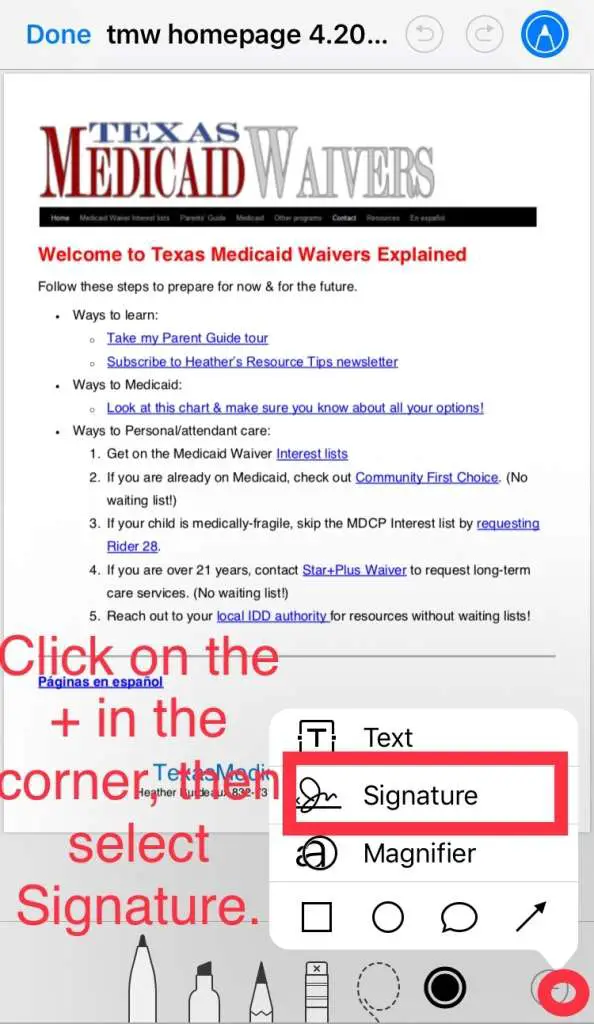
Requesting An Account Closure
SNAP recipients are free to request an account closure at any time if they no longer want to receive benefits. Call your local social services agency and inform them of your wishes or mail a request. Don’t forget to include your name, address, account number and date. If you have any questions before you take this step, contact the SNAP information hotline at 800-221-5689. The hotline has prompts in both English and Spanish.
How To Cancel Your Food Stamp Account
The Supplemental Nutrition Assistance Program, or SNAP, isn’t designed for individuals and families to receive food benefits forever, but just until they are able to get back on their feet. Once you no longer need the extra help, you can close out your food stamp account. There are several ways to go about canceling the account. Choose the one that best fits your circumstances.
What If I Think A Decision You Make Is Unfair Incorrect Or Made Too Late
You have the right to appeal the Medicaid decision. There are several ways to request an appeal. You can write the reason you disagree with the decision on the back of the decision letter and then mail or fax it to Medicaid as directed on the letter. You can also fax the decision letter to the Division of Administrative Law at 225-219-9823 or mail it to the Division of Administrative Law, Department of Health Section, P. O. Box 4189, Baton Rouge, LA 70821-4183. You can request an appeal by phone by calling Medicaid Customer Service at 1-888-342-6207 or the Division of Administrative Law at 225-342-5800.
Also Check: West Virginia Medicaid Provider Enrollment
Review Your Options And Stay Covered
Losing Medicaid coverage can be very scary and shocking at first, especially if you have ongoing health issues.
If you are dealing with losing Medicaid, remember that it is not the end of the road. You have multiple options. Keep both your healthcare needs and budget in mind when making a decision about how to move forward. And if you end up at the hospital without insurance coverage, there are options even in that situation.
No matter what path you choose to follow once youre denied Medicaid or you are dropped from Medicaid, the most important thing to do is to obtain some type of coverage. The physical and financial safety that you get from having health insurance can end up being well worth any cost.
American Disabilities Act Notice
In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
You May Like: Will Medicaid Pay For Braces For Adults
Who Is Eligible For Medicaid In Louisiana
Depending on the reason for eligibility, low-income Louisiana residents can qualify for Medicaid based on income alone, or a combination of income and assets. Eligibility is based only on household income for children, pregnant women, parents of minor children, and childless adults up to age 64 . But for the aged, blind, and disabled, eligibility rules are more stringent, with both income limits and asset limits.
What Are The Qualifications To Receive Medicaid
Medicaid beneficiaries generally must be residents of the state in which they are receiving Medicaid. They must be either citizens of the United States or certain qualified non-citizens, such as lawful permanent residents. In addition, some eligibility groups are limited by age, or by pregnancy or parenting status.
Read Also: Dentist Buffalo Ny That Accept Medicaid
Will Medicaid Provide Payment For A Family Member Who Needs Nursing Home Care
Louisiana’s Medicaid Program provides payment for special long term care support services, as well as full Medicaid health coverage, to eligible people who, because of their medical condition, require assistance with activities of daily living . Long-term care supports may be provided either in a facility or in an individual’s own home or in the community. Visit Medicaid Long-Term Care.
Do You Get A Refund If You Cancel Insurance
If youve sold your vehicle and have car insurance with us, you should let us know because you might be entitled to a refund of unused premiums when you cancel your policy. If your vehicle is insured in NSW, QLD, ACT or TAS, you can cancel your policy online. In some cases, additional cancellation fees may apply.
Don’t Miss: Pediatricians In Amarillo Tx That Accept Medicaid
If You Or Your Loved Ones Have Been Impacted By Hurricane Ida
UnitedHealthcare is helping members who may be affected by severe weather and flooding from Hurricane Ida. If you need help with things like getting to and from the doctors office or filling a prescription early, please call member services at , TTY 711.
Helpful Frequently Asked Questions can be viewed here. Behavioral Health Resources can be viewed here.
A free emotional-support help line is also available to everyone at , TTY 711 and is open 24 hours a day, seven days a week. The service is free of charge and open to anyone. Trained Optum mental health specialists can help you manage stress and anxiety.
Due to high call volumes to The Department of Children and Family Services, you may experience longer than expected wait times when calling the hot line. To make sure all calls are answered, call times have been extended and two additional days have been added this week. This applies to all – people with last names A-Z, not just a segment of the alphabet.
How Can I Get Trained On The New System
Provider There are training videos available for Provider Portal use. These can be found on the Medicaid Eligibility and Enrollment web site here:
Medicaid applicant or enrollee There is a training video on the self-service portal on the Medicaid Eligibility and Enrollment web site here: . This video shows you what you can do in the self-service portal.
Applicants and enrollees that need additional assistance can call the Medicaid Customer Service Unit at #1-888-342-6207. They can also visit a regional office or a certified Medicaid Application Center for in-person assistance.
Also Check: How Do You Apply For Medicaid In Ny
Letting Benefits Close Naturally
Another option is to simply let your benefits end naturally, with no action on your part. There are two situations when this can occur. First, you may be close to a re-certification and you want to forgo the re-certification interview and the associated paperwork. Failure to supply the required information results in the agency closing out your food stamp account. Second, you can report changes that would put you over the maximum income and resource limit, so that when the social worker reviews the new information, she will adjust the amounts in the system. The system then determines that you are no longer eligible for benefits, and you will receive a notice of account closure in the mail.
New Medicaid Eligibility And Enrollment System Launched In November 2018
In November 2018, Louisiana rolled out a new Medicaid eligibility and enrollment system that allows for real-time eligibility determinations using data from state and federal systems, instead of relying on manual eligibility determinations. And enrollees no longer receive phone calls from Louisiana Medicaid when their coverage is up for renewal notices and requests for additional information will be sent by mail instead, and the system was set up to require enrollees to provide updated information in a timely manner in order to avoid termination of their coverage.
However, in August 2019, the state temporarily suspended the program that would terminate Medicaid coverage for people who dont respond to requests for updated information. And when the COVID pandemic began several months later, Medicaid eligibility redeterminations ground to a halt nationwide. The Families First Coronavirus Response Act, enacted in March 2020, provides states with additional federal Medicaid funding, but on the condition that enrollees cannot have their coverage terminated for the duration of the COVID public health emergency .
You May Like: Does Medicaid Cover Cochlear Implants
Louisiana Hhs Director Pushes To Keep Medicaid Expansion
On January 5, 2016, Edwards named Dr. Rebekah Gee to be the director of Louisianas Department of Health and Hospitals, which is the agency that oversees the states Medicaid program. Edwards said that Medicaid expansion would be one of Gees primary tasks, and Gee noted that the state would need to hire almost 250 people to process enrollments and manage the expansion of Medicaid.
Gee also said that Edwards administration would focus on working with doctors to ensure that there would be an adequate network of providers willing to work with the influx of new Medicaid patients gaining coverage under Healthy Louisiana.
Gee noted that in addition to the states portion of the cost of coverage for the newly eligible population, the state also had to pay 25% of the cost of hiring the 248 new state employees to handle the additional volume in the Medicaid program. The federal government would pay 75% of that cost, but the states portion was expected to be $2 million. Gee said that she was aware of the budget problems that were inheriting, calling them humbling but noting that the new administration had plans to deal with the budget issues.
How Can I Find A Doctor That Accepts Medicaid
For Healthy Louisiana plan members, contact the member services department with questions about how to access care.
For information on dental benefits please contact your dental plan.
For members enrolled with MCNA Dental call 1-855-702-6262 .
For Legacy Medicaid members, call 1-877-455-9955 to find a specialist in your area.
It is important to remember that not all doctors who are active in the Medicaid program are taking new patients. When you call for an appointment, be sure to ask if the doctor is taking new Medicaid patients.
Read Also: Does Princeton House Accept Medicaid
How Does Medicaid Work
The Medicaid program does not provide health care services for everyone. Your application will be reviewed for all Medicaid programs. If you are found eligible for Medicaid, you will get:
- A letter in the mail from Medicaid telling you about your coverage
- A Medicaid ID card
- A Healthy Louisiana plan ID card, if you enroll in a plan.
Each time you go to your health care provider or pharmacy, take your Medicaid ID and Healthy LA plan ID cards with you. Show them at all medical visits before you receive any service. The health care provider or pharmacy will tell you if they accept your Medicaid benefits. You should also ask your health care provider or pharmacy if the service or prescription is covered by Medicaid before receiving the service or filling a prescription.
Medicaid does not pay money to you instead, it sends payments directly to your health care provider or pharmacy.
You May Get A Notice From The Marketplace
If our records show youre enrolled in both a Marketplace plan with premium tax credits or other cost savings and Medicaid or CHIP something we check a few times a year you may get a notice in the mail that lists the household members who are enrolled in both kinds of coverage. The notice explains what to do next.
Take action within 30 days
Update your Marketplace application to show youre not enrolled in Medicaid or CHIP, or end your Marketplace coverage with premium tax credits or other cost savings by the date indicated on your initial warning notice .
If you dont take action:
- The Marketplace will end the advance payments of the premium tax credit and any extra savings being paid on your behalf for your share of the Marketplace plan premium and covered services
- Youll still be enrolled in your Marketplace plan without financial assistance and will be responsible for paying the full cost of your share of the Marketplace plan premium and covered services
If you want more information about Medicaid or CHIP, or if you arent sure if you or others in your household are enrolled in Medicaid or CHIP, you can contact the office in your state:
- For CHIP, visit www.insurekidsnow.gov, or call 1-877-543-7669
Also Check: Molina Medicaid Michigan Prior Authorization Form
What Is Healthy Louisiana
Healthy Louisiana is the way most of Louisiana’s Medicaid recipients receive health care services. As soon as you or family members are eligible for Medicaid, you need to choose a Healthy Louisiana Health Plan to manage your or your family members health care. If you do not choose a health plan, Healthy Louisiana will choose one for you or your family. Compare health plans to find the best plan for you. If you have questions, call Healthy Louisiana at 1-855-229-6848 .
What Are The Benefits Of The New System
The new system includes advanced new tools that will enhance customer service, improve efficiency and strengthen the integrity of the Medicaid program. Specifically, this includes:
- Real-time verification connections to state and federal databases will provide more data for real-time verification of citizenship, income, disability and lawful presence in the United States. Applicants can potentially learn of eligibility determinations within minutes.
- More self-service opportunities for applicants and case management options for enrollees, including being able to report changes in contact information online and request a replacement Medicaid card.
- Consistent enforcement of Medicaid eligibility policy through more automated processes. Starting in January, the new system will automatically terminate coverage for those who fail to respond to requests for information that have been mailed to the enrollees primary address. This new automated closure process does not include long-term care recipients.
- Reduced paper work. Streamlined and automated processes, as well as new online services will reduce paperwork and lessen the likelihood of important documentation being lost or misplaced.
- Refocused Priorities for Medicaid Staff. Instead of working through cumbersome manual processes that require entry into several different systems, Medicaid staff will be able to focus on individual client needs and cases.
Also Check: What Does It Take To Get Medicaid
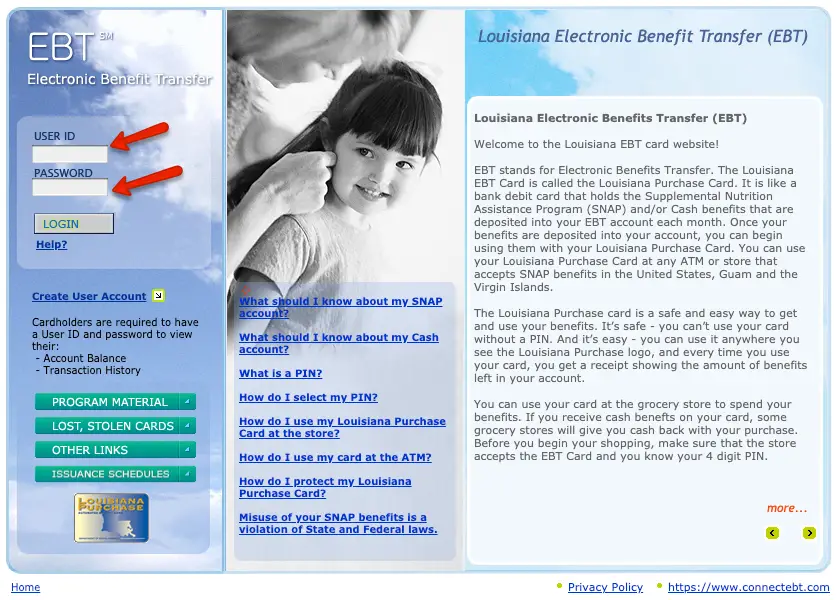
How Do I Report An Address Change
Call Medicaid Customer Service toll free at 1-888-342-6207 or go online by visiting the Medicaid Self-Service Portal to update your address.
If you do not have an online account, you can create an account at any time. Creating an online account allows you to check the status of your application, report any household changes, report an address change, request a replacement Medicaid ID card, and renew your Medicaid benefits.
Louisiana Has Accepted Federal Medicaid Expansion

- 1,745,824 Number of Louisianans covered by Medicaid/CHIP as of May 2021
- 726,037 Increase in the number of Louisianans covered by Medicaid/CHIP fall 2013 to May 2021
- 50% Reduction in the uninsured rate from 2010 to 2019
- 71% Increase in total Medicaid/CHIP enrollment in Louisiana since late 2013
You May Like: Dental Care That Accepts Medicaid
Medicaid / Healthy Louisiana
Louisiana Receives Approval for Unique Strategy to Enroll SNAP Beneficiaries in Expanded Medicaid CoverageWednesday, June 1, 2016 Contact: Samantha Faulkner 225.342.9010,
Baton Rouge, La. Yesterday, the U.S. Department of Health and Human Services announced that Louisiana has received final federal approval to enroll residents in Medicaid using data from the Supplemental Nutrition Assistance Program , more commonly known as food stamps. With this approval, Louisiana has become the first state in the country to receive approval to both determine Medicaid income eligibility and enroll people receiving SNAP benefits using this special fast-track enrollment process.
The authority granted by the Centers for Medicare and Medicaid Services allows the state to enroll individuals who are certain to be eligible for Medicaid without the need for a full Medicaid application because the financial eligibility requirements for Medicaid and SNAP are nearly identical and non-financial eligibility requirements are also already met.
Governor John Bel Edwards thanked CMS for expediting the approval of the state plan amendment, the formal request to make a change to the Medicaid program, to allow for the automatic enrollment of SNAP enrollees, as it will allow more people to get health care coverage as soon as July 1.
Questions and Answers
Will This New System Slow Down Or Delay Applications And Renewals
The new system is designed for more efficient and accurate Medicaid eligibility determinations. However, as workers adjust to a new system and technical issues are addressed, expect some service delays and longer wait times on our toll-free line.
Some Medicaid applications will also take longer to process because states are now required to collect additional information to verify eligibility.
The new system has been thoroughly tested, but there will be some technical and business process issues we may need to fix or refine after it is launched. We have rapid-response teams and processes in place to resolve issues, minimize inconveniences and ensure applicants and enrollees get the services they need as quickly as possible.
The modern system we have implemented includes new automated processes and program integrity measures to ensure that applicants and enrollees are, in fact, eligible. As a result, some people may be denied coverage when they apply and others may lose benefits at renewal because they do not meet eligibility requirements.
- Although this may cause understandable frustration, in most cases, the system will be working exactly as it was designed.
- To minimize surprises, please remember to always make sure that Medicaid has the most current contact information and that the household and income information provided is accurate and complete.
Don’t Miss: Medicaid Brooklyn Ny Phone Number
Wellhop For Mom & Baby
Connect with other expectant moms. Get support and information during your pregnancy and after you deliver. This program is part of your health plan and there is no extra cost to you.Heres how it works:
- Join video conversations every other week with women who have similar due dates and a group leader.
- Chat and share experiences with moms from your group on the Wellhop app or website.
- Visit the Wellhop library. Youll find articles, videos and more.
