Arizona Medicaid Income Limits Summary
We hope this post on Arizona Medicaid Income Limits was helpful to you.
If you have any questions about Medicaid in the state of Arizona, you can ask us in the comments section below.
Help us spread the word! If you found this post on Arizona Medicaid Income Limits helpful, help us spread the word by sharing it using the Share this button below.
Be sure to check out our other articles about Medicaid.
How Working With An Attorney Can Help
Many state and federal government programs are complex and may unfairly deny benefits to applicants. Having a lawyer to speak with through the process can help for support and advice on the application process. They can point you in the right direction for determining eligibility for not only AHCCCS but also Social Security benefits, Food Stamps, Unemployment, and more.While an attorney cant always help you qualify if your income is too high for benefits, they can ensure that you receive fair treatment during the application process, such as communication about the results of your application and a timely application review. If your benefits are denied unfairly, they can also assist you in appealing the decision.
How Do I Enroll In Medicaid In Arizona
The quickest way to apply for AHCCCS is online at www.healthearizonaplus.gov.
Or you can enroll through healthcare.gov if you are a non-disabled person under age 65.
You can also print an Application for Benefits form, complete it, and submit it by mail or in person. Use the locator tool to find a nearby office.
If you need help completing an application, call 1-855-HEA-PLUS or search online for a community assister.
Recommended Reading: Moving To Another State Medicaid
Altcs Benefits And Coverage:
ALTCS coverage varies based on where a person is living. For example, if a person resides in a long-term care facility, they will receive different long-term care supports than a person who remains at home. Depending on income level, medical neediness, and where the person lives, applying for ALTCS may help you receive some or all of the following services:
- If Applicable, Behavioral Health Care
- Up to $1,000/year in Dental Care
- Adult Day Care or Respite Care
- Home Health Services
- Medical Supplies and Durable Medical Equipment
- In-home Caregiving
- Meal Delivery
What Are The Requirements For Medicaid In Arizona

Medicaid benefits are overseen by the Family Assistance Administration and are dispensed through the Arizona Health Care Cost Containment System . In order to qualify for Medicaid in AZ, petitioners must meet several Medicaid requirements. There are general requirements for Medicaid as well as income requirements for Medicaid. The Arizona Medicaid eligibility requirements are outlined below.
First, an applicant must be a U.S. citizen in order to qualify for Medicaid in Arizona. Have available documentation to prove United States citizenship or legal presence in the country. If you a candidate is illegally residing in AZ, he or she may not meet the state Medicaid qualifications. In the event that petitioners are unable to provide the proper papers, they may still be eligible for emergency medical assistance through the federal government.
Next, Medicaid requirements state that a candidate must be a resident of Arizona to collect AZ Medicaid benefits. Applicants must have proof of state residency available, so they can confirm that they live within state borders before starting the Medicaid application process.
Moreover, petitioners must have a registered Social Security Number in order to meet Medicaid benefits eligibility. All state benefits are dispensed through the use of an SSN, which acts as an identifier for different governmental bodies.
You May Like: Does Medicaid Pay For Dentures In Nc
Not Eligible For Or Enrolled In Medicare
AHCCCSs eligibility rules are different for most people who are eligible for or enrolled in Medicare. If you are eligible for or getting Medicare, read DB101s Medicare article or contact your local DES/Family Assistance Administration office.
Exception: If you are enrolled in Medicare and are the parent or caretaker of a child or are pregnant, you may be able to get AHCCCS through the rules discussed in this article.
If you are not on Medicare, keep reading this article.
How Many People Are On Medicaid
According to the Centers for Medicare & Medicaid Services, as of November 2020, here are the number of people enrolled in Medicaid and Chip in the entire United States:
- 78,521,263 individuals were enrolled in Medicaid and CHIP
- 72,204,587 individuals were enrolled in Medicaid
- 6,695,834 individuals were enrolled in CHIP
Recommended Reading: Does Medicaid Cover Long Term Care Facilities
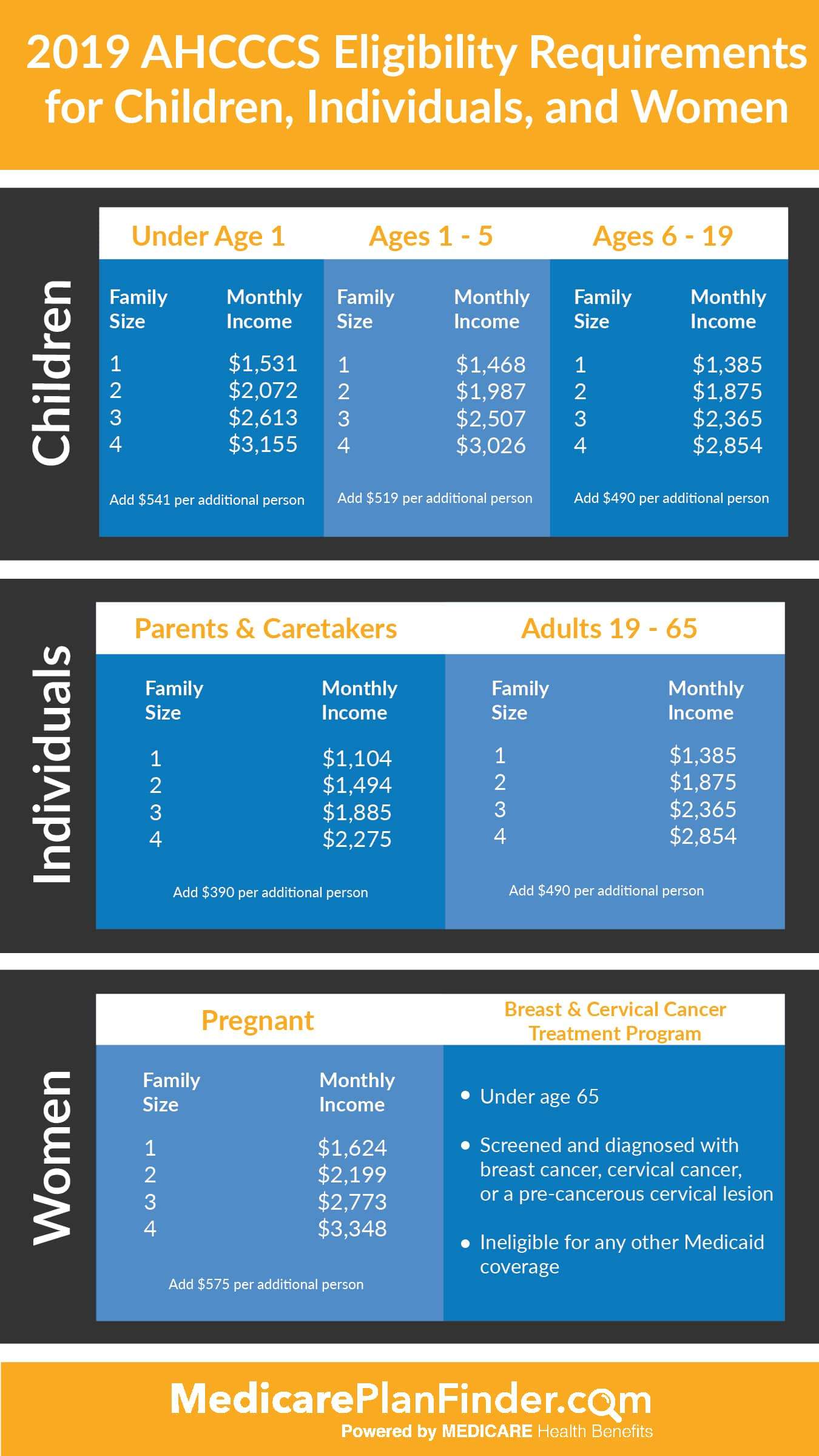
Arizona Medicaid Income Limit Charts
The Arizona Medicaid eligibility income limit charts are divided by groups.
For example, the first chart is focused on income limits for children who qualify for Medicaid.
Similarly, the second chart below focuses on the Medicaid income limits for adults in Arizona who qualify for Medicaid.
Arizona Medicaid Income Limit for Children
Below is the income limit for children by age category. Find the age category your child falls into and you will see the income limit by household size.
| Arizona Medicaid Income Limit Children |
| Children Medicaid Ages 0-1 |
| $59,398 |
How to Read the Arizona Medicaid Income Limits Charts Above
You cannot have an income higher than the Federal Poverty Level percentage described for your group to be eligible for Medicaid.
Similarly, when you identify the income group that applies to you, the income limit you see refers to the maximum level of income you can earn to qualify for benefits.
For example, if you are pregnant, to qualify for Medicaid, you cannot have an income higher than 156% of the Federal Poverty Level which for a family of two is $27,175 as shown in the chart above.
Meeting Ahcccs Eligibility Requirements
AHCCCS eligibility is different based on your age, income, and required services. On the most basic level, you must be an American citizen , an Arizona resident, and financially needy. Use the chart below to help figure out if you are eligible for Arizona Medicaid.
Note that if you or your child is under the age of 19 but does not meet the AHCCCS eligibility requirements, kids can still qualify for Arizona KidsCare at 200% of the federal poverty level. KidsCare comes with a premium of anywhere from $10-$70. Reach out to your local Family Assistance Office or call 1-855-HEA-PLUS for more information on KidsCare. The Arizona Medicaid phone number is 602-417-4000.
Don’t Miss: Therapist That Accept Medicaid Nyc
Learn About Requirements For Medicaid In Arizona
The first question you may ask yourself is, What are the requirements for Medicaid in Arizona? if you are interested in applying for medical assistance through the state. There are many factors that determine Medicaid benefits eligibility, including income level, residency status and citizenship status. It is important for applicants to be aware of all of the Medicaid eligibility requirements before beginning a Medicaid application so they can be prepared with all of the correct documentation and information. If you have reviewed all of the basic qualifications to receive Medicaid benefits and are prepared with the proper information the application requests, then you have a better chance of being accepted into Arizonas Medicaid program, otherwise known as the Arizona Health Care Cost Containment System . Another question you may have is What are the income requirements for Medicaid?, which can help you determine your eligibility for medical assistance. To learn how to qualify for Medicaid in AZ, continue reading the sections below.
Who qualifies for Medicaid in Arizona?
While the requirements for Medicaid in Arizona vary by applicants ages and financial circumstances, the AHCCCS also has very specific requirements for all prospective Medicaid beneficiaries. Each applicant must meet the following requirements for Medicaid in order to qualify to receive benefits:
What are the income requirements for Medicaid in Arizona?
Financial Resources For Arizona Medicare Enrollees
This page explains how Arizona regulations and policies affect you as a Medicare beneficiary. The page also provides information on avenues for financial help with paying for Medicare and long-term care, including benefits for individuals who are dually eligible for Medicare and Medicaid.
Also Check: Can A Person Have Medicaid And Private Insurance
Arizona Health Plan Finder
Need help looking for Arizona Medicaid plans and other health insurance? There are a handful of good Arizona health plan finder tools that you can use. If youre looking for Medicare plans, you can head straight to Medicare.gov. If youre looking for general insurance plans, you can go to healthcare.gov. We actually have a plan finder tool of our own, as well, called MedicarePlanFinderTool.com.
Ahcccs And Arizona Long

At Long-Term Assurance, were experts in one particular AHCCCS program: Arizona Long-Term Care System . The program benefits Arizonans who require a level of care equal to that provided by a nursing facility. This is often referred to as long-term care.To qualify for ALTCS, you do not have to live in a nursing home. You may also receive needed services while living in your own home or an assisted living facility.
Don’t Miss: Eye Exam Places That Take Medicaid
Arizona Long Term Care System
Arizonas long term care Medicaid program is also known as the Arizona Long Term Care System or with the acronym ALTCS. ALTCS is designed for people who are medically needy but cannot afford the care they need to remain healthy and safe. Applicants must meet certain medical requirements as well as income and asset requirements.
Arizona is an income cap state, meaning that in order to be eligible for Medicaid long term care, there is a hard income limit. Non income cap states allow applicants to spend down money for their care, whereas income cap states require the amount to be no higher than their limit at time of application.Like many other states, Arizona sets their income limit at 300% of the Federal Benefit Rate. The exact dollar amount changes annually. If an applicants income is higher than the states limit, an income only trust must be created for any excess income above the maximum.
Points To Keep In Mind On Medicaid Eligibility
- AHCCCS typically covers state residents who are younger than 65
- Residents who are older than 65 or disabled should apply for ALTCS
- If you have children, they may be entitled to Medicaid services, too
- The application processing period is usually between 60 and 90 days
- If you dont meet the financial requirements for ALTCS, a lawyer might be able to help
You May Like: Is Invisalign Covered By Medicaid
Q: Does Medicaid Cover Dental In Arizona
You might be able to use your AHCCCS benefits to cover some emergency dental costs, such as treatment fees for a jaw fracture, infection, or acute pain. Covered services may include required x-rays, anesthesia, oral surgery, an exam of cavities, and pain or antibiotic medications for your treatment. Note that restorative services or preventative dental care arent covered.
How Medicaid Eligibility Is Determined
Income eligibility is determined by your modified adjusted gross income , which is your taxable income, plus certain deductions. Those deductions include non-taxable Social Security benefits, individual retirement contributions and tax-exempt interest. For most people, MAGI is identical or very close to your adjusted taxable income, which you can find on your tax return. Specific income requirements in dollars rise alongside the size of your household.
Our guide focuses on each stateâs major programs for adults. Most are only available to state residents, U.S. citizens, permanent residents or legal immigrants .
Looking for insurance for a child? Check out our guide to the Children’s Health Insurance Program .
Don’t Miss: Florida Medicaid In Home Care
What If Im Turned Down By Medicaid
- You may be able to buy a private health plan through the Marketplace instead for the 2018 plan year in the fall. You may qualify for savings based on your income through a premium tax credit and savings on out-of-pocket costs.
- If you don’t qualify for either Marketplace or Medicaid savings, you still have options. Learn more here.
Information Needed To Apply
Whether you are applying for the first time, or renewing your benefits, you may need one or more of the following pieces of information to complete your application:
- Proof of citizenship and identity for everyone who is applying for benefits.
- Alien Registration Cards, if there are non-U.S. citizens applying for benefits in your household.
- Social Security numbers for everyone, or proof that a Social Security number has been applied for.
- Birth certificates for everyone who is applying for benefits.
- Name, address & daytime phone number of landlord or neighbor.
- A statement verifying your address and the names of everyone living with you. The statement must be made by a non-relative who doesnt live with you. It must be signed, dated and include that person’s address and telephone number.
- Proof of ALL money your household received from any source last month and this month.
- Proof that your employment ended and last date paid.
- Verification of any medical insurance other than AHCCCS.
Recommended Reading: Vermont Medicaid Dental Fee Schedule
What Benefits Does Arizona Medicaid Cover
Arizona Medicaid provides a wide range of healthcare services including but not limited to well-check exams, ambulance services, hospitalization, family planning, labs and X-rays, prescription drugs, surgeries, pregnancy care and vision services. Routine health check exams for children under 21 are also part of the Arizona Medicaid program. These may include wellness exams, comprehensive dental care, immunizations, eye exams and glasses, nutrition checks and hearing screenings.
Option 1 Apply Online
You can apply online through the Arizona Health-e-Arizona Plus account . If you have an account, you can log in or create your Health-e-Arizona Plus Account. to be taken to the website.
The short video below, from the Arizona Department of Economic Security , will walk you through the Medicaid Electronic Application process.
We highly encourage you to watch it.
Recommended Reading: How To Apply For A Replacement Medicaid Card
Who Qualifies For Medicaid
In all but 13 states, adults who make below a certain income may qualify for Medicaid. In all states, Medicaid is available to people who make a low income and also meet other criteria such as being at least 65 years old, disabled, pregnant or other qualifications.
Each state runs its own Medicaid programs with its own set of qualifying criteria.
Choosing From Ahcccs Plans
There are more than ten health plans that you can choose from . All Access Arizona health plans include the same covered services, but they do not all have the same network. That means that not every doctor, hospital, or pharmacy will accept every AHCCCS plan. It may be a good idea to check with your favorite doctors before you select your plan to make sure you do not have to switch doctors.
Not all plans will be available in your area. for the full list of AHCCCS plans that you can choose from. You can filter by county or city to only see the options available to you.
Also Check: Braces Place That Take Medicaid
Arizona Health Care Cost Containment System Coverage
If you hear a doctor or anyone refer to Access Arizona, they are most likely referring to the Arizona Health Care Cost Containment System. Access Arizona plans work similarly to a marketplace HMO plan. Youll have to select one primary physician who accepts your plan to be the first doctor you go to for all your health care needs. That one doctor will be the person who authorizes all your medical services and can refer you to specialists for treatment.
AHCCCS provides coverage for adults, caretaker relatives, children, seniors, the blind and disabled, nursing home residents, pregnant women, and other disabled persons who need financial assistance. Covered services include :
- Doctor visits
- Hospital visits
- Surgeries
Arizonas Requirements For Medicaid Qualification
The state of Arizona follows specific criteria when making a decision on eligibility for their Medicaid program. Only those applicants who are facing financial hardships and meet the income requirements can get approved. Children and women who are pregnant are also far more likely to receive insurance than adults who have no prior health concerns. A larger family may qualify easier than a single individual.
Don’t Miss: Does Medicaid Cover Hearing Aids In Ohio
What Is The Lowest Income To Qualify For Medicaid
There are 13 states that do not grant Medicaid access to individuals based on income alone.
Of those that do, only Wisconsin uses a limit lower than 138%. An individual in Wisconsin can make no more than the federal poverty level in order to qualify for Medicaid.
Texas has the lowest income limit to qualify on a family basis, at 17% of the FPL. A two-parent household with one child in Texas can make no more than $37,332 and qualify for Medicaid.
Children’s Health Insurance Program
The Children’s Health Insurance Program is a public healthcare program for low-income children who are ineligible for Medicaid. CHIP and Medicaid are related programs, and the former builds on Medicaid’s coverage of children. States may run CHIP as an extension of Medicaid, as a separate program, or as a combination of both. Like Medicaid, CHIP is financed by both the states and the federal government, and states retain general flexibility in the administration of its benefits.
CHIP is available specifically for children whose families make too much to qualify for Medicaid, meaning they must earn incomes above 138 percent of the federal poverty level, or $33,948 for a family of four in 2017. Upper income limits for eligibility for CHIP vary by state, from 175 percent of the federal poverty level in North Dakota to 405 percent of the FPL in New York. States have greater flexibility in designing their CHIP programs than with Medicaid. For instance, fewer benefits are required to be covered under CHIP. States can also charge a monthly premium and require cost sharing, such as copayments, for some services the total cost of premiums and cost sharing may be no more than 5 percent of a family’s annual income. As of January 2017, 14 states charged only premiums to CHIP enrollees, while nine states required only cost sharing. Sixteen states required both premiums and cost sharing. Eleven states did not require either premiums or cost sharing.
Read Also: Does Missouri Medicaid Cover Assisted Living
