What Are Dual Health Plans
Dual health plans are designed just for people who have both Medicaid and Medicare. Theyre a special type of Medicare Part C plan. Dual health plans combine hospital, medical and prescription drug coverage. Youll keep all your Medicaid benefits. Plus, you could get more benefits than with Original Medicare. And you could get it all with as low as a $0 plan premium.
View the “Do I Lose My Medicaid Benefits?” article.
How Effective Is Medicaid
Medicaid is very effective in providing health insurance coverage to the most vulnerable. Since the ACAs major coverage expansions took effect in 2014, Medicaid has helped to reduce the number of uninsured from 45 million to 29 million. If Medicaid did not exist, most of the tens of millions of Medicaid enrollees would be uninsured. This is because private health insurance is generally not an option for Medicaid beneficiaries: many low-income workers do not have access to coverage for themselves and their families through their jobs and cannot afford to purchase coverage in the individual market. The creation of Medicaid, subsequent expansions of Medicaid coverage to children and pregnant women in the 1980s and 1990s, and the most recent expansion of Medicaid coverage to low-income adults under the ACA all have led to significant drops in the share of Americans without health insurance coverage.
Medicaid is also effective in improving access to care, in supporting financial stability among low-income families, and in improving health outcomes. Some of the clearest evidence comes from the ACA expansion of Medicaid coverage to low-income adults, which provides a recent natural experiment, letting researchers compare outcomes in states that did and did not adopt the expansion.
Most Medicaid Enrollees Get Care Through Private Managed Care Plans
Over two-thirds of Medicaid beneficiaries are enrolled in private managed care plans that contract with states to provide comprehensive services, and others receive their care in the fee-for-service system . Managed care plans are responsible for ensuring access to Medicaid services through their networks of providers and are at financial risk for their costs. In the past, states limited managed care to children and families, but they are increasingly expanding managed care to individuals with complex needs. Close to half the states now cover long-term services and supports through risk-based managed care arrangements. Most states are engaged in a variety of delivery system and payment reforms to control costs and improve quality including implementation of patient-centered medical homes, better integration of physical and behavioral health care, and development of value-based purchasing approaches that tie Medicaid provider payments to health outcomes and other performance metrics. Community health centers are a key source of primary care, and safety-net hospitals, including public hospitals and academic medical centers, provide a lot of emergency and inpatient hospital care for Medicaid enrollees.
Figure 6: Over two-thirds of all Medicaid beneficiaries receive their care in comprehensive risk-based MCOs.
Also Check: Utah Medicaid Mental Health Providers
Where Can I Find Companion Care
Dr. Rx
Spend time finding the right personeven if you feel desperate for help. Remember, the safety and security of your loved one is at stake: They will be in your seniors home alone, possibly driving them around, and providing close care. Involve your senior in the process, check references, and ask the hard questions at the front end. Dr. Wegner
Many agencies that provide home health care also offer companion services. Typically, you can find private caregivers through word-of-mouth or local organizations.
Local religious and other organizations may have home visitation services, where they send volunteer visitors. The national organization, Senior Corps, trains volunteers over age 55 to offer companion care. You can also find local organizations that work with Senior Corps. Also, check with the National Association of Area Agencies on Aging for local companion care services.
Everything Medicare Covers Around The House: Home
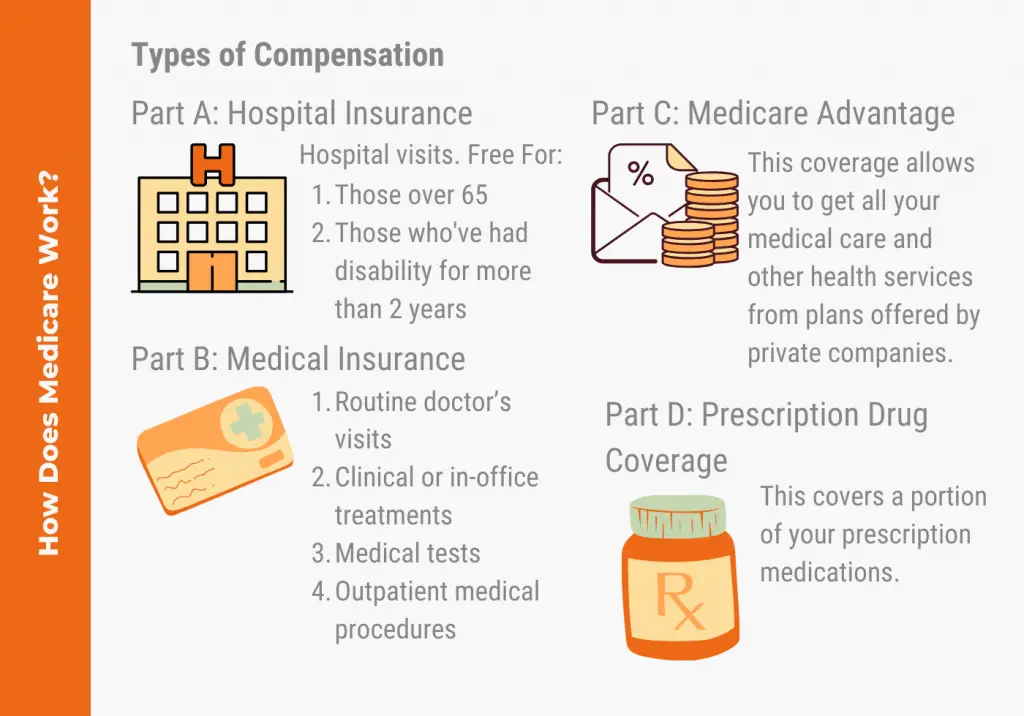
Chronically ill seniors enrolled in certain Medicare Advantage plans could be eligible for better indoor air quality equipment and home modifications such as grab bars, The safely items covered by this benefit include: Shower/bathtub grab bar Tub stool or transfer bench Commode rails Elevated toilet
Dont Miss: Does Medicare Medicaid Cover Assisted Living
You May Like: Does Family Planning Medicaid Cover Mammograms
Medicare Vs Medicaid Compare Benefits
In the context of long term care for the elderly, Medicares benefits are very limited. Medicare does not pay for personal care . Medicare will pay for a very limited number of days of skilled nursing . Medicare will also pay for some home health care, provided it is medical in nature. Starting in 2019, some Medicare Advantage plans started offering long term care benefits. These services and supports are plan specific. But they may include:
- Adult day care
How Do The Benefits Differ
Private insurance and original Medicare plans provide varying benefits and coverage.
Most of both types of plans cover hospital care and outpatient medical services, including doctors visits, physical therapy, and diagnostic tests.
However, Medicare may have gaps in coverage that private insurers cover. For example, Medicare does not cover prescription drugs, meaning that a person needs to get a Medicare Part D plan. However, private insurance plans often include prescription drug coverage.
Medicare Advantage plans, which replace original Medicare, may offer coverage that more closely resembles that of a private insurance plan. Many Medicare Advantage plans offer dental, vision, and hearing care and prescription drug coverage.
You May Like: Pregnancy Medicaid Florida Phone Number
To View This Video Please Enable Javascript And Consider Upgrading To Aweb Browser Thatsupports Html5 Video Does Medicaid Cover Air Purifiers
Medicare does not cover air purifiers under most plans unless it is deemed DME .However, some plans and health insurance providers may consider reimbursing you for an air purifier if it is proven to be medically necessary.
Furthermore, Medicaid may reimburse you for an air purifier as long as it is prescribed and medically necessary.
You must provide proof of necessity, such as a prescription or, even better, a Letter of Medical Necessity.
National Federation Of The Blind Vs Centers For Medicare And Medicaid Services
What happened in 2016 to change Medicare for the blind? Three blind beneficiaries decided to challenge how Medicare information is provided to those who are blind or have low vision.
The National Federation of the Blind partnered with these three beneficiaries and aimed to make a change among the Centers for Medicare and Medicaid Services
This dispute brought attention to those who are Medicare-eligible and blind and highlighted that they are not provided with equal access to Medicare information. They explained that there was a lack of materials available to someone who was blind or had vision loss.
Recommended Reading: Does Social Security Automatically Sign You Up For Medicare
Also Check: Yearly Income To Qualify For Medicaid
Does Medicaid Pay For Assisted Living Communities
Your parent would qualify for Medicaid if they have a low income and few assets besides their home. Medicaid is funded partly by the government and partly by the states. Thats why qualifications for an individual to receive this type of coverage varies.
Many people wonder about Medicaid assisted living coverage. Almost all state Medicaid programs will cover some assisted living costs for eligible residents. However, similar to Medicare, Medicaid does not pay for the cost of living in an assisted living community.
For qualified seniors, Medicaid does pay for these assisted living services:
- Nursing care
- Medical exams
What Does Medicaid Not Cover
Medicaid is a healthcare program that assists individuals or families with minimal resources and also provides much-needed assistance for individuals requiring long-term medical care. Contrary to Medicare, a social insurance program that typically covers some care for people aged 65 years or older, Medicaid covers an assortment of healthcare-related costs for people of all ages.
You May Like: Family Doctors In Charleston Wv That Accept Medicaid
How Does Medicaid Affect Work Incentives
Medicaid supports work, evidence shows. Most Medicaid beneficiaries who can work do so: two-thirds of non-elderly adults enrolled in Medicaid who dont receive federal disability benefits live in a family with at least one worker. Moreover, one recent study found that people in states with more generous Medicaid eligibility levels and benefits are more likely to leave a job for another position with greater growth potential. This research suggests that comprehensive Medicaid coverage can support work and help beneficiaries take advantage of promising job opportunities without worrying about losing their coverage.
In 2018, the Trump Administration began encouraging states to take Medicaid coverage away from people who are not working or participating in work-related activities for a specified number of hours each month. In Arkansas, the first state to implement such a policy, more than 18,000 individuals lost coverage in the first seven months, before a federal court blocked the policy. Researchers found no significant increases in employment, number of hours worked, or overall rates of community engagement activities among those subject to the work requirement.
Medicaid Coverage Has Evolved Over Time
Under the original 1965 Medicaid law, Medicaid eligibility was tied to cash assistance or federal Supplemental Security Income starting in 1972) for parents, children and the poor aged, blind and people with disabilites. States could opt to provide coverage at income levels above cash assistance. Over time, Congress expanded federal minimum requirements and provided new coverage options for states especially for children, pregnant women, and people with disabilities. Congress also required Medicaid to help pay for premiums and cost-sharing for low-income Medicare beneficiaries and allowed states to offer an option to buy-in to Medicaid for working individuals with disabilities. Other coverage milestones included severing the link between Medicaid eligibility and welfare in 1996 and enacting the Childrens Health Insurance Program in 1997 to cover low-income children above the cut-off for Medicaid with an enhanced federal match rate. Following these policy changes, for the first time states conducted outreach campaigns and simplified enrollment procedures to enroll eligible children in both Medicaid and CHIP. Expansions in Medicaid coverage of children marked the beginning of later reforms that recast Medicaid as an income-based health coverage program.
Figure 3: Medicaid has evolved over time to meet changing needs.
You May Like: Will Medicaid Pay For Assisted Living In Ohio
How Much Does Pace Cost
If an older adult has Medicaid, they wont have to pay a monthly premium for the long-term care portion of the PACE benefit.
If they dont qualify for Medicaid, but do have Medicare, theyll pay a monthly premium to cover the long-term care portion of the PACE benefit and a premium for Medicare Part D drugs.
If an older adult doesnt have Medicare or Medicaid, they have the option to pay for the PACE monthly premium out of pocket.
With PACE, there are no co-pays, deductibles, or coverage gaps.
But seniors may have to pay out of pocket for any care received outside the program that isnt approved by their PACE healthcare team.
To qualify for PACE, a person must:
- Be age 55 or older
- Live in a PACE service area
- Be certified by the state to need nursing home level care
- Be able to live safely in their home with PACE services
For example, a typical PACE participant is an 80 year old woman with eight medical conditions who needs help with three activities of daily living. And almost half of PACE participants have been diagnosed with dementia.
The good news is that even though these older adults need a high level of care, more than 90% of PACE participants are able to continue to live in their homes with the programs support.
Aged & Disabled Federal Poverty Level Program
If you are aged or disabled and are not eligible for the SSI program, you may be able to get Medi-Cal through the Aged & Disabled Federal Poverty Level program. To qualify, you must:
This Medi-Cal program uses SSI countable income rules as well as a few extra rules you should know. For more information, visit the Medi-Cal section of the Disability Benefits 101 website.
Don’t Miss: Does Medicaid Cover All Pregnancy Costs
Why Did I Get Denied For Medicaid
Theres a multitude of reasons why someone may get denied for Medicaid coverage. Aside from not meeting the financial or demographic requirements, some common reasons for a denied Medicaid application include:
- Incomplete application or documents
- Failure to respond to a request within a timely manner
- Late filing
- Disability not proven or otherwise not medically qualified
Dont forget that mistakes can be made on behalf of Medicaid, and you have a right to appeal Medicaids decision concerning your coverage. Contact your state Medicaid program for instructions about how to appeal a decision if you are denied benefits.
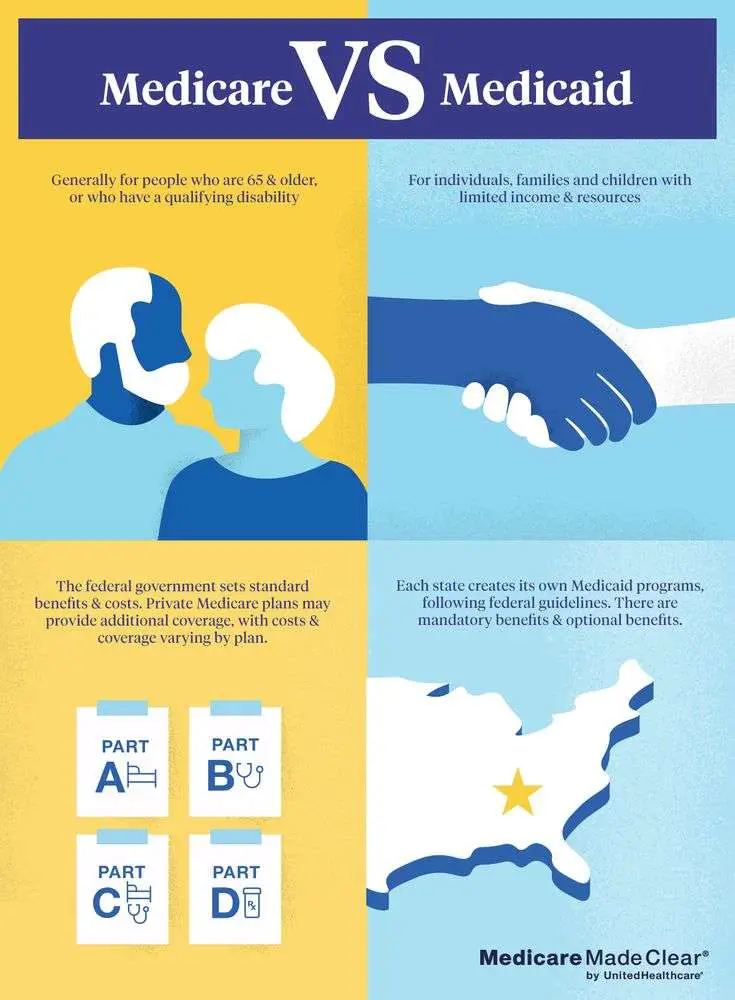
What Is Medicare Vs Medicaid
Medicare
- A federal health insurance program for people who are:
- 65 or older
- Under 65 with certain disabilities
- Of any age and have End Stage Renal Disease or Amyotrophic Lateral Sclerosis
Medicaid
A joint federal and state program that helps pay health care costs for certain individuals and families with limited income and resources.
Also Check: Dentists In Grand Island Ne That Accept Medicaid
Medicare Vs Medicaid: Differences And Costs
TheStreet
Medicare and Medicaid both come from the same government cradle, but are much different when it comes to health care coverage.
Medicare and Medicaid are two government health care insurance programs created in 1965 as part of President Johnson’s “Great Society” to help older Americans and impoverished Americans get good health insurance, but that’s where the similarity ends.
Both government-backed health care insurance programs deliver coverage to U.S. individuals, but under different plan funding, different plan management, and different plan products.
How can you tell the difference between Medicare and Medicaid? Start by understanding what each program does, and how each program works, and go from there.
How Are My Health Care Costs Reimbursed If I Have Medicare And Medicaid
When dual eligible beneficiaries have healthcare expenses, Medicare pays first and Medicaid pays last. But this is not the case for things Medicare doesnt cover, like long-term care. If Medicaid is covering a beneficiarys long-term care, Medicare will still be the primary payer for any Medicare-covered services like skilled nursing care or physical therapy.
Although it is less common, if a dual eligible individual has additional coverage then Medicare pays first, Medigap will pay second, and Medicaid is the last payer for their claims .
Also Check: Choose A Health Plan Medicaid
Opting For Part A Only
Some people choose only to have Medicare Part A coverage so that they dont have to pay the monthly premiums for Medicare Parts B and D. If you still have insurance through a current employer , you can add the other parts later with no penalty.
However, if you decline Parts B and D and don’t have another insurance plan in place, you’ll face a late enrollment penalty when you add the other parts later.
In the past, Medicaid programs typically didn’t offer a lot of choice in terms of plan design. Today, most states utilize Medicaid managed care organizations . If there’s more than one MCO option in your area of the state, you will likely be given the option to select the one you prefer.
Does Medicaid Cover Home Care

Medicaid is a bit less black and white than Medicare because it is administered by the states. Therefore, the state you live in determines which home care services are covered and what eligibility requirements you must meet. In general, you can expect that if you qualify for Medicaid in your state, some level of home care will be covered.
Did You Know: In some states, family members can be paid by Medicaid for providing personal care to their aging loved one.2
To find out whether you are eligible for Medicaid home care and which services are available to you, find your state’s Medicaid profile on Medicaid’s Home & Community Based Services page. Then, contact your state’s Medicaid department directly.
Also Check: Does Medicaid Cover Weight Loss Pills
Who Is Eligible For Medicaid
Medicaid is an entitlement program, which means that anyone who meets eligibility rules has a right to enroll in Medicaid coverage. It also means that states have guaranteed federal financial support for part of the cost of their Medicaid programs.
In order to receive federal funding, states must cover certain mandatory populations:
- children through age 18 in families with income below 138 percent of the federal poverty line
- people who are pregnant and have income below 138 percent of the poverty line
- certain parents or caretakers with very low income and
- most seniors and people with disabilities who receive cash assistance through the Supplemental Security Income program.
States may also receive federal Medicaid funds to cover optional populations. These include: people in the groups listed above whose income exceeds the limits for mandatory coverage seniors and people with disabilities not receiving SSI and with income below the poverty line medically needy people and other people with higher income who need long-term services and supports and thanks to the Affordable Care Act non-disabled adults with income below 138 percent of the poverty line, including those without children. The ACA was intended to extend coverage to all such adults, but a 2012 Supreme Court decision gave states the choice of whether to expand their programs.
Differences In Dental And Vision Care
Medicare parts A and B do not include dental care like cleanings, fillings, getting teeth pulled, dentures, dental plates, or other dental items. Medicaid may cover dental care for adults in some states as well as treatment in others. This varies by state but can be a big plus over Medicare alone.
In certain cases, Medicare Part A may cover dental care if received in a hospital. Most times this would not include your standard dental care.
Medicaid, on the other hand, only covers dental care for children.
Eye exams or glasses may be covered by Medicaid in most states. Medicare may include a basic vision test as part of Part B care in the first preventive visit or the yearly wellness visit.
Read Also: Does Medicaid Cover Therapy In Michigan
