Q How Do I Join A Managed Care Organization
A. After being notified that you are eligible for Medicaid , you will receive in the mail a packet of information about the different MCO plan options for receiving your Medicaid benefits. You may choose any plan described in this mailing. You probably want to choose a Managed Care Organization to which your doctor belongs. If you need help making this decision, call the Health Benefit Manager at the phone number in the mailing.
Q How Can I Find Out If I Can Get Medicaid
A. You can find out if you qualify for Medicaid or other medical assistance and social service programs by speaking with a representative at your local State Service Center. Call Medicaid Customer Relations at 1-800-372-2022 or 255-9500 to be directed to the appropriate office where someone can help you.
Medicaid Eligibility And Waivers
While Medicaid eligibility is based on federal law, the eligibility standards, services, and support available through Medicaid waivers vary dramatically between states. These services include case management, residential services, employment services, and other non-residential services. An important consideration is that many states have years-long waiting lists for home and community-based services, and new residents must reapply and go to the end of the line.
Read Also: What Home Health Services Are Covered By Medicaid
Q If I Have Private Health Insurance Can I Be Eligible For Medicaid
A. It depends. If your income is low, and you have minor children, you and your children can have private health insurance and still be eligible for Medicaid. Certain Medicaid qualifying programs require that you not have any other health insurance in order for you to get Medicaid. If you have both private health insurance and Medicaid, you should show both your Medicaid card and your private health insurance card to your medical provider each time you receive services.
I Just Moved I Need To Transfer Medicaid To Another State How Do I Go About Doing So And Can I Apply Online
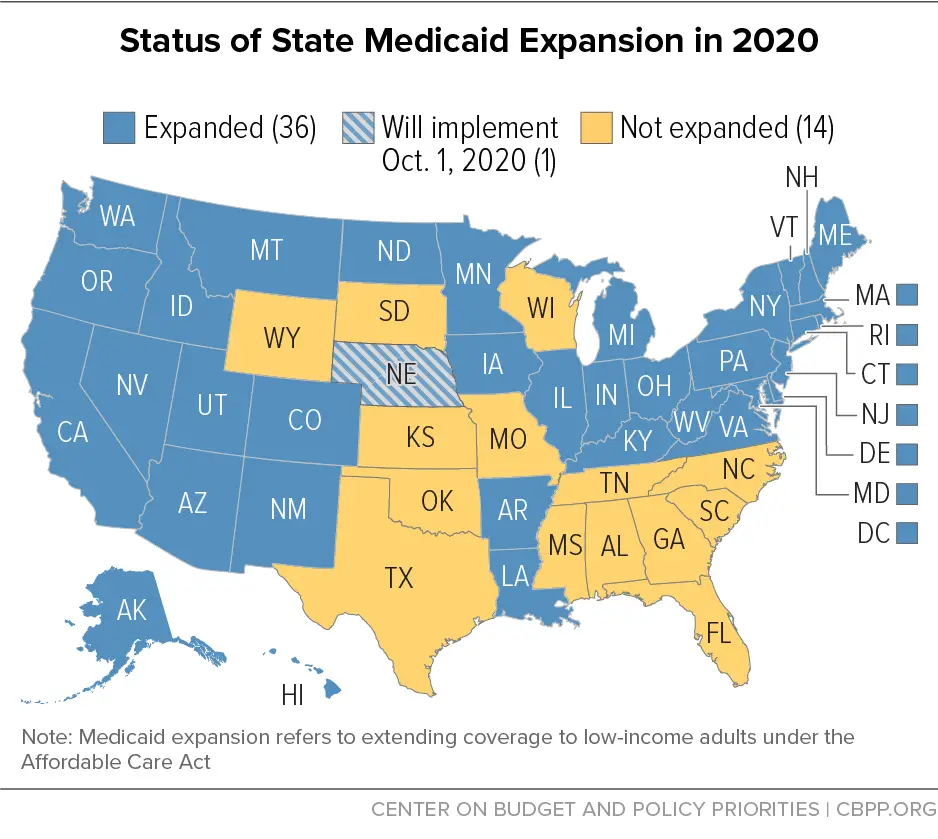
A) Each of the fifty states operates their Medicaid program differently. Therefore, Medicaid eligibility requirements are not consistent across states. Individuals are required to reapply for Medicaid in the state in which they are relocating. In addition, an individual cannot receive Medicaid benefits simultaneously in two states. There is no program that allows you to transfer your Medicaid coverage from one state to another. Therefore, if you are relocating and moving from one state to the next, you will need to reapply for Medicaid in the new states. Yes you can apply online for Medicaid in all states.
You May Like: Iowa Dhs Medicaid Income Guidelines
Health Plan Report Cards
People across Texas shared their thoughts about their health plan, and rated them, one to five stars, on the services their plan provided. You can compare plans using the overall ratings or by looking at the services that matter the most for you and your family.
You can view the report cards on the Managed Care Report Cards page. Click the program you are enrolled in and find your service area to see plans available to you.
Income Eligibility For Medicaid
Medicaid eligibility may be based on your modified adjusted gross income , if you are:
- 19 and 20 years old and living with your parents
- A childless adult between the ages of 19-64 years old, living in a state with Expanded Medicaid
- Eligible for the Family Planning Benefit Program
- Filing for a child who is younger than 19 years old
- The parent or caretaker of someone meeting these criteria
- A pregnant woman
To calculate your MAGI:
See MAGI requirements for each state.
You May Like: Nys Medicaid Home Care Eligibility
How To Switch Medicaid When Moving
- https://obamacarefacts.com/questions/how-to-switch-medicaid-when-moving/
- Reply. Erin on February 23, 2017. There really is no way to switch Medicaid from one state to another without contacting the state you are insured in. It is a state run program, so heâll need to apply in New York. Heâll also need to cancel his Medi-Cal coverage immediately once he is enrolled in Medicaid in NY. Reply.
Do You Have A Medicare Supplement Plan Heres How To Handle Your Move To Another State
If youre enrolled in a Medicare Supplement plan and move to another state, you may be able to keep the same policy. There are 10 standardized Medigap plans available in 47 states . Because the plans are standardized in most states, you may be able to remain with the same plan. But be aware that you might have to pay more for the Medigap plan in your new state, and you might have to answer some questions about your health history..
Most Medicare Supplement plans let you see any doctor who accepts Medicare assignment, but one type of Medigap plan called Medicare SELECT may require you to use providers within its network. If you have a Medicare SELECT policy and you move out of the plans service area:
- You can sign up for a standardized Medigap policy from your current Medigap policy insurance company that includes the same, or fewer, benefits as your current Medicare SELECT policy.
- Generally, you can sign up to buy any Medigap Plan A, B, C, F, K, or L thats available in the area where you live.
- You wont have to undergo medical underwriting if youve had your Medicare SELECT policy for more than six months. Otherwise, the insurance company may review your health history and may charge you more if you have a health condition.
You May Like: United Healthcare Medicaid Louisiana Application
Recommended Reading: Does Sc Medicaid Cover Breast Pumps
Q If I Dont Qualify For Medicaid Is There Any Other Help For Me Or My Children
A. Yes. Many organizations in Delaware are dedicated to the principle that health care should never be beyond the reach of those who need it. If you need health care, but do not have insurance coverage, the people at the Delaware HelpLine have a wealth of information about organizations that provide health care at reduced rates for uninsured individuals. Call the Delaware HelpLine toll-free at 1-800-464-HELP from Monday Friday from 8:00 a.m. to 5:00 p.m. The Delaware Helpline service is also available in Spanish. Additional information about the support provided by the Delaware Helpline can also be found by visiting www.delawarehelpline.org.
For example, you may qualify to receive discounted medical services through the Community Healthcare Access Program . CHAP helps connect uninsured individuals with affordable health care from primary care doctors, medical specialists, and other health providers including prescription programs, laboratory and radiology services. To find out more about this program, visit the website for the Community Healthcare Access Program, or call 1-800-996-9969 for eligibility guidelines.
You can read about CHAP and other healthcare resources for uninsured individuals in the Delaware Healthcare Resource Guide. This guide is also available in Spanish: Guía de Recursos de Salud.
Under 18:
Over 65:
Welcome To Indiana Medicaid
Welcome to Indiana Medicaid. On this site, you can learn about the different Medicaid programs and how to apply. Check out our Eligibility Guide to learn about eligibility for certain programs and see if you may qualify.
If you use assistive technology and the format of any material on this website interferes with your ability to access information, please . If you have a complaint about web accessibility or print communications in accessible formats, you may also . To enable us to respond in a manner most helpful to you, please indicate the nature of your accessibility issue, the preferred format in which to receive the material, the web address of the requested material, and your contact information.
Don’t Miss: First Choice Medicaid Sc Address
What Would The Process Be
While Medicaid is administered through each state,there is a federal law that says that you cannot have two Medicaid accountsoperating at the same time. If you wanted to move to a new state, you wouldneed to close your Florida Medicaid account, apply for Medicaid in your newstate, and then wait for approval.
Tips For Moving To Another State With Medicare
Home / FAQs / General Medicare / Tips for Moving to Another State with Medicare
If youre moving to another state with Medicare, youre going to want the best tips! Before relocating, you might want to learn more about how Medicare works in your new state. Also, you may want to prepare yourself for a change in premium or coverage options depending on your current policy.
Recommended Reading: Assisted Living Facilities That Take Medicaid
Recommended Reading: Dentist In Denver Co That Take Medicaid
Moving To A New State Can Affect Medicaid Eligibility
What happens if you or your family member must move from one state to another and then apply for Medicaid? What if you or your family member is already in the Medicaid program and then moves? Will you lose your eligibility?
First of all, it is a violation of the U.S. Constitution to impose a residency requirement on an individual who moves into a state and then needs to apply for Medicaid. So the day after an individual moves, he or she can apply for Medicaid.
That being said, the person who is moving will still need to meet the asset and income requirements of the new state’s version of the Medicaid program. In addition to the federal requirements that apply to all states , there are other optional requirements and regulations that vary from state to state. If the requirements for eligibility are different in a person’s new state of residence than they were in their previous state of residence, then they must meet the eligibility requirements of the new state before Medicaid will cover their expenses.
For example, there may be different requirements as what types of gifts are allowed, different calculations for penalty periods following gifts, or different rules governing Medicaid annuities or the exemption of the personal residence.
Just Moved Heres What You Need To Know About Health Insurance
Whether youâre moving to or within California, find out how your coverage is affected.
Between packing up belongings, filling out paperwork and finding a new home, moving is a huge challenge. In all the chaos, you may not have considered how relocating could affect your health insurance. It might not be practical now for you to see the same health care providers, and your current health plan may not extend to your new area. No matter what, you will want to find a plan that meets all of your medical needs in your new locale.
Getting Covered in Your New Home
When youâre moving, your address might not be the only thing changing. You may also be able to change your existing health plan or sign up for new health coverage.
Normally, the only time you can enroll in a health plan is during the open enrollment period. However, your move may be considered a qualifying life event, giving you access to special enrollment. If you qualify, you have 60 days from the date of your move to apply for coverage.
For your move to qualify, it must meet one of the following criteria: Either you moved to California from another state or country, or you moved within California, and at least one health plan is available in your new area that wasnât available at your previous residence.
How to Applyfor Coverage
Step 1: Weigh all your options.
Step 2: Gather necessary paperwork.
Before you apply for a new health plan, make sure you have these items handy:
Step 3: Apply for health coverage.
Read Also: Will Medicaid Pay For A Hospital Bed
How Retroactive Medicaid Helps In The Moving Process
A common worry among Medicaid Long Term Care recipients who are moving out of state is having a lapse in benefits. This is understandable since its not possible to simply transfer Medicaid coverage from one state to another, and having Medicaid coverage in two states at the same time is not allowed, either.
These circumstances will lead to a lapse in coverage for a Medicaid recipient moving out of state because coverage in their old state will end before the application in their new state is approved. However, Retroactive Medicaid will pay for the expenses accrued during that lapse, up to three months, as long as the Medicaid applicant is eligible for Medicaid coverage in their new state during that time. Worth noting though is that some states are beginning to limit their retroactive Medicaid coverage.
While the three-month window Retroactive Medicaid provides for someone to apply for Medicaid Long Term Care in a new state is not especially big, it should be big enough There are no residency requirements for Medicaid, so a person can apply for Medicaid on the first day they become a resident in a new state. And the application process for Medicaid approval does not take very long, usually between 15 and 90 days.
Q How Will I Receive My Medical Care
A. In Delaware, Medicaid benefits are provided mainly through a managed care organization, or MCO, under contract with the state. Managed care is an organized way to ensure that people receive the quality medical care they need in the most cost-effective manner. Some Medicaid recipients in Delaware those who also receive Medicare and those in Long Term Care Medicaid programs such as the Nursing Facility program do not receive their medical care through a managed care organization.
DMMA provides a choice of managed care organizations so you can select the MCO plan that is best for you and your family. Delaware contracts with two managed care plans AmeriHealth Caritas and Highmark Health Options.
The Medicaid MCO provides almost all of the care for Medicaid members who join their plan. Prescription and non-emergency medical transportation services are covered directly by Medicaid, not through the MCO. Medicaid recipients need to show their Medicaid card to pharmacies and transportation providers when receiving these services.
Don’t Miss: Is There Medicaid In North Carolina
What Happens With Medicaid Long Term Care Coverage When Moving From State To State
SummaryMedicaid Long Term Care coverage cannot be directly transferred from state to state. Instead, a Medicaid recipient who is moving out of state must end their Medicaid coverage in the state they are leaving and then reapply in their new state. The process can be complicated, but proper research and advance planning, it is possible with minimal or no loss of coverage.
Changing Plan In The First 90
Once you enroll in the Medicaid program, you will be given an introductory booklet from your local Medicaid office. As you open and read the booklet, you will see the different plans that you could choose.
You may either choose by yourself or your local Medicaid office will choose the plan for you based on the personal details you provided when you signed up. Since you are a new member, there are times that you are not knowledgeable enough about the program therefore, you end up choosing the plan, which is not right for your needs, or the initial plan chosen by the Medicaid office does not suit your needs.
Fortunately, as a new member of the Medicaid program, you are still free to change your plan within the first 90-day trial. Here are the steps on how to do it:
Online Vs. Visit local Medicaid office
Well, in switching Medicaid healthcare plans, you may do it online or you may call your local Medicaid office to set you an appointment. Either ways are effective methods in changing your local Medicaid healthcare plan.
Changing your Medicaid Plan Online
The easiest and most convenient way to change your Medicaid healthcare plan is to do it online since most states offer online accounts for Medicaid members. You may also change your plan through Healthcare.gov if you have signed up there initially.
- Set up your online account by visiting your local Medicaid website.
- You need to provide your Social Security card number and then your Medicaid ID number.
You May Like: List Of Texas Medicaid Managed Care Plans
Need Help Applying For Altcs In Arizona
If youre moving to Arizona and need help setting up Medicaid, speaking with a lawyer is a good place to start. The application process itself can be complex and confusing, and making mistakes can set you back in attaining benefits and services. If your situation is complicated or you need help meeting the eligibility requirements, one of our attorneys can answer your questions.
Contact the JacksonWhite ALTCS team today at and learn more your options for long term care.
How Long Does It Take To Transfer Medicaid To Another State
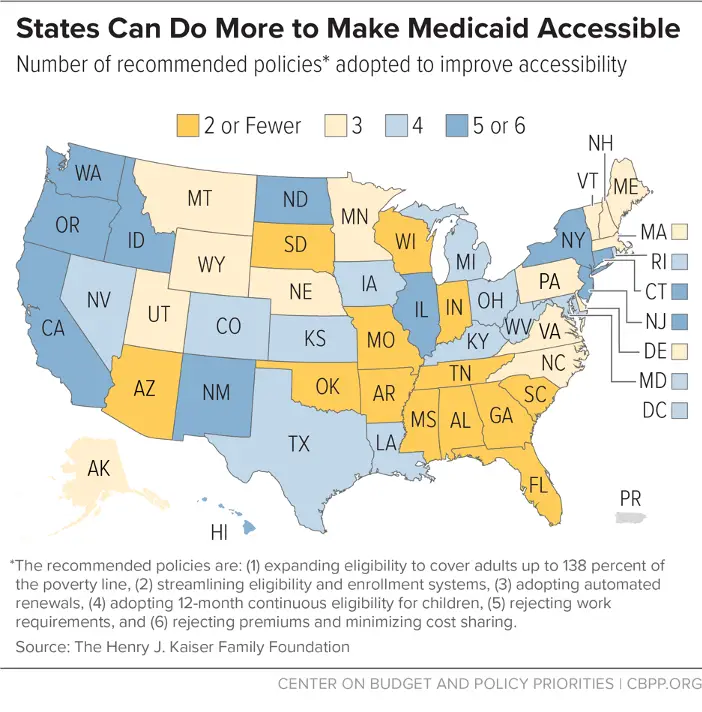
How long it takes to switch state Medicaid coverage depends on the state in which you’re applying for coverage. After submitting an application, it usually takes between 15 and 90 days to receive a letter of approval. Most states offer retroactive Medicaid coverage, meaning you can receive coverage for medical services prior to the date of your applications approval. However, you may need to pay for services out of pocket until the retroactive coverage begins. For this reason, it’s important to keep all the medical bills and receipts that you receive while you are waiting for Medicaid approval.
Read Also: Does Medicaid Cover Contacts In Florida
