Medicare Part B Enrollment And Penalties
Medicare Part B is optional, but in some ways, it can feel mandatory, because there are penalties associated with delayed enrollment. As discussed later, you dont have to enroll in Part B, particularly if youre still working when you reach age 65.
However, if you dont qualify for a Special Enrollment Period , then you may incur penalty charges. These penalty charges are indefinite for as long as you keep Medicare Part B. When should you enroll in Medicare Part B? If youre not automatically enrolled because of the aforementioned conditions, then here are your enrollment options:
- You have a seven-month initial period to enroll in Medicare Part B. The seven months include the three months prior to your 65th birthday, the month containing your 65th birthday and the three months that follow your birthday month. If you turn 65 on March 8, then you have from December 1 to June 30 to enroll in Medicare Part B.
- If you delay enrollment, then you have to wait until the next general enrollment period begins. For Medicare Part B, you have from January 1 through March 31 to enroll. Coverage doesnt begin until July.
How Do I Know If I Qualify For Medicaid And Medicare
Twelve million individuals are currently enrolled in both Medicaid and Medicare.1 These individuals are known as dual eligible beneficiaries because they qualify for both programs. As long as you meet the federal qualifications for Medicare eligibility and the state-specific qualifications for Medicaid eligibility, you will qualify as a dual eligible. To qualify for Medicare, individuals generally need to be 65 or older or have a qualifying disability.
There are several levels of assistance an individual can receive as a dual eligible beneficiary. The term full dual eligible refers to individuals who are enrolled in Medicare and receive full Medicaid benefits. Individuals who receive assistance from Medicaid to pay for Medicare premiums or cost sharing* are known as partial dual eligible.
*Cost sharing is the amount of your health care that you pay out of your own pocket. Typically, this includes deductibles, coinsurance, and copayments.
Do I Need Medicaid If I Have Medicare
Medicaid and Medicare are the two largest publicly funded health programs in the country, with different missions that often overlap. Medicare provides health coverage to seniors and some individuals with disabilities. Medicaid covers adults and children who cannot afford insurance, or who have health care costs they cannot afford. Often, an individual will be eligible for coverage through both programs. The following blog will describe how Medicare and Medicaid interact. Part one gives an overview of Medicare, what it covers, and what options are available for more coverage. Part two will describe how Medicare and Medicaid work together.
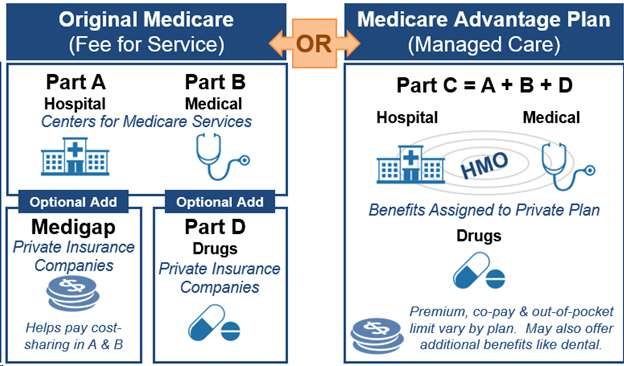
Part 1: Medicare, MediGap, and Medicare AdvantageFor many seniors, health insurance coverage can be very confusing. Most seniors know that they are eligible for Medicare when they reach age 65, but its easy to get confused about what is and isnt covered. Lets dive into the different Medicare options to help make things clear.
Seniors who are retired should enroll in both A and B as soon as they are eligible. If they enroll late, they may be penalized by having to pay Part A premiums or a higher premium for Part B. Seniors who are still working or whose spouse is still working may be able to delay enrolling in Medicare and keep the insurance provided by the employer.
Donât Miss: Are Walkers Covered By Medicare
Don’t Miss: How Much Money Disqualifies You For Medicaid
Where Can I Find Out More
- Medicaid.gov has links to information explaining the program and to every states Medicaid office.
- Each state has a State Health Insurance Assistance Program that provides counseling and help for Medicare beneficiaries. SHIP counselors can answer some of your Medicaid questions and refer you to local Medicaid officials to help with others.
- The National Council on Aging has a benefits checkup website that has information on Medicare, Medicaid and other programs that help older Americans.
More on Medicare
What Might Medicaid Pay For That Medicare Doesnt
- The premium for Medicare Part B, which covers doctor visits and other outpatient services. That monthly premium will be $135.50 in 2019.
- The Medicare Part B deductible, which will be $185 for 2019.
- The Medicare PartA deductible, which for 2019 will be $1,364 for hospital stays.
- Both Medicare Part A and Part B copays and coinsurance.
- The Medicare Part D premium, deductibles and copays for prescription drugs. Coverage for those costs is available through the Extra Help program, which Medicaid and Medicare Savings Program enrollees automatically qualify for.
- Nursing home care and home- and community-based long-term services and supports.
- In some states, Medicaid will cover benefits that Medicare does not, such as dental care, transportation to and from doctor visits, eyeglasses, physical therapy and other services.
Read Also: Medicaid Omaha Nebraska Phone Number
Qualified Disabled And Working Individual
You may be eligible to purchase Medicare Part A benefits, but unable to afford it because of your low income. In this case, Medicaid will pay your Medicare Part A premium. This is more common with people under the age of 65.
In 2021, the maximum monthly income to qualify is $4,379 for an individual and $5,892 for a couple. The 2021 maximum asset level, however, is set at just $4,000 for an individual and $6,000 for a couple.
Are You Dual Eligible
Some people can be eligible for both Medicare and Medicaid at the same time.
Dual-eligible beneficiaries are individuals who are eligible for both Medicare and Medicaid.
People who are dual eligible share costs with state-run Medicare Savings Programs , which provide help with premiums, deductibles, coinsurance and copayments, depending on the participantâs income level and the specific MSP. There are programs where eligible participants may have no copayments or cost shares.
This material is provided for informational use only and should not be construed as medical advice or used in place of consulting a licensed medical professional. You should consult your doctor to determine what is right for you.
Humana is a Medicare Advantage HMO, PPO and PFFS organization and a stand-alone prescription drug plan with a Medicare contract. Humana is also a Coordinated Care plan with a Medicare contract and a contract with the state Medicaid program. Enrollment in any Humana plan depends on contract renewal.
Some links on this page may take you to Humana non-Medicare product or service pages or to a different website.
Y0040_GNHKMBZEN
Also Check: Who Is The Medicare Coverage Helpline
You May Like: Medicaid Fraud Cases In Louisiana
Medicare Faqs And Information To Consider
Automatic Enrollment:
If you are already receiving Social Security benefits, Railroad Retirement benefits, or Federal Retiree benefits, your enrollment in Medicare is automatic. Your Medicare card should arrive in the mail shortly before your 65th birthday. Check the card when you receive it to verify that you are entitled to both Medicare Parts A and B.
Initial Enrollment Period:
If you are not eligible for Automatic Enrollment, contact the Social Security Administration at 800-772-1213 or enroll online at www.socialsecurity.gov, or visit the nearest Social Security office to enroll in Medicare Part A and Medicare Part B. You have a seven month window in which to enroll in Medicare without incurring a penalty. If youre not automatically enrolled in premium-free Part A, you can sign up for it once your Initial Enrollment Period starts. Your Part A coverage will start six months back from the date you apply for Medicare, but no earlier than the first month you were eligible for Medicare. However, you can only sign up for Part B during the times listed below.
General Enrollment Period:
- General Enrollment Period for Medicare Parts A & B
If you have coverage through a current employer, you are not required to enroll in Medicare Part A and B. Below are some things to keep in mind about each part of Medicare.
Also Check: Does Medicare Pay For Mobility Scooters
Extra Help Program For Medicare Part D
Medicaid is not the only government-sponsored resource that helps pay for medical costs. An individual can also apply for Extra Help, a program that helps beneficiaries with Medicare Part D, which covers prescription drug costs.
To qualify for Extra Help, a personâs combined investments, real estate, and savings must not exceed $29,160 if a person is married and living with their spouse or $14,610 if a person is single.
A person can visit Medicareâs website to find out more about getting and applying for Extra Help.
Read Also: Does Kelsey Seybold Accept Medicaid
Low Income Subsidy Questions
No. The “extra help” is a subsidy that people with Medicare and Medicaid automatically qualify for without having to complete an application.
If you do not have Medicaid, but Medicaid pays your Medicare Part B premium, you automatically qualify for “extra help” and you don’t need to apply.
You may still be eligible for “extra help” to pay for the Medicare prescription drug plan premiums. To apply for extra help, you should visit or call your local Social Security Administration office or apply on line at
What Is The Medicare Part B Deductible For 2021
Medicare Part B Premium and Deductible The standard monthly premium for Medicare Part B enrollees will be $170.10 for 2022, an increase of $21.60 from $148.50 in 2021. The annual deductible for all Medicare Part B beneficiaries is $233 in 2022, an increase of $30 from the annual deductible of $203 in 2021.
You May Like: How Much Money Will Medicaid Pay For Assisted Living
What Is Medicare Extra Help
Extra Help is a federal program that helps pay for out-of-pocket costs related to Medicare prescription drug coverage. Extra Help is also known as the Medicare Part D Low-Income Subsidy
The assistance that Medicare Extra Help may provide includes:
- Help paying Part D premiums
- Lowered out-of-pocket costs of prescription drugs
- An annual Special Enrollment Period to enroll in a Part D plan or switch to a new one
- Elimination of Part D late enrollment penalties
You automatically qualify for Extra Help if you are enrolled in Medicaid, Supplemental Security Income or a Medicare Savings Program.
You may still qualify for Extra Help if you are not enrolled in any of those programs but still have income and assets below a certain limit.
What Is Medicare What Is Medicaid

Medicare is a federal program generally for people who are 65 or older or have a qualifying disability or medical condition. Medicare Part A and Part B are provided by the federal government, and Medicare Part C and Part D, while federally governed, are provided by private insurance companies.
Medicaid is a state government program that helps pay health care costs for people with limited income and resources, and different programs exist for specific populations. Medicaid plans vary from state-to-state but follow federal guidelines for benefits.
Don’t Miss: Eye Doctors That Accept Straight Medicaid
If I Have Medicaid Do I Need Medicare Part D
Those that have Medicare and Medicaid will automatically be enrolled in a Part D plan if they dont select one for themselves. Its in the enrollees best interest to select a policy to enroll in, instead of being dropped into a plan. But, either way, Medicaid will help cover the costs associated with premiums, copayments, or coinsurances.
What Is Pace For Medicare And Medicaid
Another Medicare and Medicaid program is PACE, or Programs of All-Inclusive Care for the Elderly.
PACE helps older Medicare beneficiaries to seek health care within their community, in their home and at PACE facilities.
Some of the things that can be covered by PACE include:
- Adult day primary care
- Caregiver training
- Transportation to a PACE facility when medically necessary
PACE is not strictly restricted to Medicare dual eligible beneficiaries. You may be eligible for PACE with only Medicare or only Medicaid .
However, you must meet all of the following conditions:
- Be at least 55 years old
- Live in the service area of a PACE organization
- Require a nursing home-level of care
- Be able to live safely in the community with help from PACE
Dont Miss: Does Medicare Cover Chronic Pain Management
Also Check: Pregnancy Medicaid Ga Phone Number
Is Part B Worth It
Another mistake we see is people who thought they didnt need Part B because they are healthy. Ive seen a number of individuals who said they didnt get sick often so they opted to only enroll in Part A. Every one of these people assumed that Part A Hospital benefits cover everything in the hospital. So they decided to skip Part B thinking that they didnt mind paying out of pocket for an occasional doctor visit. They didnt realize Part B covers many things that occur in a hospital.
Usually they discover their error when they are sent for an MRI or a surgery and find out they now owe thousands or tens of thousands of dollars. Be sure you dont make the same mistake. If you are unsure, ask your insurance agent: Do I Need Medicare Part B?
If he or she tells you no, be sure you get a full explanation on why you are able to delay your. Get a second opinion if you are unsure, and never rely on Social Security to give you the right answer. Weve seen too many people get wrong answers from inexperience government employees.
Related Article: 7 Medicare Mistakes That Could Cost You
Medicaid Services Waivers & Fees
Some health care services are covered under Medicaid. For a full list of services covered and detailed explanations, consult the HUSKY Health Program Member Handbook. Download and/or print the handbook for your reference. HUSKY Health also includes enhanced services that have additional requirements. These benefits are below.
Community First Choice is a program in Connecticut offered to active Medicaid members. It allows individuals to receive supports and services in their home. These services include, but are not limited to, help to prepare meals and doing household chores, and assistance with activities of daily living . Go here for more information about Community First Choice and start the CFC Application online here.
Home and Community Based Services Medicaid Waivers help people who are financially and functionally eligible receive long-term Services & Supports in their homes.
Money Follows the Person Program is for Medicaid recipients in care facilities such as nursing homes, hospitals and other qualified institutions. The program can help people successfully transition back into the community.
Also Check: Can I Get A Breast Pump Through Medicaid
Do I Qualify For Full Medicaid
- The eligibility requirements vary from state to state, but generally states consider your annual income and financial assets when determining whether you are eligible for full Medicaid.
- If you live in one of the 37 states that will have expanded Medicaid as of next January and you earn no more than 138 percent of the federal poverty level , you may qualify. In states that havent expanded the program, the income levels for Medicaid eligibility vary greatly. For all eligibility questions, you should check with your state Medicaid office.
- If you are a Medicare beneficiary, your enrollment in Medicaid may be subject to a financial asset test. The value of assets youre allowed to have and still be eligible varies from state to state. The federal guidelines allow you $2,000, but some states have higher thresholds while others dont have an asset test at all.
- Excluded from the $2,000 asset test are such things as your home, one car, some burial expenses, some life insurance and household and personal items. States generally look back at an applicants assets for five years to make sure they havent divested themselves of those resources just to qualify for Medicaid.
- The asset income limits for Medicare Savings Programs are higher and change every January. For 2018, the limits for those programs are $7,560 for a single person and $11,340 for a married person living with a spouse and no dependents. As with full Medicaid, some states have higher resource thresholds.
Already Enrolled In Medicare
If you have Medicare, you can get information and services online. Find out how to .
If you are enrolled in Medicare Part A and you want to enroll in Part B, please complete form CMS-40B, Application for Enrollment in Medicare Part B . If you are applying for Medicare Part B due to a loss of employment or group health coverage, you will also need to complete form CMS-L564, Request for Employment Information.
You can use one of the following options to submit your enrollment request under the Special Enrollment Period:
Note: When completing the forms CMS-40B and CMS-L564
- State I want Part B coverage to begin in the remarks section of the CMS-40B form or online application.
- If possible, your employer should complete Section B.
- If your employer is unable to complete Section B, please complete that portion as best as you can on behalf of your employer without your employers signature and submit one of the following forms of secondary evidence:
- Income tax form that shows health insurance premiums paid.
- W-2s reflecting pre-tax medical contributions.
- Pay stubs that reflect health insurance premium deductions.
- Health insurance cards with a policy effective date.
- Explanations of benefits paid by the GHP or LGHP.
- Statements or receipts that reflect payment of health insurance premiums.
Some people with limited resources and income may also be able to get .
Read Also: Moving To Another State Medicaid
