Who Meets Requirements For Medicaid In Florida
The first step in determining if you are eligible for Medicaid in Florida is to review the types of patients the state deems as qualified. What are the Medicaid application guidelines regarding Medicaid eligibility groups in FL? There are many different candidates that qualify for Medicaid, even though the state has not yet elected for Medicaid expansion plans. The following patients meet eligibility for Medicaid benefits in Florida:
- Pregnant women
- Those eligible for Temporary Cash Assistance in Florida
- Families who have lost Medicaid due to increased income or alimony
- Individuals who were formerly in foster care under age 26
- Any residents who currently receive Supplemental Security Income through the Social Security Administration
- Those in nursing home facilities or who receive home- or community-based care
- Patients over age 65 as well as the disabled
If the candidate does not qualify for Medicaid because he or she does not belong to one of the Medicaid eligibility groups listed, he or she may still be able to receive medical assistance. If the petitioner is considered Medically Needy in Florida, he or she can receive shared-cost Medicaid.
Effective Date Of Coverage
Once an individual is determined eligible for Medicaid, coverage is effective either on the date of application or the first day of the month of application. Benefits also may be covered retroactively for up to three months prior to the month of application, if the individual would have been eligible during that period had he or she applied. Coverage generally stops at the end of the month in which a person no longer meets the requirements for eligibility.
I Was Approved For Medicaid Whats Next
Congratulations! This is an important first step to better health and well-being. Coverage isnt only important when you are sick, its helpful when you dont feel sick. Now that you have Medicaid coverage, you can use your insurance to:
-Visit your doctor
-Get preventive care
-Get prescription medicines that you need
Follow the links on the right side of this page to learn what you need to do next, how to stay covered, and how to get the most out of your Medicaid coverage.
You May Like: Medicaid Services Department Frankfort Ky
Medicaid V Medicare: Terminology Whats Covered Eligibility
First, it is essential to understand the basic differences between Medicaid and Medicare. The two terms are so similar they can be confusing.
Medicare is the federal health insurance program for people who are 65 or older, certain younger people with disabilities, and people with End-Stage Renal Disease. Payroll taxes go into paying for the program, and this along with other sources of revenue, provides coverage for retirees and others who qualify. Different parts of Medicare pay for different services. Medicare is not means-tested , though some costs are now tied to a recipients income. You can get a good overview in our Medicare Fact Sheet.
Medicare covers skilled home health care in specific circumstances. You can also download our resource sheet about paying for home care. Medicare is considered more of an acute-care health insurance, so the coverage it provides for such services tends to be for short-term and/or intermittent needs. Medicaid, long-term care insurance and private pay are the typical means of paying for longer term or more custodial care .
Medicaid is defined on Wikipedia as a social health care program for families and individuals with low income and limited resources. It is a means-tested program, jointly funded by states and federal government and managed by each state. The states have discretion in many areas of how they manage the program, including eligibility.
Contact Local Welfare Office
Another way to find out about your Medi-cal status is to contact the local welfare office. Dont forget that even though Medi-cal is a statewide program, local offices administer it. If you are not sure where your local welfare office is located, then dont worry. Just go to the website of the Department of Health Care Services and check the list of county welfare offices. You can also find out the location of your local welfare office in your local phone book. It will be mentioned under the category of Social Services or Health and Human Services.
You May Like: How Do I Change My Primary Care Physician For Medicaid
Verify Your Enrollment Online
Its quick and convenient to check Medicaid status online in the comfort of your own home. The first step is to log in to your account. If you dont have an account, create one by providing your email address and then verifying your account. Once you have created your online account, find and then click on the My application and coverage link from the sites drop-down menu. Here youll discover whether or not you have Medicaid coverage, including the date your Medicaid coverage starts if youve recently enrolled in the Medicaid benefits program.
Dont Miss: Nevada Medicaid And Nevada Check Up Phone Number
How To Check If My Health Insurance Is Valid
It is always a good idea to confirm that your health insurance is valid. The first step is to enroll in a Marketplace plan. The second step is to pay the first premium to your health insurance company. Do not confuse Health Insurance Marketplace with a health insurance company. After that you can check if your health insurance is active. You must continue to pay your monthly health premiums to your health insurance company to keep your health insurance valid. You can check the validity of your health insurance online whenever you want.
Once your health insurance becomes valid, you can use your coverage to cover the medical expenses of health services such as visiting a doctor, emergency care, and filling prescriptions at pharmacies. It is always a good idea to thoroughly read the details about your health coverage provided in the enrollment materials of your health insurer. It will enable you to use your health coverage in a more efficient way.
Some health insurance companies do not pay for a specific health service or for specific health care providers. If that is your case, then you can file an appeal to your insurance company to change the decision.
Also Check: Is There Dental Coverage With Medicaid
Eligibility For Medicaid Services
Recipient eligibility for Medicaid is determined by the:
- Department of Children and Families, Office of Economic Self Sufficiency The Department of Children and Families determines eligibility for low-income children and family programs and the institutional care program.
- Social Security Administration The Social Security Administration determines eligibility for the Supplemental Security Income program.
Each program has its own income and asset requirements.
Information about Medicaid eligibility criteria for the aged, blind and disabled, and children and family programs can be obtained from the Department of Children and Families Web site or the DCF region / circuit office closest to you.
Also Check: Medicaid Albany Ny Phone Number
How To Apply / Getting Started
Every State has an agency that is in charge of administering the Medicaid Applications within that state. The Florida Department of Children and Families is the agency that administers the application process in Florida.
Eligibility for Medicaid for long-term care services, Nursing Home Medicaid, and Medicaid programs that provide for Assisted Living Facility or at home assistance all have the same financial requirements that must be met. Both husband and wife will need to provide documentation regarding assets and income as part of the application process. I know this seems like a violation of our right to privacy, but the Congress and Senate have not yet made it a right for everyone to receive Medicaid Long Term Care. Medicaid qualification for Long Term Care is optional and available for those who choose to apply and are willing to provide the necessary documentation to prove they meet the requirements. The basic financial requirements are that an individual receives less than $2,313/month income and has less than $2,000 in assets. For a couple, the community spouse may retain $126,420 for what is called a resource allowance, and the community spouse income is unlimited. That is the basic Financial Standards for Medicaid Institutional Care Program , which covers Long Term Care. These standards DO NOT APPLY to any other Medicaid program.
Read Also: Aged Blind Disabled Medicaid Nj
Recommended Reading: Michigan Medicaid Eligibility For Seniors
How Can I Check My Medicaid Status Online
Verify your enrollment online
Likewise, people ask, how can I check my Medicaid status?
Verify your enrollment online
One may also ask, how do I access my Medicaid account? See Your Medicaid Information
Additionally, can I lookup my Medicaid number online?
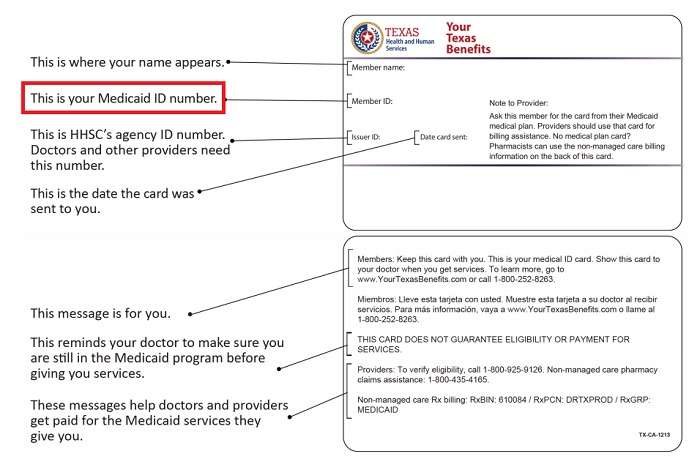
If you cant find your Medicaid identification number, you can get it from your states health and human services department. Although methods vary between states, this can often be done over the phone, in person or online.
How do I find out if my medical is active?
You can also check on your Medi-Cal status by calling the Medi-Cal hotline at 541-5555. If youre outside of California, call 636-1980.
Dont Miss: Apply For Sc Medicaid Online
How To Check Medicaid Status In Florida
In the United States, people can be eligible for free or low-cost healthcare through the federal Medicaid program, which is administered by states. After applying or, if they need to make changes afterward, people need to stay updated on their Medicaid status to make sure they are covered. States have different means of communicating this information, and Florida residents can use the Florida Medicaid Portal and the Florida Department of Children and Families website. Once a Medicaid application in Florida is complete, eligibility is determined by the Social Security Administration and the Department of Children and Families .
Read Also: Can I Have Medicare And Medicaid
How To Check If My Medicaid Is Active
The Center for Medicaid and CHOP Services is the state and federal organization founded in 1965 by the US government to run medical assistance programs like Medicaid, the Basic Health Program , and the Childrens Health Insurance Program .
Medicaid is the one with the most coverage in the country, providing medical assistance to over 72.5 million American citizens. Its primary mission is to guarantee quality health to low-income families, qualified pregnant women, seniors, parents, and disabled people that are not capable of providing this service to themselves.
In this article, we will explain more about this subject, and specifically how to check if your Medicaid is active.
Contents
Application Processing And Case Overview

Case ReviewAfter you submit an application for Mississippi Medicaid health benefits, the regional office that serves your county of residence will be in contact with you by phone or you may get a letter regarding your eligibility determination. If something is incorrect, missing or needs clarification a regional office staff member will contact you.
Case ApprovalIf you are approved to receive health benefits, a letter and a blue Medicaid identification card will be mailed to you. Mississippi Medicaid has a large network of health care providers available for medical services. When you make an appointment be sure the provider you choose accepts Mississippi Medicaid.
You may be eligible for health benefits through a coordinated care program called Mississippi Coordinated Access Network . Those who are automatically qualified for this program will have the option of choosing between one of three Coordinated Care Organizations : Magnolia Health, UnitedHealthcare Community Plan and Molina Healthcare. Mandatory populations are not eligible for dis-enrollment.
Those individuals who qualify for this program in an optional population have the choice to either enroll in a CCO or choose to stay in the traditional Medicaid fee-for-service program.
The Childrens Health Insurance Program is currently administered by Molina Healthcare and UnitedHealthcare Community Plan.
You May Like: Can A Person Have Medicaid And Private Insurance
Recommended Reading: Can Medicaid Take Your Life Insurance
What Happens After I Apply For Medicaid In Florida
After you submit your Florida Medicaid application, you may be required to attend an interview with a Department of Children & Families case worker.
Whether you will required to attend an interview depends on your situation:
If you are applying for Medicaid for your child alone, then no interview will likely be required.If you are applying for any other benefits at the same time, then an interview will likely be required.
During this interview, you will be required to bring documents that prove the information that you provided on your initial Florida Medicaid application.
See above for the list of documents that may be required during the interview.
Once you complete this interview, you will receive a call or a letter in the mail that will tell you whether you were approved or denied.
If you are denied benefits, you have the right to appeal but that appeal must be filed within a certain timeframe. As your caseworker for details.
Will Medicaid Provide Payment For A Family Member Who Needs Nursing Home Care
Louisiana’s Medicaid Program provides payment for special long term care support services, as well as full Medicaid health coverage, to eligible people who, because of their medical condition, require assistance with activities of daily living . Long-term care supports may be provided either in a facility or in an individual’s own home or in the community. Visit Medicaid Long-Term Care.
Don’t Miss: Is There Medicaid In North Carolina
North Carolina Medicaid Eligibility
Beyond the standard financial requirement, North Carolina looks at several factors in determining whether your application for benefits will be accepted. These include family size, need for long-term care, ability level, and if you receive Medicare.
Which Medicaid plan is best in North Carolina?
North Carolina provides different levels of coverage based on the above-mentioned factors, as well as other benefits for children and pregnant women. What coverage you qualify for depends on your level of medical and financial need.
Youll need to submit an online application to the Department of Health and Human Services.
North Carolina Medicaid Application:
How Do I Know If My Child Is Due For A Texas Health Steps Checkup
Texas Health Steps will send you a letter when it’s time for your child’s medical and dental checkups. You can also visit YourTexasBenefits.com or call the number below to find out if your child is due for a checkup.
Phone
Also Check: Does Medicaid Pay For Gastric Sleeve
What If I Am Not A U S Citizen
To be eligible for Medicaid in Louisiana, you must be resident of Louisiana and either U.S. citizen or a non-citizen who is lawfully present in the U.S. Non-citizens can qualify for coverage for emergencies and labor and delivery services if income requirements are met.Medicaid and LaCHIP coverage may be available to children up to age 19 who are lawfully residing and are otherwise eligible.
Apply For Medicaid In Florida
Online at ACCESS Florida, or submit a paper application by mail, fax or in person to a local service center. For help with the application process, call 866-762-2237.
Eligibility: Children up to 1 year old with family income up to 206% of FPL children 1-5 with family income up to 140% of FPL children 6-18 with family income up to 133% of FPL pregnant women with family income up to 191% of FPL young adults 19-20 with family income up to 30% of FPL adults with dependents with family income up to 30% of FPL.People who qualify for Supplemental Security Income automatically qualify for Medicaid. For information: SSI-Related Programs Financial Eligibility Standards
Recommended Reading: Dentist In Madisonville Ky That Accept Medicaid
Use Mybenefits Calwin Online Portal
The online portal of MyBenefits CALWIN is a great way to answer the question: how do I know if my Medi cal is active? You can also use the portal to find out your benefits amount. It also allows you to view all the notices that were sent to you. Typically, the notices are about documents that are required to keep your Medi-cal status active. Some notices inform you that you qualify for additional assistance programs.
If you do not have a MyBenefits CALWIN account, then create one and enjoy the convenience to check your Medi-cal status any time you want.
How Can I Check The Status Of My Health First Colorado Application
If you applied for Health First Colorado or Child Health Plan Plus , you can check your application status online through Colorado PEAK.
Even if you applied by mail, in-person, or over the phone, you can still create a Colorado PEAK account and find out the status of your application online. It may take up to 45 days or up to 90 days if the application requires a disability determination from the date your application was received for a case number to be assigned to you. Once you are assigned a case number, you can check your status and benefits online through Colorado PEAK. Get more information about your case number and where to find it.
More Topics
Recommended Reading: Dental Care That Accepts Medicaid
Don’t Miss: How Does Someone Get Medicaid
How To Find Out Medicaid Application Status
There are close to 75 million people covered by Medicaid in the U.S., and this program is funded and administrated by states and the federal government. Once an application is complete, it can take a while to process applicants can easily check the status of Medicaid applications, though. It is also important to note that some states have expanded their Medicaid services recently, and Healthcare.gov has links that provide specific details on this.
Video of the Day
You May Like: How To Qualify For Medicaid
