What Basic Medicare Coverage Means
Itâs good for Mom and Dad to know what basic Medicare covers. Start with Medicare Part A. It typically helps pay the costs of:
- Inpatient hospital care
- Home health care if you are homebound and need skilled care after an inpatient hospital stay
- Hospice care if you are terminally ill and your doctor certifies you need this care.
This isnât a complete list of what Part A may cover.
Medicare Part B helps pay for medical and outpatient services. Medicare Part B covered services generally include:
- Doctor visits
- Lab work, x-rays, and scans
- Speech, physical, and occupational therapies
- Durable medical equipment such as walkers, wheelchairs, and oxygen tanks
- Ambulance services to and from the hospital in an emergency
- Outpatient hospital or clinic care
- Certain medications, usually administered by a physician or in a doctorâs office, such as anti-cancer medications and certain vaccines
This isnât a complete list of what Part B may cover.
How Do I Apply For The Fpbp
You can go to a Family Planning Services Provider for a presumptive eligibility screening and/or to get an FPBP application and enrollment assistance. You may access a list of these locations by visiting our website at Family Planning Program Sites.
If you need your application to remain completely confidential with regard to your residence address, you must clearly tell us this on your application and give us a safe and confidential mailing address and contact phone number so we may reach you if needed to further determine your eligibility for the FPBP
A Few Frequently Asked Questions About What Medicaid Covers
What coverage do pregnant women get under Medicaid?
Pregnant women are covered for all care related to the pregnancy, delivery and any complications that may take place during pregnancy and up to 60 days postpartum.
Pregnant women may also qualify for care that was received for their pregnancy before they applied and received Medicaid. Some states call this Presumptive Eligibility and it was put in place so that all women would start necessary prenatal care as early in pregnancy as possible. Pregnant women are usually given priority in determining Medicaid eligibility. Most offices try to qualify a pregnant woman within about 2-4 weeks.
Does Medicaid cover VSG?
Vertical sleeve gastrectomy, also known as VSG, is surgery to help with weight loss. Medicaid does not cover weight loss surgery in most cases. However, it is best to check with your state on an individual basis to confirm that they do not offer it as a benefit separate from mandatory federal benefits.
Does Medicaid cover dental services?
Medicaid pays for emergency and medically necessary dental work across the country. Medicaid also pays for comprehensive dental care in more than 30 states. However, others may only cover certain categories of treatments. Medicaid does cover dental services for all child enrollees as part of the Early and Periodic Screening, Diagnostic and Treatment benefit. Check with your state to see what your exact level of dental coverage is.
What does Medicaid cover for children?
Recommended Reading: Florida Medicaid Waiver For Developmental Disability
How Much Does It Cost
Medicaid cost $553 billion in fiscal year 2016. Of that amount, $348.9 billion came from the federal government the states paid $204.5 billion.
Medicaid accounts for 9 percent of federal domestic spending. For states, it is the biggest source of federal funding and the second-largest budget item, behind education.
The biggest costs in Medicaid are for the elderly and the disabled, often because of long-term care in nursing homes.
Washington pays 50 to 75 percent of Medicaid costs for most eligible groups, with poor states receiving more money.
Under the Affordable Care Act, the federal government initially covered all of the costs for the roughly 11 million people insured under the laws expansion of Medicaid, who are largely adults without disabilities.
Under the law, Washington picks up 95 percent of state costs for the expansion of Medicaid this year, whittling down to 90 percent in 2020.
What Are My Medicare Coverage Options
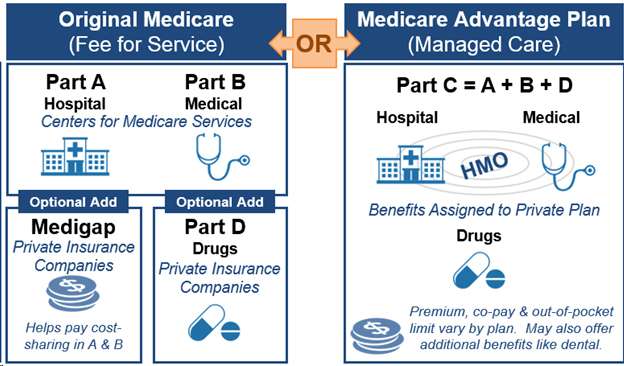
In a nutshell, here are your basic choices for Medicare coverage.
- Stay with Original Medicare and do nothing else. A few things to be aware of:
- You get Medicare Part A premium-free if youâve worked at least 10 years, or 40 quarters, while paying Medicare taxes.
- Most people pay a monthly premium for Medicare Part B. You can decide not to enroll in this part of Original Medicare. Some people âopt outâ of Part B coverage if they have group health coverage through an employer, for example. You can sign up for Part B later when you stop working or your group coverage ends. But you must be enrolled in Part B if you want to sign up for a Medicare Advantage plan or a Medicare Supplement plan. If you delay enrollment in Part B, you might face a late-enrollment penalty for as long as you have the coverage, unless you qualify for a Special Enrollment Period.
- Outside of certain specific situations, Original Medicare doesnât cover prescription drugs. Medicare plan options to cover prescription drugs are discussed below.
- Original Medicare does come with certain out-of-pocket costs. Medicare Part A and Part B have deductibles and sometimes coinsurance, copayments, and certain coverage limits.
Don’t Miss: Kentucky Food Stamps And Medicaid Phone Number
Medicare Part D Coverage
Part D refers to the prescription drug coverage portion of Medicare and each plan has its own set of covered drugs. Additionally, each drug is placed in a designated tier within that plan, which ultimately determines the copayment and/or coinsurance cost of the drug.
To find out the specific medications your plan covers, check with your Medicare provider or read through your individual plan.
Alternatively, if youre taking a particular drug and want to find a Medicare plan offering the best benefits possible for that specific medication, Medicare.gov has a Medicare Plan Finder on its website that helps you locate options to consider.
What Are Other Medicare And Medicaid Assistance Programs
QMB is not the only program available to dual-eligible beneficiaries. Others include:
- The Specified Low-Income Medicare Beneficiary program covers Medicare Part B premiums.
- The Qualified Disabled Working Individual program allows individuals who lost Medicare Part A benefits after returning to work can buy back these benefits under this program.
Dual-eligible beneficiaries may also enroll in a Dual-eligible Special Needs Plan . This is a particular type of Medicare Advantage plan with a benefits package that is tailored to the needs of those with the limited income and resources common among Medicaid recipients.
Special Needs Plans are sold by private insurance companies, so contact a licensed insurance agent for additional information. You can also compare plans online to see if there are Medicare SNPs available where you live.
Recommended Reading: How Much Money Disqualifies You For Medicaid
Basic Health Program Blueprint
The Basic Health Program Blueprint is the form that states must use to make an official request for certification of a Basic Health Program as set forth in 42 CFR 600.110. The Blueprint is intended to collect the program design choices of the state and to provide a full description of the operations and management of the program and its compliance with the federal rules.
Who Is Eligible For The Fpp
- Men and women, ages 12 through 54, who are:
- Iowa residents or
- U.S. citizens or qualified immigrants
- Who meet income limits
Women whose pregnancies and deliveries were covered by Medicaid will have family planning services covered for an additional 12 months without having their eligibility re-determined.
In determining FPP eligibility, the households countable monthly income shall not exceed the amounts shown in the chart below for a household of the same size.
FAMILY PLANNING PROGRAM MONTHLY INCOME LIMITS: 300% OF POVERTY |
|---|
| HH SIZE |
You May Like: Does Medicaid Cover Alternative Medicine
Family Planning Benefit Program
To apply for the Family Planning Benefit Program please bring the items found on the checklist and the completed application form with you to your appointment.
This free program provides family planning services to women and men of childbearing age who meet certain income and residency requirements. The program is funded through Medicaid, but you do not need to be a current Medicaid patient to participate. Many more people can get free services with this program than other Medicaid programs.
In order to be eligible you must meet these requirements:
- Male or female of childbearing age, including teens and college students
- New York State resident that meets satisfactory citizenship or immigration requirements
- Eligible income level
This program provides coverage for family planning-related health care including:
- Most FDA approved birth control methods, devices, and supplies including birth control pills, condoms, the patch, Nuvaring, IUDs and Nexplanon
- Emergency contraception and follow-up care
- Male and female sterilization
- Preconception counseling, preventive screening and family planning options before pregnancy
The following services are also free when they are part of a family planning visit. You MUST have these services as part of or follow up to a family planning visit or they will not be covered by the Family Planning Benefit Program.
Can I Use My Medicaid Coverage In Any State
Home> FAQs> Can I use my Medicaid coverage in any state?
Q. Can I use my Medicaid coverage in any state?
A: No. Because each state has its own Medicaid eligibility requirements, you cant just transfer coverage from one state to another, nor can you use your coverage when youre temporarily visiting another state, unless you need emergency health care.
Medicaid offers health coverage to millions of Americans, and in many states, that coverage matches or even surpasses that of private health insurance. Medicaid is jointly funded by the federal government and state governments, but each state has the option to set its own rules and requirements for eligibility. As such, transferring your Medicaid coverage from one state to another isnt always possible.
Read Also: How Do You Sign Up For Medicaid In Michigan
Unitedhealthcare Dual Complete Plans
Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
Who Is Eligible For Qmb
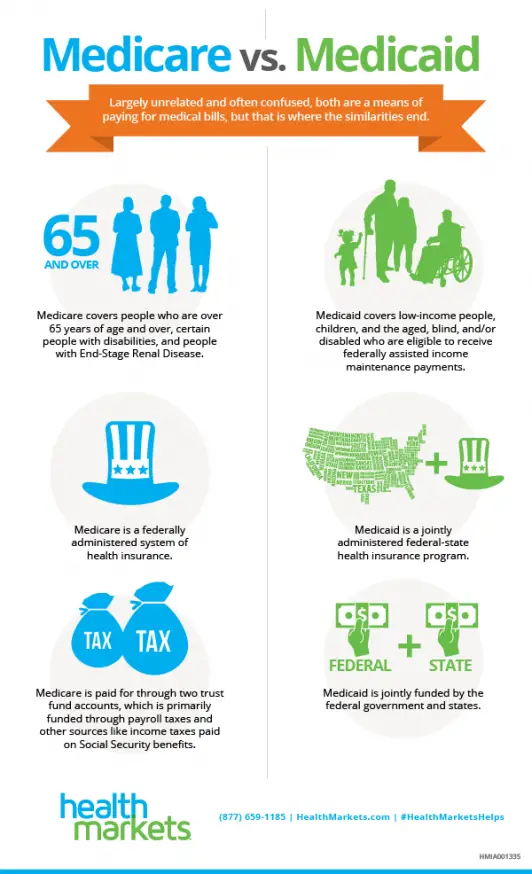
You must be eligible for both Medicare and Medicaid to be eligible for QMB benefits. While Medicares eligibility requirements are federally mandated, each state may set its own qualifying restrictions for Medicaid.
You must also meet the QMB income and resource limits in 2022:
- The individual monthly income limit is $1,094
- The value of an individuals combined resources are capped at $7,970
To apply for the QMB program, contact your state Medicaid program. Please not that if your income or financial resources are close to the totals listed above, you should still apply, as you may potentially be eligible.
Don’t Miss: What Is The Best Medicaid Plan In Ohio
Provider And Facility Guidelines
Medicaid guidelines require all providers to practice within the scope of their State Practice Act. Some states have enacted legislation that requires providers using telemedicine technology across state lines to have a valid state license in the state where the patient is located. Any such requirements or restrictions placed by the state are binding under current Medicaid rules.
What Medicare Does Not Cover
Medicare as a whole covers a wide variety of physical and mental health serviceswhether in whole or in partbut there are some expenses it will not pay toward.Among them are:
- A majority of dental care services, including dentures
- Eye exams needed for prescription glasses
- Hearing aids and fitting exams
- Routine foot care
Read Also: Annual Income Eligibility For Medicaid
What Does Part B Of Medicare Cover
Medicare Part B helps cover medically-necessary services like doctors services and tests, outpatient care, home health services, durable medical equipment, and other medical services. Part B also covers some preventive services. Look at your Medicare card to find out if you have Part B.
The basic medically-necessary services covered include:
- Abdominal Aortic Aneurysm Screening
- Bone Mass Measurement
- Cardiac Rehabilitation
- Durable Medical Equipment
- EKG Screening
- Foot Exams and Treatment
- Glaucoma Tests
- Kidney Dialysis Services and Supplies
- Kidney Disease Education Services
- Outpatient Medical and Surgical Services and Supplies
- Pap Tests and Pelvic Exams
- Physical Exams
- Smoking Cessation
- Speech-Language Pathology Services
- Tests
- Transplants and Immunosuppressive Drugs
To find out if Medicare covers a service not on this list, visit www.medicare.gov/coverage, or call 1-800-MEDICARE . TTY users should call 1-877-486-2048.
How Much Do Part C Part D And Medigap Cost
Medicare Part C, Part D, and Medigap all have varying costs based on your county, ZIP code, and the plan provider you choose.
These plans are purchased through private insurance companies but are required to follow federal guidelines. For that reason, there are caps on associated costs, such as your out-of-pocket maximums, deductibles, and monthly premiums.
For example, for Medicare Part C, your maximum out-of-pocket annual limit for in-network providers is $7,550. If you use both in-network and out-of-network providers, your maximum out-of-pocket annual limit is $10,000.
Many Part C plans have a $0 premium. Others can go as high as $200 a month, or more, which is in addition to your monthly Part B premium.
The national base beneficiary premium for Medicare Part D is $33.37 in 2022. However, this cost can be higher based on your income. Some Part D plans also have a $0 deductible.
Medicare requires you to use Medicare-approved providers and suppliers when you seek medical care. Most doctors in the United States accept Medicare, but there are exceptions. Its always important to ask if your doctor takes Medicare when you make an appointment.
Read Also: Can I Get A Breast Pump Through Medicaid
America’s Foremost Disability Expert
3 Things You Must Know About Social Security Disability Claims
Are you eligible?
Self-help services may not be permitted in all states. The information provided on this site is not legal advice, does not constitute a lawyer referral service, and no attorney-client or confidential relationship is or will be formed by use of the site. The attorney listings on this site are paid attorney advertising. In some states, the information on this website may be considered a lawyer referral service. Please reference the Terms of Use and the Supplemental Terms for specific information related to your state. Your use of this website constitutes acceptance of the Terms of Use, Supplemental Terms, Privacy Policy and Cookie Policy. Do Not Sell My Personal Information
Transferring Medicaid Benefits To Another State
Technically, theres no formal program or option that allows you to transfer your Medicaid coverage from one state to another. Therefore, if youre relocating, youll need to reapply for Medicaid in the new states.
The good news is that youre allowed to apply for Medicaid in your new state immediately after relocating, and doing so can help you avoid a lapse in benefits. It generally takes anywhere from 15 to 90 days to receive a letter of approval once you apply for Medicaid, and you can usually submit your application online.
One thing you should know about Medicaid is that you cant be covered by it in two different states at the same time. Therefore, to transfer your coverage so to speak youll need to first terminate your original Medicaid coverage and then apply in your new state once youve relocated.
Most states offer retroactive Medicaid coverage, which allows you to receive coverage for up to three months prior to the date of your applications approval. However, you may be forced to pay for healthcare services out of pocket until that retroactive coverage kicks in and renders you eligible for reimbursement. To this end, make sure to retain copies of all medical receipts for services received during your coverage gap.
Read Also: Urologist In Baton Rouge That Accept Medicaid
What Does Medicare Part A Cost
Depending on your income, you may have to pay a premium for Part A coverage. If you have worked and paid FICA taxes for 10 years, you pay no premium for Part A. However, You may have to pay copayments or a deductible for any services under Medicare Part A. You can apply for assistance or help if you cant pay.
According to Medicare, in addition to a $1,484 deductible, your 2021 Part A costs include:
- $0 coinsurance for hospitalization days 160
- $371 coinsurance per day for hospitalization days 6190
- $742 coinsurance per day for hospitalization day 91 and beyond for each lifetime reserve day
- all costs for each hospitalization day over your lifetime reserve days
- no charge for the first 20 days of approved skilled nursing facility care
- $185.50 per day for 21100 days of approved skilled nursing facility care
- all costs after 101 days of approved skilled nursing facility care
- no charge for hospice care
For hospital services to be covered by Medicare, you must be approved and receive care in a Medicare-approved facility.
- diabetes supplies
Basic Eligibility Requirements To Get Coverage

The basic requirements to qualify for any Medicaid benefits in Mississippi are:
- You must be a citizen of the United States or a qualified alien.
- You must be a resident of Mississippi.
- You must meet requirements for age and/or disability, income and other Mississippi Medicaid eligibility requirements such as resources for certain aged, blind or disabled coverage groups.
- You must file an application form.
- You must provide requested verification within the allowed time limits.
For more information regarding eligibility, refer to the policies below:
Read Also: Does West Virginia Have Expanded Medicaid
