Michigan Medicaid Eligibility Guidelines
To qualify for Medicaid in Michigan, an individual must meet the eligibility requirements of the program.
There are several Medicaid programs that people in Michigan can be eligible for. Each program has its own income and asset requirements.
However, all applicants must meet the general requirements below in order to qualify for Michigan Medicaid.
Medicaid And Long Term Care Planning
In addition to the above benefits, Medicaid can help cover the costs of long-term care, such as nursing homes. With the cost of long-term care rising quickly, this can be a major concern for many Texans as they, and their family members get older. Because Medicaid eligibility is means-based, many people who cannot afford long-term care may find that they are nonetheless ineligible for Medicaid.
Estate planning attorneys often work with clients to create ways around this problem. Using trusts and other devices, they can often work out ways to maintain a clients eligibility for Medicaid without completely losing access to their assets.
Spending Down Assets To Qualify For Medicaid In Ny
Medicaid has very strict rules that applicants have to abide by in order to qualify. Many of these qualifying rules have to do with your assets and how much you own.
In that sense, Medicaid has strict income and asset requirements, so it can be difficult to know what things you can buy without endangering your Medicaid eligibility.
So we put together this comprehensive article on how you can spend down your assets to qualify for Medicaid . We will also talk about income limits for Medicaid in the state and what kinds of items you can spend down on and not hurt your Medicaid eligibility status. Lastly, we will talk about some strategies on how to protect your income and assets from Medicaid in old age.
Recommended Reading: How To Obtain Medicaid In Florida
Also Check: Is Neurofeedback Covered By Medicaid
Spousal Impoverishment Prevention Coverage
This coverage applies to couples where one needs Nursing Care Services in a facility or at home.
The spouse receiving the nursing care services is allowed $3,000. The spouse who remains in the community is entitled to keep half of the couple’s countable assets, but not less than $26,076 and not more than $130,380 for calendar year 2021.
The spouse receiving the nursing care services may keep up to $65 of their monthly income and may deem income to bring the income of the spouse in community up to $2,550 per month and any dependent household members up to $718.
How Much Is The Federal Poverty Level
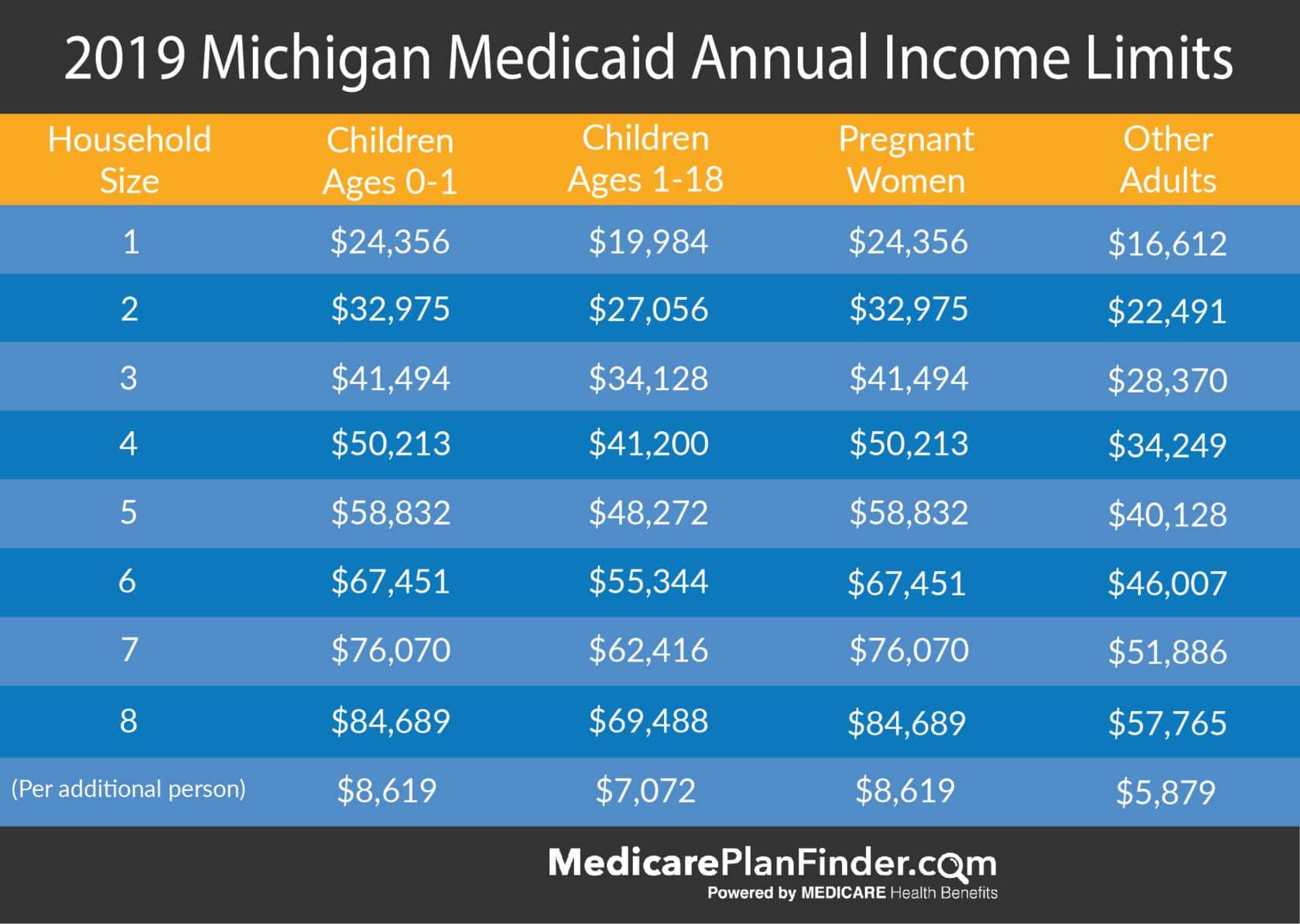
The federal poverty level in 2021 is equal to an income of $12,880 per year for an individual adult, plus $4,540 for each additional household member. Alaska and Hawaii have different benchmarks because of their differing costs of living.
|
Number of people in home |
48 states and Washington D.C. |
Alaska |
|---|
Recommended Reading: Medicaid Doctors In Raleigh Nc
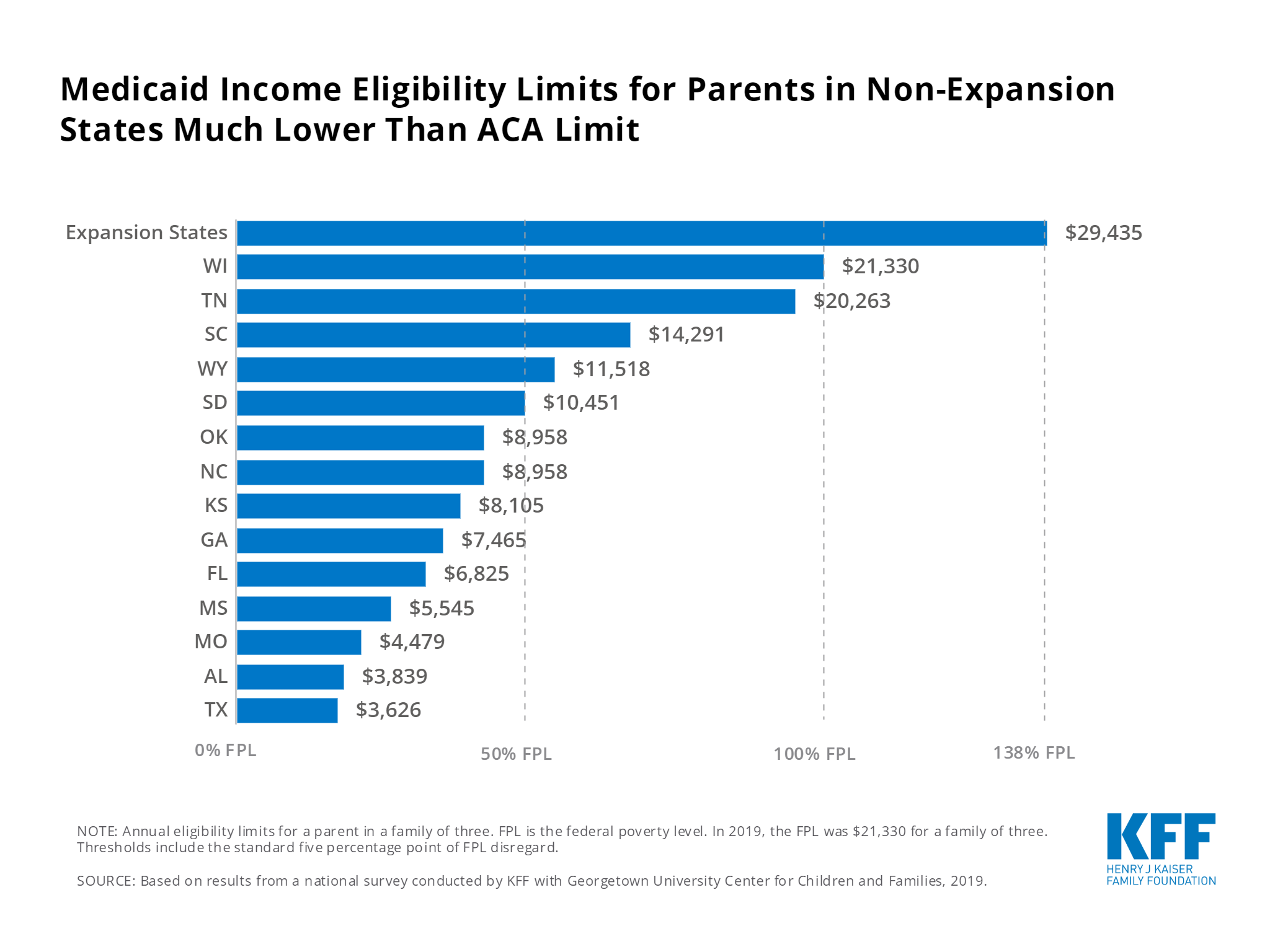
What Is The Lowest Income To Qualify For Medicaid
There are 13 states that do not grant Medicaid access to individuals based on income alone.
Of those that do, only Wisconsin uses a limit lower than 138%. An individual in Wisconsin can make no more than the federal poverty level in order to qualify for Medicaid.
Texas has the lowest income limit to qualify on a family basis, at 17% of the FPL. A two-parent household with one child in Texas can make no more than $37,332 and qualify for Medicaid.
What Money Does The Government Consider Your Income
The income used to determine Medicaid eligibility is called Modified Adjusted Gross Income . Adjusted gross income is the total of all the money you earned during the year minus any allowable tax deductions. MAGI is your AGI plus any untaxed foreign income, non-taxable Social Security benefits, and tax-exempt interest. According to the federal government, for many people MAGI is identical or very close to adjusted gross income. To learn more about calculating MAGI, use this government resource linked here.
As a general rule, if your income is below 138% FPL and your state has expanded Medicaid coverage, you qualify for Medicaid based only on your income. But check with your state-specific Medicaid program to get specific requirements.
Don’t Miss: Do I Make Too Much For Medicaid
What Is Child Health Plan Plus
Child Health Plan Plus is public low-cost health insurance for certain children and pregnant women. CHP+ has different rules for qualifying than Health First Colorado. Some individuals who earn too much for Health First Colorado qualify for CHP+.
CHP+ covers doctor visits, emergency care, preventive care such as screenings and immunizations, and other procedures and treatments. CHP+ can help you and your family get healthy and stay healthy.
What Does CHP+ Cost?
CHP+ costs vary depending on your household size and income. CHP+ members may have to pay an annual enrollment fee. This fee is due within 30 days of your CHP+ approval. If the enrollment fee is not paid within the 30 days allowed then the family will be denied and will need to re-apply. Some CHP+ clients may also have to pay co-pays to their health care provider at the time of service. Pregnant women, American Indians and Alaskan Natives do not have to pay annual enrollment fees or co-pays.
Read Also: What State Has The Best Medicaid Benefits
Texas Medicaid Income Limit
The Texas Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the Texas Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 198 percent of FPL
- Any child age 1-5 with a family income up to 144 percent of FPL
- Children ages 6- 18 with family income up to 133 percent of FPL
- CHIP for children with family income up to 201 percent of FPL
- Pregnant women with family income up to 198 percent of FPL
- Parents of minor children with family income up to 14 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 74% of the FPL
You May Like: Medicaid Provider Id Number Lookup
Medicaid: What Do I Count As Income
Marketplaces, Medicaid, and CHIP all use MAGI to determine a households income for eligibility. MAGI stands for Modified Adjusted Gross Income. The best way to figure it out is to work through the numbers backward.
Start with your gross income, which is your total taxable income. If you have multiple income streams, you add them all together to get your total income. Taxable income may include wages, salaries, bonuses, alimony, self-employment income, pensions, punitive damages, IRA distributions, jury duty fees, unemployment compensation, rents, royalties, severance pay, gambling winnings, interest, tips, and estate or trust income.
You may also be receiving income that is not considered taxable. You do not have to include this income when applying for Medicaid. Types of non-taxable include may include child support, gifts, veterans benefits, insurance proceeds, beneficiary payments, AFDC payments, injury payments, relocation pay, TANF payments, workers compensation, federal income tax refunds, and SSI payments.
Once you know your gross income, you can subtract IRS-approved deductions to get your adjusted gross income . For those that are self-employed, these deductions include any business related expenses. They also include alimony payments, IRA contributions, tuition and fees, student loan interest, and work-related moving expenses.
Income Limits For Medicaid And Chip Programs
Internal Revenue Service rules for Modified Adjusted Gross Income are used to determine countable income and, in some instances, household size. Household gross income is then compared to the limits shown below based on household size for the applicable program. A 5% disregard based on the federal poverty level is applied, if needed, and is reflected in the amounts shown below. Eligibility is determined for Medicaid first, then CHIP using the 5% FPL disregard. The limits below are effective March 1, 2021.
Medicaid for Infants from Birth to Age 1 | 194% FPL
| Family Size |
Recommended Reading: Does Medicaid Cover Spinal Cord Stimulators
How Is Medicaid Qualification Different In Expansion States Vs Non
If you are a resident of one of the states with Medicaid expansion, your income alone can be used to determine eligibility.
To qualify, your monthly income will be considered. However, because some people have income that varies throughout the year, the state must consider your yearly income if you do not qualify with your monthly income. This is important in the case of a seasonal worker who may be over the income limit monthly but under the limit over the course of the year.
Apply For Medicaid Coverage Even If Your State Hasnt Expanded
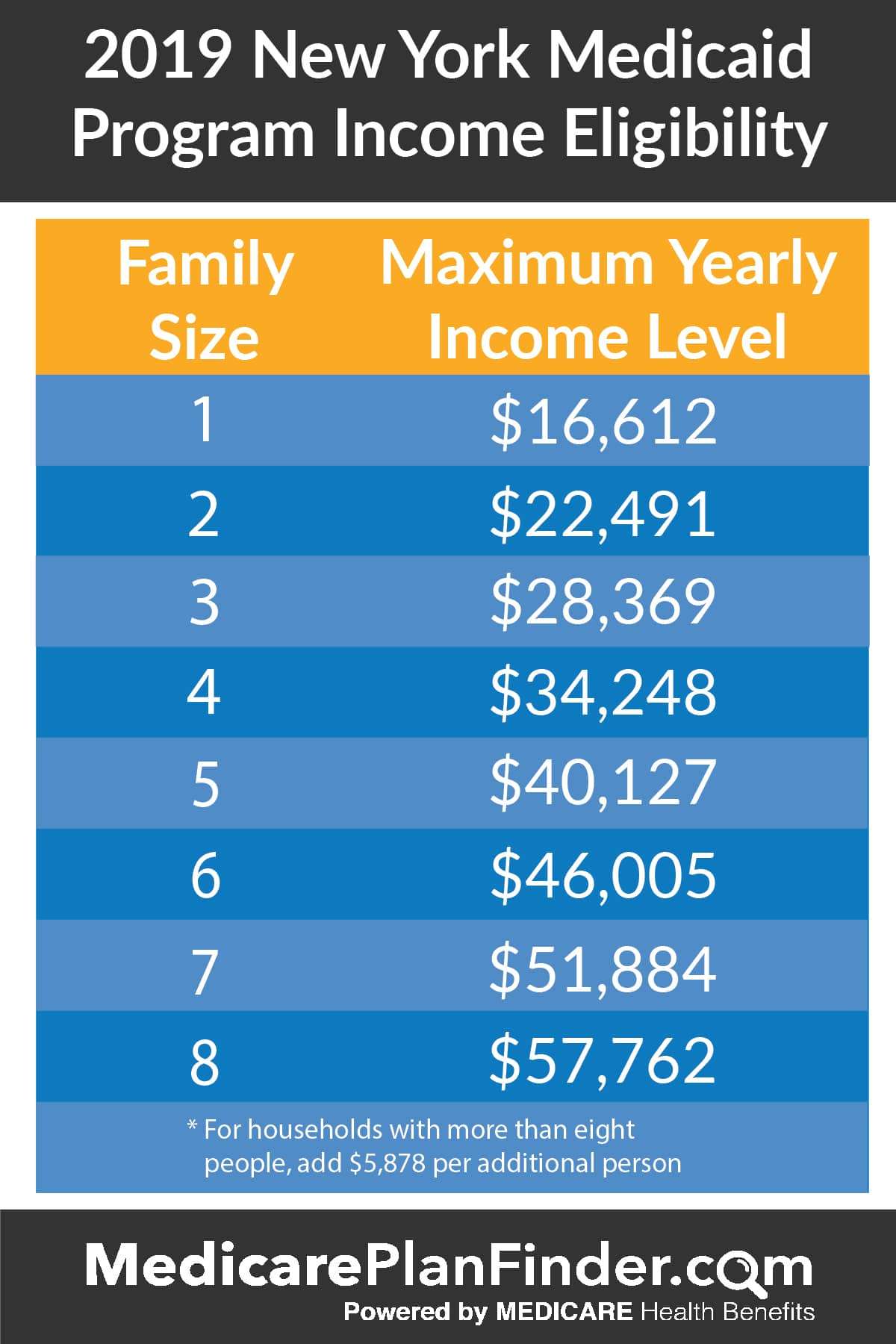
Even if your state hasn’t expanded Medicaid and it looks like your income is below the level to qualify for financial help with a Marketplace plan, you should fill out a Marketplace application.
Each state has coverage options that could work for you particularly if you have children, are pregnant, or have a disability. And when you provide more detailed income information you may fall into the range to save.
Also Check: Do Chiropractors Take Medicaid In Nc
How Do You Calculate Your Medicaid Income Eligibility
Follow these steps to calculate whether or not your income may qualify you for Medicaid:
- Find the FPL for your household using the chart above
- Multiply that number by your states Medicaid income limit found below, and then divide by 100
For example, if there are two people living in your household and you live in Arizona, you would multiply $17,420 by 138 and then divide by 100. That equals $24,039.60.
You may also multiply $17,420 by 1.38.
What Are The Different Types Of Care Available
The Medicaid programs available in each state are: regular Medicaid, Medicaid for long-term nursing home care, and Medicaid for home-based nursing care.
Regular Medicaid is the health care benefits program available to all of a states residents, providing they meet the eligibility requirements. Some of the eligibility requirements include:
- Low-income
- Legal status on the United States
- Resident of the state of application
Those who meet these criteria are able to use their regular Medicaid benefits for their doctors visits, hospital care, laboratory testing, and transportation for medical purposes.
The income limit for regular medicaid will be a set amount, depending on state and marital status. Some states allow one lump sum for a married couple and others have an income limit per spouse.
Medicaid for long-term nursing home care is for those who are elderly and can no longer live independently, those with chronic illness, and people with disabilities. At the facility, the residents receive 24/7 supervision and medical care, as well as lodgings and meals.
All state residents who meet the eligibility criteria and require long-term nursing home care are entitled to and will receive the care. There are no waitlists or lotteries for this benefit and you cant be denied if you meet the eligibility requirements.
Don’t Miss: How Can I Get Medicaid In Florida
What Happens After I Apply For Medicaid In Michigan
After you submit your Michigan Medicaid application, you may be required to attend an interview with a Department of Health and Human Services caseworker.
Whether you will be required to attend an interview depends on your situation:
If you are applying for Medicaid for your child alone, then no interview will likely be required.
If you are applying for any other benefits at the same time, then an interview will likely be required.
During this interview, you will be required to bring documents that prove the information that you provided on your initial Michigan Medicaid application.
Once you complete this interview, you will receive a call or a letter in the mail that will tell you whether you were approved or denied.
If you are denied benefits, you have the right to appeal but that appeal must be filed within a certain timeframe. As your caseworker for details.
What Do I Need For Proof Of Income
In order to prove that you fall within the limit for income eligibility, you will need to provide documentation of all sources of income that you have.
Documents to include are things like pay stubs from wages, copies of social security deposits, copies of alimony checks, and award letters from any other monthly financial benefit that you may receive.
It would also be helpful to have all of your most recent income tax returns and any other tax forms that would be relevant to verifying your income.
Some states are able to electronically gather the resources to verify your income, which does simplify the process as well as eliminate fraud. To find out if your state has this technology for your application, click here to learn more about the application process in your state of residence.
Also Check: Alabama Medicaid Office Birmingham Al
Who Is Eligible For Medicaid In Michigan
In Michigan, there is traditional Medicaid and the Healthy Michigan Plan . HMP started in 2014 as part of the Affordable Care Act. Once you are enrolled, TM and HMP work just like other health insurance.
The following people may qualify for Michigan Medicaid if they meet certain financialrequirements:
- Infants and children under the age of 21
- People who are aged 65 or older
- People who are blind or expected to be disabled for at least a year
- Recipients of Supplemental Security Income
- People who need nursing home care or home and community-based care
- People who are on Medicare
- Individuals who are medically needy
Medicaid Income Eligibility Chart State By State
The following is each of the states, listed alphabetically. Under your state of residence, you will find all of the relevant information regarding the Medicaid Income Eligibility Chart for each of three programs available: regular, in-home nursing care, and institutional nursing care.
Additionally, each of these programs will have additional information about the income limits for those who are single, married with both spouses applying, and married with only one spouse applying.
You May Like: Gastro Doctors That Take Medicaid
Who Is Eligible For Medicaid
You may qualify for free or low-cost care through Medicaid based on income and family size.
In all states, Medicaid provides health coverage for some low-income people, families and children, pregnant women, the elderly, and people with disabilities. In some states the program covers all low-income adults below a certain income level.
- First, find out if your state is expanding Medicaid and learn what that means for you.
- If your state is expanding Medicaid, use this chart to see what you may qualify for based on your income and family size.
Even if you were told you didnt qualify for Medicaid in the past, you may qualify under the new rules. You can see if you qualify for Medicaid 2 ways:
- Visit your states Medicaid website. Use the drop-down menu at the top of this page to pick your state. You can apply right now and find out if you qualify. If you qualify, coverage can begin immediately.
- Fill out an application in the Health Insurance Marketplace. When you finish the application, well tell you which programs you and your family qualify for. If it looks like anyone is eligible for Medicaid and/or CHIP, well let the state agency know so you can enroll.
Also Check: Dental Care That Accepts Medicaid
How Many People Are On Medicaid
According to the Centers for Medicare & Medicaid Services, as of November 2020, here are the number of people enrolled in Medicaid and Chip in the entire United States:
- 78,521,263 individuals were enrolled in Medicaid and CHIP
- 72,204,587 individuals were enrolled in Medicaid
- 6,695,834 individuals were enrolled in CHIP
Dont Miss: Texas Medicaid Application Form For Elderly
Read Also: Does Medicaid Give You A Free Breast Pump
Michigan Medicaid Expansion Update
Michigan expanded Medicaid as of April 2014. The expanded Medicaid program is called Healthy Michigan.
Nearly 750,000 Michiganders are enrolled in expanded Medicaid as of mid-2020, up from about 650,000 before the COVID-19 pandemic began.
In addition, work requirement for Medicaid took effect as of January 2020, but a judge overturned it in March 2020.
University of Michigan researchers reported that the expansion of Medicaid in Michigan resulted in about 30,000 new jobs.
Furthermore, it resulted in a $2.3 billion increase in personal income in the state in 2016.
Are You In Need Of Assistance With Long
Long-Term Services and Supports include services that:
- support individuals who need ongoing care due to age, physical or intellectual disability or chronic illness and
- assist an individual or their caregiver, to live as independently as possible in their homes and communities.
Examples include: meals, transportation, chore services, personal care, counseling, respite for caretakers, adult day health care, benefits counseling, home modifications, assistive technology, etc.
If you would like more information, please take the Assess My Needs survey from the Department of Health and Human Services.
Recommended Reading: Eye Doctors That Accept Straight Medicaid
What Is Nevada Check Up
Nevada Check Up is the State of Nevadas Childrens Health Insurance Program . Depending on your income, your children may qualify for coverage through Nevada Check Up. If you qualify, you will be required to pay a quarterly premium based upon your family size and income, but wont be responsible for things like co-payments and deductibles.
In Nevada, children living in households with an annual income of up to 200% of the federal poverty level may qualify for coverage through Nevada Check Up. This is $50,200 for a family of four.
