Medicaid Is The Nations Public Health Insurance Program For People With Low Income
Medicaid is the nations public health insurance program for people with low income. The Medicaid program covers 1 in 5 Americans, including many with complex and costly needs for care. The program is the principal source of long-term care coverage for Americans. The vast majority of Medicaid enrollees lack access to other affordable health insurance. Medicaid covers a broad array of health services and limits enrollee out-of-pocket costs. Medicaid finances nearly a fifth of all personal health care spending in the U.S., providing significant financing for hospitals, community health centers, physicians, nursing homes, and jobs in the health care sector. Title XIX of the Social Security Act and a large body of federal regulations govern the program, defining federal Medicaid requirements and state options and authorities. The Centers for Medicare and Medicaid Services within the Department of Health and Human Services is responsible for implementing Medicaid .
Figure 1: Medicaid plays a central role in our health care system.
How Will My Health Insurance Provider Network Change When I Move To A New State
Particularly in the individual market, health insurers have been moving towards HMOs and narrower networks. So its becoming rare for plans to offer network coverage in multiple states. Be prepared for the fact that you will almost certainly have a new provider network with your new plan.
Its also important to note that even if your health insurer is a big-name carrier that offers plans throughout the country, it will have different individual market plans in each state. So although you might have a Cigna plan already, and Cigna might also be available in the individual market in the state where youre moving, youll need to re-enroll in the new plan once you move.
And although Blue Cross Blue Shield is a household name in the health insurance market, their coverage varies from state to state. The Blue Cross Blue Shield name is licensed by 36 different health insurance carriers across the country a Blue Cross Blue Shield plan in one state is not the same as a Blue Cross Blue Shield plan in another state.
Also Check: Neurologist In Alexandria La That Accept Medicaid
How To Transfer Medicaid Between States
Using Medicaid Out of State
Find Medicaid Planning Lawyers
You might be wondering if you can usde your Medicaid coverage in any state? The answer is No. Because each state has its own Medicaid eligibility requirements, you can’t just transfer coverage from one state to another, nor can you use your coverage when you’re temporarily visiting another state.
Should a beneficiary need to be admitted to a hospital in another state or if he must receive essential, regular psychiatric care or medications from an out-of-state provider, the home state will not pay for the services through Medicaid. In these situations, a caregiver or other family member is often required to sign an agreement to pay for the services before the person with special needs can receive care.
How long does it take to transfer Medicaid to another state?
Technically, there’s no formal program or option that allows you to transfer your Medicaid coverage from one state to another. Therefore, if you’re relocating, you’ll need to re-apply for Medicaid in the state you’re planning to reside in.
A common concern is the lapse of benefits between canceling ones Medicaid plan in their original state and reapplying in the state in which they are relocating.
You can also consider hiring aTexas Elder Law Attorney specializing in Medicaid planning to help with the process.
Application Process
Related Articles:
Recommended Reading: Blue Choice Medicaid Provider Portal
What If Im Moving Out Of State
As opposed to traveling to or through another state, if youre planing to move to another state, you need to give Medicare your new address.
The fastest way to update your contact information for Medicare is to use the My Profile tab on the Social Security website. You do not have to be receiving Social Security benefits to use this site.
However, to access this site, you must first register. You can only create an account for your own use, and you must be able to verify information about yourself, including your:
- Social Security number
- U.S. mailing address
- valid email address
You can also update your Medicare contact information by calling the Social Security Administration at 800-772-1213. If youd prefer to update in person, you can go to your local Social Security field office, which you can find here.
Medicaid Benefits Do Not Transfer From State To State
If Medicaid is paying for all or part of your loved ones nursing home costs, a move to another state will be more challenging than if she is a private-pay resident. This is because Medicaid programs are administered on a state level, and there is no option for transferring coverage from one state to another. In fact, under federal law, you cannot be eligible for Medicaid in two states at the same time. Steps for moving to a nursing home in a new state include:
- Locate a nursing home in the new state. You will need to find a facility that has open Medicaid beds and apply for admission. It would also be smart to review the Medicaid requirements in the new state because, even though federal law regulates Medicaid programs, each state sets its own requirements, and you want to be sure your loved one will qualify.
- Dis-enroll from Medicaid. You will have to close out your loved ones coverage in the state she is leaving before you can apply in a new state. Ideally, you will time the move for the end of a month because thats when her coverage will end once its canceled.
- Move to the new nursing home. Once your loved one is in the new facility, she can apply for Medicaid in that state. The nursing home should be able to help with the application process. It can take up to 90 days to get approval, but Medicaid benefits are retroactive, so any unpaid, qualified medical expenses during this retroactive period will be covered.
Also Check: Group Homes That Take Medicaid
Where To Start When Moving To A New State
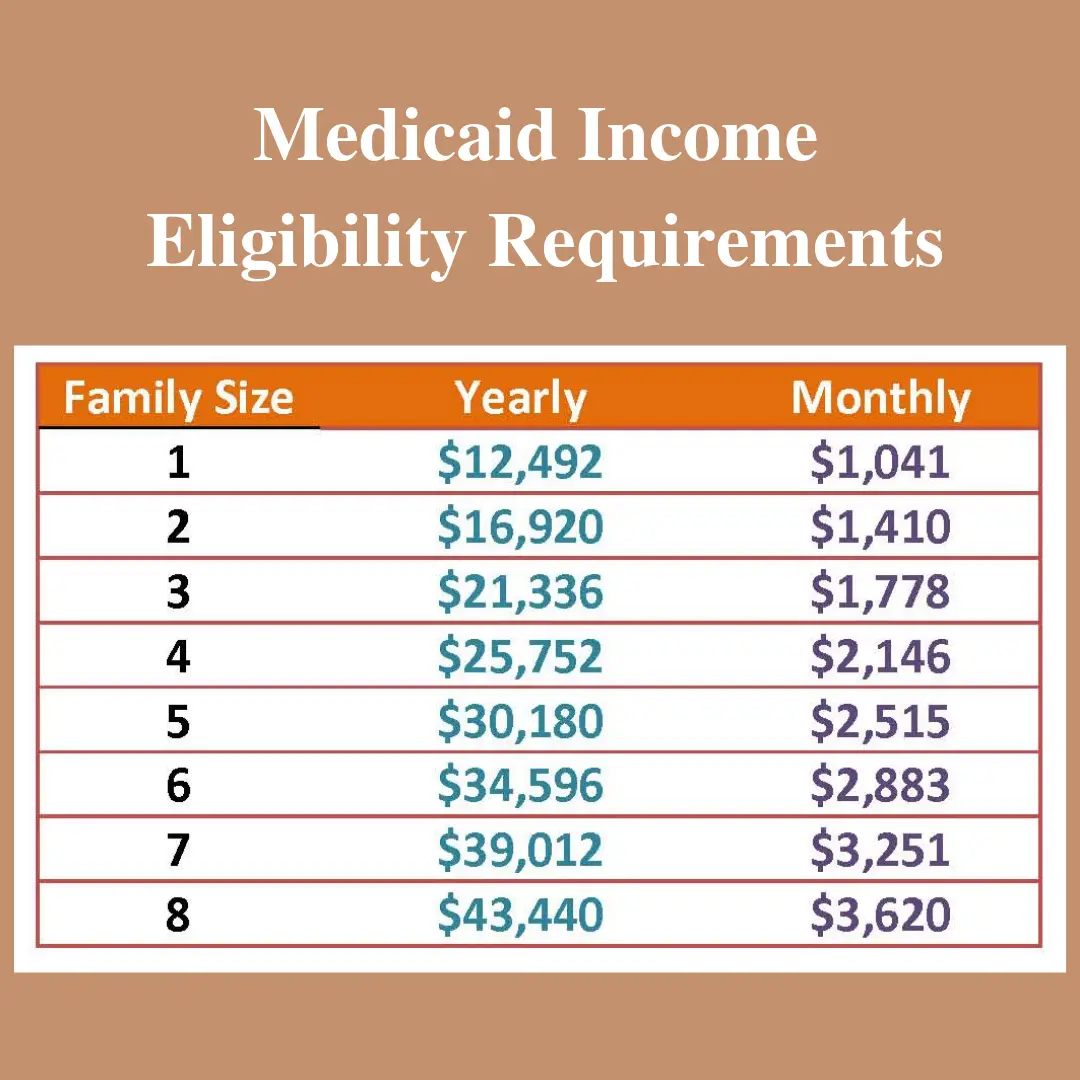
If you have Medicaid and are moving to a new state, your first step is to research Medicaid rules in the state you are moving to. Visit our State Resources to find the contact information for Medicaid in your state.
It is important to find out if your new state offers Expanded Medicaid, which may make it easier to qualify for Medicaid, because it is available to adults under 65, with a household income up to 138% of the Federal Poverty Level. Minnesota and New York give individuals with a household income between 138-200% FPL access to Medicaid through the Basic Health Program.
You should also look to see how Medicaid benefits in your new state compare to your current benefits. For example, your new state may offer more or less optional benefits, such as dental coverage.
Elder Wills Estates Trusts Special Needs Tax & Business Law Attorney John Sweeney
Sweeney Legal, LLC, provides legal, practical, and business counsel to Seniors, families, and businesses in the Fairfield, Connecticut area, including the communities of Bridgeport CT, Bethel CT, Brookfield CT, Danbury CT, Darien CT, Easton CT, Fairfield CT, New Canaan CT, Newtown CT, Norwalk CT, Redding CT, Ridgefield CT, Stamford CT, Weston CT, Westport CT and Wilton CT. John is also licensed in New York serving Westchester County including the towns of Bedford NY, Lewisboro NY, Mount Kisco NY, North Salem NY, Pound Ridge NY, Somers NY and South Salem NY.
Also Check: Apply For Emergency Medicaid Utah
Also Check: Where Can I Get Glasses With Medicaid
How Medicaid Coverage Works When You Move
You should reapply for Medicaid benefits as soon as you can to avoid a lapse in benefits coverage when you relocate across state lines. While the application process varies by state, you can usually apply online. In most cases, you’ll receive a letter of approval within 15 to 90 days.
Another thing to keep in mind is you can’t get Medicaid benefits in two states at the same time. Instead, you have to terminate your old Medicaid coverage in one state and reapply for benefits in your new home state.
Medicaid Is Structured As A Federal
Subject to federal standards, states administer Medicaid programs and have flexibility to determine covered populations, covered services, health care delivery models, and methods for paying physicians and hospitals. States can also obtain Section 1115 waivers to test and implement approaches that differ from what is required by federal statute but that the Secretary of HHS determines advance program objectives. Because of this flexibility, there is significant variation across state Medicaid programs.
The Medicaid entitlement is based on two guarantees: first, all Americans who meet Medicaid eligibility requirements are guaranteed coverage, and second, states are guaranteed federal matching dollars without a cap for qualified services provided to eligible enrollees. The match rate for most Medicaid enrollees is determined by a formula in the law that provides a match of at least 50% and provides a higher federal match rate for poorer states .
Figure 2: The basic foundations of Medicaid are related to the entitlement and the federal-state partnership.
You May Like: Is Nebraska Total Care Medicaid
Using Medicare Supplement Insurance In Another State
Medicare Supplement Insurance, or Medigap, may be used in any state with any provider that accepts Original Medicare. Any time that you use Medicare Part A or Part B benefits, you may use a Medigap plan along with it.
Additionally, some Medigap plans can provide coverage for qualified emergency care received outside of the United States, which is something that Original Medicare does not cover.
Does Medicaid Transfer From One State To Another
While Medicaid is a federal program available nationwide, each state has the ability to establish its own eligibility policies. If a move is in your future, its important to understand what factors should be evaluated to help you determine if you will be eligible for Medicaid in a different state.
Financial Requirements
Unlike Medicare, Medicaid is a needs-based program that looks at a combination of income and assets for each applicant to determine their eligibility for services. Because states set their own limits for income and assets, your eligibility can change if you move. Although these differences in limits between each state may not be very much, these policies can also change throughout the year, which makes planning carefully all the more important.
Financial requirements for Medicaid eligibility are classified under the following categories:
Other factors that decide financial limits include age and disability status. People over the age of 65 may have different income and asset limits than those under the age of 65. Blind or disabled individuals can also have different eligibility requirements in each state.
Some states also conduct whats called a look-back period, which checks to see if applicants have transferred their assets to non-applicants in order to be eligible. If these transfers are deemed inappropriately handled, there may be an additional waiting period before the applicant can become eligible.
Differences in Level of Care Requirements
Don’t Miss: Medicaid Doctors In Baton Rouge
Medicaid Is Jointly Financed By States And The Federal Government
Medicaid is financed jointly by the federal government and states. The federal government matches state Medicaid spending. The federal match rate varies by state based on a federal formula and ranges from a minimum of 50% to nearly 75% in the poorest state. Under the ACA, the federal match rate for adults newly eligible was 100% for 2014-2016, phasing down gradually to 90% in 2020 and thereafter . The federal matching structure provides states with resources for coverage of their low-income residents and also permits state Medicaid programs to respond to demographic and economic shifts, changing coverage needs, technological innovations, public health emergencies such as the opioid addiction crisis, and disasters and other events beyond states control. The guaranteed availability of federal Medicaid matching funds eases budgetary pressures on states during recessionary periods when enrollment rises. Federal matching rates do not automatically adjust to economic shifts but Congress has twice raised them temporarily during downturns to strengthen support for states.
Total federal and state Medicaid spending was $577 billion in FY 2017. Medicaid is the third-largest domestic program in the federal budget, after Social Security and Medicare, accounting for 9.5% of federal spending in FY 2017. In 2017, Medicaid was the second-largest item in state budgets, after elementary and secondary education .
Figure 8: Medicaid is a budget item and a revenue item in state budgets.
Using Medicare Advantage Or Medicare Part D In Another State
Medicare Advantage and Medicare Part D prescription drug plans are both sold by private insurance companies.
Medicare Advantage plans can come in a few different forms that can determine how the plan may be used in another state.
Two popular types of Medicare Advantage plans include:
- Health Maintenance Organization plansHealth Maintenance Organization plans feature a network of providers who participate in the plan. These networks can be local or regional, so they can span multiple states in some cases. In order to use the plans benefits, you must visit one of these participating providers. Be sure to check with your plan to ensure you can use your Medicare Advantage HMO plan in another state.
- Preferred Provider Organization plansPreferred Provider Organization plans also feature a network of participating providers, but they typically have fewer restrictions than HMO plans on which providers you may see. You may pay more to receive care outside of your Medicare Advantage PPO network.Also be sure to check with your plan provider to ensure you can use your Medicare plan in another state.
Many Medicare Part D plans may feature a network of pharmacies. Some plans include regional or national networks, while other plans may have more localized networks.
Don’t Miss: Is Geisinger Ghp Family Medicaid
Virginia Medicaid Enrollment Numbers
By June 2016, total enrollment in Virginias Medicaid program was 968,666, which was 4% higher than it had been in late 2013. Enrollment growth hovered in the single digits until Medicaid was expanded, and then it grew substantially. By July 2020, total Medicaid and CHIP enrollment had grown to over 1.5 million, which was an increase of more than 50% increase since late 2013. Medicaid enrollment in Virginia, and in much of the nation, had a sharp increase in 2020 driven by the coronavirus pandemic.
As of November 2021, 1,926,548 Virginians are covered by Medicaid/CHIP programs.
Medicaid Facilitates Access To Care
A large body of research shows that Medicaid beneficiaries have far better access to care than the uninsured and are less likely to postpone or go without needed care due to cost. Moreover, rates of access to care and satisfaction with care among Medicaid enrollees are comparable to rates for people with private insurance . Medicaid coverage of low-income pregnant women and children has contributed to dramatic in the U.S. A growing body of research indicates that Medicaid eligibility during childhood is associated with reduced teen mortality, improved long-run educational attainment, reduced disability, and lower rates of hospitalization and emergency department visits in later life. Benefits also include second-order fiscal effects such as increased tax collections due to higher earnings in adulthood. Research findings show that state Medicaid expansions to adults are associated with increased access to care, improved self-reported health, and reduced mortality among adults.
Figure 7: Nationally, Medicaid is comparable to private insurance for access to care the uninsured fare far less well.
Recommended Reading: South Carolina Medicaid Long Term Care
What Is Managed Care Ffs
Under the FFS model, the state pays providers directly for each covered service received by a Medicaid beneficiary. Under managed care, the state pays a fee to a managed care plan for each person enrolled in the plan.
What is the difference between MCO and FFS?
MCO refers to risk-based managed care PCCM refers to Primary Care Case Management. FFS/Other refers to Medicaid beneficiaries who are not in MCOs or PCCM programs.
What is Marylands all-payer system?
MD-APM is a capitated payment model that functions through a Centers for Medicare and Medicaid Services waiver this waiver has allowed for an all-payer system since the 1970s. The latest iteration is known as the total cost of care model.
Most Medicaid Enrollees Get Care Through Private Managed Care Plans
Over two-thirds of Medicaid beneficiaries are enrolled in private managed care plans that contract with states to provide comprehensive services, and others receive their care in the fee-for-service system . Managed care plans are responsible for ensuring access to Medicaid services through their networks of providers and are at financial risk for their costs. In the past, states limited managed care to children and families, but they are increasingly expanding managed care to individuals with complex needs. Close to half the states now cover long-term services and supports through risk-based managed care arrangements. Most states are engaged in a variety of delivery system and payment reforms to control costs and improve quality including implementation of patient-centered medical homes, better integration of physical and behavioral health care, and development of value-based purchasing approaches that tie Medicaid provider payments to health outcomes and other performance metrics. Community health centers are a key source of primary care, and safety-net hospitals, including public hospitals and academic medical centers, provide a lot of emergency and inpatient hospital care for Medicaid enrollees.
Figure 6: Over two-thirds of all Medicaid beneficiaries receive their care in comprehensive risk-based MCOs.
You May Like: Eye Place That Takes Medicaid
How Can Providers Receive Remittance Advices
Providers may access their remittance advices via the Provider Online Portal. The Provider Online Portal gives the provider the ability to view and download copies of Remittance Advices.
- Information about how to access the portal
- For assistance and questions regarding the Portal providers may send an email to or call 605.773.3495.
