Effects On Access To Care
focuses on the outcomes related to access. The top panel shows that the ACA led to statistically significant increases in access to care at the sample mean pretreatment uninsured rate in both Medicaid expansion and nonexpansion states in the postreform period. States that participated in the Medicaid expansion saw a 9.5 percentage point increase in insurance coverage, a 3.4 percentage point increase in reporting having a primary care doctor, and a 5.6 percentage point reduction in the probability of reporting cost being a barrier to receiving care. Results were somewhat smaller in states that refused the Medicaid expansion . The difference between these 2 sets of estimates is also reported in and is due to the Medicaid expansion alone. These results are generally larger than those found by a recent article using BRFSS data and the same identification strategy but only 2 posttreatment years, suggesting larger effects in 2016 than in 2014 and 2015.
How Much Does Obamacare Cost Monthly
The Affordable Care Act will reach record affordability during the 2022 coverage year because of the American Rescue Plan Act of 2021. New financial assistance with premiums means that 4 out of 5 people will be able to find a plan for $10 or less per month.
Your premium, or the amount you might pay monthly for Obamacare, will vary depending upon where you live, your income, your household size, what plan you choose, and the amount of your premium tax credit.
Generally, ACA plans are organized into metal tiers, which determine how you and your plan split the cost of care.
| Has high monthly premiums but low costs when you need care. | |
| Platinum | Has the highest monthly premiums and the lowest costs when you need care. |
According to a Kaiser Family Foundation analysis of marketplace plans nationwide for a 40-year-old person, the average premium for a silver plan in 2022 is $438. The price ranges from $309 in New Hampshire to $762 in Wyoming.
The Aca Protects People With Preexisting Conditions From Discrimination
Prior to the ACA, insurers in the individual market routinely set pricing and benefit exclusions and denied coverage to people based on their health status, a practice known as medical underwriting. Nearly 1 in 2 nonelderly adults have a preexisting condition, and prior to the ACA, they could have faced discrimination based on their medical history if they sought to buy insurance on their own.
The ACA also established guaranteed issue, meaning that insurers must issue policies to anyone and can no longer turn away people based on health status.
The ACA added a number of significant new protections for people with preexisting conditions. One group of reforms involved changes to the rating rules, prohibiting insurers from making premiums dependent on gender or health status and limiting their ability to vary premiums by age. The ACA also established guaranteed issue, meaning that insurers must issue policies to anyone and can no longer turn away people based on health status.
Read Also: How Do I Renew My Ohio Medicaid Benefits Online
Medicaid And Health Outcomes: Necessary But Not Sufficient
Medicaid expansion under the Affordable Care Act represents an important and historic step toward mitigating health insurancerelated disparities, likely improving access, reducing patient financial strain, and possibly improving health status. However, it is important to recognize that even if universally adopted at the state level, the availability of insurance does not guarantee that individuals will ultimately receive high-quality care. Even when insurance is available, patients must enroll and overcome deficiencies in access to covered services, clinicians and institutions, and deficiencies in access to high-quality primary care and specialty services . In this regard, Medicaid is typically underfunded compared with private insurance, leading to deficiencies that may curb its ability to eliminate insurance-related disparities.
How Many People Are Enrolled In Coverage Due To Medicaid Expansion
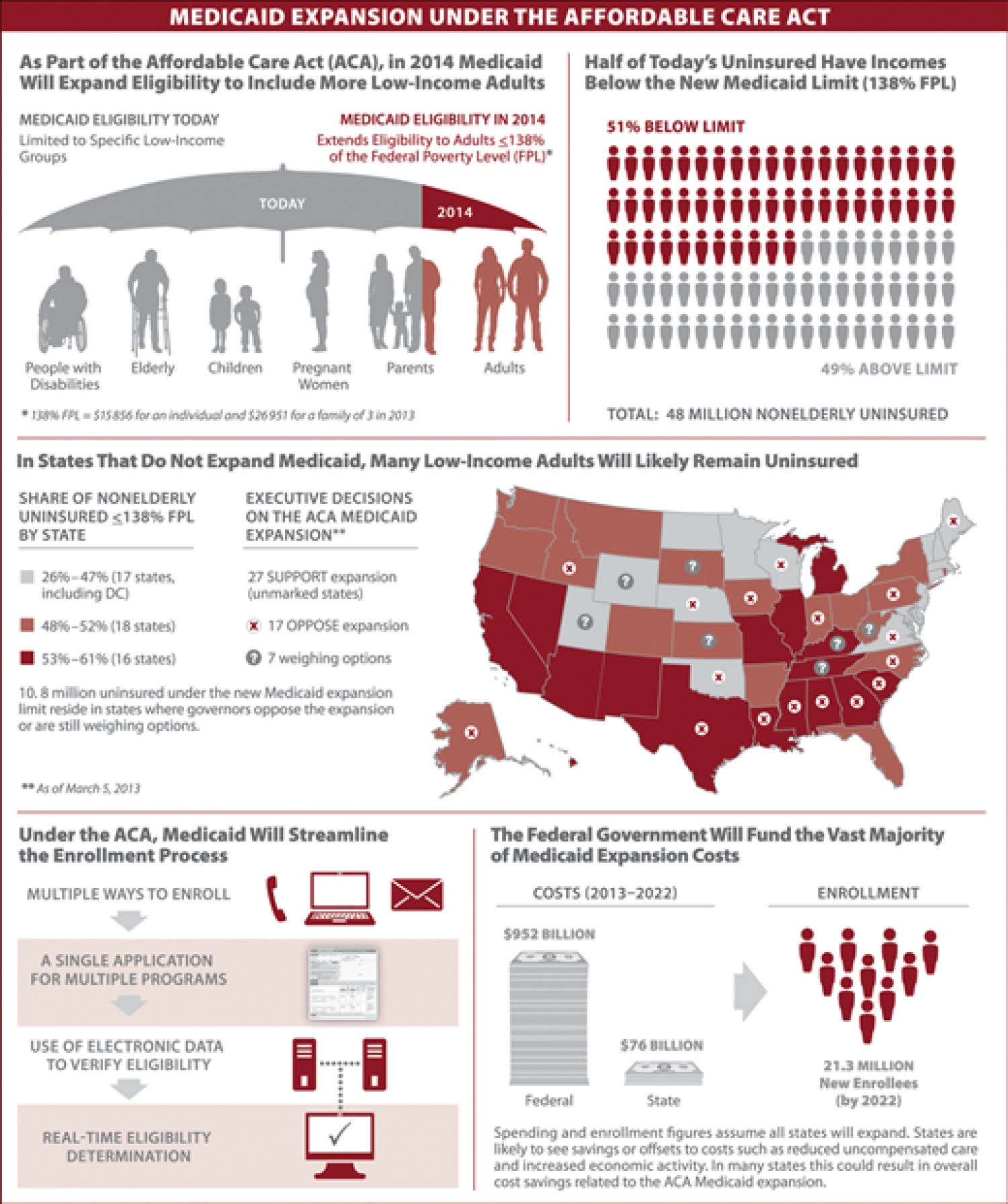
As of 2019, there were about 10 million people who had become newly eligible for Medicaid due to the ACAs expanded eligibility guidelines. But the COVID pandemic drove the enrollment numbers significantly higher: As of 2021, there were about 14.8 million Medicaid enrollees who had gained eligibility due to Medicaid expansion, plus another 4 million who were already eligible for Medicaid under pre-ACA rules, but who had enrolled due to outreach and enrollment assistance efforts since the ACA was implemented.
Total enrollment in Medicaid/CHIP has increased by 44% since 2013, and that includes the dozen states that continue to reject federal funding to expand Medicaid.
Also Check: What Does It Take To Get Medicaid
Getting People Covered And Helping Them Stay Covered
APIAHF leverages a considerable network of national and community-based partners throughout the country to support continued enrollment efforts through culturally and linguistically appropriate strategies. We work with federal and state policymakers to ensure that policies and programs meet the needs of AA and NHPIs and other immigrant communities.
In 2012, APIAHF co-founded Action for Health Justice with the Association of Asian Pacific Community Health Organizations , Asian Americans Advancing Justice Los Angeles, Asian Americans Advancing Justice AAJC and 72 federally qualified health centers and community based organizations. Across three enrollment periods, Action for Health Justice outreached and educated nearly 1 million AAs and NHPIs in 56 different languages, helping to substantially lessen the coverage gap in these populations.
Million Fewer Americans Are Uninsured
The ACA generated one of the largest expansions of health coverage in U.S. history. In 2010, 16 percent of all Americans were uninsured by 2016, the uninsured rate hit an all-time low of 9 percent. About 20 million Americans have gained health insurance coverage since the ACA was enacted. The ACAs coverage gains occurred across all income levels and among both children and adults, and disparities in coverage between races and ethnicities have narrowed.
Nationwide, 11.4 million people are enrolled in plans for 2019 coverage through the ACA health insurance marketplaces.
Two of the biggest coverage expansion provisions of the ACA went into full effect in 2014: the expansion of Medicaid and the launch of the health insurance marketplaces for private coverage. Together, these programs now cover tens of millions of Americans. Nationwide, 11.4 million people are enrolled in plans for 2019 coverage through the ACA health insurance marketplaces. Medicaid expansion currently covers 12.7 million people made newly eligible by the ACA, and the ACAs enrollment outreach initiatives generated a welcome-mat effect that spurred enrollment among people who were previously eligible for Medicaid and CHIP.
You May Like: Does Medicaid Cover More Than Medicare
Medicare And The Affordable Care Act
The Affordable Care Act was signed into law on March 23, 2010. Its goals were to provide greater access to health care coverage, to improve the quality of health care services provided, and to slow the rate of increase in health spending.
As far as Medicare is concerned, the Affordable Care Act primarily made improvements to preventive services and prescription drug coverage, which ultimately lowers the out-of-pocket costs for millions of senior citizens.
Ways The Aca Has Improved Health Care In The Past Decade
The health care law provides coverage for millions of Americans and protects people with preexisting conditions, but it remains under threat from a Trump administration-backed lawsuit.
- Emily Gee
- Maura Calsyn
Ten years ago this month, the Affordable Care Act was signed into law. Since then, the law has transformed the American health care system by expanding health coverage to 20 million Americans and saving thousands of lives. The ACA codified protections for people with preexisting conditions and eliminated patient cost sharing for high-value preventive services. And the law goes beyond coverage, requiring employers to provide breastfeeding mothers with breaks at work, making calorie counts more widely available in restaurants, and creating the Prevention and Public Health Fund, which helps the Centers for Disease Control and Prevention and state agencies detect and respond to health threats such as COVID-19.
The consequences of ACA repeal would be dire:
As the nation awaits a final ruling on the lawsuit, the Center for American Progress is celebrating how the ACA has helped the American people access affordable health care in the past decade. In honor of the laws 10th anniversary, here are 10 ways in which it has changed Americans lives for the better. Each of these gains remains at risk as long as the Trump administration-backed lawsuit remains unresolved.
Also Check: What Is The Difference Between Medicare & Medicaid
Deficiencies In Essential Health Benefits Package
The Affordable Care Act includes an essential health benefits package, which establishes a comprehensive set of the minimum necessary services that a Medicaid expansion plan must provide . The Affordable Care Act mandates coverage in the 10 essential health benefits categories. Coverage is thus assured for the majority of services commonly performed and billed by pulmonary and critical care providers. However, states ultimately have discretion to determine how many services within each of the 10 categories their Medicaid plans will cover, which may lead to significant state-to-state variability in benefits. Furthermore, newly eligible groups may not receive benefits as comprehensive as traditional Medicaid, provided they cover at least 1 service within each of the 10 categories .
Children’s Health Insurance Program
The Children’s Health Insurance Program was signed into law in 1997 and provides federal matching funds to states to provide health coverage to children in families with incomes too high to qualify for Medicaid, but who can’t afford private coverage. All states have expanded children’s coverage significantly through their CHIP programs, with nearly every state providing coverage for children up to at least 200 percent of the Federal Poverty Level .
Read Also: What Is The Website To Apply For Medicaid
Executive Order On Strengthening Medicaid And The Affordable Care Act
Section 1. Policy. In the 10 years since its enactment, the Affordable Care Act has reduced the number of uninsured Americans by more than 20 million, extended critical consumer protections to more than 100 million people, and strengthened and improved the Nations healthcare system. At the same time, millions of people who are potentially eligible for coverage under the ACA or other laws remain uninsured, and obtaining insurance benefits is more difficult than necessary. For these reasons, it is the policy of my Administration to protect and strengthen Medicaid and the ACA and to make high-quality healthcare accessible and affordable for every American.
Sec. 3. Immediate Review of Agency Actions. The Secretary of the Treasury, the Secretary of Labor, the Secretary of Health and Human Services, and the heads of all other executive departments and agencies with authorities and responsibilities related to Medicaid and the ACA shall, as soon as practicable, review all existing regulations, orders, guidance documents, policies, and any other similar agency actions to determine whether such agency actions are inconsistent with the policy set forth in section 1 of this order. As part of this review, the heads of agencies shall examine the following:
policies or practices that may undermine protections for people with pre-existing conditions, including complications related to COVID-19, under the ACA
JOSEPH R. BIDEN JR.
Temporary Assistance For Needy Families
A program administered under North Dakota Century Code Chapter 50-09 and Title IV-A of the Social Security Act. References to TANF include TANF Kinship Care Assistance, Diversion Assistance, and Transition Assistance.
Title II of the Social Security Act .
Title IV-D of the Social Security Act .
Title IV-E of the Social Security Act .
Title XVI of the Social Security Act ).
Title XIX of the Social Security Act .
You May Like: Dentist That Take Medicaid Nj
The Affordable Care Act
One of the most drastic policy changes in the last 50 years, the Affordable Care Act had a number of effects on the healthcare system. It’s constantly under scrutiny from lawmakers and healthcare experts and is often subject to changes. See ACA news for current policy updates.
Terms to be familiar with while perusing this site:
Affordable Care Act Terms
-
Individual Mandate: a tax penalty that individuals must pay if they do not have health insurance. Exceptions are made for individuals that would pay more than 9.5% of their income in premiums.
-
Health Insurance Marketplace: government created platforms that offer subsidized commercial health insurance plans for eligible Americans .
-
Federal Poverty Level : federally calculated income levels calculated based on household size and cost of living. Determine Medicaid eligibility and commercial insurance subsidies
-
Medical Loss Ratio: the portion of health insurance premiums that insurance companies spend on health care cost versus administrative costs
Consequences Of Nonparticipation In State Medicaid Expansion
In states that fail to expand access to Medicaid there is a significant probability that millions of lower-income parents and childless adults will remain without health insurance. Paradoxically, many states choosing not to expand Medicaid coverage potentially have the most to gain as they have a relatively greater proportion of residents without health insurance . Many uninsured individuals in these states are low-income, do not have access to employee-based coverage, and will remain ineligible for their states current Medicaid coverage after reform. Furthermore, their incomes will be too low to qualify for health insurance premium credits, which would otherwise offset the expense of purchasing insurance coverage through state insurance exchanges. These individuals are left in a coverage gap where they are ineligible for both subsidies to facilitate the purchase of private insurance because their income is too low and ineligible for Medicaid because their income is too high. Although subsidies are not required to purchase insurance through the exchange, the cost of purchasing coverage without premium credits will likely remain prohibitive for those in this coverage gap, as the average premium for a 40-year-old adult is $224 per month for the most basic bronze plan .
Also Check: How To Switch Providers On Medicaid
Texas Loses Billions To Treat The Poor By Not Expanding Medicaid Advocates Say
“If that is not getting states to move, then that suggests that the deep root of their hesitation is not about financial constraint,” says Jamila Michener, a professor of government at Cornell University and author of the book Fragmented Democracy: Medicaid Federalism And Unequal Politics.
Instead, Michener says, the reluctance among some Republican-led legislatures and governors to expand Medicaid may be a combination of partisan resistance to President Obama’s signature health law, and not believing “this kind of government intervention for these groups of people is appropriate.”
What’s Next: When asked about progress on this front in an April press briefing, Biden’s press secretary Jen Psaki said “the President is certainly supportive of and an advocate for states expanding Medicaid,” but did not answer a follow up about whether the White House was directly reaching out to governors regarding this option.
The Department Of Human Services And The Affordable Care Act
Most people in Hawaii have health care coverage through their employment or through Medicare or Medicaid. However, there were some people who fell through the cracks.
The federal Affordable Care act gave states permission to open their local Medicaid programs to more low-income people. The state of Hawaii fully implemented the Affordable Care Act and expended Medicaid eligibility to more individuals. In addition, the ACA provided support for a new electronic eligibility system that lets people apply and enroll for Medicaid online and manage their own accounts. Starting in January 2016, DHS will maintain the call center and outreach and enrollment services for Hawaiis state-based insurance marketplace.
Medicaid is a federal/state partnership with shared authority and financing. The program covers nearly 50 million low-income Americans, including more than 386,000 Hawaii residents. States must meet minimum federal requirements such as covering families with children and offering certain benefits. States also may provide optional expanded coverage.
Under the ACA, states had the option to open Medicaid to more people. Hawaii chose to do so. Under that 2014 expansion any adult under 65 years of age with qualified residency or citizenship and income under 138% federal poverty level , will be eligible for Medicaid irrespective of their assets.
For an FAQ about Medicaid, go here:
You May Like: Difference Between Obamacare And Medicaid
Option : Get Around Stubborn States By Letting Cities Expand Medicaid
Instead of centralizing the approach, this next idea goes even more local. The COVER Now Act, introduced by Rep. Lloyd Doggett, D-Texas, would empower local jurisdictions to expand Medicaid. So, if you live in Austin, Texas, maybe you could get Medicaid, even if someone in Lubbock still couldn’t.
The political and logistical challenges would be tough, policy analysts say. Logistically, such a plan would require counties and cities to create new infrastructure to run a Medicaid program, Rudowitz notes, and the federal government would have to oversee how well these new local programs complied with all of Medicaid’s rules.
“It does not seem feasible politically,” Michener says. “The legislators who would have to vote to make this possible would be ceding quite a bit of power to localities.” It also might amplify geographic equity concerns, she says. People’s access to health insurance would not just “be arbitrarily based on what state you live in which is the current state of affairs It’s also going to be arbitrary based on what county you live in, based on what city you live in.”
What’s next: Doggett introduced the bill earlier this month. There’s no guarantee it would get a vote on the House floor and even if it did it wouldn’t survive a likely filibuster in the evenly divided Senate.
Will The Affordable Care Acts Expansion Of Medicaid Remedy Insurance
One can gain insight into the expected impact of Medicaid expansion from prior observational and quasi-experimental analyses of health insurance expansion in the United States . Massachusetts initiated health insurance reform in 2006 in a comprehensive program that includes many provisions incorporated in the Affordable Care Act, including the majority of new insurance beneficiaries obtaining insurance through Medicaid expansion. In Massachusetts, health insurance reform was associated with an increase in primary care use , a decrease in use of the emergency department for low-severity conditions and nonurgent conditions , and a concomitant decrease in overall hospitalizations for preventable conditions . Massachusetts health insurance reform was also associated with an increase in outpatient surgical referrals among lower income racial/ethnic minorities in the postreform period . There was also a significant reduction in the number of critically ill patients without health insurance in Massachusetts after health insurance reform. Despite this reduction, intensive care unit use as measured by intensive care unit admissions per capita or intensive care unit admissions per hospitalization was unchanged, and there were no changes in mortality or use of postacute care facilities among patients admitted to the intensive care unit .
You May Like: Can You Have Both Medicare And Medicaid
