctors and other health care providers. All health plans offer the same basic benefits and services. Some may also offer added services. When choosing a health plan, you may want to ask:
- How do I keep my current doctors, hospitals and specialists?
- What are my choices if I change doctors?
- What added services does each health plan have?
You can learn more about what health plans are available to you and the services they provide by visiting ncmedicaidplans.gov or calling 833-870-5500.
If you are new to Medicaid, you can get help in plan selection/change in one of the following ways:
Recommended Reading: Eye Exam Places That Take Medicaid
Who Must Choose A Health Plan
Most people in NC Medicaid must choose a health plan in the NC Medicaid Managed Care program, including:
- Most families and children
- Children who get NC Health Choice
- Pregnant women
- People who are blind or disabled and do not get Medicare
NC Medicaid will send you a letter that tells you if you must enroll. To find out now, call us at 1-833-870-5500 . The call is toll free. Or use the chat tool to chat with us online. To learn more about NC Medicaid Managed Care, go to Get answers.
More People Are Getting Healthy With The Healthy Michigan Plan
Looking for health care coverage that works for your health and your budget? There’s an option to help working people like you get healthy at a cost that works in your budget. It’s the Healthy Michigan Plan.
We understand you shouldn’t have to choose between taking care of your health and taking care of your bills. That’s why the Healthy Michigan Plan makes health care benefits available to individuals at a low cost. Learn more to see if the Healthy Michigan Plan is for you and find out if you may be eligible.
On March 4, 2020, a federal judge ruled that approval of the HMP work requirements was unlawful. It is MDHHS responsibility to follow the federal judges ruling. This ruling stopped MDHHS implementation and enforcement of the work rules.This means HMP participants are no longer required to report work, school or other activities to maintain HMP health care coverage. This change is effective immediately.MDHHS is notifying individuals of the change online, by mail, and by phone. MDHHS will mail letters to active HMP beneficiaries throughout the month of March 2020. It is possible work requirements could be restarted because of a future court decision. MDHHS will notify stakeholders if this happens. Health plans, providers, and other community partners who may be utilizing HMP work requirements-related materials that were previously issued by MDHHS should remove these documents from circulation.
Don’t Miss: Till What Age Does Medicaid Cover
Medicaid Managed Care Plans
Members who live in Utah, Salt Lake, Davis, Weber, Box Elder, Cache, Iron, Morgan, Rich, Summit, Tooele, Wasatch, or Washington County, must choose a health plan. Members who live in any other county in Utah have the option of selecting a health plan or using the Fee for Service Network. The State of Utah currently has four managed care health plans/ACOs:
Managed Care Health Plans
The following members have dental benefits and must choose a dental plan:
- Pregnant Women
- Medicaid members who are eligible for Early and Periodic Screening, Diagnostic, and Treatment benefits
The State of Utah currently has two managed care dental plans statewide:
Managed Care Dental Plans
|
1-877547-5415 |
Members who are on the following Medicaid programs will receive dental benefits through fee for service Medicaid and are not required to be enrolled in a dental plan:
- Foster Care Medicaid
- Targeted Adult Medicaid members who are age 19 and 20
- Adult Expansion Medicaid members who are age 19 and 20
For more information about Medicaid dental plans and coverage,
The following Medicaid members will receive dental benefits through the University of Utah School of Dentistry and their network of providers:
- Targeted Adult Medicaid members who are receiving treatment in a Substance Use Disorder Treatment Program
- Adults, 21 and older, who are on Medicaid because of a disability or blindness
- Adults, age 65 and older, eligible for Traditional Medicaid
Managed Care Health Plans
Find And View Providers And Health Plans
This website has new tools to help you find and view primary care providers and health plans.
Medicaid and NC Health Choice Provider and Health Plan Lookup ToolYou can use the Medicaid and NC Health Choice Provider and Health Plan Lookup Tool to find a PCP. Our new provider search will help you find the best PCP for you and your family.
To search for a provider, go to Find a provider.
Health Care Option GuideYou can use the Health Care Option Guide to view health plans. It will help you choose the best health plan to meet your health care needs.
To view health plans, go to View health plans.
Read Also: How To Apply For Medicaid In Houston
Choices You Have To Make And Tips For Choosing A Plan
Illinois Client Enrollment Services will mail you an enrollment packet. This packet will include a letter saying by what date you need to choose a health plan. If you do not choose a plan by that date, a health plan and Primary Care Provider will be chosen for you. Click here to view samples of all of the materials that will be in your enrollment packet.Once you have picked a PCP and health plan, you will get information about your health plan and your health plan member ID card in the mail. You will use your health plan member ID card to get healthcare services.
Here are some questions to ask yourself that may help you decide which health plan and PCP are right for you.
- Is there a doctor I already like?
- What health plans does my doctor work with?
- Does someone in my family have special needs?
- How far do I want to travel to see my doctor?
- Do I need a doctor who speaks a certain language?
To research the plans and decide which is right for you, go to EnrollHFS.Illinois.Gov for more information. You can also call the plans member services line to learn more about each plan.
For more help choosing a plan and finding a doctor, you can call Illinois Client Enrollment Services at 912-8880 or go online to EnrollHFS.Illinois.Gov.
American Disabilities Act Notice
In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
Read Also: Dentist In Meridian Ms That Accept Medicaid
Unitedhealthcare Senior Care Options Plan
UnitedHealthcare SCO is a Coordinated Care plan with a Medicare contract and a contract with the Commonwealth of Massachusetts Medicaid program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is a voluntary program that is available to anyone 65 and older who qualifies for MassHealth Standard and Original Medicare. If you have MassHealth Standard, but you do not qualify for Original Medicare, you may still be eligible to enroll in our MassHealth Senior Care Option plan and receive all of your MassHealth benefits through our SCO program.
Your Medicaid And Famis Id Cards
Once you or your child are enrolled in Medicaid or FAMIS, you will get a Commonwealth of Virginia health insurance card from the Department of Medical Assistance Services . Each enrolled person in your household will get a card.
If you need a replacement Medicaid ID card, call Cover Virginia at 833-5CALLVA to order a new one. You can also contact your local Department of Social Services .
Members who are in a health plan will also get an ID card from the plan.
You must:
- Make sure the provider accepts Medicaid or FAMIS insurance and accepts your health plan, if you are in one
- Show your cards to the provider each time you get medical, dental, or other covered services
- Pay any required co-pays
If you need a replacement health plan card, call the Managed Care Organization Helpline at 1-800-643-2273. Or contact your health plan to ask for a new card.
Recommended Reading: Dentists In Grand Island Ne That Accept Medicaid
