Spousal Impoverishment Income And Resource Levels Increase
Providers of nursing facility services, home and community based waiver services and services to individuals enrolled in a managed long term care plan, are required to print and distribute the “Information Notice to Couples with an Institutionalized Spouse” at the time they begin to provide services to their patients.
Effective January 1, 2017, the federal maximum community spouse resource allowance increases to $120,900 while the community spouse income allowance increases to $3,022.50. The maximum family member monthly allowance increases to $677.
This information should be provided to any institutionalized spouse, community spouse, or representative acting on their behalf so as to avoid unnecessary depletion of the amount of assets a couple can retain under the spousal impoverishment eligibility provisions.
Income and Resource Amounts| Federal Maximum Community Spouse Resource Allowance: $120,900Note: A higher amount may be established by court order or fair hearing to generate income to raise the community spouse’s monthly income up to the maximum allowance.Note: The State Minimum Community Spouse Resource Allowance is $74,820. |
| Community Spouse Minimum Monthly Maintenance Needs Allowance is an amount up to: $3,022.50 Note: A higher amount may be established by court order or fair hearing due to exceptional circumstances that result in significant financial distress. |
| Family Member Monthly Allowance for each family member is an amount up to: $677 |
Medicaid Alternative Benefit Plan Coverage Requirements For Larc Methods
Since 2005, states have had the authority to enroll Medicaid enrollees, with some exceptions, in Alternative Benefit Plans . The benefit packages in these ABPs mirror the benefits in certain specified commercial health plans. The ACA raised the significance of ABPs by designating them as the benefit packages offered to the majority of the ACAs Medicaid expansion population.
While all state Medicaid plans are required to cover family planning services and supplies without cost-sharing, federal regulations now additionally require Medicaid ABPs to cover all of the preventive services that most commercial insurance plans must cover under the ACA, including all FDA-approved contraceptive methods, without cost-sharing. This means that millions of newly eligible low-income women who enroll through the Medicaid expansion will receive coverage of all LARC methods, no matter how the state defines its family planning benefit for the rest of its Medicaid program. Additionally, as explained in the section on commercial plans, the ACA contraceptive coverage requirements include related follow-up and side effect management, and importantly, LARC method removal. A growing number of states, including Idaho, West Virginia, and Kentucky, also enroll groups of Medicaid-eligible individuals other than the Medicaid expansion population into ABPs, who will also benefit from these requirements.
What Services Are Available Through This Program
- Physical exams which may include a pap smear, breast exam, and STD testing
- Family planning counseling and pregnancy test
- Birth control supplies including condoms
- Colposcopies and treatment for STDs which are limited to a six week period after a family planning exam, counseling visit, or supply visit
- Related pharmaceuticals and laboratory test
Please noteAll Services are CONFIDENTIAL
Read Also: How Much Does It Cost For Medicaid
What Do Family Planning Services Cost
There is no cost for family planning services, including office visits and drugs/devices. You do not have to pay a co-payment for family planning services.
Where can you go for family planning services?
You can go to any Health First Colorado provider who offers family planning services, such as:
-
An ob/gyn or gynecologist
-
A nurse practitioner or other advanced practice nurse
-
A family planning clinic
-
Your regular doctor or primary care provider
You do not need a referral from your primary care provider in order to get family planning services. You can choose to see any Health First Colorado family planning provider even if you are in a managed care plan and the provider you want to see is out-of-network. For help finding a family planning provider, please see the Find a Doctor page or call the Member Contact Center.
Program Contact:
Dont Miss: How To Recertify For Medicaid
Your Partner Shouldnt Be Able To Feel Your Iud Strings During Sex But If They Can You Should Talk To Your Doctor
Usually, your partner cannot feel the strings, Dr. Worly says. That doesnt mean this cant happen, though. Its also worth mentioning that, if your partner can feel your strings or they appear longer than usual, this could be a sign that your IUD has moved and needs to be adjusted, according to the Mayo Clinic. If your IUD is firmly in place, you can also talk to your medical practitioner about trimming the strings, Dr. Worly says. Also, dont worryhaving sex shouldnt dislodge your IUD.
Also Check: Whats Better Medicare Or Medicaid
Recommended Reading: Does Medicaid Pay For Oxygen
How Much Does It Cost
The cost of an IUD can vary depending on the health insurance plan and the type of IUD. Many health insurance plans cover the costs, and family planning clinics may charge less, particularly for teens and young adults.
Because an IUD lasts for many years, the cost works out to about the same as monthly birth control methods, such as the Pill or ring.
Can I Get An Iud For Free Or Low
Theres a good chance you can get an IUD for free if you have health insurance. Because of the Affordable Care Act , most insurance plans must cover all methods of birth control, including IUDs.
However, some plans dont cover all brands of IUDs. Your health insurance provider can tell you which ones they pay for. Your doctor may also be able to help you get your birth control method of choice covered by health insurance. Learn more about health insurance and affordable birth control.
If you dont have health insurance, youve still got options. Depending on your income and legal status in the U.S., you may qualify for Medicaid or other state programs that can help you pay for birth control and other health care.
Planned Parenthood works to provide you with the services you need, whether or not you have insurance. Most Planned Parenthood health centers accept Medicaid and health insurance, and many charge less for services and birth control depending on your income. Contact your local Planned Parenthood health center for more information.
Don’t Miss: Does Medicaid Cover Rabies Vaccine
License For Use Of Current Dental Terminology
End User License Agreement:These materials contain Current Dental Terminology , copyright © 2021 American Dental Association . All rights reserved. CDT is a trademark of the ADA.
The license granted herein is expressly conditioned upon your acceptance of all terms and conditions contained in this agreement. By clicking below on the button labeled I accept, you hereby acknowledge that you have read, understood and agreed to all terms and conditions set forth in this agreement.
If you do not agree with all terms and conditions set forth herein, click below on the button labeled I do not accept and exit from this computer screen.
If you are acting on behalf of an organization, you represent that you are authorized to act on behalf of such organization and that your acceptance of the terms of this agreement creates a legally enforceable obligation of the organization. As used herein, you and your refer to you and any organization on behalf of which you are acting.
How Much Is A Copper Iud Without Insurance
There are two types of IUD one uses copper and the other, progestin and the copper IUD is popular among women who want a non-hormonal form of birth control. Typical costs: For patients not covered by insurance, an IUD typically costs between $175 and $600 for the device, insertion and a follow-up appointment.
Recommended Reading: Can I Change Medicaid Plan
Ny Medicaid Ehr Incentive Program Update
The NY Medicaid Electronic Health Records Incentive Program provides financial incentives to eligible professionals and hospitals to promote the transition to EHRs. Providers who practice using EHRs are in the forefront of improving quality, reducing costs and addressing health disparities. Since December 2011, over $784 million in incentive funds have been distributed within 24,999 payments to New York State Medicaid providers.
Also Check: Medicaid Data Warehouse New York
Does An Iud Help Prevent Stds
No. The IUD does not protect against sexually transmitted diseases . Couples who are having sex must always use condoms along with the IUD to protect against STDs.
A doctor or nurse practitioner will check to be sure a woman doesnt have any STDs before putting in an IUD. Getting an IUD put in while she has an STD could lead to pelvic inflammatory disease .
Abstinence is the only method that always prevents pregnancy and STDs.
Also Check: Missouri Medicaid For College Students
Don’t Miss: Get A Copy Of Medicaid Card
How Does The Copper Iud Work
IUDs affect the way sperm move and survive in the uterus , stopping sperm from meeting and fertilising an egg. IUDs can also change the lining of the uterus, making it difficult for a fertilised egg to stick to the lining to start a pregnancy.
Local anaesthetic: a medicine used to numb a part of yourbody for a short while. You remain conscious.
Sedation: a medicine used to cause a relaxed, sleep-like state so you are unaware of the procedure.
Recommended Reading: What Is The Household Income Limit For Medicaid
Who Is Eligible For Family Planning

Beneficiaries must meet the following eligibility criteria:
- Family income no more than 194 percent of the federal poverty level conversion)
- Must be capable of reproducing ages 13-44 years of age.
- Must not have had a procedure that prevents them from reproducing.
- Must not have Medicare, CHIP, or any other health insurance or third party medical coverage.
Donât Miss: Does Medicaid Cover Dementia Care
Also Check: How To Find Case Number For Medicaid
Information Notice To Couples With An Institutionalized Spouse
- Information Notice to Couples with an Institutionalized Spouse is available as a PDF.
- Additionally, the form Request for Assessment should be printed and distributed.
Medicaid is an assistance program that may help pay for the costs of your or your spouses institutional care, home and community based waiver services, or enrollment in a managed long term care plan. The institutionalized spouse is considered medically needy if his/her resources are at or below a certain level and the monthly income after certain deductions is less than the cost of care in the facility.
Federal and State laws require that spousal impoverishment rules be used to determine an institutionalized spouses eligibility for Medicaid. These rules protect some of the income and resources of the couple for the community spouse.
Note: Spousal impoverishment rules do not apply to an institutionalized spouse who is eligible under the Modified Adjusted Gross Income rules.
If you or your spouse are:
Women Shouldnt Get A Bill For An Iud But Sometimes They Do
By Shefali LuthraFebruary 7, 2020
We encourage organizations to republish our content, free of charge. Heres what we ask:
You must credit us as the original publisher, with a hyperlink to our khn.org site. If possible, please include the original author and Kaiser Health News in the byline. Please preserve the hyperlinks in the story.
Its important to note, not everything on khn.org is available for republishing. If a story is labeled All Rights Reserved, we cannot grant permission to republish that item.
Have questions? Let us know at
Read Also: How To Apply For Medicaid And Food Stamps In Michigan
Attention Family Planning Providers: Medicaid
LARC Description| Etonogestrel implant system, including implant and supplies | J7307 |
The New York State Medicaid program provides coverage for FDA-approved birth control methods, devices, and supplies ). Long-acting reversible contraceptives , such as IUDs and contraceptive implants, are the most effective forms of contraceptives. One major advantage of LARCs is that they do not require ongoing effort on the part of the user for long-term and effective use. More than 22,000 fee-for-service Medicaid members chose LARC as their method of birth control since April 1, 2015.
Which Is The Best Medicaid Plan In Florida
NCQA Health Insurance Plan Ratings 2019-2020 Summary Report Rating Plan Name 3.5 Coventry Health Care of Florida, Inc. d/b/a Aetna Better Health of Florida 3.5 Humana Medical Plan, Inc. 3.5 Molina Healthcare of Florida, Inc. Special Project: Managed Medical Assistance 3.5 Simply Healthcare Plans, Inc.
Recommended Reading: Eye Doctor That Takes Medicare And Medicaid
How To Check If Your Insurance Will Cover Mirena
You may be able to get Mirena with no out-of-pocket cost.
Follow these steps to check:
*Please note: Other product-related costs may apply.
If you need help understanding your insurance coverage, visit CoverHer.org.
Undue Hardship Occurs When:
An institutionalized spouse will not be determined ineligible for Medicaid because the community spouse refuses to make his or her resources in excess of the community spouse resource allowance available to the institutionalized spouse if:
Also Check: Nursing Homes That Accept Medicaid Pending
What Is The Family Planning Program
This program allows men and women to get family planning services only. This program is a form of limited insurance coverage. If you are able to enroll in the FPP, most of your basic family planning services will be paid for. However, it does not meet the Affordable Care Act requirements for a minimum essential benefits plan.
I Want To Get An Iud Do I Have To Go With A Parent Is It Covered By My Insurance
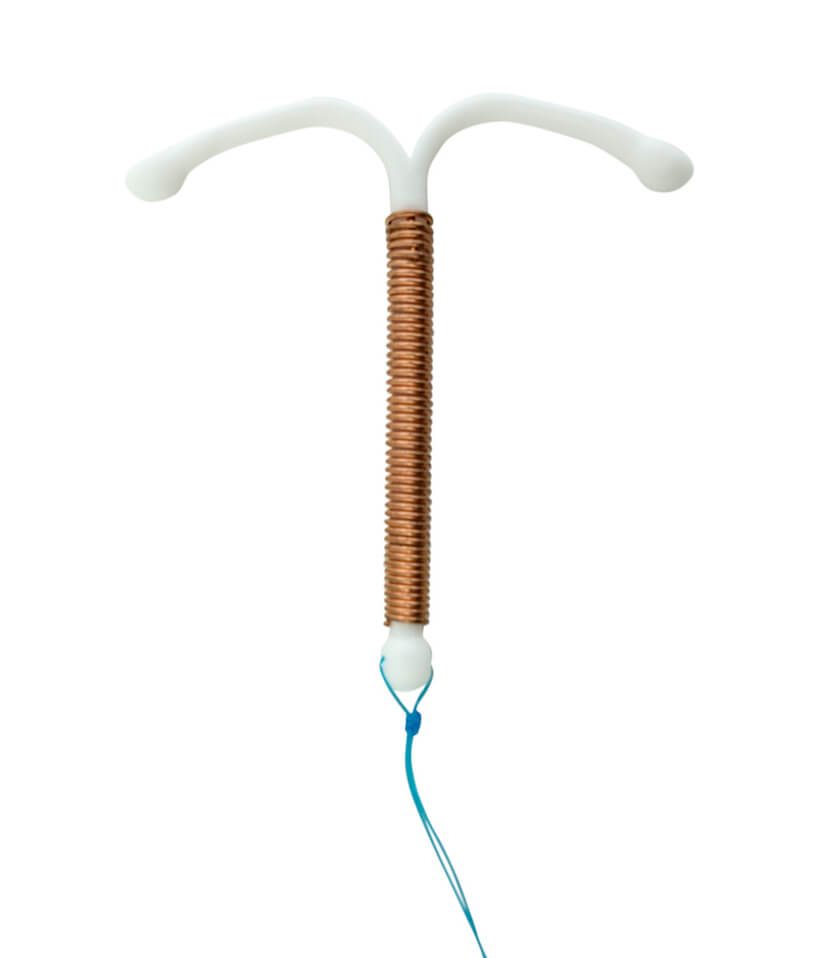
I want to get an IUD. Do I have to go with a parent? Is it covered by my insurance?
In general, you dont need a parents permission to get birth control. Butthere are some situations and locations where, for one reason or another,you will need a parents consent. This is something to ask about whenyou call to make your appointment. The same goes for cost and insurancecoverage. Planned Parenthood works to make health care as affordableas possible, and some health centers are able to charge according toincome. And while many health centers do accept Medicaid, whether ornot Medicaid covers IUDs and how much theyll cover can vary from stateto state. The staff at your local Planned Parenthood health center can giveyou specific information on the insurance they take and the cost of an IUD.
Most women can use an IUD safely even younger women and womenwho havent had children. But before you get an IUD, youll need to talkwith a health care provider to make sure its right for you.
Tags:cost, IUD, parents, Insurance
Planned Parenthood delivers vital reproductive health care, sex education, and information to millions of people worldwide. Planned Parenthood Federation of America, Inc. is a registered 501 nonprofit under EIN 13-1644147. Donations are tax-deductible to the fullest extent allowable under the law.
Read Also: How To Enroll My Newborn In Medicaid
The Device: The Cheaper Place Is Costco
While Medicare covers the insertion or removal, it doesnât cover the cost of the device.
There are three devices on the market, according to Desrosiers one with the hormone progesterone, one with copper, and one with copper and silver.
Most health and drug insurance plans cover the device with progesterone since itâs a device that has a hormone on it, itâs considered a form of medication.
Desrosiers said the cost of the progesterone device varies, but the cheapest place to buy one is Costco. The Mirena device, one of the older progesterone devices, runs about $360 to $380 there, she said, but can go up to around $420 at a pharmacy.
The copper devices go for around $70 to $140, Desrosiers said. Since they donât have progesterone, theyâre not considered medication and arenât covered by insurance, though Desrosiers said she thinks they should be.
âIf you want to decrease the amount of unwanted pregnancy and abortion and all of that, I mean, you should make sure that people can have options for contraception that can be covered,â she said.
Donât Miss: Home Health Aide Services Covered By Medicaid
