Assistance For Children With Severe Disabilities
If you are a parent caring for a child with a severe disability, you may be able to receive financial support through the Assistance for Children with Severe Disabilities Program.
This program provides financial support for low-income to moderate-income families to cover some of the extra costs of caring for a child who has a severe disability.
You can apply for ACSD:
- by contacting your local office
Have You Or Your Spouse Worked For At Least 10 Years At Jobs Where You Paid Medicare Taxes
Generally, youre first eligible to sign up for Part A and Part B starting 3 months before you turn 65 and ending 3 months after the month you turn 65.
Avoid the penalty If you dont sign up when youre first eligible, youll have to wait to sign up and go months without coverage. You might also pay a monthly penalty for as long as you have Part B. The penalty goes up the longer you wait to sign up. How much is the Part B late enrollment penalty?
What Benefits Does Pregnancy Medicaid Provide
Similar to other health care assistance programs, Medicaid does not pay monetary benefits directly to covered participants. Certain health care providers and health care facilities have a contract with Medicaid to treat those who are covered by Medicaid insurance.
When receiving Medicaid benefits, you should be given a list of medical providers who accept Medicaid or given a website to look for a provider in your area. As long as you receive care from a Medicaid provider, your health care costs will be submitted through Medicaid and will be covered. Pregnant women are covered for all care related to the pregnancy, delivery and any complications that may occur during pregnancy and up to 60 days postpartum.
Additionally, pregnant women also may qualify for care that was received for their pregnancy before they applied and received Medicaid. Some states call this Presumptive Eligibility and it was put in place so that all women would start necessary prenatal care as early in pregnancy as possible.
Talk with your local office to find out if you qualify for presumptive eligibility.
Pregnant women are usually given priority in determining Medicaid eligibility. Most offices try to qualify a pregnant woman within about 2-4 weeks. If you need medical treatment before then, talk with your local office about a temporary card.
Don’t Miss: Blue Cross Blue Shield Texas Star Medicaid
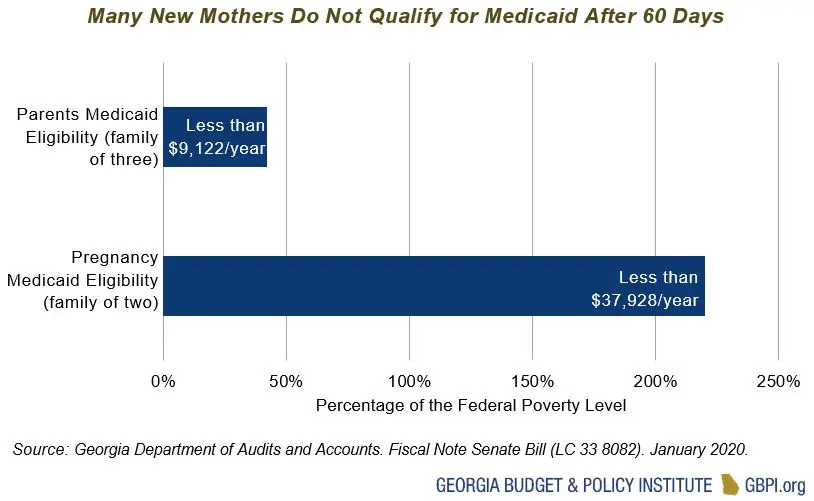
Maternal Deaths After 60 Days
According to the federal Centers for Disease Control and Prevention, nearly 23% of pregnancy-related deaths after the day of delivery occur in the period between six weeks after delivery and the end of the first year.
Yet for most pregnant women who receive health coverage through Medicaid, those benefits end 60 days after delivery, leaving them without health insurance during a still precarious postpartum period.
That 60-day cutoff is based on a false belief that pregnancy-related complications end then, said Dr. Charlene Collier, an OB-GYN at the University of Mississippi Medical Center in Jackson, Mississippi, and chair of the states Mortality Review Committee, which tracks maternal deaths in the state. Now we know those complications extend through the end of the first year.
How Long Does Medicaid Cover Baby After Birth
- Find out how long your newborn baby can be covered by Medicaid after they’re born and learn the answers to other common questions about Medicaid and childbirth.
If you’re pregnant or hoping to become pregnant, you might be wondering how long Medicaid covers baby after birth. Thankfully, newborn babies are automatically covered under their mothers’ Medicaid plans. Read on to find out how long babies are covered and how Medicaid coverage works during pregnancy.
Read Also: Rehabs In Florida That Take Medicaid
Sign Up: Within 8 Months After You Or Your Spouse Stopped Working
Your current coverage might not pay for health services if you dont have both Part A and Part B .
Avoid the penalty & gap in coverageIf you miss this 8-month Special Enrollment Period, youll have to wait to sign up and go months without coverage. You might also pay a monthly penalty for as long as you have Part B. The penalty goes up the longer you wait to sign up. How much is the Part B late enrollment penalty?
What Is Medicaid For Pregnant Women
With Medicaid for pregnant women, you get full health care benefits during your pregnancy and for two months after your babys birth. Medicaid may also cover your medical bills for the three months before you enroll. You also get dental benefits during your pregnancy. Dental services are through the Smiles for Children program. For help finding a dentist or to learn more, call Smiles For Children at 1-888-912-3456. Also read the Guide to Dental Coverage.
Also Check: Medicaid Eligibility Income Chart Florida
Form For Applying For Medicaid
If you haven’t already, apply for Medicaid to see if you’re eligible for coverage. Please refer to the above-mentioned requirements for Medicaid before applying. Most applicants apply online, but there is an option to get a paper application as well. Listed below is the Medicaid application for Alabama residents.
This form was created by the Alabama Medicaid Agency for Alabama residents that can be accessed here.
How Much Does Medicaid Cover For Pregnancy
If you’re pregnant and enrolled in a Medicaid or CHIP plan, you’ll have coverage for prenatal medical care, labor and delivery and any medically necessary services you receive during that time. Federal regulations stipulate that all states must provide coverage for inpatient and outpatient hospital care during pregnancy. Other mandatory benefits include:
- Nurse midwife services
Don’t Miss: Find Primary Care Doctor Medicaid
What Is Covered By Medicaid
Medicaid provides a variety of different services for different populations. Listed below are some of the services provided by Medicaid to various populations.
· Low-income families: prenatal care and delivery costs, routine medical visits and specialized care for children, coverage for unexpected emergencies
· Disabled individuals: assisted care, in-home therapy, speech/occupational therapy, physician services, prescription drugs
· Seniors : nursing home care, personal care, and community-based care, Medicare beneficiary
Medicaid is beneficial for the elderly population as it provides them with coverage for long-term care that is not provided through Medicare.
Rural America Has A Maternal Mortality Problem Midwives Might Help Solve It
Hospitals are shutting down across rural America, creating a shortage of care.
The CDC data also underscores the gaping disparity in maternal mortality between White and Black women. The number of pregnancy-related deaths per 100,000 live births for White women is 13 for Black women, its more than three times higher, at nearly 43.
The leading causes of deaths immediately after the end of pregnancy also were different than those occurring months later, the CDC analysis revealed. For women who died between the seventh and 42nd days after pregnancy, strokes and infection were among the leading causes of death. Women who died later were more likely to succumb to cardiomyopathy, a disease of the heart muscle that can lead to heart failure. Other prevalent causes at that stage were embolisms and other cardiovascular conditions.
Many OB-GYNs also say postpartum depression often doesnt emerge until weeks after delivery.
Yet many women who receive health benefits through Medicaid during pregnancy lack coverage both before pregnancy and for most of the first year after delivery.
What I see constantly in the communities I care for is a normal process, said Ebony Marcelle, director of midwifery at Community of Hope, a community health center in Washington, D.C. You get the 60 days, and youre dropped.
Read Also: Montefiore Medicaid Office Bronx Ny
Medicaid For Pregnant Beneficiaries Extended To 12 Months After Birthnew Legislation Extends Medicaid For Pregnant Beneficiaries From 60 Days To 12 Months After Birth Effective April 1 2022
Effective April 1, 2022, NC Medicaid coverage for pregnant beneficiaries will extend to the last day of the month in which the 12-month postpartum period ends. The change is made pursuant to NC Senate Bill 105 Session Law 2021-180 Section 9D.13 and the American Rescue Plan Act of 2021. These laws are in effect through March 31, 2027.
- All Medicaid beneficiaries who are pregnant and have benefits in a program that covers the birth of the child will be able to access full coverage Medicaid benefits for the duration of pregnancy and the extended 12-month postpartum period. For example, Medicaid for Pregnant Women will now cover dental services for the full 12-month postpartum period after the day of delivery.
- Prior Authorization guidelines currently in place to limit services related to pregnancy and to other conditions that may complicate pregnancy will be removed.
Beneficiaries who are in their current 60-day postpartum period on April 1, 2022, will be extended for the remainder of the 12-month period following the date the pregnancy ends.
Coverage for the 12-month postpartum extension does not apply for those beneficiaries with Emergency Medicaid.
A future Medicaid provider bulletin will be published once the 1E-5, Obstetrical Services Policy is finalized and posted.
Can An Uninsured Woman Enroll In A Public Health Insurance Plan Upon Becoming Pregnant

Yes, women who meet the eligibility criteria for Medicaid or Childrens Health Insurance Program can enroll in one of these public programs at any point during pregnancy:
Full-Scope Medicaid
A pregnant woman is eligible for full-scope Medicaid coverage at any point during pregnancy if eligible under state requirements. Eligibility factors include household size, income, residency in the state of application, and immigration status. An uninsured woman who is already pregnant at the time of application is not eligible for enrollment in expansion Medicaid.
Pregnancy-Related Medicaid
If household income exceeds the income limits for full-scope Medicaid coverage, but is at or below the states income cutoff for pregnancy-related Medicaid, a woman is entitled to Medicaid under the coverage category for pregnancy-related services and conditions that might complicate the pregnancy. The income limits for pregnancy-related Medicaid vary, but states cannot drop eligibility for this coverage below a legal floor that ranges from an income of 133% to 185% of FPL , depending on the state. States are permitted to set a higher income cutoff.
Childrens Health Insurance Program
Recommended Reading: Medicaid Eligibility For Nursing Home Care
Pregnant Women And Infants
Healthy Connections provides coverage to pregnant women with low income. This coverage for the mother continues for 60 days after the baby’s birth. The infant is covered up to age one.
A woman who may qualify for this program must:
- Be pregnant
- Be a South Carolina resident
- Be a U.S. citizen or Lawful Permanent Resident Alien
- Have a Social Security number or verify an application for one
Individuals who are eligible will receive all Medicaid covered services.
Apply online or complete the following form and submit it electronically to , by mail to SCDHHS-Central Mail, P.O. Box 100101, Columbia, SC 29202-3101 or to your .
The Omnibus Budget Reconciliation Act of 1986 gave states the option to provide Medicaid coverage to pregnant women with low income.
What Changes When A Woman Already Enrolled In Medicaid Becomes Pregnant
Generally, nothing. A woman who was previously eligible and enrolled in full-scope Medicaid who becomes pregnant continues to be eligible, and will be able to access pregnancy services. A woman who becomes pregnant while enrolled in Medicaid Expansion can stay in that coverage, at least until redetermination. The state must inform the woman of the benefits afforded to pregnant women under other coverage categories, such as pregnancy-related Medicaid, and provide the option to switch categories if the woman is eligible.
Recommended Reading: Does Medicaid Cover A Breast Reduction
Extending Medicaid After Childbirth Could Reduce Maternal Deaths
Evidence shows women should receive follow-up care for a year after giving birth.
The easier bureaucratic pathway in this years American Rescue Plan wont be available to states until next year. For the moment, however, no matter where they live, new mothers on Medicaid dont have to worry about losing benefits after 60 days. Thats because the COVID-19 relief bill that former President Donald Trump signed last year prohibited the states from dropping anyone from Medicaid during the public health emergency.
Although new mothers with low incomes are already covered beyond 60 days in states that expanded Medicaid, states could increase the number of women who would be covered. Thats what Illinois has done.
Previously in Illinois, only women whose income was less than 138% of the federal poverty line qualified for the extended time on Medicaid. The states waiver now ensures new mothers up to 213% of the poverty line can continue on Medicaid after 60 days as well.
We determined that over two-thirds of pregnancy-related deaths were potentially preventable, and that one-third of pregnancy-related deaths occurred more than 60 days postpartum, said Dr. Robin Jones, an OB-GYN who chairs the states Maternal Mortality Review Committee, which had become alarmed after digging into the data and asked Illinois lawmakers to approve the waiver application.
How Does Payment/reimbursement Work
You have been deemed eligible for retroactive Medicaid, now what? You will receive a document that shows that you received retroactive Medicaid. This document should be given to your healthcare provider that you owe unpaid medical bills too. You can attach the approval to the claim and submit it to your provider so they can be paid for their services.
Healthcare providers often have a certain period in which they have to bill the state Medicaid agency. If they do not send the bill to the state within the period, they will not be paid. You should have received a Medicaid card in the mail in which you would also attach to the forms you give to your healthcare provider. If you havenât received your Medicaid card yet, or it was never mailed to you, the time limit will not apply to you.
There are certain circumstances in which your stateâs Medicaid agency may allow you to be reimbursed for any paid bills. With this, you would show your Medicaid to your healthcare provider and ask to have the money refunded and then bill Medicaid the remainder. It is to be noted that not every healthcare provider accepts Medicaid, so retroactive eligibility will not be beneficial in this case.
Remember, you are legally responsible for paying for any unpaid medical services you receive. This responsibility lasts until your retroactive eligibility is enacted and your healthcare provider is notified. Also, your healthcare provider must agree to send your medical bills to Medicaid.
Recommended Reading: Medicaid For The Elderly And People With Disabilities
Request For Retroactive Medicaid Coverage
With this form, you would apply for retroactive Medicaid. Completing this form will start the process of you obtaining retroactive coverage for up to three months before your Medicaid application date.
This is the form created by D.C. Department of Human Services for D.C. residents that can be accessed here. A Spanish version is available here.
Can A Pregnant Woman Receive Medicaid Or Chip Services Prior To An Eligibility Decision
Maybe. States may elect, but are not required, to provide some categories of Medicaid enrollees, including pregnant women, with presumptive eligibility. This allows pregnant women to receive immediate, same-day Medicaid services, typically at the clinic or hospital where they submit an application for Medicaid presumptive eligibility. Currently, 30 states provide presumptive eligibility to pregnant women.
Also Check: Does Medicaid Cover Auto Accidents In Michigan
States Push To Extend Postpartum Medicaid Benefits To Save Lives
More states are moving to extend Medicaid benefits to new mothers up to a full year after giving birth, far beyond the 60 days required by federal law.
That development, promoted by numerous medical groups as well as official state medical boards that focus on maternal health, reflects increasing alarm over the United States maternal mortality rate, which is the worst among developed nations and is trending in the wrong direction. There also is a growing awareness that women face increased health risks not only during pregnancy and labor and delivery, but also for months afterward. Nearly a quarter of postpartum-related deaths occur six weeks to a year after the end of a pregnancy.
States moves have been somewhat bipartisan, with Republicans supporting the expansion in some cases. And now the Biden administration is bolstering states efforts through a provision in the COVID-19 relief package that President Joe Biden signed in Marchmaking it more likely that states will quickly win approval for the requested changes.
Last month, Illinois became the first state to receive a waiver from the federal Centers for Medicare and Medicaid Services, allowing it to continue providing Medicaid benefits to women from 60 days to a year after delivery . Medicaid is the public health plan for low-income Americans.
Can I Apply For Medicaid If We Already Have Private Health Insurance
Medicaid is one of the most famous entitlement programs in America, but there is some confusion on who can apply and how they can do it. Medicaid is available to people who fit into several categories, including those with very low incomes, some who are disabled and the children of people who fit into various categories. If youre thinking about trying to qualify for Medicaid, you need to know whether you qualify. One of the most common questions has to do with private health insurance. Are you barred from seeking Medicaid if you already have insurance? The short answer is no, but there are other questions to answer about your financial situation.
Medicaid eligibility varies from state to stateThe first thing to know about Medicaid eligibility is that there is no singular national standard. The original version of the Affordable Care Act sought to force states to expand Medicaid to include people up to a higher level of income. The Supreme Court struck this down as unconstitutional, though, leaving states to make a choice on expansion. While some states chose to expand the program, others chose to keep it the same. This has let to a hodgepodge of state requirements.
You May Like: What Is The Difference Between Medicare & Medicaid
