How Can I Find A Dentist Accepting Medicaid
Not all dentists take Medicaid patients, so you need to find a dentist that accepts your dental coverage. You can phone around or ask your doctor for a referral if you have specific dentists in mind.
If you arent hoping to see a specific dentist and are open to new care options, DentaQuest is a great resource. All you need is your city name and Medicaid ID card, and the website can give you a complete list of all the dentists in your area that accept Medicaid. They will also contact the clinic on your behalf in the case of a conflict.
Transitioning From Expanded Medicaid To Medigap
The more expensive way to cover the gaps in traditional Medicare is to buy a Medigap policy, which generally costs anywhere from a minimum of $25/month to more than $200/month to cover out-of-pocket costs for Parts A and B. Thats on top of premiums for Medicare Parts B and D .
The payoff is maintaining unlimited access to all healthcare providers who accept Medicare which almost all providers do. Heres more about choosing between Medigap and Medicare Advantage.
How Much Will Medicaid Cost Me
It depends. Every state is different. You will probably not have to pay a monthly premium for Medicaid, but most people do have some out-of-pocket costs.2 Emergency services, family-planning services, pregnancy-related services and preventive care for children are all fully covered with no additional cost to you.
Recommended Reading: Texas Medicaid Application Form For Elderly
Effective Date Of Coverage
Once an individual is determined eligible for Medicaid, coverage is effective either on the date of application or the first day of the month of application. Benefits also may be covered retroactively for up to three months prior to the month of application, if the individual would have been eligible during that period had he or she applied. Coverage generally stops at the end of the month in which a person no longer meets the requirements for eligibility.
Can I Qualify Even If My State Does Not Have Expanded Medicaid
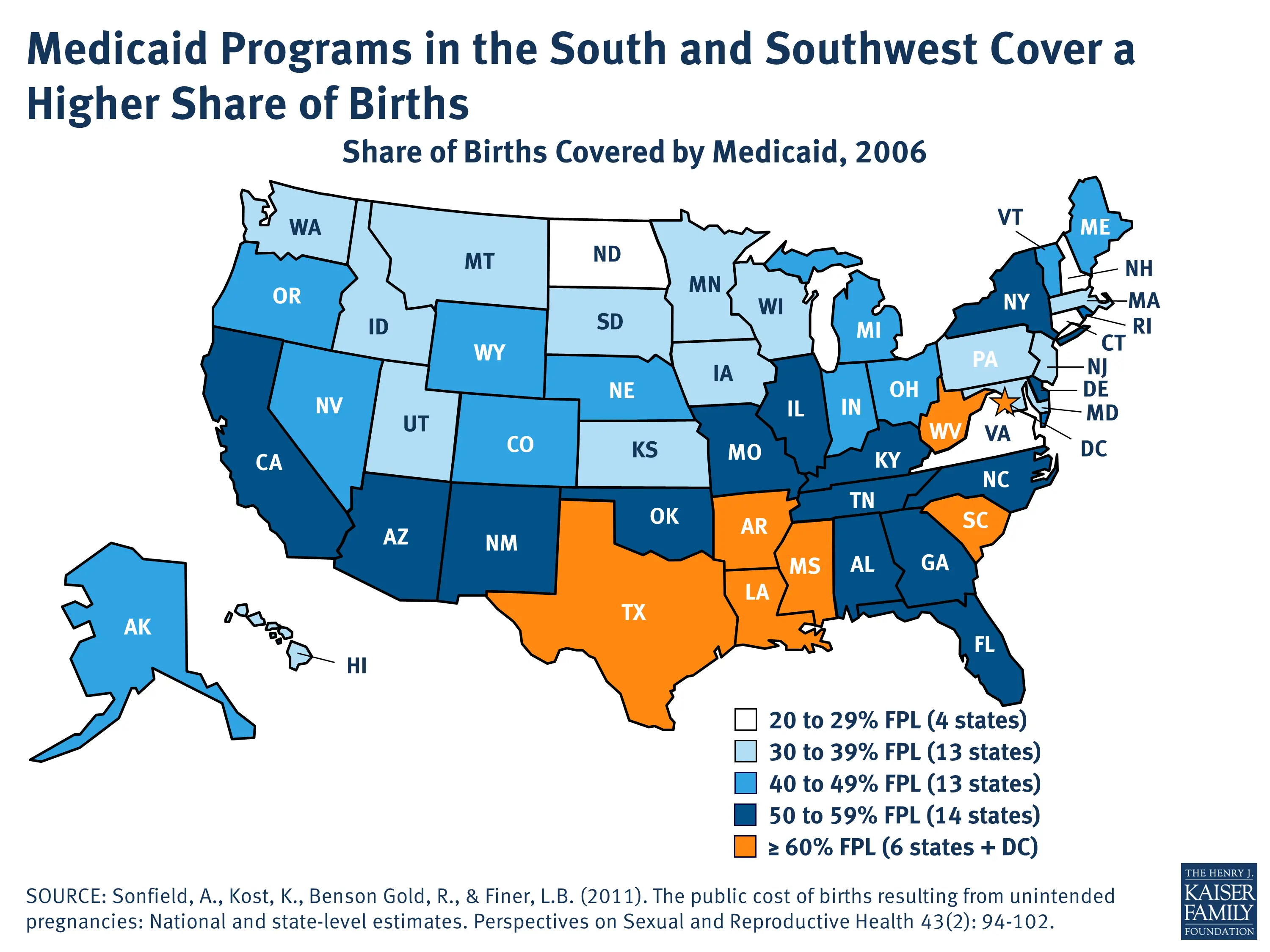
In states that have not expanded Medicaid, eligibility levels are lower than in states that have expanded. Even if your state hasn’t expanded Medicaid and it looks like your income is below the level to qualify for financial help with a Marketplace plan, you should fill out a Marketplace application.
Also Check: Does Medicaid Cover Weight Loss Pills
What Steps Do I Need To Take To Move From Expanded Medicaid To Medicare
If youre enrolled in expanded Medicaid and youll soon be 65, youll want to familiarize yourself with the health coverage and assistance programs that might be available to you.
Understand that although your assets have not been taken into consideration to determine your eligibility for expanded Medicaid, that will likely change when you turn 65. Every state has an asset limit for full Medicaid eligibility if youre 65 or older, and most states also have asset limits for their MSPs.
But if you do qualify for an MSP particularly the Qualified Medicare Beneficiary program along with Extra Help for prescription drugs you may find that you still qualify for premium-free coverage and very limited out-of-pocket costs.
Youll want to reach out to your states Medicaid office prior to turning 65, to be sure you understand the specifics of 65+ Medicaid and MSP eligibility.
You can also reach out to the Medicare SHIP in your state, to see what resources and assistance are available to you.
You might also want to find a Medicare broker who can help you understand the available Medigap, Part D, and Medicare Advantage plans. Your limited income might make you a good candidate for a low-cost or zero-premium Medicare Advantage plan, leaving you with just the cost of Medicare Part B.
Heres more about choosing between Medigap and Medicare Advantage theres no single solution that works for everyone, so take your time and compare the options available to you.
Do You Need More Help
If you arent sure if your Medicaid coverage has been approved yet or if it is still active, you can check Manage My Case or call the states Automated Voice Recognition System at 1-855-828-4995 with your Recipient Identification Number .
If you have an urgent medical need and need Medicaid quickly, call the DHS Helpline at 1-800-843-6150.
You May Like: Medicaid Assistance For Nursing Home Care
About Medicaid For Adults
Medicaid offers healthcare coverage for adults that address a variety of health needs, including coverage for low-income adults, pregnant women, the elderly, and people with disabilities who meet certain income criteria.
- Women diagnosed with breast or cervical cancer through Women’s Health Check.
- People aged 65 or older who meet income requirements
- People who are blind or disabled
- Medicare Savings Program
- Basic Plan This plan provides health, prevention, and wellness benefits for adults who do not have special health needs. This plan includes annual physicals, immunizations, most prescriptions, doctor and hospital visits, and more.
- Enhanced Plan This plan is for individuals with disabilities or special health needs. This plan has all the benefits of the Basic Plan, plus additional benefits. Most of the time, individuals will need to be referred by a doctor to become eligible for the enhanced plan.
- Medicare-Medicaid Coordinated Plan Designed for people who are eligible and enrolled in both Medicare and Medicaid, . This plan has all the benefits of the Enhanced Plan, plus allows people to enroll in a managed care plan to help coordinate Medicare and Medicaid benefits. There are many advantages to enrolling in managed care, one of the most valuable is access to a care coordinator who helps people with complex medical conditions to achieve better health.
Steps to sign up for the PHA program
Q How Can I Find Out If I Can Get Medicaid
A. You can find out if you qualify for Medicaid or other medical assistance and social service programs by speaking with a representative at your local State Service Center. Call Medicaid Customer Relations at 1-800-372-2022 or 255-9500 to be directed to the appropriate office where someone can help you.
Don’t Miss: Does Medicaid Cover An Iud
Work Requirements And Medicaid In The Future
In April 2021, President Biden began unwinding the previous administrations attempts to create and implement new eligibility requirements for adults without children or disabilities. These requirements would have allowed states to remove Medicaid coverage from childless adults who are not disabled, who do not have jobs, or are not involved in work-related or volunteer programs. Even states that received approval had not enforced work requirements as of April 2021, because federal courts invalidated the rules.
In an effort to encourage states to expand Medicaid, President Bidens 2021 American Rescue Plan contains more matching of federal funds as an incentive. The U.S. Department of Health and Human Services has now revoked work requirements in the Medicaid programs of Arizona, Arkansas, Indiana, Michigan, New Hampshire, Ohio, South Carolina, Utah, and Wisconsin. Kentucky and Nebraska withdrew their applications for work requirements after initially receiving approval.
According to the Pew Charitable Trusts, at least 15 states either applied for or received permission to impose work requirements during the previous administration. The nonpartisan research and policy Center on Budget and Policy Priorities reported that in 2018, Arkansas removed more than 18,000 Medicaid beneficiaries off the rolls because they did not meet new eligibility requirements.
Q How Will I Receive My Medical Care
A. In Delaware, Medicaid benefits are provided mainly through a managed care organization, or MCO, under contract with the state. Managed care is an organized way to ensure that people receive the quality medical care they need in the most cost-effective manner. Some Medicaid recipients in Delaware those who also receive Medicare and those in Long Term Care Medicaid programs such as the Nursing Facility program do not receive their medical care through a managed care organization.
DMMA provides a choice of managed care organizations so you can select the MCO plan that is best for you and your family. Delaware contracts with two managed care plans AmeriHealth Caritas and Highmark Health Options.
The Medicaid MCO provides almost all of the care for Medicaid members who join their plan. Prescription and non-emergency medical transportation services are covered directly by Medicaid, not through the MCO. Medicaid recipients need to show their Medicaid card to pharmacies and transportation providers when receiving these services.
Recommended Reading: Does Medicaid Cover Substance Abuse Treatment
We Still Have Savings But Our Work Has Gone Away Is Medicaid An Option
Maybe. The answer varies by state. In general, a single person must have no more than $2,000 in cash assets to qualify. If youre over 65, the requirements are more complex. Whatever your age, there are strict rules about asset transfers. Medicaid may take into consideration any gifts or transfers of cash youve made recently.
Which States Have Emergency Adult Dental Coverage
There are situations where the need for dental care becomes an emergency. Infections of the mouth can be very dangerous due to the proximity to the brain.
What counts as a dental emergency can vary from state to state. If it is life-threatening or requires surgery, then it is an emergency. Severe and acute pain is probably an emergency, so you can probably get extractions if needed as well.
If you arent sure if you are in an emergency, your best course of action is to call a dentist or have someone call for you. They will be able to advise on the situation.
States with only emergency adult dental:
- Alaska
- Utah
- Virginia
If you live in one of these states, Medicaid will cover you in a dental emergency. If you need treatment outside of this, see above for resources for those without dental coverage.
Don’t Miss: Medicaid Doctors In Raleigh Nc
What Costs Should You Expect If Youre Moving From Expanded Medicaid To Medicare
If youve been enrolled in expanded Medicaid, its likely that you havent had to pay any monthly premiums. But that may change when you turn 65.
For most people, Medicare Part A is premium-free, but Medicare Part B costs $148.50/month in 2021, and is projected to be $158.50/month in 2022. This is true even for many of the people who qualified for premium-free expanded Medicaid prior to age 65.
However, full Medicaid coverage is available to people age 65+ who have very limited income and assets. And there are Medicare Savings Programs that will cover the cost of the Part B premiums , for people who are eligible. Depending on the MSP, the income limits can be quite a bit higher than the income limit for expanded Medicaid eligibility.
But the catch is the asset limits. There are several states that dont use asset limits for their MSPs. In most states, however, to be eligible for MSP assistance, your assets cant exceed $7,970 if youre single, or $11,960 if youre a couple. There are some assets that arent taken into consideration, including your primary residence, one car, household belongings, and a burial plot, along with up to $1,500 in burial expenses.
Which States Have Limited Adult Dental Coverage
When Medicaid has limited coverage for dental, this usually means one of two things. Either there is a financial cap to the dental care you can have covered, or there is a fixed list of services that will be covered.
If it is a financial cap, the range is usually somewhere between $500 to $1000. Once that amount is met, dental wont be covered unless it is an emergency.
If it is a fixed list, your Medicaid dental benefits will typically include preventative care such as cleanings and restorative care such as fillings, as well as emergency care.
States with limited adult dental care:
- Arkansas
- Washington
- Wisconsin
Something that is not typically covered even in comprehensive plans is adult orthodontic care or braces. If this is something that you require, you may need to pay out-of-pocket. Luckily, this is not something that would be an emergency, so you will still have all the care that you need to maintain good dental health.
Also Check: Dentist Fayetteville Nc Accept Medicaid
Medicaid Covers 1 In 5 Americans And Serves Diverse Populations
Medicaid provides health and long-term care for millions of Americas poorest and most vulnerable people, acting as a high risk pool for the private insurance market. In FY 2017, Medicaid covered over 75 million low-income Americans. As of February 2019, 37 states have adopted the Medicaid expansion. Data as of FY 2017 show that 12.6 million were newly eligible in the expansion group. Children account for more than four in ten of all Medicaid enrollees, and the elderly and people with disabilities account for about one in four enrollees.
Medicaid plays an especially critical role for certain populations covering: nearly half of all births in the typical state 83% of poor children 48% of children with special health care needs and 45% of nonelderly adults with disabilities and more than six in ten nursing home residents. States can opt to provide Medicaid for children with significant disabilities in higher-income families to fill gaps in private health insurance and limit out-of-pocket financial burden. Medicaid also assists nearly 1 in 5 Medicare beneficiaries with their Medicare premiums and cost-sharing and provides many of them with benefits not covered by Medicare, especially long-term care .
Figure 4: Medicaid plays a key role for selected populations.
Medicaid Spending Is Concentrated On The Elderly And People With Disabilities
Seniors and people with disabilities make up 1 in 4 beneficiaries but account for almost two-thirds of Medicaid spending, reflecting high per enrollee costs for both acute and long-term care . Medicaid is the primary payer for institutional and community-based long-term services and support as there is limited coverage under Medicare and few affordable options in the private insurance market. Over half of Medicaid spending is attributable to the highest-cost five percent of enrollees. However, on a per-enrollee basis, Medicaid is low-cost compared to private insurance, largely due to lower Medicaid payment rates for providers. Analysis shows that if adult Medicaid enrollees had job-based coverage instead, their average health care costs would be more than 25% higher. Medicaid spending per enrollee has also been growing more slowly than private insurance premiums and other health spending benchmarks.
Figure 9: Medicaid per enrollee spending is significantly greater for the elderly and individuals with disabilities compared to children and adults.
Read Also: Medicaid Funded Home Care Services
Appeals And Fair Hearings
Medicaid estate recovery is the process through which each state recovers the costs of medical services it has paid from the estate of the person who received those services. The Medicaid estate recovery program impacts two groups of people receiving Medicaid benefits:
- Anyone over the age of 55 who has received Medicaid assistance, and
- Anyone who is permanently institutionalized and has received Medicaid assistance, regardless of age.
The estate recovery program may collect money from the estate of a deceased Medicaid recipient as repayment for any medical care services that were provided to the recipient and paid for by Medicaid, while the recipient was over 55 years of age, or permanently institutionalized, regardless of age.
Medical care includes a wide range of services, including nursing home and community based in-home care services. It also includes any hospital and prescription drug services the participant received while in a nursing home, or while receiving in-home care. Medical care also includes capitation payments to Medicaid-contracted health insurance companies or medical providers administering a defined package of benefits. The federal government directs states to pursue Medicaid estate recovery for these services.
- During the lifetime of the surviving spouse, regardless of where he or she lives.
- From a surviving child who is under age 21 years or is blind or permanently disabled , regardless of where he or she lives.
Canceling Classic Medicaid Coverage
Don’t Miss: Apply For Medicaid Rochester Ny
I Got Laid Off But They Offered Me Cobra It Is Way Too Expensive Can I Qualify For Medicaid
Maybe. For many people, COBRA, the insurance you can buy into when you lose your job, is too expensive. And even if you decide to enroll in COBRA, it doesnt mean you cant apply for Medicaid. You can apply for and enroll in Medicaid any time. If you qualify for Medicaid, you can drop your COBRA coverage even after you enrolled in it.
